Oesophago-Gastro Duodenoscopy (OGD) with PEG feeding tube insertion. Patient information. Endoscopy Unit,
|
|
|
- Vernon May
- 6 years ago
- Views:
Transcription
1 Oesophago-Gastro Duodenoscopy (OGD) with PEG feeding tube insertion Patient information Endoscopy Unit, The Royal Infirmary of Edinburgh Endoscopy Nurses: Endoscopy Booking Line: This document contains important information about your upcoming procedure and should be read immediately, giving you time for questions, if you have any. Reviewed May 2011 Next review May 2012 Responsible H Chisholm CN 1
2 Contents Page Introduction 3 General information about the procedure 4 Preparation and Medication 5 The OGD procedure 6 Risks of the procedure 7 After the procedure 9 Points to remember 9 Information for patients with diabetes 10 How to get to the hospital 11 Consent form 14 2
3 Introduction You have been advised by your GP or hospital doctor to have a procedure to insert a PEG feeding tube to help your nutrition. This is inserted at the time of an oesophago-gastroduodenoscopy (OGD, or gastroscopy) If you are unable to keep your appointment, please notify the department as soon as possible. This will enable the staff to arrange another date and time for you (and give your appointment to someone else) It is essential that you read this booklet thoroughly and carefully. Please bring this booklet and appointment letter with you when you attend. This procedure requires your formal consent. This booklet has been written to enable you to make an informed decision about agreeing to the procedure. At the back of the booklet is the consent form. The consent form is a legal document, therefore please read it carefully. Once you have read and understood all the information, including the possibility of complications, and you agree to undergo the procedure, please sign and date the consent form. You will notice that the consent form is duplicated, allowing you to keep a copy for your records. Please fill it in while it is still attached to this booklet. If however there is anything you do not understand or wish to discuss further, but still wish to attend, do not sign the form, but bring it with you and you can sign it after you have spoken to a health care professional. If having read the information you do not wish to go ahead with the procedure, or want to consider alternative methods of investigation, please discuss with your GP or hospital doctor as soon as possible before the date of your appointment. Sedation If you are having sedation, the drug can remain in your system for up to 24 hours and you may feel drowsy later on, with intermittent lapses of memory. If you are not already an in-patient in the hospital, it will usually be necessary to be admitted overnight after this procedure. 3
4 General information about the procedure What is an OGD? The procedure you will be having is called an oesophago-gastro-duodenoscopy (OGD), sometimes known more simply as a gastroscopy or endoscopy. This is an examination of your oesophagus (gullet), stomach and the first part of your small intestine called the duodenum. The instrument used in this investigation is called a gastroscope. It is flexible and has a diameter less than that of a little finger. The gastroscope relays images back the Endoscopist on a TV screen. During the investigation, the Endoscopist may need to take some tissue samples (biopsies) from the lining of your upper digestive tract for analysis, this is painless. The samples may be retained. Photographs and/or a video recording may be taken for your records. The procedure will be performed by, or under the supervision of, a trained doctor and we will make the investigation as comfortable as possible for you. In routine examinations some patients have sedation injected into a vein for this procedure. In your particular circumstances, if the Endoscopist has decided that you require endoscopic treatment, you will receive intravenous sedation, often in combination with a painkiller. Your OGD is more involved than having a straightforward inspection. The Endoscopist is also using the procedure to give you treatment for your condition, in this case placement of a PEG feeding tube. This is known as a therapeutic gastroscopy. What is a PEG? A PEG is a way of directly introducing food, fluids and medicines through a thin tube inserted through the skin into the stomach. This allows you to be fed without swallowing. PEG stands for percutaneous endoscopic gastrostomy. Percutaneous refers to something that is inserted through the skin. Endoscopic refers to the endoscope that is used to carry out the procedure. Gastrostomy refers to an opening into the stomach. Why do I need a PEG tube? A PEG tube bypasses the throat and gullet and can therefore be used for people who have difficulty with swallowing or if there is a risk of the food going the wrong way into the lungs. Sometimes it is recommended you have a PEG inserted before a treatment starts even if you do not have swallowing problems at this point if the treatment planned is likely to affect your swallowing in the future. This will help you maintain good nutrition, which is important to your recovery. 4
5 The food, which goes through the PEG tube, is a specialised prescribed liquid mix of the nutrition your body needs. Your dietitian will be able to provide more information on this and the ways of using the tube to feed. Are there any alternatives? Although tube feeding can be achieved by passing a thin tube through the nose and into the stomach, this method of feeding is more visible and less comfortable. It is therefore not so suitable for longer term use. For people who need tube feeding for long periods of time, a PEG is more comfortable and easier to manage at home. PEG tubes are also more discreet as they can be tucked away under your clothes. If you would like to discuss the options available to you, please speak to your medical team, dietitian or nutrition nurse. How long will I be in the endoscopy department? If you are coming in from home you may be in the department 2-3 hours before the procedure therefore you may want to bring something to read. We recommend you do not bring any valuable items with you to the hospital. Patients having more complex procedures such as PEG insertion are sometimes admitted to hospital in advance of the procedure. It is usually necessary to remain in hospital for a few days afterwards Preparation for the procedure Eating and drinking It is important to have clear views and for this the stomach must be empty. If your appointment is in the morning, take no food or drinks after midnight If your appointment is in the afternoon, you may have a light breakfast (tea & toast) no later than 8am, but no food or drinks after that. Small amounts of water are ok to take up to two hours before the procedure, providing you have been told it is safe to swallow What about my medication? If you usually take your medication by mouth it can be taken in the normal way on the day of the procedure. For people with diabetes If you have diabetes that is controlled by insulin or medication, please ensure the Endoscopy department is aware so that the appointment can be made at the beginning of the list. Please see guidelines printed in the back of this booklet. 5
6 Anticoagulants Please telephone the unit on if you are taking blood-thinning drugs such as Warfarin or Clopidogrel. If you have any other queries regarding your medications please telephone the Endoscopy Unit on Allergies Please telephone the endoscopy unit on for information if you think you have a latex allergy. What happens when I arrive? When you arrive in the department, a qualified nurse or health care assistant will meet you and will ask you a few questions, including about your arrangements for getting home. You will also be able to ask further questions about the investigation. The nurse will ensure you understand the procedure and discuss any outstanding concerns or questions you may have. If you are having sedation they may insert a small cannula (plastic tube) into a vein in your arm through which sedation will be administered later. You will have a brief medical assessment where a nurse will ask you some questions regarding your medical condition and any surgery or illnesses you have had. This is to confirm that you are fit to undergo the investigation. Your blood pressure and heart rate will be recorded, and if you have diabetes, your blood glucose level will also be recorded. If you have not already done so, and you are happy to proceed, you will be asked to sign your consent form at this point. The OGD procedure You will be escorted into the procedure room where the Endoscopist and the nurses will introduce themselves. You will also be able to ask further questions about the investigation. If you have any dentures you will be asked to remove them at this point. Any remaining teeth will be protected by a small plastic mouth guard, which will be inserted immediately before the examination starts. If you are having local anaesthetic throat spray, this will be sprayed on to the back of your throat whilst you are sitting up and swallowing: the effect is rapid and you will notice loss of sensation of your tongue and throat. The nurse looking after you will ask you to lie on your left side. If you are having sedation, the medication will be administered into the cannula in your vein, which will make you relaxed and lightly drowsy but not unconscious. This means that, although drowsy, you will still hear what is said to you and therefore will be able to follow simple instructions during the investigation. Some patients experience amnesia with the 6
