Research. Survey of educators end-of-life care learning needs in a Canadian bacclalureate nursing programme
|
|
|
- Teresa Kelley
- 5 years ago
- Views:
Transcription
1 Survey of educators end-of-life care learning needs in a Canadian bacclalureate nursing programme Susan Brajtman, Frances Fothergill-Bourbonnais, Valerie Fiset Diane Alain Abstract Aim: To examine the potential need for faculty development in end-oflife care (EOLC) of theory and clinical educators in a collaborative bilingual undergraduate nursing programme in a Canadian university. Method: A purposive sample of 53 Anglophone and Francophone theory and clinical educators completed the Palliative Care Quiz for Nursing, the Frommelt Attitude Toward Care of the Dying Scale and an adapted Educators Educational [Q1: inserted for consistency with wording in text -?OK] Needs Questionnaire (Patterson et al, 2007 [Q2:?correct date in ref list and on PubMed]). Results: Results indicated that educators held positive attitudes towards caring for dying patients and had modest knowledge levels. Participants identified personal educational needs, preferred learning formats, support and barriers to teaching EOLC and to their participation in continuing educational programmes. Strategies to enhance the teaching and learning of EOLC content in the theory and clinical context were suggested. Conclusion: Nurse educators require time, opportunities and relevant resources to develop the competencies required to support the theoretical and experiential learning of students in EOLC. Recommendations include a variety of approaches for faculty development initiatives, including face to face and virtual, which allow nurse educators to share expertise. Key words: Curriculum content l Educators l End-of-life care l Learning needs l Nursing programmes l Palliative care Susan Brajtman is Associate Professor and Frances Fothergill- Bourbonnais is Professor, School of Nursing, Faculty of Health Sciences, University of Ottawa, Canada, Valerie Fiset is Nursing Professor, Algonquin College, Ottawa, Canada, and Diane Alain is Professor, School of Nursing, Faculty of Health Sciences, University of Ottawa, Canada Correspondence to: Susan Brajtman brajtman@ uottawa.ca Current trends in demographics and types and frequencies of disease in Canada and the world reflect an ageing population and a rising incidence and prevalence of cancer and other progressive life-threatening chronic diseases (World Health Organization, 2004; Haydon et al, 2006; Statistics Canada, 2007). This new reality requires all health professionals to shift their focus from only curing disease to also managing symptoms, maximizing function, and enhancing or maintaining quality of life. In Canada, priority has been given at the national level to the improvement of education of healthcare providers in palliative and end-of-life care (EOLC) (Health Canada, 2001). A national project, Educating Future Physicians in Palliative and End-of-life Care (EFPPEC, 2004), which initially focused on the education of medical students, has sparked some curriculum reforms and interest across the country in other healthcare disciplines. However, there is wide variation in the degree to which specific theory and clinical practice is part of undergraduate nursing curricula (Manias et al, 1997; Brajtman et al, 2007). This situation exists despite the expectation that graduating students meet the current standards of core competencies in end-of-life nursing care as determined by the Canadian Nurses Association (2003). The frequency and continuity of contact that nurses have with their patients makes their role central to the provision of care to the terminally ill and their families (Vachon, 2001). However, despite societal expectation that nurses have the knowledge and skills necessary to care for dying patients and their families, nursing education may not adequately prepare nurses for this critical role (Ferrell et al, 2000; White et al, 2001). The need for additional education in EOLC has been identified as a major concern of graduate nurses providing care for terminally ill patients in diverse settings, and a range of educational interventions have been developed to enhance nurses knowledge, attitudes and skills in this critical area (Samaroo, 1996; Adriaansen and Frederiks, 2002; Loftus and Thompson, 2002; Meraviglia et al, 2003). Nurse educators recognize the need to prepare undergraduate nursing students to acquire the relevant attitudes, knowledge and skills in various aspects of EOLC, such as effective pain and symptom management, supportive care interventions, ethical frameworks and the use of therapeutic communication skills (Sherman et al, 2004; Brajtman et al, 2007). Nursing students also need to be involved in learning experiences that facilitate an understanding of the relationship between relief of suffering and promotion of quality of life to patients and families psychosocial, spiritual, cultural and bereavement needs (Coyle, 2006). To date, studies have focused on assessing 170 International Journal of Palliative Nursing 2009, Vol 15, No 5 IJPN_15_5_Survey.indd /5/09 13:40:18
2 nursing students EOLC knowledge, skills and/or attitudes (Arber, 2001; Mallory, 2003), the amount and distribution of teaching that students receive in palliative care during their training (Lloyd-Williams and Field, 2002) and exploring new pedagogic strategies to enhance learning (Johnson and Jackson, 2005). Few studies have addressed the readiness and ability of the educators themselves to teach this content. It is assumed that nurse educators will have the knowledge required to teach EOLC, when in reality they may not feel adequately prepared to teach these specific competencies and may require additional education in this area (Sherman et al, 2004; Sullivan et al, 2005). To address the potential need for faculty development in EOLC, a learning needs survey was conducted with theory and clinical educators in a collaborative bilingual undergraduate nursing programme in a Canadian university. The objectives of the survey were to assess: 1. Educators current attitudes and knowledge related to EOLC using the Palliative Care Quiz for Nursing (PCQN) (Ross et al, 1996) and the Frommelt Attitude Toward Care of the Dying (FATCOD) scale (Frommelt, 1991) 2. Their perceived specific learning needs 3. The resources and support required to teach and integrate EOLC content into the curriculum using an adapted version of the Educators Educational Needs Questionnaire (Patterson et al, 1997). Educational needs assessments are necessary to identify preferred content and format of educational interventions, and to guide the development of programmes targeted at participants identified learning needs, preferences and work environment (Grant, 2002). This information can provide the basis for the development of educational interventions to enhance educators competence to teach and model key aspects of EOLC, and to effectively integrate the content into the curriculum. Methods A survey method was employed at the three sites of the baccalaureate 4-year programme, offered in both French and English. Participants included all full-time and part-time theory and clinical educators. Surveys were distributed in mailboxes and included an information letter explaining the purpose of the study and a request for completed anonymous surveys to be returned to the nursing faculty offices. To increase the response rate, an reminding them of the survey was sent to all educators 3 weeks later (Dillman, 1978). Ethical approval for the study was received from the academic institutions research ethics boards. Measures The measures used in this study assessed educators attitudes, knowledge, learning needs and teaching challenges in the area of EOLC. All measures, excluding one, were available in English and French. Palliative Care Quiz for Nursing (PCQN) (Ross et al, 1996): The PCQN is a 20-item true, false, and don t know quiz, which takes approximately 20 minutes to administer. It is used to assess nurses knowledge of palliative care (the basic type of information required for entry to practice), identify misconceptions and stimulate discussion. It can also be used to assess learning needs, as a teaching tool, and can contribute to the evaluation of educational programmes related to the provision of palliative care. It is widely used in Canada, and has been translated for use in China, Taiwan, and for the Francophone nursing community (Carroll et al, 2005). It has shown positive item total correlation coefficient and high internal consistency, validity and test retest reliability. Frommelt Attitude Toward Care of the Dying (FATCOD) scale (Frommelt, 1991): The FATCOD instrument consists of 30 Likert-type items scored on a five-point scale. It is used to assess nurses attitudes towards care of the dying and their families, with higher scores reflecting more positive attitudes. Possible scores range from a low of 30 to a high of 150. Results can provide educators with direction for course content development. The content validity index was 1.00 with an inter-rater agreement of A Pearson coefficient of 0.90 indicated reliability. This tool has not been translated into French and can therefore only be administered in English. Educators Educational Needs Questionnaire: A survey of the EOLC educational needs of longterm healthcare providers, developed by Patterson et al (1997), was adapted for use in this project. The questionnaires were coded to ensure anonymity. Questions asked about location and type of programme, courses taught, academic preparation, clinical experience, personal educational needs in EOLC, preferred learning format, and barriers to participation in educational programmes. Participants were also asked to provide additional comments in the sections related to educational needs in EOLC, preferred learning format, and barriers to participation in educational programmes. It is assumed that nurse educators will have the knowledge required to teach EOLC International Journal of Palliative Nursing 2009, Vol 15, No IJPN_15_5_Survey.indd /5/09 13:40:18
3 Thirty per cent had additional specialty training in palliative care, which varied from certification to ad hoc Analysis Content analysis was used to analyse data received from the open-ended questions (Polit and Beck, 2004). Descriptive statistics were used to analyse the demographic data, survey questions and data obtained from the PCQN and FATCOD. Results Of the 195 surveys distributed to all sites and programmes, 53 were returned (27% overall response rate). The response rate of full-time educators was 18/37 (49%), and part-time educators 35/158 (22%). The results reported reflect the combined responses of all four sites and programmes involved in the survey. Palliative Care Quiz for Nursing (PCQN) Analysis of the PCQN scores revealed a mean score of 12.8 out of a possible 20. One participant did not respond to this tool, therefore n=52. Table 1 shows examples of PCQN statements. The eight items in the table reflect the highest and lowest scores achieved by the educators. Frommelt Attitude Toward Care of the Dying Scale (FATCOD) The total score was determined by summing item scores on this Likert scale (Polit and Beck, 2004). Although Likert scales are considered to be ordinal, they have frequently been treated as interval data, and this has not been found to jeopardize the statistical analysis (Polit and Hungler, 1995). The FATCOD mean score was 132 out of a possible highest score of 150. Table 2 shows examples of FATCOD statements with participants responses. Educators Educational Needs Questionnaire (Patterson et al, 1997) Participants were asked a series of closed and open-ended questions related to demographics, if they were involved in teaching activities related to palliative care, and their perception of existing personal and organizational support and challenges to teaching this content. Background of subjects Of the 53 surveys returned, 18 were from teachers with full-time status and 35 were