7 sedation so that afterwards they remember very little of the procedure, but this does not always happen. During the procedure we will monitor your breathing, heart rate and oxygen levels. This is done by means of a probe attached to your finger or earlobe. Your blood pressure may also be recorded during the procedure using a cuff, which will inflate on your arm from time to time. You may also be given oxygen to breathe through a mask or small tubes placed at your nose. Any saliva or other secretions produced during the investigation will be removed using a small suction tube like the one used at the dentist. The Endoscopist will introduce the gastroscope into your mouth, and by asking you to swallow can pass it down your oesophagus, into your stomach and then into your duodenum. Your windpipe is deliberately avoided and your breathing will be unhindered. Insertion of the PEG For the procedure to insert the PEG, you will be helped to turn so that you are lying on your back. An antiseptic solution will be used to clean the skin over your abdomen. Local anaesthetic, which may sting initially, will be used to numb the area where the PEG tube is to be placed. A thin, hollow needle will then be passed through your skin and into your stomach. A thread is passed through this needle into the stomach, grasped using the endoscope, and is then withdrawn through the mouth bringing the thread with it. The feeding tube is then attached to the thread and the thread and tube are drawn back into the stomach and out through the skin so that the PEG feeding tube now passes through the skin of your abdomen directly into your stomach. Although you will feel some pressure and some prodding over your stomach, you should not feel any pain. Once in place either a small plastic disc or a small balloon inside the stomach stops the tube from being pulled out. Another plastic disc on the outside stops the tube falling into the stomach. PEG insertion usually takes 20 to 30 minutes. It is important that you let the doctor or nurse know if you are uncomfortable afterwards so that you can be offered appropriate medication. Risks of the procedure The doctor who has requested the procedure will have considered and discussed this with you. The risks must be compared to the benefit of having the procedure carried out. There are three sets of procedural risks you should be aware of: 1. Risks associated with intravenous sedation Sedation can occasionally cause problems with breathing, heart rate and blood pressure. If any of these problems do occur, they are normally short lived. Careful monitoring by a fully 7
8 trained endoscopy nurse ensures that any potential problems can be identified and treated rapidly. Older patients and those who have significant health problems (for example, people with significant breathing difficulties due to a bad chest) may be assessed by a doctor before having the procedure. In these situations it may be advised that a lesser degree of sedation is used, as the risks of complications from sedation may be higher. 2. Risks associated with endoscopic examination and biopsy Gastroscopy is generally a very safe investigation, but as with any invasive procedure it has the possibility of complications. A sore throat after the procedure is the most common side effect. More serious complications occur infrequently but can include: Damage to teeth. For this reason dentures are removed and you will be asked about loose teeth, crowns or bridgework Chest infection can occur after the procedure if some fluid passes into the lungs. The risk of this is greater with procedures requiring heavier sedation. Treatment with antibiotics may be necessary. Bleeding from the site of a biopsy. This is usually minor and stops on its own Perforation (or tear) of the lining or wall of the digestive tract. This is very rare with a diagnostic examination only, but can occur more often with the more complex procedures involving endoscopic treatment (see below). A perforation would require admission to hospital for treatment with fluids and antibiotics, and might require surgery to repair the tear. 3. Risks associated with the endoscopic treatment of your condition Endoscopic treatment has revolutionised the way in which some diseases are treated. It is often the case that conditions previously only treated by surgery can now be dealt with using endoscopy. The specific risks associated with endoscopic treatment you are having are described below. The occurrence of any of these may delay your discharge from hospital. It is important to appreciate that a serious complication in rare circumstances could prove fatal. PEG insertion Although the procedure is relatively safe, there are risks involved in passing the endoscope and in making a hole in the stomach. Minor complications occur in 15% of cases and are mostly related to infection around the site of the tube. This can usually be treated successfully with antibiotics. In around 5% of procedures there can be more significant complications. These may include: Bleeding at the site of the tube Unintended perforation (tear) of the stomach. Severe infection in the abdomen. Damage to another organ in the abdomen With some of these complications it might be necessary to remove the tube and/or have a surgical operation. 8
9 Most people will not experience any serious complications from their PEG placement. However, risks do increase with age and for those who already have heart, chest or other medical conditions, such as diabetes, or those who are overweight or smoke. After the procedure Your blood pressure and heart rate will be recorded and if you are diabetic, your blood glucose will be monitored. Should you have underlying breathing difficulties or if your oxygen levels were low during the procedure, we will continue to monitor your breathing. When the tube is first placed, it can feel a little uncomfortable. This is due to wind, but generally settles after a few hours. Painkillers can be given if needed. Because of discomfort you may be reluctant to take deep breaths, however it is important that you do to help prevent chest infections occurring. In most cases liquid feed can be given via the PEG tube about four hours after insertion. If you are also able to swallow safely you will be able to eat and drink as soon as the effects of the sedation have worn off, in most cases. If you have had your throat sprayed with local anaesthetic you will need to wait a little longer. What will happen over the following days? Either before the procedure or over the next few days you and your family will be shown how to use and care for your PEG tube either by a nutrition nurse, the ward nurses, or the homecare team in your own home. You can take as long as you need to learn this. If there is pain on feeding, external leaking or bleeding, you should stop using the tube and either contact your dietitian, specialist nurse, nutrition nurse or the endoscopy department (or NHS 24). Points to remember If you are unable to keep your appointment please notify the endoscopy unit as soon as possible. It is our aim for you to be seen as soon as possible after your arrival. However, the department is very busy and your procedure may be delayed. If emergencies occur, these patients may be given priority over less urgent cases. The hospital cannot accept any responsibility for the loss or damage to personal property during your time on the premises. If you have any problems with worsening neck/chest/abdominal pain, after your procedure, please inform the nurses who are looking after you. 9
10 Information for patients with diabetes You should inform the Endoscopy department about your diabetes and request an early morning appointment. The day of the procedure Diet-controlled and tablet-controlled diabetes (Type 2 Diabetes) Check your blood glucose on waking. If your blood glucose is less than 5 mmol/l, or you feel that your blood glucose level may be low, have a small glass of a sugar-containing drink. Inform the nurse on arrival in the Endoscopy unit that you have done this. A nurse will check your blood glucose level when you arrive in the Endoscopy Unit. Do not take your morning dose of tablets; bring your tablets with you to have after the procedure Report to the nursing staff if you have needed glucose before arriving and inform them immediately if you feel hypo at any time during your visit Your dosage of tablets can be given as soon as you are able to eat and drink safely; the nursing staff will inform you when it is safe. Insulin-controlled diabetes Monitor your blood glucose at least 4 times during the day, but ideally you should monitor even more frequently than this. Continue to take your daily insulin injections, but the amount you take may need to be altered according to how your blood glucose levels are behaving and how much carbohydrate containing drinks you are taking. In general, insulin doses often need to be reduced by one quarter to one third. You should reduce your evening insulin injection by one third, unless your blood glucose levels are running very high (e.g. greater than 15 mmols/l) when you should leave your dose unaltered. If you have concerns about adjusting your insulin dosage please contact the Diabetes Specialist Nurses on , to discuss appropriate measures. You can also contact the diabetes doctor on call on and ask to speak to the diabetes doctor. Carrying glucose to treat hypoglycaemia If you are on tablets or insulin for your diabetes, then on the day before and day of the procedure, carry glucose tablets (Dextrosol) in case of hypoglycaemia. As these are absorbed quickly through the tissues of the mouth, if sucked, they will not interfere with the procedure. Take three (3) tablets initially, followed by a further three (3) if symptoms continue after 15 minutes. If your medication has been adjusted this should not be a problem. Blood glucose monitoring If you usually test your blood glucose levels, check them, as usual, on the morning of the procedure and carry your equipment with you to the appointment. If you do not usually test your blood, do not worry, your blood glucose levels will be checked when you arrive for the procedure. 10