from part-time teachers. The majority (36; 68%) of participants were teaching clinical courses. Of those teaching clinical courses, 3% had a PhD, 33% a masters degree, 50% a BScN and 14% a diploma. The teachers were very experienced, with 28 (53%) having taught for at least 6 years while 25 (47%) had 0 5 years teaching experience. Thirty per cent had additional specialty training in palliative care, which varied from certification to ad hoc courses. Table 1. Palliative Care Quiz for Nursing highest and lowest percentages of correct responses * No. in % correct Item sample (n) responses Adjuvant therapies are important in managing 52 96% pain Drug addiction is a major problem when 52 93% morphine is used on a long-term basis for the management of pain The provision of palliative care requires 52 91% emotional detachment Individuals who are taking opioids should also 52 89% follow a bowel regimen During the terminal stages of an illness, drugs 52 40% that can cause respiratory depression are appropriate for the treatment of severe dyspnoea In high doses, codeine causes more nausea and 52 36% vomiting than morphine During the last days of life, drowsiness 51 28% associated with electrolyte imbalance may decrease the need for sedation The philosophy of palliative care is compatible 52 13% with that of aggressive treatment *Composite scores of all programmes; One subject did not respond to this item Teaching palliative care Twenty-three respondents (43%) had taught content related to palliative care in the past year and 26 (49 %) had not. Four respondents (8%) did not answer the question. Twelve of the 53 (23%) felt very well prepared to teach students to care for the dying, 43% felt somewhat prepared and 34% did not feel well prepared. Teaching palliative care: open-ended responses Educators teaching palliative care: The overriding impression from the open-ended responses of those who taught this content (19 of the 23 who responded) was that these educators saw the possibilities that existed to enhance the teaching and learning of EOLC. Participants suggested focusing on clinical conferences, identifying relevant patients in the clinical setting, encouraging students to communicate with patients and families about dying, allowing students to reflect on their experiences and their emotions, learning from other nurses, performing care after death, and including guest speakers in clinical conferences. 172 International Journal of Palliative Nursing 2009, Vol 15, No 5 IJPN_15_5_Survey.indd /5/09 13:40:19
4 Educators not teaching palliative care: Responses from the 12 respondents included comments such as: no interest in EOLC, EOLC not relevant, and EOLC not a priority. Support for student education in palliative care Participants were asked to identify their perception of support (almost none, some, a great deal) for student education in palliative care in their institution. Of the 44 who responded, 12 felt there was no support, 26 some support and 6 a great deal of support. Participants were asked to comment on their support for and barriers to teaching palliative care. Support for teaching palliative care content Participants felt that they could access support from nursing faculty with expertise and from clinical experts in the agencies, such as those in acute care hospitals. For example, 9 participants stated that they could access nursing faculty with expertise; 11 accessed clinical experts in agencies; 2 mentioned having flexibility in courses to add content or learn about resources; 3 described being able to access resources; 1 recalled a supportive 4th-year course coordinator. Table 3 provides examples of comments expressed by the educators that reflect their perceptions of greatest support for teaching palliative care at their educational institution. To ensure anonymity, participants are identified only by programme and full-time or part-time status. Resistance to student education in palliative care Participants were asked to identify their perception of resistance (almost none, some, a great deal) to education in palliative care in their institution. Of the 39 respondents, 33 felt there was no resistance, while 6 felt there was some. Barriers to teaching palliative care Participants identified specific barriers to teaching palliative care. These centered on the lack of a formal plan to integrate EOLC content in the current curriculum (8), and no room or time to add anything else to the curriculum, whether in theory or clinical courses (13). Table 3 shows examples of comments expressed by the educators that reflect their perceptions of barriers to teaching palliative care at their educational institution. Preferred learning formats Participants were asked in which format they would like to learn palliative care and to rank the Table 2. Examples of FATCOD statements and composite teacher responses * I would be uncomfortable talking about impending death with the dying person Strongly Strongly disagree Disagree Uncertain Agree agree 19 (37%) 15 (29%) 4 (8%) 11 (21%) 3 (6%) The nurse should not be the one to talk about death with the dying person (n=52) Strongly Strongly Not disagree Disagree Uncertain Agree agree applicable 33 (64%) 18 (35%) 1 (2%) 0% 0% 0% The dying person and his or her family should be the in-charge decisions makers Strongly Strongly Not disagree Disagree Uncertain Agree agree applicable 0% 0% 5 (10%) 18 (35%) 29 (56%) 0% FATCOD = Frommelt Attitude Toward Care of the Dying; *Composite scores of all programmes; n=52 Table 3. Examples of support for [Q16: added because it reads better -?OK] and barriers to teaching end-of-life care Support In a medical unit I have encouraged students to reflect on their emotional responses to dying patients and to interact with these patients and their families. (English programme, part time) Colleagues discussing what techniques they use with teaching students. (English programme, full time) Freedom to teach any related nursing issue in the clinical area. (English programme, part time) Il y a toujours des possibilités de demander de participer aux activités de formation en général, y compris en soins palliatifs. (French programme, part time) (Translation: There are always possibilities to ask to participate in activities for your development in general, including palliative care. ) We have some faculty with a keen interest in the topics and much clinical expertise. (English programme, full time) I suggest a palliative care teaching and research group such as the history of nursing research unit. We have such wonderful professors who specialize in palliative care yet their knowledge and resources do not appear visible to students on all levels of study. (English programme, part time) Barriers I integrated death and dying into the first year nursing course, but it was taken out when another prof took over! (English programme, full-time teacher [Q17:?delete for consistency with other comments, or is this intentionally different?] La résistance des collègues et l organisation du curriculum. (French programme, full time) (Translation: The resistance of colleagues and how the curriculum is organized. ) Competition with other topics for curriculum time and space. Lack of a clear plan for how, when and what specific topics and competencies will be included. (English programme, full time) Time constraints within the curriculum and when palliative care should be approached. (English programme [Q18: added for clarity -?OK], full time) International Journal of Palliative Nursing 2009, Vol 15, No IJPN_15_5_Survey.indd /5/09 13:40:19
5 It is therefore essential that theory and clinical nurse educators be adequately prepared in EOLC throughout the nursing programme [Q15: top L/H corner of picture in centre obscures some of the text in Physical domain please correct this and resubmit artwork. Also, please reset Decision Support in Psychological domain as Decision support (ie with lower case s in support)] choices from seminars, conferences, case studies, written information, lectures and online resources. Seminars were ranked first overall. Thirty-five (70%) of the 50 educators who responded ranked seminars as first, second or third choice. Conferences were the second choice, and a total of 28/44 (64%) respondents ranked them as first, second or third choice. Online resources were ranked as a first choice by only one educator, and by only 18/42 (43%) as first, second or third choice. Respondents also identified factors that prevented them from participating in palliative care education activities. Conflict with work schedule was ranked first: of the 45 who responded, 26 (58%) ranked it first. Location of educational activity was ranked first, second or third by 18 (51%) of the 35 who responded, while timing of educational activities was ranked first, second or third by 26 (76%) of the 34 who responded. Language of instruction was ranked first, second or third by 18 (62%) of the 29 who responded. Palliative care content desired Participants responses were divided into physical, psychological, sociocultural and spiritual domains. These are illustrated in a model developed by the Canadian Hospice and Palliative Care Association (CHPCA) to reflect the complex needs of persons living with complex illnesses (CHPCA, 2002) (Figure 1). This model was developed through a national consensus building strategy by the CHPCA, is applicable to all Figure 1. Learning needs identified by educators. Adapted from Domains of issues associated with illness and bereavement (CHPCA, 2002). persons with an illness, and represents the four domains of the needs of the person being cared for (CHPCA, 2002). Figure 1 shows the percentages of participants who expressed a wish for specific content in the selected domains. Only those [Q3: What is those referring to questions, curriculum content, items, needs? please specify] in which more than 50% participants responded have been included. Resources required for the integration of palliative care content into teaching Participants were asked to identity the resources required to integrate palliative care content into their teaching. They were provided with a list of items and asked whether they would use them in their teaching. The results were as follows: audiovisual 34/53 (64%), access to clinical experts 41/53 (77%), case studies 39/53 (74%), online learning 29/53 (55%), practice guidelines 38/53 (72%) and published literature 40/53 (75%). Items ranked first, second or third in descending order were: clinical experts 34/41 (83%); case studies 29/39 (74%), practice guidelines 26/38 (68%), audiovisual material 22/34 (65%), published literature 21/40 (53%) and online learning 15/29 (52%). Discussion At various times during their programme, in almost every context of care, student nurses may encounter individuals and their families facing lifethreatening illness, and/or be involved in the care of those who are imminently dying. It is therefore essential that theory and clinical nurse educators be adequately prepared in EOLC throughout the nursing programme, and have access as necessary to relevant teaching resources and faculty and clinicians with additional EOLC expertise. While perceived learning needs assessments in EOLC have been conducted in many contexts with pre- and post-licensure healthcare students and practising clinicians (Samaroo et al, 1996; Ury et al, 2000), this study is one of the first to examine the learning needs of theory and clinical nurse educators themselves, their attitudes towards caring for the dying, and their basic knowledge in palliative care nursing. The results of the study highlight not only the specific learning needs of educators in EOLC, but also the personal and organizational support and challenges that influence the learning and teaching of this important subject, with specific implications for teaching and faculty development. This information can be used to create feasible, acceptable and meaningful 174 International Journal of Palliative Nursing 2009, Vol 15, No 5 IJPN_15_5_Survey.indd /5/09 13:40:20