11 Location of the Endoscopy Unit The endoscopy unit is located within the Medical Daycase Unit of the Royal Infirmary Directions to the Medical Day Case Unit If entering via North Junction Road/Car park B: Entrance signed Day Case & Day Surgery (No.2 on map) adjacent to Main Front Entrance (West) If entering via South Junction Road/Car park C: Enter the hospital through Main Rear Entrance (East). Continue through main mall and exit at Main Front Entrance (West). Turn left and enter at Day Case & Day Surgery (No.2 on map). Please report to reception desk on arrival. Plan of the hospital and grounds. Entrance to Endoscopy Unit is at 2 11
12 Location of the Royal Infirmary of Edinburgh. The hospital is on the south side of Edinburgh on old Dalkeith Road (A7). The full address is: Royal Infirmary of Edinburgh, 51 Little France Crescent, Old Dalkeith Road, EH16 4SA By Public Transport The following services stop at the hospital, either at the West main entrance bus stop, or close by on Old Dalkeith Road. LRT 8, Muirhouse to Little France LRT 18, Gyle Centre to Little France LRT 21, Gyle Centre to Little France LRT 24, Davidson s Mains to Little France LRT 33 & N33 Baberton Mains to Little France LRT 38, Muirhouse to Little France LRT 49, The Jewel to NRIE Munros 51 or 52, Edinburgh to Jedburgh or Kelso respectively. First 79, Haymarket to Rosewell First 86, Clerwood to Mayfield Eve Car and Coaches 128, Haddington to Little France First 140 & 142, Rosewell to NRIE, passing Musselburgh Please note that the proposed services and timetables may have changed by the time of your appointment, therefore you are advised to check the details by contacting the City of Edinburgh Council s Traveline or the bus operator on the numbers below. Contact details for full timetables or further information are: Lothian Buses: First Edinburgh: Stagecoach: Munros: Traveline By car: Directions from City Centre Leave the city centre via North Bridge at the East end of Princes Street. Follow this road for approx. two and a half miles until you reach the Liberton Road/Lady Road junction. Turn left on to Lady Road. Go straight over the Lady Road roundabout to the Cameron Toll roundabout. Take the 3rd exit sign posted to Dalkeith and New Royal Infirmary (A7). Continue on this road for around ¾ mile. The hospital is on the left hand side. Directions from Bypass Leave the Edinburgh City Bypass (A720) at the Sheriffhall Roundabout onto Old Dalkeith Road (A7) toward Edinburgh City Centre. Turn right into the hospital after just over 2 miles. 12
13 Entry to the site is via two access roads, one to the north and one to the south of the site. The nearest Car Park and drop off point to our department is reached by entering the North Junction road. Please use Car Park B and enter the Hospital by the entrance signed Day Case & Day Surgery. There are free disabled parking spaces located near the main entrances. The current parking charges for all other patients and visitors are: 0-1 hours hours hours hours hours hours hours 7.00 By bicycle/motorbike: New cycle/bus lane from Cameron Toll to the Royal Infirmary of Edinburgh via Old Dalkeith Road, as well as improvements to the cycle and footpaths on Craigmillar Castle Road, may make this an option for some patients and visitors. There is currently provision to park both bicycles and motorbikes on site, free of charge. Motorcycle parking is within marked spaces out with the car parks at various points around the perimeter of the building. Cycle parking is available close to all the entrances to the building, in the form of Sheffield stands. CCTV monitors these areas at all times. 13
14 Patient Details Consent Form Patient agreement to endoscopic investigation or treatment Name of procedure/s (include a brief explanation if the medical term is not clear) Oesophago-Gastro Duodenoscopy (OGD) and Percutaneous endoscopic gastrostomy Inspection of the upper gastrointestinal tract with a flexible endoscope and insertion of a PEG feeding tube (with or without biopsy, photography) Biopsy samples will be retained Statement of patient You have the right to change your mind at any time, including after you have signed this form I have read and understood the information in the attached booklet including the benefits and any risks. I agree to the procedure described in the booklet and on this form. I understand that you cannot give me a guarantee that a particular person will perform the procedure. The person will, however, have appropriate experience. If a trainee performs this examination it will be performed under supervision by a fully qualified practitioner. I would like to have: local anaesthetic throat spray sedation Please tick box Signed (patient) Date Name (print in capitals) If you would like to ask further questions please do not sign the form now. Bring it with you and you can sign it after you have spoken to the healthcare professional. Confirmation of consent (To be completed by a healthcare professional when patient is admitted for procedure) I have confirmed that the patient/guardian understands what the procedure involves, including the benefits and any risks I have confirmed that the patient/guardian has no further questions and wishes for the procedure to go ahead Signed Name (print in capitals) Date Designation (If your patient requires further information please complete page 3 of this consent form) 14
15 Patient Details Consent Form - COPY Patient agreement to endoscopic investigation or treatment Name of procedure/s (include a brief explanation if the medical term is not clear) Oesophago-Gastro Duodenoscopy (OGD) and Percutaneous endoscopic gastrostomy Inspection of the upper gastrointestinal tract with a flexible endoscope and insertion of a PEG feeding tube (with or without biopsy, photography) Biopsy samples will be retained Statement of patient You have the right to change your mind at any time, including after you have signed this form I have read and understood the information in the attached booklet including the benefits and any risks. I agree to the procedure described in the booklet and on this form. I understand that you cannot give me a guarantee that a particular person will perform the procedure. The person will, however, have appropriate experience. If a trainee performs this examination it will be performed under supervision by a fully qualified practitioner. I would like to have: local anaesthetic throat spray sedation Please tick box Signed (patient) Date Name (print in capitals) If you would like to ask further questions please do not sign the form now. Bring it with you and you can sign it after you have spoken to the healthcare professional. Confirmation of consent (To be completed by a healthcare professional when patient is admitted for procedure) I have confirmed that the patient/guardian understands what the procedure involves, including the benefits and any risks I have confirmed that the patient/guardian has no further questions and wishes for the procedure to go ahead Signed Name (print in capitals) Date Designation (If your patient requires further information please complete page 3 of this consent form) 15
16 Patient Details Consent Form Patient agreement to endoscopic investigation or treatment Statement of healthcare professional (to be completed by a healthcare professional with appropriate knowledge of proposed procedure, as specified in the consent policy) In response to a request for further information I have explained the procedure to the patient. In particular I have explained: The intended benefits 1. Investigation of symptoms 2. Endoscopic therapy Potential Risks 1. Procedure risks: 2. Sedation risks: I have also discussed what the procedure is likely to involve, the benefits and risks of any available alternative investigations/treatments (including no treatment), any extra procedures, which may become necessary and any particular concerns of those involved. Signed Name (print in capitals) Date Designation Statement of interpreter where appropriate I have interpreted the information above to the patient/guardian to the best of my ability and in a way in which I believe she/he/they can understand. Signed Date Name (print in capitals) 16
Oesophago-Gastro Duodenoscopy (OGD) with Haemostasis
 South Tyneside NHS Foundation Trust Oesophago-Gastro Duodenoscopy (OGD) with Haemostasis Patient information booklet Endoscopy Unit Providing a range of NHS services in Gateshead, South Tyneside and Sunderland.
South Tyneside NHS Foundation Trust Oesophago-Gastro Duodenoscopy (OGD) with Haemostasis Patient information booklet Endoscopy Unit Providing a range of NHS services in Gateshead, South Tyneside and Sunderland.
Gastroscopy. Please bring this booklet with you to your appointment. Oesophago-gastro duodenoscopy (OGD)
 Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination, and consent form Please bring this booklet with you to your appointment 1 2 Your appointment
Gastroscopy Oesophago-gastro duodenoscopy (OGD) Your appointment details, information about the examination, and consent form Please bring this booklet with you to your appointment 1 2 Your appointment
Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion
 Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion Patient Information Ninewells Hospital Endoscopy Unit Telephone: 01382 660111, extension: 40078 or bleep 4470 Perth Royal Infirmary Endoscopy Unit
Percutaneous Endoscopic Gastrostomy (PEG) Tube Insertion Patient Information Ninewells Hospital Endoscopy Unit Telephone: 01382 660111, extension: 40078 or bleep 4470 Perth Royal Infirmary Endoscopy Unit
Endoscopic Ultrasound (EUS) or Endosonography
 Endoscopic Ultrasound (EUS) or Endosonography This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment
Endoscopic Ultrasound (EUS) or Endosonography This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment
Having a Gastroscopy. A guide to the test. Information for patients
 Having a Gastroscopy A guide to the test Information for patients Your doctor has recommended that you have a gastrointestinal endoscopy, this is sometimes called a Gastroscopy or Endoscopy. This leaflet
Having a Gastroscopy A guide to the test Information for patients Your doctor has recommended that you have a gastrointestinal endoscopy, this is sometimes called a Gastroscopy or Endoscopy. This leaflet
Gastroscopy and Dilatation
 i If you need this information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need this information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
Percutaneous Endoscopic Gastrostomy (PEG)
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Endoscopic Gastrostomy (PEG) Nursing and Clinical Governance Why do I need a feeding tube? You may be due to have
HAVING A GASTROSCOPY. ENDOSCOPY DEPARTMENT Patient Information
 ENDOSCOPY DEPARTMENT Patient Information HAVING A GASTROSCOPY Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information in large print,
ENDOSCOPY DEPARTMENT Patient Information HAVING A GASTROSCOPY Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information in large print,
Patient Information Leaflet. Gastroscopy. Prepared by Endoscopy Department
 Patient Information Leaflet Gastroscopy Prepared by Endoscopy Department February 2013 Review due February 2016 1 If you require this leaflet in another language, large print or another format, please
Patient Information Leaflet Gastroscopy Prepared by Endoscopy Department February 2013 Review due February 2016 1 If you require this leaflet in another language, large print or another format, please
PATIENT PROCEDURE INFORMATION LEAFLET GASTROSCOPY & FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL)
 PATIENT PROCEDURE INFORMATION LEAFLET GASTROSCOPY & FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Gastroscopy? A gastroscopy (or simple endoscopy) is a test which allows the Endoscopist to look
PATIENT PROCEDURE INFORMATION LEAFLET GASTROSCOPY & FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Gastroscopy? A gastroscopy (or simple endoscopy) is a test which allows the Endoscopist to look
Diagnostic Upper Gastrointestinal Endoscopy
 Diagnostic Upper Gastrointestinal Endoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a gastroscopy, including the benefits, risks and any alternatives and
Diagnostic Upper Gastrointestinal Endoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a gastroscopy, including the benefits, risks and any alternatives and
Endoscopy Department Patient Information Gastroscopy with Oesophageal Dilation
 Endoscopy Department Patient Information Gastroscopy with Oesophageal Dilation This leaflet provides information about the Endoscopy and Dilation procedure. It aims to answer any questions you may have
Endoscopy Department Patient Information Gastroscopy with Oesophageal Dilation This leaflet provides information about the Endoscopy and Dilation procedure. It aims to answer any questions you may have
Gastroscopy - Inpatients
 PATIENT INFORMATION Gastroscopy - Inpatients Welcome to the Endoscopy Unit You have been referred by your doctor to have a Gastroscopy. This booklet has been written to explain the procedure. This will
PATIENT INFORMATION Gastroscopy - Inpatients Welcome to the Endoscopy Unit You have been referred by your doctor to have a Gastroscopy. This booklet has been written to explain the procedure. This will
Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure
 Page 1 of 7 Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure Introduction This leaflet only contains information regarding a PEG tube and includes important information about the procedure.
Page 1 of 7 Undergoing a Percutaneous Endoscopic Gastrostomy (PEG) Tube procedure Introduction This leaflet only contains information regarding a PEG tube and includes important information about the procedure.