6 initiatives for faculty, which will ultimately influence the quality of the nursing education received by students. Identifying specific learning needs The majority of the educators held positive attitudes towards caring for the dying, as evidenced by the scores on the FATCOD, but achieved only average scores in the PCQN. The need to acquire additional specific knowledge in EOLC was also reflected by the topics identified by the participants, which reflected their particular learning needs. Although there does not appear to be a direct relationship between the scores achieved on the FATCOD and PCQN and many of the identified topics, this could be a reflection of the specific subjects addressed by the instruments. The topics are illustrated within a model that reflects the physical, psychological, sociocultural and spiritual dimensions and needs of persons living with complex illnesses (Figure 1). The pie was used as a framework to organize the EOLC topics identified by educators as areas where they required further knowledge and skill, such as cultural influences, the paediatric population, pain management and suffering. The topics address many of the essential aspects of EOLC illustrated by the model. Thus, enhancing nurses knowledge in these areas can contribute to the provision of comprehensive quality care for patients facing lifethreatening illness, regardless of age or context of care. This model can also be used to guide the development of educational interventions for students and educators that reflect a holistic approach to care, which recognizes and integrates the dimensions of the person and the influence of community, care setting and environment on the individual (Hall et al, 2008). Addressing support and barriers Participants identified various personal and organizational support and barriers that influenced their opportunities to engage in palliative care education activities, and also impacted on their teaching of this subject, such as competing demands and lack of time to devote to continuing education activities (Table 3). Consequently, organizers of activities need to take into account [Q4: reworded for clarity is this what you mean?] factors such as work schedules, the location of the activity, timing and the language of instruction. For example, the language of instruction is a major consideration in a school of nursing with French and English programmes. Devoting a faculty professional development day to the teaching of EOLC can bring together educators to address topics related to perceived needs in a desired format, and developing online resources that educators can access at their convenience, are strategies that may be used to address several of the barriers related to time and competing demands. Opportunities to teach student nurses can also be influenced by the reality of crowded curricula, which some participants identified as a barrier to teaching EOLC [Q5: is this what you mean?]. However, opportunities to integrate EOLC into the theory component of many courses do exist. For example, educators teaching students about cardiac and renal disease can also include content related to the role of palliative care when these diseases become end stage, and consult faculty with EOLC expertise for additional advice. Overcrowded curricula and limited time and human and financial resources do indeed present challenges for faculty engaged in teaching and supporting students [Q6: reworded for clarity is this what you mean?]. However, these issues and concerns are not unique to this institution, as many schools of nursing currently face several challenges related to shortages of staff and pressure on clinical facilities and instructional resources to meet increasing student enrolment in response to public and policy demands for more nurses (Oermann, 2004). Nevertheless, from examination of the support for and barriers to teaching EOLC, it is clear that many opportunities exist in the clinical and academic setting. Whether these opportunities are utilized seems to depend on the support that educators perceive they have from, for example, coordinators or the programme in general, in terms of the transparency of EOLC in the curriculum. If the perception is that opportunities for educators to bring EOLC to students are not prevalent, then teachable moments will be missed. Providing opportunities for students Care of the [Q7: inserted for clarity -?OK] dying patient and family are inevitable in the nursing profession. Learning the skills and coping mechanisms is a must for nurses, starting from the undergraduate programme (English programme, part time). Findings indicated that nurse educators appreciated the importance of providing their students with education in EOLC, recognized the possibilities that currently exist to enhance the teaching and learning of this subject, and believed that it was important to identify [Q8: reworded for clarity is this what you mean?] teachable moments. They recommended focusing on The language of instruction is a major consideration in a school of nursing with French and English programmes International Journal of Palliative Nursing 2009, Vol 15, No IJPN_15_5_Survey.indd /5/09 13:40:20
7 Participants identified seminars and conferences as their most preferred learning formats clinical conferences, identifying relevant patients in the clinical setting, encouraging students to communicate with patients and families about dying, allowing students to reflect on their experiences and their emotions, learning from other nurses, performing care after death, and including guest speakers at clinical conferences. Many of these educators teach and supervise students in the clinical area where encounters with death and dying occur. It is during these encounters that students may experience feelings of anxiety, helplessness and incompetence if they feel that they do not have enough knowledge of EOLC to provide care that meets the needs of the dying patient (Cooper and Barnett, 2005). Consequently, clinical professors [Q9: do you mean educators?] play an active and significant role in addressing students experiences and providing appropriate supportive interventions (Cooper and Barnett, 2005; Allchin, 2006). While essential information on EOLC can be acquired in theory classes, students must also have the opportunity to apply their knowledge in the clinical context (Lloyd- Williams and Field, 2002). Findings from previous studies indicate that the arts and humanities can also be used successfully in teaching and learning contexts with nursing and other healthcare students to make it easier for them to share their feelings about the various life situations depicted in the arts and literature, as well as the real-life experiences they evoke (Johnson and Jackson, 2005; Hall et al, 2006a). Additional strategies shown to be effective in supporting student learning of the various dimensions of EOLC include assignments that encourage personal reflection (Dakin, 2003), participation in virtual online modules (Hall et al, 2006b) and the problem-based learning approach (Wong et al, 2001). [Implications for faculty development Participants identified seminars and conferences as their most preferred learning formats, suggesting that interactive face-to-face forums can provide educators with opportunities to discuss teaching experiences and reflect upon their practice. In this study, the online learning format was identified as the least preferred learning method, possibly reflecting participants personal experiences and comfort level with computer technology. Faculty development programmes that involve online learning methods would therefore need to incorporate opportunities to engage in user-friendly online activities that allow them to increase their abilities and confidence (Stodel et al, 2006). Participants also valued learning from other faculty and clinicians with EOLC expertise in the larger community. Experienced faculty can offer guidance and resources to assist and support educators with their individual learning goals and efforts to integrate EOLC into an already established curriculum. Providing opportunities such as workshops and professional development days for nurse educators to reflect upon and discuss teaching experiences and to learn from each other can support the development of a nurse educators community of practice in EOLC. Communities of practice are groups of people who share a concern or a passion for something they do and learn how to do it better as they interact regularly (Wenger, 2006). Membership of this type of network implies a shared interest or commitment to a specific interest, regular engagement in interactive discussions with the purpose of helping and learning from each other, and the development of a shared repertoire of resources, which may include tools, stories, experiences, and strategies for dealing with specific problems (Wenger, 2006). Ideally, educational programmes should consider combining several learning formats and components that can provide educators with opportunities to enhance their knowledge of EOLC, and learn about innovative teaching strategies based on learning objectives and students learning and support needs (Sullivan et al, 2005). Faculty development programmes in EOLC that integrate multiple approaches can enhance the sharing of expertise, knowledge, and ideas around EOLC and pedagogic best practices, and contribute towards a collaborative solution to specific EOLC teaching challenges. Limitations Study participants comprised nurse educators from only one academic institution, consequently the generalizability of the findings is limited. Also, the low response rate of 27% means that the sample was not representative of all the educators: it is possible that only those with a specific interest and/or currently teaching some degree of EOLC content completed the survey. Thirty per cent of respondents indicated that they had previously received education in EOLC, and this may have influenced the nature of their educational needs and their scores on the PCQN and FATCOD. The results should be interpreted with caution owing to the limitations of the instruments. The PCQN, for example, does not cover many of the d o m a i n s o f E O L C, i n c l u d i n g n o n - pharmacological management of symptoms, 176 International Journal of Palliative Nursing 2009, Vol 15, No 5 IJPN_15_5_Survey.indd /5/09 13:40:20