Having an Oesophageal Dilatation
 Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Having a Push Enteroscopy
 Endoscopy Unit Having a Push Enteroscopy A guide to the test Outpatient information 2 Your doctor has recommended that you have a Push Enteroscopy. This leaflet will explain the procedure and what to expect
Endoscopy Unit Having a Push Enteroscopy A guide to the test Outpatient information 2 Your doctor has recommended that you have a Push Enteroscopy. This leaflet will explain the procedure and what to expect
Endoscopy Unit Having an EUS
 Endoscopy Unit Having an EUS Information for patients 2 Your doctor has recommended that you have an Endoscopic Ultrasound. This leaflet will explain the procedure and what to expect on the day of your
Endoscopy Unit Having an EUS Information for patients 2 Your doctor has recommended that you have an Endoscopic Ultrasound. This leaflet will explain the procedure and what to expect on the day of your
Endoscopic Ultrasound Examination (EUS) Hepatobiliary Services Information for patients
 Endoscopic Ultrasound Examination (EUS) Hepatobiliary Services Information for patients i Introduction We hope that this booklet will help you to understand more about the procedure and the care that you
Endoscopic Ultrasound Examination (EUS) Hepatobiliary Services Information for patients i Introduction We hope that this booklet will help you to understand more about the procedure and the care that you
Gastroscopy and Flexible Sigmoidoscopy
 Gastroscopy and Flexible Sigmoidoscopy Your appointment details, information about the examination and the consent form Please bring this booklet with you to your appointment 1 2 Your appointment An appointment
Gastroscopy and Flexible Sigmoidoscopy Your appointment details, information about the examination and the consent form Please bring this booklet with you to your appointment 1 2 Your appointment An appointment
Upper GI Endoscopy a guide for patients and carers
 Upper GI Endoscopy a guide for patients and carers Welcome to the Endoscopy Unit. This information leaflet is intended to provide you with information about an upper endoscopy. It is not expected to cover
Upper GI Endoscopy a guide for patients and carers Welcome to the Endoscopy Unit. This information leaflet is intended to provide you with information about an upper endoscopy. It is not expected to cover
If you have any questions about the risks of this procedure please ask the endoscopist doing the test or the person who has referred you.
 What is a gastroscopy? A gastroscopy is an examination of the lining of the gullet (oesophagus), stomach, and first part of the small bowel (duodenum). It involves an endoscope (a thin, flexible tube with
What is a gastroscopy? A gastroscopy is an examination of the lining of the gullet (oesophagus), stomach, and first part of the small bowel (duodenum). It involves an endoscope (a thin, flexible tube with
Upper gastro-intestinal (GI) endoscopy
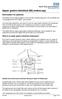 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. You have been advised by your doctor
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. You have been advised by your doctor
Having an endoscopic retrograde cholangio-pancreatograph (ERCP)
 Having an endoscopic retrograde cholangio-pancreatograph (ERCP) Patient name Appointment date Arrival time ERCP sessions run from 9am to 1pm. Every effort will be made to see you promptly on your arrival,
Having an endoscopic retrograde cholangio-pancreatograph (ERCP) Patient name Appointment date Arrival time ERCP sessions run from 9am to 1pm. Every effort will be made to see you promptly on your arrival,
Endoscopy Unit Having an Oesophageal Stent insertion
 Endoscopy Unit Having an Oesophageal Stent insertion Information for patients Your doctor has recommended that you have an Oesophageal Stent Insertion. This leaflet will explain the procedure and what
Endoscopy Unit Having an Oesophageal Stent insertion Information for patients Your doctor has recommended that you have an Oesophageal Stent Insertion. This leaflet will explain the procedure and what
Double Balloon Enteroscopy
 Endoscopy Unit Double Balloon Enteroscopy A guide to the test Outpatient information Your doctor has recommended that you have a Double Balloon Enteroscopy. This leaflet will explain the procedure and
Endoscopy Unit Double Balloon Enteroscopy A guide to the test Outpatient information Your doctor has recommended that you have a Double Balloon Enteroscopy. This leaflet will explain the procedure and
Transnasal Endoscopy (TNE)
 Transnasal Endoscopy (TNE) Information for you Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications are available in other
Transnasal Endoscopy (TNE) Information for you Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications are available in other
Having a gastroscopy
 Other formats Having a gastroscopy Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on If you need this information in another format such as audio tape or
Other formats Having a gastroscopy Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on If you need this information in another format such as audio tape or
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Colonoscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Having a Gastroscopy Information for Patients
 Endoscopy Team Information for Patients Having a Gastroscopy Information for Patients What is a Gastroscopy? You have been advised to have a gastroscopy to help find the cause of your symptoms. A gastroscopy
Endoscopy Team Information for Patients Having a Gastroscopy Information for Patients What is a Gastroscopy? You have been advised to have a gastroscopy to help find the cause of your symptoms. A gastroscopy
Antegrade Double Balloon Enteroscopy Endoscopy Unit
 Manchester Royal Infirmary Antegrade Double Balloon Enteroscopy Endoscopy Unit Information For Patients 2 You have been advised to have an antegrade double balloon enteroscopy. This booklet has been prepared
Manchester Royal Infirmary Antegrade Double Balloon Enteroscopy Endoscopy Unit Information For Patients 2 You have been advised to have an antegrade double balloon enteroscopy. This booklet has been prepared
Northumbria Healthcare NHS Foundation Trust. Your guide to having a combined Gastroscopy and Colonoscopy. Issued by the Endoscopy Team
 Northumbria Healthcare NHS Foundation Trust Your guide to having a combined Gastroscopy and Colonoscopy Issued by the Endoscopy Team You have been referred for a combined gastroscopy and colonoscopy. This
Northumbria Healthcare NHS Foundation Trust Your guide to having a combined Gastroscopy and Colonoscopy Issued by the Endoscopy Team You have been referred for a combined gastroscopy and colonoscopy. This
Having a Gastroscopy Information for Patients
 909170-WZZ 1044.qxp 27/01/2017 15:56 Page 1 Amersham Stoke Mandeville Wycombe Title of leaflet: Having a Gastroscopy information for Patients Compiled by: Sisters Sue Kenny & Deborah Coles Endoscopy Services,
909170-WZZ 1044.qxp 27/01/2017 15:56 Page 1 Amersham Stoke Mandeville Wycombe Title of leaflet: Having a Gastroscopy information for Patients Compiled by: Sisters Sue Kenny & Deborah Coles Endoscopy Services,
FLEXIBLE SIGMOIDOSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE
 DAY SURGERY UNIT FLEXIBLE SIGMOIDOSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE Why do I need to have a flexible sigmoidoscopy?
DAY SURGERY UNIT FLEXIBLE SIGMOIDOSCOPY INFORMATION SHEET PLEASE READ THIS, SIGN THE 2 CONSENT FORMS ATTACHED AND BRING THESE WITH YOU ON THE DAY OF YOUR PROCEDURE Why do I need to have a flexible sigmoidoscopy?
Flexible Sigmoidoscopy
 Flexible Sigmoidoscopy This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment 1 2 Your appointment
Flexible Sigmoidoscopy This booklet contains details of your appointment, information about the examination and the consent form. Please bring this booklet with you to your appointment 1 2 Your appointment
Information for Patients
 Having a Radiologically Inserted Gastrostomy (RIG) Information for Patients In this leaflet: Introduction.. 2 What is a RIG feeding tube?. 2 Why do I need a RIG?. 2 Are there any risks?.2 Are there any
Having a Radiologically Inserted Gastrostomy (RIG) Information for Patients In this leaflet: Introduction.. 2 What is a RIG feeding tube?. 2 Why do I need a RIG?. 2 Are there any risks?.2 Are there any
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Sigmoidoscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Sigmoidoscopy Gastroenterology Unit patient information booklet What is sigmoidoscopy? Sigmoidoscopy is a camera procedure used to examine
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Sigmoidoscopy Gastroenterology Unit patient information booklet What is sigmoidoscopy? Sigmoidoscopy is a camera procedure used to examine
Gastroscopy. What is a Gastroscopy? Website: Tel:
 Gastroscopy (Oesophago-Gastro Duodenoscopy, or OGD) This booklet contains advice for patients and carers about having a Gastroscopy or OGD Endoscopy Department Website: www.rbch.nhs.uk Tel: 01202 704668
Gastroscopy (Oesophago-Gastro Duodenoscopy, or OGD) This booklet contains advice for patients and carers about having a Gastroscopy or OGD Endoscopy Department Website: www.rbch.nhs.uk Tel: 01202 704668
Northumbria Healthcare NHS Foundation Trust. Your guide to having a gastroscopy (when on treatment) Issued by the Endoscopy Team
 Northumbria Healthcare NHS Foundation Trust Your guide to having a gastroscopy (when on treatment) Issued by the Endoscopy Team This leaflet is to inform you about having a gastroscopy. Purpose of the
Northumbria Healthcare NHS Foundation Trust Your guide to having a gastroscopy (when on treatment) Issued by the Endoscopy Team This leaflet is to inform you about having a gastroscopy. Purpose of the
Gastroscopy and Colonoscopy
 Patient Information Gastroscopy and Colonoscopy Endoscopy Department Shrewsbury and Telford Hospital NHS Trust What is a Gastroscopy and Colonoscopy? Gastroscopy and Colonoscopy is a combined procedure
Patient Information Gastroscopy and Colonoscopy Endoscopy Department Shrewsbury and Telford Hospital NHS Trust What is a Gastroscopy and Colonoscopy? Gastroscopy and Colonoscopy is a combined procedure
Endoscopy Unit. Having a Colonoscopy. A guide to the test. Outpatient information
 Endoscopy Unit Having a Colonoscopy A guide to the test Outpatient information Your doctor has recommended that you have a colonoscopy. This leaflet will explain the procedure and what to expect on the
Endoscopy Unit Having a Colonoscopy A guide to the test Outpatient information Your doctor has recommended that you have a colonoscopy. This leaflet will explain the procedure and what to expect on the
GASTROSCOPY. Travelling to London Bridge Hospital A GUIDE FOR PATIENTS. Please ensure you read this booklet as it contains important information
 Travelling to London Bridge Hospital Directions: London Bridge Hospital is situated on the south side of the River Thames. We are next to London Bridge mainline and underground stations with easy access
Travelling to London Bridge Hospital Directions: London Bridge Hospital is situated on the south side of the River Thames. We are next to London Bridge mainline and underground stations with easy access
Flexible Sigmoidoscopy Inpatients
 PATIENT INFORMATION Flexible Sigmoidoscopy Inpatients Your doctor has requested this procedure to help investigate your medical condition to aid your diagnosis and management. This booklet has been written
PATIENT INFORMATION Flexible Sigmoidoscopy Inpatients Your doctor has requested this procedure to help investigate your medical condition to aid your diagnosis and management. This booklet has been written
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology Department Patient information leaflet This leaflet informs you about the procedure known as a Percutaneous Transhepatic Cholangiogram
FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL)
 PATIENT PROCEDURE INFORMATION LEAFLET FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Flexible Sigmoidoscopy? A flexible sigmoidoscopy is a test which allows the Endoscopist to look directly at the
PATIENT PROCEDURE INFORMATION LEAFLET FLEXIBLE SIGMOIDOSCOPY (ENEMA ON ARRIVAL) 1 What is a Flexible Sigmoidoscopy? A flexible sigmoidoscopy is a test which allows the Endoscopist to look directly at the
Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Percutaneous Transhepatic Cholangiogram (PTC) and Biliary Stent Radiology This leaflet informs you about the procedure known
Having a lower gastrointestinal endoscopy (colonoscopy)
 Having a lower gastrointestinal endoscopy (colonoscopy) Patient name Appointment date Arrival time Endoscopy sessions run from 9am to 1pm and 1.30pm to 5pm. Every effort will be made to see you promptly
Having a lower gastrointestinal endoscopy (colonoscopy) Patient name Appointment date Arrival time Endoscopy sessions run from 9am to 1pm and 1.30pm to 5pm. Every effort will be made to see you promptly
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest
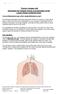 Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
UW MEDICINE PATIENT EDUCATION. Angiography: Percutaneous or Transjugular Liver Biopsy. How to prepare and what to expect. What is a liver biopsy?
 UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous or Transjugular Liver Biopsy How to prepare and what to expect This handout explains how to prepare and what to expect when having a percutaneous
UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous or Transjugular Liver Biopsy How to prepare and what to expect This handout explains how to prepare and what to expect when having a percutaneous
Having a Colonoscopy Information for Patients
 Endoscopy Team Information for Patients Having a Colonoscopy Information for Patients What is a Colonoscopy? A colonoscopy is a technique to look directly at the lining of the large bowel (colon) to try
Endoscopy Team Information for Patients Having a Colonoscopy Information for Patients What is a Colonoscopy? A colonoscopy is a technique to look directly at the lining of the large bowel (colon) to try
Endoscopy Department Patient Information Leaflet
 Having a flexible sigmoidoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Having a flexible sigmoidoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Endoscopy Department Patient Information Leaflet
 Having a Colonoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Having a Colonoscopy Endoscopy Department Patient Information Leaflet Your family doctor and/or hospital specialist has arranged for you to have this examination as this is the best way to investigate
Colonoscopy. Patient Information. Introduction
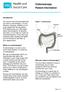 Colonoscopy Patient Information Introduction Your doctor has recommended that you have a colonoscopy. It is your decision, however, whether or not to go ahead with the procedure. This leaflet gives you
Colonoscopy Patient Information Introduction Your doctor has recommended that you have a colonoscopy. It is your decision, however, whether or not to go ahead with the procedure. This leaflet gives you
Skin Tunnelled Catheter (STC), also known as Central line
 Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Venous Sampling. Information for patients
 Venous Sampling Information for patients What is Venous Sampling? What is Venous Sampling? Venous sampling is a procedure that involves inserting a catheter (thin tube) into a specific vein or veins, taking
Venous Sampling Information for patients What is Venous Sampling? What is Venous Sampling? Venous sampling is a procedure that involves inserting a catheter (thin tube) into a specific vein or veins, taking
ERCP CONSENT TO EXAMINATION AND TREATMENT
 ENDOSCOPY DEPARTMENT Patient Information ERCP CONSENT TO EXAMINATION AND TREATMENT Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information
ENDOSCOPY DEPARTMENT Patient Information ERCP CONSENT TO EXAMINATION AND TREATMENT Endoscopy Unit North Wing Entrance 1 Dorset County Hospital Williams Avenue Dorchester DT1 2JY If you need this information
Gastroscopy and Varices
 Gastroscopy and Varices Patient information Leaflet October 2013 What is a Gastroscopy? The doctor is going to carry out a procedure called a gastroscopy to look at your gullet (food pipe) and stomach,
Gastroscopy and Varices Patient information Leaflet October 2013 What is a Gastroscopy? The doctor is going to carry out a procedure called a gastroscopy to look at your gullet (food pipe) and stomach,
Having a flexible sigmoidoscopy A guide for patients and their carers
 Having a flexible sigmoidoscopy A guide for patients and their carers Your information checklist: flexible sigmoidoscopy It is very important that you read this booklet. If you need further information
Having a flexible sigmoidoscopy A guide for patients and their carers Your information checklist: flexible sigmoidoscopy It is very important that you read this booklet. If you need further information
Flexible sigmoidoscopy and rectal bleeding clinic
 Flexible sigmoidoscopy and rectal bleeding clinic This leaflet will explain what will happen when you come to attend the One-stop Rectal Bleed Clinic. If you have any questions or concerns, please speak
Flexible sigmoidoscopy and rectal bleeding clinic This leaflet will explain what will happen when you come to attend the One-stop Rectal Bleed Clinic. If you have any questions or concerns, please speak
Chest Drain Insertion
 Chest Drain Insertion Information for Patients What is a chest drain? The insertion of a chest drain is a sterile procedure that involves placing a small drain through your skin into the space between
Chest Drain Insertion Information for Patients What is a chest drain? The insertion of a chest drain is a sterile procedure that involves placing a small drain through your skin into the space between
Having a lower GI endoscopy colonoscopy / flexible sigmoidoscopy
 Having a lower GI endoscopy colonoscopy / flexible sigmoidoscopy A guide to the test Information for patients Endoscopy Welcome to The Endoscopy Unit Sheffield Teaching Hospitals NHS Foundation Trust has
Having a lower GI endoscopy colonoscopy / flexible sigmoidoscopy A guide to the test Information for patients Endoscopy Welcome to The Endoscopy Unit Sheffield Teaching Hospitals NHS Foundation Trust has
UW MEDICINE PATIENT EDUCATION. Angiography: Percutaneous Gastrostomy. What to expect when you have a G-tube. What is a percutaneous gastrostomy?
 UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous Gastrostomy What to expect when you have a G-tube This handout explains a percutaneous gastrostomy tube and what to expect when you have one. What
UW MEDICINE PATIENT EDUCATION Angiography: Percutaneous Gastrostomy What to expect when you have a G-tube This handout explains a percutaneous gastrostomy tube and what to expect when you have one. What
UW MEDICINE PATIENT EDUCATION. How to prepare and what to expect DRAFT. What is an IVC filter?
 UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
PEG Tube (Percutaneous Endoscopic Gastrostomy)
 Patient & Family Guide 2017 PEG Tube (Percutaneous Endoscopic Gastrostomy) www.nshealth.ca PEG Tube What is a PEG tube? A PEG tube is a type of feeding tube. It is inserted (put in) by a GI specialist
Patient & Family Guide 2017 PEG Tube (Percutaneous Endoscopic Gastrostomy) www.nshealth.ca PEG Tube What is a PEG tube? A PEG tube is a type of feeding tube. It is inserted (put in) by a GI specialist
Colonoscopy. Please bring this booklet to your appointment with you.
 i Colonoscopy This booklet contains details about your appointment, information about the examination and preparation. Please bring this booklet to your appointment with you. If you need this information
i Colonoscopy This booklet contains details about your appointment, information about the examination and preparation. Please bring this booklet to your appointment with you. If you need this information
Flexible Sigmoidoscopy
 Flexible Sigmoidoscopy The procedure explained Please read this information leaflet carefully and bring it with you to your next appointment. Version Number: 3 Created: September 2014 Author: K Bridwell
Flexible Sigmoidoscopy The procedure explained Please read this information leaflet carefully and bring it with you to your next appointment. Version Number: 3 Created: September 2014 Author: K Bridwell
Stapling / Repair of Pharyngeal Pouch
 Patient information Stapling / Repair of Pharyngeal Pouch Ear, Nose and Throat Directorate PIF 1368 V2 Your consultant has advised that you have an operation to staple your pharyngeal pouch. A pharyngeal
Patient information Stapling / Repair of Pharyngeal Pouch Ear, Nose and Throat Directorate PIF 1368 V2 Your consultant has advised that you have an operation to staple your pharyngeal pouch. A pharyngeal
PATIENT INFORMATION FLEXIBLE SIGMOIDOSCOPY YOUR QUESTIONS ANSWERED
 PATIENT INFORMATION ON FLEXIBLE SIGMOIDOSCOPY YOUR QUESTIONS ANSWERED Page 1 of 8 Page 2 of 8 Your consultant has recommended that you have a flexible sigmoidoscopy to view the left side of your large
PATIENT INFORMATION ON FLEXIBLE SIGMOIDOSCOPY YOUR QUESTIONS ANSWERED Page 1 of 8 Page 2 of 8 Your consultant has recommended that you have a flexible sigmoidoscopy to view the left side of your large
Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test)
 South Tyneside NHS Foundation Trust Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test) GI Services Endoscopy Day Ward Outpatients Department Providing a range of NHS services in
South Tyneside NHS Foundation Trust Having an Oesophageal Manometry and 24-hour ph Test (a guide to the test) GI Services Endoscopy Day Ward Outpatients Department Providing a range of NHS services in
Mediastinal Venogram and Stent Insertion
 Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Colonoscopy. Endoscopy Department. Patient information leaflet
 Colonoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a colonoscopy, including the benefits, risks and any alternatives and what you can expect when you come
Colonoscopy Endoscopy Department Patient information leaflet This leaflet explains more about having a colonoscopy, including the benefits, risks and any alternatives and what you can expect when you come
Direct access flexible sigmoidoscopy
 Direct access flexible sigmoidoscopy What to expect Information for patients Endoscopy Why has my GP referred me for a direct access flexible sigmoidoscopy? Your General Practitioner (GP) has referred
Direct access flexible sigmoidoscopy What to expect Information for patients Endoscopy Why has my GP referred me for a direct access flexible sigmoidoscopy? Your General Practitioner (GP) has referred
Endoscopy Suite Patient Information
 Having a flexible sigmoidoscopy Endoscopy Suite Patient Information Contents Introduction 1 What is a flexible sigmoidoscopy? 1 What preparation will I need for my flexible sigmoidoscopy? 2 What should
Having a flexible sigmoidoscopy Endoscopy Suite Patient Information Contents Introduction 1 What is a flexible sigmoidoscopy? 1 What preparation will I need for my flexible sigmoidoscopy? 2 What should
Transjugular Liver Biopsy About your procedure
 Patient Education Transjugular Liver Biopsy About your procedure This handout explains what a transjugular liver biopsy is and what to expect when you have this procedure. What is a liver biopsy? In a
Patient Education Transjugular Liver Biopsy About your procedure This handout explains what a transjugular liver biopsy is and what to expect when you have this procedure. What is a liver biopsy? In a
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
 Information for parents This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about a colonoscopy
Information for parents This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about a colonoscopy
Mediastinal Venogram and Stent Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Flexible Sigmoidoscopy with an Enema
 Flexible Sigmoidoscopy with an Enema You must read this booklet at least seven days before your test Contents Page What is a flexible sigmoidoscopy? 1 Preparing yourself for a flexible sigmoidoscopy 2
Flexible Sigmoidoscopy with an Enema You must read this booklet at least seven days before your test Contents Page What is a flexible sigmoidoscopy? 1 Preparing yourself for a flexible sigmoidoscopy 2
Patient Information. Having a Laparoscopy
 Patient Information Having a Laparoscopy This information has been written to explain your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions you
Patient Information Having a Laparoscopy This information has been written to explain your operation, and the benefits and risks. The medical and nursing staff will be happy to answer any questions you
Contents. Welcome to the Cath Lab P4/5
 Contents Welcome to the Cath Lab Preparation Instructions : information to ensure you are ready for your procedure in the Cath Lab, set out for you as questions (Q) and answers (A) How the day will go
Contents Welcome to the Cath Lab Preparation Instructions : information to ensure you are ready for your procedure in the Cath Lab, set out for you as questions (Q) and answers (A) How the day will go