8 comfort care, cultural and ethical issues and the role of the interprofessional team; consequently it may not reflect participants knowledge in these important areas. The FATCOD does not account for important influences on attitudes towards death and dying, such as culture and religion. The survey method of the Educators Educational Needs Questionnaire does not allow in-depth information regarding educators perceptions of their teaching experiences in EOLC, which may have been captured through focus groups and/or individual interviews, to be considered [Q10: reworded (where underlined) for clarity is this what you mean?]. Conclusions are also limited due to unequal representation from the four sites of the programme, and missing data limit the generalizability of the findings. For example, when asked to rank the factors that prevented participation in palliative care educational activities, not all 53 participants responded. Despite these limitations, the researchers were provided with data that reflected the needs of educators for EOLC content, the formats in which they prefer to receive information, and the support and barriers influencing this process. Further research is required to evaluate the outcomes of educational interventions on the knowledge and attitudes of educators, and to examine the influence of faculty development in EOLC on the attitudes, skills and knowledge of nursing students and their perceived competence to care for terminally ill patients and their families. It is also necessary to establish empirical evidence to ascertain how different approaches to teaching EOLC affect patient and family care outcomes (Jordan, 2000). Conclusion At various times during their programme, in almost every context of care, student nurses may encounter individuals and their families facing life-threatening illness, and/or be involved in the care of those who are imminently dying. Consequently, it is essential that theory and clinical nurse educators are adequately prepared to teach and model EOLC throughout the nursing programme, and have access as necessary to relevant teaching resources and faculty and clinicians with additional EOLC expertise. The results of this study highlight the importance of preparing nurse educators to support the theoretical and clinical learning of students in EOLC, and of the need to provide them with the time and relevant resources to develop these competencies. Educators who are able to facilitate and teach EOLC can prepare students to graduate with the fundamental knowledge and skills required by all nurses to meet the multiple challenges involved in providing professional and compassionate care for terminally ill patients and their families across the lifespan and in varied care settings. l IJPN Acknowledgements The authors would like to thank the nurse educators who participated in this study, and Alexis Dmitruk BScN, research assistant, for their help with [Q11: added for clarity is this what you mean?] this project. Allchin L (2006) Caring for the dying: nursing student perspectives. J Hosp Palliat Nurs 8(2): Adriaansen MJM, Frederiks CMA (2002) Design of a postgraduate course in palliative care. J Contin Educ Nurs 33(6): Arber A (2001) Student nurses knowledge of palliative care: evaluation of an education module. Int J Palliat Nurs 7(12): Brajtman S, Fothergill-Bourbonnais F, Casey A, Alain D, Fiset V (2007) Providing direction for change: assessing Canadian nursing students learning needs. Int J Palliat Nurs 13(5): Canadian Hospice Palliative Care Association (CHPCA) (2002) A Model to Guide Hospice Palliative Care: Based on National Principles and Norms of Practice. CHPCA, Ottawa, Canada Canadian Nurses Association (CNA) (2003) List of Competencies for the Canadian Registered Nurse Examination. CNA, Ottawa, Canada Carroll G, Brisson DP, Ross MM, Labbe R (2005) The French version of the Palliative Care Quiz for Nursing (PCQN-F): development and evaluation. J Palliat Care 21(1): Cooper J, Barnett M (2005) Aspects of caring for dying patients which cause anxiety to first year student nurses. Int J Palliat Nurs 11(8): Coyle N (2006) Introduction to palliative nursing care. In: Ferrell BR, Coyle N eds. Textbook of Palliative Nursing. 2nd edn. Oxford University Press, Oxford, UK: 5 11 Dakin C (2003) Encouraging student nurses creative expression about end-of-life experiences. Nurs Educ 28(4): Dillman DA (1978) Mail and Telephone Surveys. John Wiley & Sons, Inc, New York Educating Future Physicians in Palliative and End-of-Life Care (EFPPEC) (2004) Available at: efppec/pages/main.html (accessed 1 May 2009) Ferrell B, Virani R, Grant M, Juarez G (2000) Analysis of palliative care content in nursing textbooks. J Palliat Care 16(1): Frommelt KH (1991) The effects of death education on nurses attitudes toward caring for terminally ill persons and their families. Am J Hosp Palliat Care 8(5): Grant J (2002) Learning needs assessment: assessing the need. BMJ 324(7330): Hall P, Weaver L, Fothergill-Bourbonnais F et al (2006a) Interprofessional education in palliative care: a pilot project using popular literature. J Interprof Care 20(1): 51 9 Hall P, Strasburg K, Willett T et al (2006b) Teaching the concept of total pain: an interprofessional learning experience. J Palliat Care 22(3):193 4 Hall P, Brajtman S, Weaver L (2008) Interprofessional education for collaborative person-centred practice through the humanities. Available at: bins/content page.asp?cid= &lang=1 [Q12: page cannot be found please check] (accessed 10 Sep- Further research is required to evaluate the outcomes of educational interventions on the knowledge and International Journal of Palliative Nursing 2009, Vol 15, No IJPN_15_5_Survey.indd /5/09 13:40:21
9 tember 2008) Haydon E, Roerecke M, Giesbrecht N, Rehm J, Kobus-Matthews M (2006) Chronic Disease in Ontario and Canada: Determinants, Risk Factors and Prevention Priorities. Prepared for the Ontario Chronic Disease Prevention Alliance and the Ontario Public Health Association. Available at: (accessed 30 April 2009) Health Canada (2001) Education for formal caregivers. Workgroup of the Federal Secretariat on Palliative and End-of-Life Care. National Action Planning Workshop on End of-life Care. Available at: ca/hcs-sss/pubs/care-soins/2002-nat-plan-palliat/index_ e.html#2education [Q13: page not found please check] (accessed 6 April 2006) Johnson A, Jackson D (2005) Using the arts and humanities to support learning about loss, suffering and death. Int J Palliat Nurs 11(8): Jordan S (2000) Educational input and patient outcomes: exploring the gap. J Adv Nurs 31(2): Lloyd-Williams M, Field D (2002) Are undergraduate nurses taught palliative care during their training? Nurs Educ Today 22(7): Loftus LA, Thompson E (2002) An evaluation of a palliative care course for generic nurses. Int J Palliat Nurs 8(7): Mallory JL (2003) The impact of a palliative care educational component on attitudes toward care of the dying in undergraduate nursing students. J Prof Nurs 19(5): Manias E, Kristjanson L, Bush T (1997) Palliative care nursing education: Australian and Canadian challenges. Contemp Nurse 6(3-4): 96 7 Meraviglia MG, McGuire C, Chesley DA (2003) Nurses needs for education on cancer and end-of-life care. J Contin Educ Nurs 34(3): Oermann MH (2004) Reflections on undergraduate nursing education: a look to the future. Int J Nurs Educ Scholarsh 1(1): 1 13 Patterson C, Molloy W, Jubelius R, Guyatt GH, Bédard, M (1997 [Q14: 2007 in Abstract - although 1997 everywhere else in text?]) Provisional educational needs of health care providers in three nursing homes in Ontario. J Palliat Care 13(3): Polit D, Beck CT (2004) Nursing Research: Principles and Methods. 7th edn. Lippincott, Williams & Wilkins, Philadelphia, PA, USA Polit D, Hungler BP (1995) Nursing Research: Principles and Methods. 5th edn. JB Lippincott, Philadelphia, PA, USA Ross M, McDonald B, McGuinness J (1996) The palliative care quiz for nursing (PCQN): the development of an instrument to measure nurses knowledge of palliative care. J Adv Nurs 23(1): Samaroo B (1996) Assessing palliative care educational needs of physicians and nurses: results of a survey. J Palliat Care 12(2): 20 2 Sherman DW, Matzo ML, Coyne P, Ferrell BR, Penn B (2004) Teaching symptom management in end-of life care: the didactic content and teaching strategies based on the end-of-life nursing education curriculum. J Nurses Staff Dev 20(3): Statistics Canada (2007) A Portrait of Seniors in Canada. Ministry of Industry. Available at: ca/english/freepub/ xie/ /demographic. htm (accessed 30 April 2009) Stodel EJ, Thompson TL, MacDonald CJ (2006) Furthering our understanding of online learning: learners perspectives on what is missing. Paper presented at the Canadian Association for Distance Learning, Montreal, Quebec, Canada Sullivan AM, Lakoma MD, Billings A, Peters AS, Block SD; PCEP Core Faculty (2005) Teaching and learning end-oflife care: evaluation of a faculty development program in palliative care. Acad Med 80(7): Ury WA, Reznich CB, Weber CM (2000) A needs assessment for a palliative care curriculum. J Pain Symptom Manage 20(6): Vachon M (2001) The nurse s role: the world of palliative care nursing. In: Ferrell B, Coyle N eds. Textbook of Palliative Nursing. Oxford University Press, Oxford, UK: Wenger E (2006) Communities of Practice: A Brief Introduction. Available at: (accessed 30 April 2009) White KR, Coyne PJ, Patel UB (2001) Are nurses adequately prepared for end-of-life care? J Nurs Scholarsh 33(2): World Health Organization (2004) Palliative Care: The Solid Facts. Available at: (accessed 30 April 2009) Wong F, Lee W, Mok E ( 2001) Educating nurses to care for the dying in Hong Kong: a problem-based learning approach. Cancer Nurs 24(2): International Journal of Palliative Nursing 2009, Vol 15, No 5 IJPN_15_5_Survey.indd /5/09 13:40:21
OUR CHALLENGE. (Ferrell, 2001, p. xiii)
 OUR CHALLENGE The new realities of our world challenge nurses to provide the most competent, expert, evidencebased care provided in a way that embodies compassion, respect for dignity, and an appreciation
OUR CHALLENGE The new realities of our world challenge nurses to provide the most competent, expert, evidencebased care provided in a way that embodies compassion, respect for dignity, and an appreciation
Hospice Palliative Care
 Position Statement Hospice Palliative Care A Position Statement September 2011 HOSPICE PALLIATIVE CARE: A SEPTEMBER 2011 i Approved by the College and Association of Registered Nurses of Alberta () Provincial
Position Statement Hospice Palliative Care A Position Statement September 2011 HOSPICE PALLIATIVE CARE: A SEPTEMBER 2011 i Approved by the College and Association of Registered Nurses of Alberta () Provincial
PALLIATIVE CARE COMPETENCIES 2. Developing Palliative Care Competencies for the Education of Canadian Nurses
 PALLIATIVE CARE COMPETENCIES 2 Developing Palliative Care Competencies for the Education of Canadian Nurses During their careers, most nurses are exposed to suffering and death, and to those requiring
PALLIATIVE CARE COMPETENCIES 2 Developing Palliative Care Competencies for the Education of Canadian Nurses During their careers, most nurses are exposed to suffering and death, and to those requiring
Palliative and End-of-Life Care
 Position Statement Palliative and End-of-Life Care A Position Statement Month Year PALLIATIVE AND END-OF-LIFE CARE MONTH YEAR i Approved by the College and Association of Registered Nurses of Alberta ()
Position Statement Palliative and End-of-Life Care A Position Statement Month Year PALLIATIVE AND END-OF-LIFE CARE MONTH YEAR i Approved by the College and Association of Registered Nurses of Alberta ()
Palliative Care Knowledge among Bachelors of Science Nursing Students
 Kennesaw State University DigitalCommons@Kennesaw State University Dissertations, Theses and Capstone Projects Fall 2013 Palliative Care Knowledge among Bachelors of Science Nursing Students Amy Pope Kennesaw
Kennesaw State University DigitalCommons@Kennesaw State University Dissertations, Theses and Capstone Projects Fall 2013 Palliative Care Knowledge among Bachelors of Science Nursing Students Amy Pope Kennesaw
QUALITY MEASURES WHAT S ON THE HORIZON
 QUALITY MEASURES WHAT S ON THE HORIZON The Hospice Quality Reporting Program (HQRP) November 2013 Plan for the Day Discuss the implementation of the Hospice Item Set (HIS) Discuss the implementation of
QUALITY MEASURES WHAT S ON THE HORIZON The Hospice Quality Reporting Program (HQRP) November 2013 Plan for the Day Discuss the implementation of the Hospice Item Set (HIS) Discuss the implementation of
Perceptions of the role of the hospital palliative care team
 NTResearch Perceptions of the role of the hospital palliative care team Authors Catherine Oakley, BSc, RGN, is Macmillan lead cancer nurse, St George s Hospital NHS Trust, London; Kim Pennington, BSc,
NTResearch Perceptions of the role of the hospital palliative care team Authors Catherine Oakley, BSc, RGN, is Macmillan lead cancer nurse, St George s Hospital NHS Trust, London; Kim Pennington, BSc,
Employers are essential partners in monitoring the practice
 Innovation Canadian Nursing Supervisors Perceptions of Monitoring Discipline Orders: Opportunities for Regulator- Employer Collaboration Farah Ismail, MScN, LLB, RN, FRE, and Sean P. Clarke, PhD, RN, FAAN
Innovation Canadian Nursing Supervisors Perceptions of Monitoring Discipline Orders: Opportunities for Regulator- Employer Collaboration Farah Ismail, MScN, LLB, RN, FRE, and Sean P. Clarke, PhD, RN, FAAN
Patients satisfaction with mental health nursing interventions in the management of anxiety: Results of a questionnaire study.