Having a blue light cystoscopy
 Having a blue light cystoscopy The aim of this information sheet is to help answer some of the questions you may have about having a blue light cystoscopy. It explains the benefits, risks and alternatives
Having a blue light cystoscopy The aim of this information sheet is to help answer some of the questions you may have about having a blue light cystoscopy. It explains the benefits, risks and alternatives
Partial glossectomy. Your operation explained. Information for patients Head and Neck Centre
 Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Percutaneous Gastrostomy G-tube, or stomach feeding tube
 Patient Education Percutaneous Gastrostomy G-tube, or stomach feeding tube This handout explains what percutaneous gastrostomy is and what to expect when you have one. What is a gastrostomy tube? A gastrostomy
Patient Education Percutaneous Gastrostomy G-tube, or stomach feeding tube This handout explains what percutaneous gastrostomy is and what to expect when you have one. What is a gastrostomy tube? A gastrostomy
Inferior Vena Cava (IVC) Filter Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Having a Vena Cava Filter
 Having a Vena Cava Filter Department of Radiology Information for Patients i Radiology Leaflet No. 30 Contents Page number Introduction 3 Referral and consent 3 Why do I need a vena cava filter inserted?
Having a Vena Cava Filter Department of Radiology Information for Patients i Radiology Leaflet No. 30 Contents Page number Introduction 3 Referral and consent 3 Why do I need a vena cava filter inserted?
Peripherally Inserted Central Catheter (PICC)
 University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
OSPIDÉAL NAOIMH SÉAMAS ST. JAMES S HOSPITAL
 OSPIDÉAL NAOIMH SÉAMAS ST. JAMES S HOSPITAL Ospidéal Naomh Séamus, Sráid Shéamais, Baile Átha Cliath 8. St. James s Hospital, James s Street, Dublin 8. + 353 1 410 3000 xxx.stjames.ie Endoscopy Unit Route
OSPIDÉAL NAOIMH SÉAMAS ST. JAMES S HOSPITAL Ospidéal Naomh Séamus, Sráid Shéamais, Baile Átha Cliath 8. St. James s Hospital, James s Street, Dublin 8. + 353 1 410 3000 xxx.stjames.ie Endoscopy Unit Route
Functional Endoscopic Sinus Surgery (FESS)
 Patient information Functional Endoscopic Sinus Surgery (FESS) Ear, Nose and Throat Directorate PIF 232 V7 Your Consultant / Doctor has advised you to have Functional Endoscopic Sinus Surgery (FESS). What
Patient information Functional Endoscopic Sinus Surgery (FESS) Ear, Nose and Throat Directorate PIF 232 V7 Your Consultant / Doctor has advised you to have Functional Endoscopic Sinus Surgery (FESS). What
Endoscopy Unit Colonic Stent insertion
 Endoscopy Unit Colonic Stent insertion Information for patients Your doctor has recommended that you have a Colonic Stent Insertion. This leaflet will explain the procedure and what to expect on the day
Endoscopy Unit Colonic Stent insertion Information for patients Your doctor has recommended that you have a Colonic Stent Insertion. This leaflet will explain the procedure and what to expect on the day
Having a flexible sigmoidoscopy
 Having a flexible sigmoidoscopy +/- banding of haemorrhoids Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on Other formats If you need this information
Having a flexible sigmoidoscopy +/- banding of haemorrhoids Gemini Endoscopy Suite Tel: 01271 349180 Patients name:.. Hospital No: Your appointment is at. on Other formats If you need this information
A Patient s Guide to Surgery
 A Patient s Guide to Surgery Welcome Welcome to Carolinas Medical Center-NorthEast. Our staff of skilled professionals look forward to providing the care you need. We want your stay to be pleasant and
A Patient s Guide to Surgery Welcome Welcome to Carolinas Medical Center-NorthEast. Our staff of skilled professionals look forward to providing the care you need. We want your stay to be pleasant and
Having a portacath insertion in the x-ray department
 Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Local Anaesthesia for your eye operation. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Local Anaesthesia for your eye operation An information guide Local Anaesthesia for your eye operation Introduction You and your doctor
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Local Anaesthesia for your eye operation An information guide Local Anaesthesia for your eye operation Introduction You and your doctor
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet
 Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Tenckhoff Catheter Insertion
 Tenckhoff Catheter Insertion Information for patients with chronic kidney disease (CKD) who have chosen to have peritoneal dialysis Renal Directorate Produced: May 2010 Review date: May 2012 This leaflet
Tenckhoff Catheter Insertion Information for patients with chronic kidney disease (CKD) who have chosen to have peritoneal dialysis Renal Directorate Produced: May 2010 Review date: May 2012 This leaflet
Rectal prolapse. Information for patients General Surgery
 Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Removal of Corflo Percutaneous Endoscopic Gastrostomy - PEG Tube
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Removal of Corflo Percutaneous Endoscopic Gastrostomy - PEG Tube Nursing and Clinical Governance The purpose of this leaflet
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Removal of Corflo Percutaneous Endoscopic Gastrostomy - PEG Tube Nursing and Clinical Governance The purpose of this leaflet
Children s Ward Parent/Carer Information Leaflet
 Operation to remove tonsils Children s Ward Parent/Carer Information Leaflet Introduction Your child s consultant has suggested that your child has an operation to remove their tonsils. This leaflet explains
Operation to remove tonsils Children s Ward Parent/Carer Information Leaflet Introduction Your child s consultant has suggested that your child has an operation to remove their tonsils. This leaflet explains
Cardiac catheterisation. Cardiology Department Patient Information Leaflet
 Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
About your PICC line. Information for patients Weston Park Hospital
 About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
Fistula in ano. Information for patients General Surgery
 Fistula in ano Information for patients General Surgery Please bring this booklet with you to your pre-operative assessment appointment and when you are admitted to hospital to Theatre Admissions Unit
Fistula in ano Information for patients General Surgery Please bring this booklet with you to your pre-operative assessment appointment and when you are admitted to hospital to Theatre Admissions Unit