 d AUSTRALIAN CATHOLIC UNIVERSITY Patients satisfaction with mental health nursing interventions in the management of anxiety: Results of a questionnaire study. Sue Webster sue.webster@acu.edu.au 1 Background
d AUSTRALIAN CATHOLIC UNIVERSITY Patients satisfaction with mental health nursing interventions in the management of anxiety: Results of a questionnaire study. Sue Webster sue.webster@acu.edu.au 1 Background
POSTGRADUATE PROSPECTUS HEALTH AND SOCIAL SERVICES
 POSTGRADUATE PROSPECTUS HEALTH AND SOCIAL SERVICES Masters Postgraduate Diploma Postgraduate Certificate 0800 944 847 info@whitireia.ac.nz www.whitireia.ac.nz 0800 935 832 info@weltec.ac.nz www.weltec.ac.nz
POSTGRADUATE PROSPECTUS HEALTH AND SOCIAL SERVICES Masters Postgraduate Diploma Postgraduate Certificate 0800 944 847 info@whitireia.ac.nz www.whitireia.ac.nz 0800 935 832 info@weltec.ac.nz www.weltec.ac.nz
Student nurses experience of, and attitudes toward care of the dying: a
 Student nurses experience of, and attitudes toward care of the dying: a cross sectional study Abstract Background Nurses are the professional group with the greatest contact with those at the end of life
Student nurses experience of, and attitudes toward care of the dying: a cross sectional study Abstract Background Nurses are the professional group with the greatest contact with those at the end of life
Path to Transformation Concept Paper Comments and Recommendations. Palliative Care Community Partners (PCCP)
 Path to Transformation Concept Paper Comments and Recommendations Palliative Care Community Partners (PCCP) c/o Hospice Care of America, Inc., 3815 N Mulford Rd, Rockford, IL / (815)316-2697 As part of
Path to Transformation Concept Paper Comments and Recommendations Palliative Care Community Partners (PCCP) c/o Hospice Care of America, Inc., 3815 N Mulford Rd, Rockford, IL / (815)316-2697 As part of
Course Syllabus. RNSG 1193 End of Life Issues. Course Syllabus. RNSG 1193 Special Topics. End of Life. Revision Date: Fall,2013
 Course Syllabus RNSG 1193 Special Topics End of Life Revision Date: Fall,2013 Course Syllabus RNSG 1193 End of Life Issues Catalog Description: Lecture Hrs. 1, Lab Hrs. 0 This class explores the issues
Course Syllabus RNSG 1193 Special Topics End of Life Revision Date: Fall,2013 Course Syllabus RNSG 1193 End of Life Issues Catalog Description: Lecture Hrs. 1, Lab Hrs. 0 This class explores the issues
Palliative Care Competencies for Occupational Therapists
 Principles of Palliative Care Demonstrates an understanding of the philosophy of palliative care Demonstrates an understanding that a palliative approach to care starts early in the trajectory of a progressive
Principles of Palliative Care Demonstrates an understanding of the philosophy of palliative care Demonstrates an understanding that a palliative approach to care starts early in the trajectory of a progressive
Canadian Social Work Competencies for Hospice Palliative Care: A Framework to Guide Education and Practice at the Generalist and Specialist Levels
 Canadian Social Work Competencies for Hospice Palliative Care: A Framework to Guide Education and Practice at the Generalist and Specialist Levels 2008 Bosma, H, Johnston, M, Cadell S, Wainwright, W, Abernathy
Canadian Social Work Competencies for Hospice Palliative Care: A Framework to Guide Education and Practice at the Generalist and Specialist Levels 2008 Bosma, H, Johnston, M, Cadell S, Wainwright, W, Abernathy
Providing Hospice Care in a SNF/NF or ICF/IID facility
 Providing Hospice Care in a SNF/NF or ICF/IID facility Education program Insert name of your hospice program Insert your logo Objectives Review the philosophy of hospice care and discuss what hospice care
Providing Hospice Care in a SNF/NF or ICF/IID facility Education program Insert name of your hospice program Insert your logo Objectives Review the philosophy of hospice care and discuss what hospice care
School of Nursing Philosophy (AASN/BSN/MSN/DNP)
 School of Nursing Mission The mission of the School of Nursing is to educate, enhance and enrich students for evolving professional nursing practice. The core values: The School of Nursing values the following
School of Nursing Mission The mission of the School of Nursing is to educate, enhance and enrich students for evolving professional nursing practice. The core values: The School of Nursing values the following
Relationship between Organizational Climate and Nurses Job Satisfaction in Bangladesh
 Relationship between Organizational Climate and Nurses Job Satisfaction in Bangladesh Abdul Latif 1, Pratyanan Thiangchanya 2, Tasanee Nasae 3 1. Master in Nursing Administration Program, Faculty of Nursing,
Relationship between Organizational Climate and Nurses Job Satisfaction in Bangladesh Abdul Latif 1, Pratyanan Thiangchanya 2, Tasanee Nasae 3 1. Master in Nursing Administration Program, Faculty of Nursing,
Hospice Isle of Man Education Prospectus 2018
 Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
Hospice Isle of Man Education Prospectus 2018 Leading the Way in Palliative Care Introduction The need for palliative and end of life care is changing, with increasing demands and complexity for patients
National Standards Assessment Program. Quality Report
 National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
PG snapshot Nursing Special Report. The Role of Workplace Safety and Surveillance Capacity in Driving Nurse and Patient Outcomes
 PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
E-Learning Module B: Introduction to Hospice Palliative Care
 E-Learning Module B: Introduction to Hospice Palliative Care This Module requires the learner to have read Chapter 2 of the Fundamentals Program Guide and the other required readings associated with the
E-Learning Module B: Introduction to Hospice Palliative Care This Module requires the learner to have read Chapter 2 of the Fundamentals Program Guide and the other required readings associated with the
RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE. INSIDE Expert advice on HIV disclosure. The end of an era in Afghanistan
 Publications Mail Agreement Number 40062599 NOVEMBER 2013 VOLUME 109 NUMBER 9 RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE INSIDE Expert advice on HIV disclosure The end of an era in Afghanistan
Publications Mail Agreement Number 40062599 NOVEMBER 2013 VOLUME 109 NUMBER 9 RIGHTS OF PASSAGE A NEW APPROACH TO PALLIATIVE CARE INSIDE Expert advice on HIV disclosure The end of an era in Afghanistan
Nursing Children and Young People Storyboarding as an aid to learning about death situations in children's nurse education
 Nursing Children and Young People Storyboarding as an aid to learning about death situations in children's nurse education --Manuscript Draft-- Manuscript Number: Article Type: Full Title: Corresponding
Nursing Children and Young People Storyboarding as an aid to learning about death situations in children's nurse education --Manuscript Draft-- Manuscript Number: Article Type: Full Title: Corresponding
The attitude of nurses towards inpatient aggression in psychiatric care Jansen, Gradus
 University of Groningen The attitude of nurses towards inpatient aggression in psychiatric care Jansen, Gradus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
University of Groningen The attitude of nurses towards inpatient aggression in psychiatric care Jansen, Gradus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you
With Graduate Student Preconference May 27 th, 2017
 CSSHE/SCEES Annual Conference: May 27 th to 30 th, 2017 With Graduate Student Preconference May 27 th, 2017 The Canadian Society for the Study of Higher Education (CSSHE) invites you to participate in
CSSHE/SCEES Annual Conference: May 27 th to 30 th, 2017 With Graduate Student Preconference May 27 th, 2017 The Canadian Society for the Study of Higher Education (CSSHE) invites you to participate in
STUDY PLAN Master Degree In Clinical Nursing/Critical Care (Thesis )
 STUDY PLAN Master Degree In Clinical Nursing/Critical Care (Thesis ) I. GENERAL RULES AND CONDITIONS:- 1. This plan conforms to the valid regulations of the programs of graduate studies. 2. Areas of specialty
STUDY PLAN Master Degree In Clinical Nursing/Critical Care (Thesis ) I. GENERAL RULES AND CONDITIONS:- 1. This plan conforms to the valid regulations of the programs of graduate studies. 2. Areas of specialty
Palliative Care. Care for Adults With a Progressive, Life-Limiting Illness
 Palliative Care Care for Adults With a Progressive, Life-Limiting Illness Summary This quality standard addresses palliative care for people who are living with a serious, life-limiting illness, and for
Palliative Care Care for Adults With a Progressive, Life-Limiting Illness Summary This quality standard addresses palliative care for people who are living with a serious, life-limiting illness, and for
Original Article Rural generalist nurses perceptions of the effectiveness of their therapeutic interventions for patients with mental illness
 Blackwell Science, LtdOxford, UKAJRAustralian Journal of Rural Health1038-52822005 National Rural Health Alliance Inc. August 2005134205213Original ArticleRURAL NURSES and CARING FOR MENTALLY ILL CLIENTSC.
Blackwell Science, LtdOxford, UKAJRAustralian Journal of Rural Health1038-52822005 National Rural Health Alliance Inc. August 2005134205213Original ArticleRURAL NURSES and CARING FOR MENTALLY ILL CLIENTSC.
Interventions to help the family cope
 Family issues and sexual problems in cardiovascular disease Interventions to help the family cope Anna Strömberg, RN, PhD, NFESC, FAAN Professor and head of Division of Nursing, Department of Medical and
Family issues and sexual problems in cardiovascular disease Interventions to help the family cope Anna Strömberg, RN, PhD, NFESC, FAAN Professor and head of Division of Nursing, Department of Medical and
Advance Care Planning: Goals of Care - Calgary Zone
 Advance Care Planning: Goals of Care - Calgary Zone LOOKING BACK AND MOVING FORWARD PRESENTERS: BEV BERG, COORDINATOR CHANDRA VIG, EDUCATION CONSULTANT TRACY LYNN WITYK-MARTIN, QUALITY IMPROVEMENT SPECIALIST
Advance Care Planning: Goals of Care - Calgary Zone LOOKING BACK AND MOVING FORWARD PRESENTERS: BEV BERG, COORDINATOR CHANDRA VIG, EDUCATION CONSULTANT TRACY LYNN WITYK-MARTIN, QUALITY IMPROVEMENT SPECIALIST
INSTRUCTIONAL DESIGN AND ASSESSMENT An Interdisciplinary Approach to Introducing Professionalism
 INSTRUCTIONAL DESIGN AND ASSESSMENT An Interdisciplinary Approach to Introducing Professionalism Bonnie Brehm, PhD, a Phyllis Breen, MA, b Bethanne Brown, PharmD, c Lisa Long, MS, a Rebecca Smith, MEd,
INSTRUCTIONAL DESIGN AND ASSESSMENT An Interdisciplinary Approach to Introducing Professionalism Bonnie Brehm, PhD, a Phyllis Breen, MA, b Bethanne Brown, PharmD, c Lisa Long, MS, a Rebecca Smith, MEd,
Understanding the Palliative Care Needs of Older Adults & Their Family Caregivers
 Understanding the Palliative Care Needs of Older Adults & Their Family Caregivers Dr. Genevieve Thompson, RN PhD Assistant Professor, Faculty of Nursing, University of Manitoba genevieve_thompson@umanitoba.ca
Understanding the Palliative Care Needs of Older Adults & Their Family Caregivers Dr. Genevieve Thompson, RN PhD Assistant Professor, Faculty of Nursing, University of Manitoba genevieve_thompson@umanitoba.ca
End-of-Life Care Action Plan
 The Provincial End-of-Life Care Action Plan for British Columbia Priorities and Actions for Health System and Service Redesign Ministry of Health March 2013 ii The Provincial End-of-Life Care Action Plan
The Provincial End-of-Life Care Action Plan for British Columbia Priorities and Actions for Health System and Service Redesign Ministry of Health March 2013 ii The Provincial End-of-Life Care Action Plan
Copyright American Psychological Association INTRODUCTION
 INTRODUCTION No one really wants to go to a nursing home. In fact, as they age, many people will say they don t want to be put away in a nursing home and will actively seek commitments from their loved
INTRODUCTION No one really wants to go to a nursing home. In fact, as they age, many people will say they don t want to be put away in a nursing home and will actively seek commitments from their loved
Did You Know? The Strategic and Compassionate Employer: How Compassionate Care Leave Policies can Improve Employee Retention and Engagement
 The Strategic and Compassionate Employer: How Compassionate Care Leave Policies can Improve Employee Retention and Engagement PRESENTATION TO THE HRPA 2015 CONFERENCE SHARON BAXTER, EXECUTIVE DIRECTOR,
The Strategic and Compassionate Employer: How Compassionate Care Leave Policies can Improve Employee Retention and Engagement PRESENTATION TO THE HRPA 2015 CONFERENCE SHARON BAXTER, EXECUTIVE DIRECTOR,
J M Kyrkjebø, T A Hanssen, B Ø Haugland
 204 Papers University of Bergen, Faculty of Psychology, N-5020 Bergen, rway J M Kyrkjebø, research fellow Medical Department, Haukeland University Hospital, Bergen, rway T A Hanssen, research fellow Betanien
204 Papers University of Bergen, Faculty of Psychology, N-5020 Bergen, rway J M Kyrkjebø, research fellow Medical Department, Haukeland University Hospital, Bergen, rway T A Hanssen, research fellow Betanien
Presented by: Marilyn Stapleton, PhD, RN Lisa Bagdan, MPS, RN June 2, 2010 QSEN National Forum
 Assessment of Quality and Safety Education in Nursing: A New York State Perspective Presented by: Marilyn Stapleton, PhD, RN Lisa Bagdan, MPS, RN June 2, 2010 QSEN National Forum Introduction Project Team:
Assessment of Quality and Safety Education in Nursing: A New York State Perspective Presented by: Marilyn Stapleton, PhD, RN Lisa Bagdan, MPS, RN June 2, 2010 QSEN National Forum Introduction Project Team:
End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces.
 End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces. Terms Definitions End of Life Care To assist persons who
End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces. Terms Definitions End of Life Care To assist persons who
13 th Hong Kong Palliative Care Symposium
 Sponsored by TUYF Charitable Trust, the symposium was held on 22 October 2016. There were over 430 healthcare professionals from various clinical settings to attend this symposium. We are honoured to have
Sponsored by TUYF Charitable Trust, the symposium was held on 22 October 2016. There were over 430 healthcare professionals from various clinical settings to attend this symposium. We are honoured to have
2014 ONS Distinguished Researcher Award Susan C. McMillan
 Susan McMillan, PhD, ARNP, FAAN, (left) receiving the 2014 ONS Distinguished Researcher Award from Paula Rieger, RN, MSN, CAE, FAAN, chief executive officer, ONS, at ONS annual Congress, May 1, 2014. 2014
Susan McMillan, PhD, ARNP, FAAN, (left) receiving the 2014 ONS Distinguished Researcher Award from Paula Rieger, RN, MSN, CAE, FAAN, chief executive officer, ONS, at ONS annual Congress, May 1, 2014. 2014
Final Report ALL IRELAND. Palliative Care Senior Nurses Network
 Final Report ALL IRELAND Palliative Care Senior Nurses Network May 2016 FINAL REPORT Phase II All Ireland Palliative Care Senior Nurse Network Nursing Leadership Impacting Policy and Practice 1 Rationale
Final Report ALL IRELAND Palliative Care Senior Nurses Network May 2016 FINAL REPORT Phase II All Ireland Palliative Care Senior Nurse Network Nursing Leadership Impacting Policy and Practice 1 Rationale
second year level nursing courses (NURS 210, NURS 250, NURS 251, NURS 252 and NURS 360) and admission to program.
 Nursing (NURS) 1 Nursing (NURS) NURS 189. Skills for Academic Success. 1 Credit. This course is designed to ease the transition for new students at NDSU. Students will be introduced to campus and learn
Nursing (NURS) 1 Nursing (NURS) NURS 189. Skills for Academic Success. 1 Credit. This course is designed to ease the transition for new students at NDSU. Students will be introduced to campus and learn
PAHT strategy for End of Life Care for adults
 PAHT strategy for End of Life Care for adults 2017-2020 End of Life Care encompasses all care given to patients who are approaching the end of their life and following death, and may be delivered on any
PAHT strategy for End of Life Care for adults 2017-2020 End of Life Care encompasses all care given to patients who are approaching the end of their life and following death, and may be delivered on any
Faculty of Health Studies. Programme Specification. Programme title: MSc Professional Healthcare Practice. Academic Year:
 Faculty of Health Studies Programme Specification Programme title: MSc Professional Healthcare Practice Academic Year: 2018-19 Degree Awarding Body: Partner(s), delivery organisation or support provider
Faculty of Health Studies Programme Specification Programme title: MSc Professional Healthcare Practice Academic Year: 2018-19 Degree Awarding Body: Partner(s), delivery organisation or support provider
Mississauga Halton Local Health Integration Network (LHIN) Francophone Community Consultation - May 9, 2009
 Mississauga Halton Local Health Integration Network (LHIN) Francophone Community Consultation - May 9, 2009 The LHIN invited representatives of the francophone community in the LHIN area to discuss the
Mississauga Halton Local Health Integration Network (LHIN) Francophone Community Consultation - May 9, 2009 The LHIN invited representatives of the francophone community in the LHIN area to discuss the
Challenging The 2015 PH Guidelines - comments from the Nurses. Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust
 Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
NURS - Nursing. NURSING Courses
 NURS - Nursing NURSING Courses NURS 304. Principles of Practice: Foundations of Health Assessment. 3 This didactic and laboratory course emphasizes the assessment phase of the nursing process. Supervised
NURS - Nursing NURSING Courses NURS 304. Principles of Practice: Foundations of Health Assessment. 3 This didactic and laboratory course emphasizes the assessment phase of the nursing process. Supervised
Prevalence of Stress and Coping Mechanism Among Staff Nurses of Intensive Care Unit in a Selected Hospital
 International Journal of Neurosurgery 2018; 2(1): 8-12 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.12 Prevalence of Stress and Coping Mechanism Among Staff Nurses of Intensive
International Journal of Neurosurgery 2018; 2(1): 8-12 http://www.sciencepublishinggroup.com/j/ijn doi: 10.11648/j.ijn.20180201.12 Prevalence of Stress and Coping Mechanism Among Staff Nurses of Intensive
Advance Care Planning Exploratory Project. Rhonda Wiering, MSN, RN,BC, LNHA Regional Director, Quality Initiatives Avera Health October 18, 2012
 Advance Care Planning Exploratory Project Rhonda Wiering, MSN, RN,BC, LNHA Regional Director, Quality Initiatives Avera Health October 18, 2012 Agenda Overview of the Advance Care Planning Exploration
Advance Care Planning Exploratory Project Rhonda Wiering, MSN, RN,BC, LNHA Regional Director, Quality Initiatives Avera Health October 18, 2012 Agenda Overview of the Advance Care Planning Exploration
Nurses Knowledge of Pain in the Elderly
 Vol. 21 No. 4 April 2001 Journal of Pain and Symptom Management 317 Original Article Nurses Knowledge of Pain in the Elderly Rod Sloman, PhD, RN, Maureen Ahern, MHP, RN, Alex Wright, MappSc(res), RN, and
Vol. 21 No. 4 April 2001 Journal of Pain and Symptom Management 317 Original Article Nurses Knowledge of Pain in the Elderly Rod Sloman, PhD, RN, Maureen Ahern, MHP, RN, Alex Wright, MappSc(res), RN, and
Make changes to palliative and end-of-life care in Canada
 CNA Webinar Series: Progress in Practice Make changes to palliative and end-of-life care in Canada Louise Hanvey Louise Hanvey Consulting March 10, 2014 Canadian Nurses Association, 2012 Jill Norman, RN,
CNA Webinar Series: Progress in Practice Make changes to palliative and end-of-life care in Canada Louise Hanvey Louise Hanvey Consulting March 10, 2014 Canadian Nurses Association, 2012 Jill Norman, RN,
CanMEDS- Family Medicine. Working Group on Curriculum Review
 CanMEDS- Family Medicine Working Group on Curriculum Review October 2009 1 CanMEDS-Family Medicine Working Group on Curriculum Review October 2009 Members: David Tannenbaum, Chair Jill Konkin Ean Parsons
CanMEDS- Family Medicine Working Group on Curriculum Review October 2009 1 CanMEDS-Family Medicine Working Group on Curriculum Review October 2009 Members: David Tannenbaum, Chair Jill Konkin Ean Parsons
ACUTE CARE NURSES SELF-REPORTED COMPETENCE IN PALLIATIVE CARE. Chelsi Rae Hayter
 ACUTE CARE NURSES SELF-REPORTED COMPETENCE IN PALLIATIVE CARE by Chelsi Rae Hayter A thesis submitted in partial fulfillment of the requirement for the degree of Master of Nursing MONTANA STATE UNIVERSITY
ACUTE CARE NURSES SELF-REPORTED COMPETENCE IN PALLIATIVE CARE by Chelsi Rae Hayter A thesis submitted in partial fulfillment of the requirement for the degree of Master of Nursing MONTANA STATE UNIVERSITY
Shifting Public Perceptions of Doctors and Health Care
 Shifting Public Perceptions of Doctors and Health Care FINAL REPORT Submitted to: The Association of Faculties of Medicine of Canada EKOS RESEARCH ASSOCIATES INC. February 2011 EKOS RESEARCH ASSOCIATES
Shifting Public Perceptions of Doctors and Health Care FINAL REPORT Submitted to: The Association of Faculties of Medicine of Canada EKOS RESEARCH ASSOCIATES INC. February 2011 EKOS RESEARCH ASSOCIATES
Nursing perspectives on palliative care 2015
 Perspective Nursing perspectives on palliative care 2015 Margaret I. Fitch 1, Monika C. Fliedner 2, Margaret O Connor 3 1 Bloomberg Faculty of Nursing, University of Toronto, Toronto, Canada; 2 Oncology/Palliative
Perspective Nursing perspectives on palliative care 2015 Margaret I. Fitch 1, Monika C. Fliedner 2, Margaret O Connor 3 1 Bloomberg Faculty of Nursing, University of Toronto, Toronto, Canada; 2 Oncology/Palliative
Teaching Compassion: Incorporating Jean Watson s Caritas Processes into a Care at the End of Life Course for Senior Nursing Students
 International Journal of Caring Sciences September-December 2017 Volume 10 Issue 3 Page 1113 Original Article Teaching Compassion: Incorporating Jean Watson s Caritas Processes into a Care at the End of
International Journal of Caring Sciences September-December 2017 Volume 10 Issue 3 Page 1113 Original Article Teaching Compassion: Incorporating Jean Watson s Caritas Processes into a Care at the End of
The Consolidation Practicum
 Transitioning 4 th year nursing students into intensive care using a consolidation experience: How it works By Frances Fothergill Bourbonnais, RN PhD, School of Nursing, University of Ottawa and, Sue Malone
Transitioning 4 th year nursing students into intensive care using a consolidation experience: How it works By Frances Fothergill Bourbonnais, RN PhD, School of Nursing, University of Ottawa and, Sue Malone
Nursing Awards of Excellence Awards & Criteria
 Nursing Awards of Excellence Awards & Criteria Table of Contents Lifetime Achievement... 2 Excellence in Nursing Administration... 3 Excellence in Advancing Nursing Knowledge & Research... 4 Excellence
Nursing Awards of Excellence Awards & Criteria Table of Contents Lifetime Achievement... 2 Excellence in Nursing Administration... 3 Excellence in Advancing Nursing Knowledge & Research... 4 Excellence
Transdisciplinary Care: Opportunities and Challenges for Behavioral Health Providers
 Transdisciplinary Care: Opportunities and Challenges for Behavioral Health Providers Virna Little Journal of Health Care for the Poor and Underserved, Volume 21, Number 4, November 2010, pp. 1103-1107
Transdisciplinary Care: Opportunities and Challenges for Behavioral Health Providers Virna Little Journal of Health Care for the Poor and Underserved, Volume 21, Number 4, November 2010, pp. 1103-1107
Determinants and Outcomes of Privately and Publicly Financed Home-Based Nursing
 Determinants and Outcomes of Privately and Publicly Financed Home-Based Nursing Peter C. Coyte, PhD Denise Guerriere, PhD Patricia McKeever, PhD Funding Provided by: Canadian Health Services Research Foundation
Determinants and Outcomes of Privately and Publicly Financed Home-Based Nursing Peter C. Coyte, PhD Denise Guerriere, PhD Patricia McKeever, PhD Funding Provided by: Canadian Health Services Research Foundation
Best Practice to Achieving Personhood in End-of-Life in Long-term Care Facilities
 Best Practice to Achieving Personhood in End-of-Life in Long-term Care Facilities Lou Vivian W. Q. Fang Christine M. S. Kong Shirley S. T. November 30, 2015 Contents Conserving Dignity at the End of Life
Best Practice to Achieving Personhood in End-of-Life in Long-term Care Facilities Lou Vivian W. Q. Fang Christine M. S. Kong Shirley S. T. November 30, 2015 Contents Conserving Dignity at the End of Life
Talking to Your Family About End-of-Life Care
 Talking to Your Family About End-of-Life Care Sharing in significant life events during both happy and sad occasions often strengthens our bond with family and close friends. We plan for weddings, the
Talking to Your Family About End-of-Life Care Sharing in significant life events during both happy and sad occasions often strengthens our bond with family and close friends. We plan for weddings, the
Payment Reforms to Improve Care for Patients with Serious Illness
 Payment Reforms to Improve Care for Patients with Serious Illness Discussion Draft March 2017 Payment Reforms to Improve Care for Patients with Serious Illness Page 2 PAYMENT REFORMS TO IMPROVE CARE FOR
Payment Reforms to Improve Care for Patients with Serious Illness Discussion Draft March 2017 Payment Reforms to Improve Care for Patients with Serious Illness Page 2 PAYMENT REFORMS TO IMPROVE CARE FOR
Advance Care Planning: the Clients Perspectives
 Dr. Yvonne Yi-wood Mak; Bradbury Hospice / Pamela Youde Nethersole Eastern Hospital Correspondence: fangmyw@yahoo.co.uk Definition Advance care planning [ACP] is a process of discussion among the patient,
Dr. Yvonne Yi-wood Mak; Bradbury Hospice / Pamela Youde Nethersole Eastern Hospital Correspondence: fangmyw@yahoo.co.uk Definition Advance care planning [ACP] is a process of discussion among the patient,
JENNIFER A. SPECHT, PHD, RN
 MENTORING RELATIONSHIPS AND THE LEVELS OF ROLE CONFLICT AND ROLE AMBIGUITY EXPERIENCED BY NOVICE NURSING FACULTY JENNIFER A. SPECHT, PHD, RN This study explored the effect of mentoring on the levels of
MENTORING RELATIONSHIPS AND THE LEVELS OF ROLE CONFLICT AND ROLE AMBIGUITY EXPERIENCED BY NOVICE NURSING FACULTY JENNIFER A. SPECHT, PHD, RN This study explored the effect of mentoring on the levels of
One Chance to Get it Right:
 One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
Patient Reference Guide. Palliative Care. Care for Adults
 Patient Reference Guide Palliative Care Care for Adults Quality standards outline what high-quality care looks like. They focus on topics where there are large variations in how care is delivered, or where
Patient Reference Guide Palliative Care Care for Adults Quality standards outline what high-quality care looks like. They focus on topics where there are large variations in how care is delivered, or where
KNOWLEDGE, BACKGROUND, AND PERCEPTIONS: PAIN AND PALLIATIVE CARE GIVING RESEARCH PROPOSAL SUBMITTED TO THE GRADUATE SCHOOL
 KNOWLEDGE, BACKGROUND, AND PERCEPTIONS: PAIN AND PALLIATIVE CARE GIVING RESEARCH PROPOSAL SUBMITTED TO THE GRADUATE SCHOOL IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE MASTERS OF SCIENCE BY
KNOWLEDGE, BACKGROUND, AND PERCEPTIONS: PAIN AND PALLIATIVE CARE GIVING RESEARCH PROPOSAL SUBMITTED TO THE GRADUATE SCHOOL IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE MASTERS OF SCIENCE BY
Nursing (NURS) Courses. Nursing (NURS) 1
 Nursing (NURS) 1 Nursing (NURS) Courses NURS 2012. Nursing Informatics. 2 This course focuses on how information technology is used in the health care system. The course describes how nursing informatics
Nursing (NURS) 1 Nursing (NURS) Courses NURS 2012. Nursing Informatics. 2 This course focuses on how information technology is used in the health care system. The course describes how nursing informatics
PERCEPTIONS OF CLINICAL PLACEMENT EXPERIENCE AMONG DIPLOMA NURSING STUDENTS
 PERCEPTIONS OF CLINICAL PLACEMENT EXPERIENCE AMONG DIPLOMA NURSING STUDENTS * Leong Sui Wan & Chan Siok Gim Kolej Kejururawatan Kubang Kerian Open University Malaysia, Kelantan *Corresponding Author Email:
PERCEPTIONS OF CLINICAL PLACEMENT EXPERIENCE AMONG DIPLOMA NURSING STUDENTS * Leong Sui Wan & Chan Siok Gim Kolej Kejururawatan Kubang Kerian Open University Malaysia, Kelantan *Corresponding Author Email:
Unit 301 Understand how to provide support when working in end of life care Supporting information
 Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Introducing Telehealth to Pre-licensure Nursing Students
 DNP Forum Volume 1 Issue 1 Article 2 2015 Introducing Telehealth to Pre-licensure Nursing Students Dwayne F. More University of Texas Medical Branch, dfmore@utmb.edu Follow this and additional works at:
DNP Forum Volume 1 Issue 1 Article 2 2015 Introducing Telehealth to Pre-licensure Nursing Students Dwayne F. More University of Texas Medical Branch, dfmore@utmb.edu Follow this and additional works at:
Leadership in Palliative Care: Strategies for APNs
 Leadership in Palliative Care: Strategies for APNs April 20, 2018 Lyn Ceronsky DNP, GNP, CHPCA, FPCN lcerons1@fairview.org System Director, Palliative Care Director, Fairview Palliative Care Leadership
Leadership in Palliative Care: Strategies for APNs April 20, 2018 Lyn Ceronsky DNP, GNP, CHPCA, FPCN lcerons1@fairview.org System Director, Palliative Care Director, Fairview Palliative Care Leadership
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP
 Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
GLASGOW CALEDONIAN UNIVERSITY
 GLASGOW CALEDONIAN UNIVERSITY PROGRAMME SPECIFICATION PRO-FORMA (PSP) 1. GENERAL INFORMATION 1. Programme Title: BSc Nursing Studies: Adult Nursing; Child Nursing; Learning Disability Nursing; Mental Health
GLASGOW CALEDONIAN UNIVERSITY PROGRAMME SPECIFICATION PRO-FORMA (PSP) 1. GENERAL INFORMATION 1. Programme Title: BSc Nursing Studies: Adult Nursing; Child Nursing; Learning Disability Nursing; Mental Health
Nursing student experiences of death and dying during a palliative care clinical placement: Teaching and learning implications
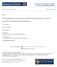 University of Notre Dame Australia ResearchOnline@ND Nursing Conference Papers School of Nursing 2014 Nursing student experiences of death and dying during a palliative care clinical placement: Teaching
University of Notre Dame Australia ResearchOnline@ND Nursing Conference Papers School of Nursing 2014 Nursing student experiences of death and dying during a palliative care clinical placement: Teaching
Factors Influencing Acceptance of Electronic Health Records in Hospitals 1
 Factors Influencing Acceptance of Electronic Health Records in Hospitals 1 Factors Influencing Acceptance of Electronic Health Records in Hospitals by Melinda A. Wilkins, PhD, RHIA Abstract The study s
Factors Influencing Acceptance of Electronic Health Records in Hospitals 1 Factors Influencing Acceptance of Electronic Health Records in Hospitals by Melinda A. Wilkins, PhD, RHIA Abstract The study s
Nurse education integrates today a broader awareness of other disciplines allied to
 AIHA Internet Resources Digest Supporting Access to High Quality Online Resources Spotlight on: Nurse Education and Training January 2015 Nurse education integrates today a broader awareness of other disciplines
AIHA Internet Resources Digest Supporting Access to High Quality Online Resources Spotlight on: Nurse Education and Training January 2015 Nurse education integrates today a broader awareness of other disciplines
Translating advanced practice nursing competence into clinical practice
 Translating advanced practice nursing competence into clinical practice Frances Kam Yuet WONG RN PhD School of Nursing The Hong Kong Polytechnic University Hong Kong Society for Nursing Education 25 th
Translating advanced practice nursing competence into clinical practice Frances Kam Yuet WONG RN PhD School of Nursing The Hong Kong Polytechnic University Hong Kong Society for Nursing Education 25 th
Note EDUCATION. Keywords: Pharmacists Patient Care Process, faculty development, video
 Use of a Video Module to Improve Faculty Understanding of the Pharmacists Patient Care Process Crystal M. Deas, PharmD, BCPS; Angela R. Thomason, PharmD, BCPS; Robert M. Riggs, PhD, RPh; Michael C. Thomas,
Use of a Video Module to Improve Faculty Understanding of the Pharmacists Patient Care Process Crystal M. Deas, PharmD, BCPS; Angela R. Thomason, PharmD, BCPS; Robert M. Riggs, PhD, RPh; Michael C. Thomas,
Programme name MSC Advanced Nurse Practitioner-Child/Adult (Advanced Practice in Health and Social Care)
 PROGRAMME SPECIFICATION KEY FACTS Programme name MSC Advanced Nurse Practitioner-Child/Adult (Advanced Practice in Health and Social Care) Award MSc School School of Health Sciences Department Division
PROGRAMME SPECIFICATION KEY FACTS Programme name MSC Advanced Nurse Practitioner-Child/Adult (Advanced Practice in Health and Social Care) Award MSc School School of Health Sciences Department Division
Text-based Document. The Effect of a Workplace-Based Intervention on Moral Distress Among Registered Nurses. Powell, Nancy Miller
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
This is a repository copy of Non-medical prescribing in palliative care: a regional survey.
 This is a repository copy of Non-medical prescribing in palliative care: a regional survey. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/879/ Version: Accepted Version
This is a repository copy of Non-medical prescribing in palliative care: a regional survey. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/879/ Version: Accepted Version
Exploring Nurses Perceptions of Spiritual Care and Harm Reduction in an Acute Inpatient HIV Unit: A Quality Improvement Perspective
 Exploring Nurses Perceptions of Spiritual Care and Harm Reduction in an Acute Inpatient HIV Unit: A Quality Improvement Perspective Opening reflection Now that most people do not have a religious focus,
Exploring Nurses Perceptions of Spiritual Care and Harm Reduction in an Acute Inpatient HIV Unit: A Quality Improvement Perspective Opening reflection Now that most people do not have a religious focus,
GLASGOW CALEDONIAN UNIVERSITY
 GLASGOW CALEDONIAN UNIVERSITY PROGRAMME SPECIFICATION PRO-FORMA (PSP) 1. GENERAL INFORMATION 1. Programme Title: BSc (Hons) Nursing Studies: Adult Nursing; Child Nursing; Learning Disability Nursing; Mental
GLASGOW CALEDONIAN UNIVERSITY PROGRAMME SPECIFICATION PRO-FORMA (PSP) 1. GENERAL INFORMATION 1. Programme Title: BSc (Hons) Nursing Studies: Adult Nursing; Child Nursing; Learning Disability Nursing; Mental
Programme Specification and Curriculum Map for MSc Health Psychology
 Programme Specification and Curriculum Map for MSc Health Psychology 1. Programme title Health Psychology 2. Awarding institution Middlesex University 3. Teaching institution Middlesex University 4. Programme
Programme Specification and Curriculum Map for MSc Health Psychology 1. Programme title Health Psychology 2. Awarding institution Middlesex University 3. Teaching institution Middlesex University 4. Programme
Georgian College of Applied Arts & Technology
 Georgian College of Applied Arts & Technology Program Outline (Effective Fall 2005) RN Nephrology Nursing (Post Basic Certificate) Program Code: H662 Ministry Approval Date: March 24, 2000 Ministry Code:
Georgian College of Applied Arts & Technology Program Outline (Effective Fall 2005) RN Nephrology Nursing (Post Basic Certificate) Program Code: H662 Ministry Approval Date: March 24, 2000 Ministry Code:
Models of Support in the Teacher Induction Scheme in Scotland: The Views of Head Teachers and Supporters
 Models of Support in the Teacher Induction Scheme in Scotland: The Views of Head Teachers and Supporters Ron Clarke, Ian Matheson and Patricia Morris The General Teaching Council for Scotland, U.K. Dean
Models of Support in the Teacher Induction Scheme in Scotland: The Views of Head Teachers and Supporters Ron Clarke, Ian Matheson and Patricia Morris The General Teaching Council for Scotland, U.K. Dean
Lessons On Dying. What Patients Taught Me That Was Missing From Medical School. By Amberly Orr
 Lessons On Dying { What Patients Taught Me That Was Missing From Medical School By Amberly Orr Carve your name on hearts, not tombstones. A legacy is etched into the minds of others and the stories they
Lessons On Dying { What Patients Taught Me That Was Missing From Medical School By Amberly Orr Carve your name on hearts, not tombstones. A legacy is etched into the minds of others and the stories they
Bedside Teaching Creating Competent Physicians
 Bedside Teaching Creating Competent Physicians "The student begins with the patient, continues with the patient and ends his studies with the patient, using books and lectures as tools as means to an end
Bedside Teaching Creating Competent Physicians "The student begins with the patient, continues with the patient and ends his studies with the patient, using books and lectures as tools as means to an end
Initiative for a Palliative Approach in Nursing: Evidence and Leadership
 Initiative for a Palliative Approach in Nursing: Evidence and Leadership Led by Kelli Stadjuhar (UVic) and Carolyn Tayler (FHA) How and in which contexts can a palliative approach better meet the needs
Initiative for a Palliative Approach in Nursing: Evidence and Leadership Led by Kelli Stadjuhar (UVic) and Carolyn Tayler (FHA) How and in which contexts can a palliative approach better meet the needs
Theory Application: Theory of Comfort. RobERT Pinkston. Old Dominion University
 Running head: THEORY OF COMFORT 1 Theory Application: Theory of Comfort RobERT Pinkston Old Dominion University THEORY OF COMFORT 2 THEORY APPLICATION: THEORY OF COMFORT The Theory of Comfort was developed
Running head: THEORY OF COMFORT 1 Theory Application: Theory of Comfort RobERT Pinkston Old Dominion University THEORY OF COMFORT 2 THEORY APPLICATION: THEORY OF COMFORT The Theory of Comfort was developed
Running Head: READINESS FOR DISCHARGE
 Running Head: READINESS FOR DISCHARGE Readiness for Discharge Quantitative Review Melissa Benderman, Cynthia DeBoer, Patricia Kraemer, Barbara Van Der Male, & Angela VanMaanen. Ferris State University
Running Head: READINESS FOR DISCHARGE Readiness for Discharge Quantitative Review Melissa Benderman, Cynthia DeBoer, Patricia Kraemer, Barbara Van Der Male, & Angela VanMaanen. Ferris State University
Masters of Arts in Aging Studies Aging Studies Core (15hrs)
 Masters of Arts in Aging Studies Aging Studies Core (15hrs) AGE 717 Health Communications and Aging (3). There are many facets of communication and aging. This course is a multidisciplinary, empiricallybased
Masters of Arts in Aging Studies Aging Studies Core (15hrs) AGE 717 Health Communications and Aging (3). There are many facets of communication and aging. This course is a multidisciplinary, empiricallybased
TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT)
 TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT) Introduction The National Institute for Clinical Excellence has developed Guidance on Supportive and Palliative Care for patients with cancer. The standards
TOPIC 9 - THE SPECIALIST PALLIATIVE CARE TEAM (MDT) Introduction The National Institute for Clinical Excellence has developed Guidance on Supportive and Palliative Care for patients with cancer. The standards
Producing and utilising research: Barriers for a nursing faculty in
 Producing and utilising research: Barriers for a nursing faculty in Oman Gillian White Correspondence Professor Gillian White SCM., RM., MTD., Cert Ad Ed BEd., Dip.Soc.Sci (Psych), MA (Hons), PhD Education
Producing and utilising research: Barriers for a nursing faculty in Oman Gillian White Correspondence Professor Gillian White SCM., RM., MTD., Cert Ad Ed BEd., Dip.Soc.Sci (Psych), MA (Hons), PhD Education
NCLEX-RN 2015: Canadian Results. Published by the Canadian Council of Registered Nurse Regulators (CCRNR)
 NCLEX-RN 2015: Canadian Results Published by the Canadian Council of Registered Nurse Regulators (CCRNR) March 31, 2016 Contents Message from the president 3 Background on the NCLEX-RN 4 The role of Canada
NCLEX-RN 2015: Canadian Results Published by the Canadian Council of Registered Nurse Regulators (CCRNR) March 31, 2016 Contents Message from the president 3 Background on the NCLEX-RN 4 The role of Canada
emja: Measuring patient-reported outcomes: moving from clinical trials into clinical p...
 Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Improving End of Life Care in Long Term Care Facilities: Perspectives of Healthcare Providers
 Improving End of Life Care in Long Term Care Facilities: Perspectives of Healthcare Providers Christine Beck, MD CCFP MSc Department of Family Medicine Dalhousie University January 15, 2010 NELS Work In
Improving End of Life Care in Long Term Care Facilities: Perspectives of Healthcare Providers Christine Beck, MD CCFP MSc Department of Family Medicine Dalhousie University January 15, 2010 NELS Work In
