In This Issue. Issue: 8. Codes Utilization FAQs Harry s Health Highlights. Who s Harry? HEDIS News
|
|
|
- Jessica Johnston
- 6 years ago
- Views:
Transcription
1 Issue: 8 Who s Harry? Born from the mists of success, and integrated into the core of our measures; Harry forges forward in an undying quest to bring H knowledge to Cenpatico s provider network. In This Issue H News Codes Utilization FAQs Harry s Health Highlights Value Added Dental Benefits Six Month Work Training Program H I New S s Cenpatico Integrated Care is very excited to announce an innovative approach to assisting Integrated Care members address their oral health care and dental needs. Adults over the age of 20 with an SMI qualifying diagnosis are eligible for preventative dental services through a prior-authorized process once they complete the six month work training program with their assigned Employment Specialists. The training program is accessed through Relias Learning Systems. Integrated Members employed 1/4 time (10 hours per/week) and/or transition age young adults are eligible for this benefit without completing the training program Who: Any TXIX adult members receiving integrated care (RBHA 79) With a qualifying diagnosis of a Serious Mental Illness (SMI) Who complete a six-month pre-job training program What: Oral Health includes medically necessary dental services including emergency dental services, dental screening and preventive services in accordance with AHCCCS Dental Periodicity Schedule. Prior Authorization for these services is required. When: Value added benefit will become effective on the 1st of the month following acceptance of the demographic record with a qualifying employment code. Length of eligible benefit is 1 year and tracked by Relias Learning Systems. Eligible adults may be granted one additional year following completion of a second training program. Where: Training program is accessed on the Relias Learning Systems under 6 Month Pre-Employment Work Program (Value Added Dental Benefit). Members should partner with the ICC Agency s Employment Specialist to register and start training. Cenpatico Integrated Care (Cenpatico IC) services are funded through a contract with the Arizona Department of Health Services and AHCCCS.
2 Codes! Welcome to the special code issue of Harry s H Hints! The purpose of this issue is to identify commonly used codes to meet some of the contracted performance measures. This is not billing advice. The H measures are split into two tables, standard and utilization. The standard measures have codes included in the specifications that meet the measure. Utilization measures are run through inclusive/exclusive events. For details on how the measures are calculated, please refer to prior issues of Harry s H Hints or the DBHS BQ&I Specification Manual. Breast Cancer Screening Women age 50-74: A mammogram Bilateral Mastectomy Cervical Cancer Screening Women age 21-64: A PAP test (cervical cytology) Women age 30-64: HPV test & a PAP test (cervical cytology) on the same day Cervical cytology: , , 88150, , , Cervical cytology: , , 88150, , , HPV tests: Hysterectomy with no residual cervix Documentation of complete, total or radical abdominal or vaginal hysterectomy meets the criteria. Documentation of hysterectomy alone does not meet the criteria Hysterectomy with no residual cervix Chlamydia Screening Women age and identified as sexually active (by claims or pharmacy data) Documentation of complete, total or radical abdominal or vaginal hysterectomy meets the criteria. Documentation of hysterectomy alone does not meet the criteria 87110,87270,87320, ,87810 Documentation of total hysterectomy with absence of cervix
3 ! es Cod Comprehensive Diabetes Care Adults age with diabetes (type 1 or type 2) , , , , 9341,99345,99347,99350, , , ,99411,99412, 99420, 99429,99455,99456 Members without a diagnosis of diabetes, but with either: Gestational diabetes or Steroid-induced diabetes Comprehensive Diabetes Care: HbA1c The percentage of members age 83036, 83037, 3045F,3044F with diabetes (Type 1 or type 2) who had a Hemoglobin A1c Test Gestational diabetes, steroid induced diabetes Comprehensive Diabetes Care: Retinal Eye Exam Most recent date of dilated eye exam 67028,67030,67031,67036, 67039,67040,67041, 67041,67043,67101,67105,67107, 67108,67110,67112, 67113, 57141,67145,672118,67220, 67221,67227,67228,92002, 92004,92012,92014,92018, 92019, ,92226, 92227,92228,92230,92250, Gestational diabetes, steroid induced diabetes Adult Access to Preventive Care Adults age 20 or older: An ambulatory or preventive care visit 99201,99202,99203,99204, 99205,99211,99212,99213, 99214,99215,99241,99242, 99243,99244,99245,99341, 99343,99244,99245,99347, 99348,99349,99350,99373, 99381,99382,99384,99386, 99387,99391,99392,99393, None 57170,58300,59430,99501, 0503F Deliveries not resulting in a live birth Postpartum Care Deliveries with a postpartum visit on or between 21 and 56 days after delivery
4 ! es Cod Timeliness of Prenatal Care Deliveries that received 59400,59425,59426,59510, 59610,59618 prenatal care in the first trimester or within first 42 days of enrollment Deliveries not resulting in a live birth Influenza Vaccine Age Age 65 and older 90654,90655,90656,90658, 90672,90673,90686,90688, 90630,90661 None 90654,90655,90656,90658, 90686,90688,90673,90662, None 99383,-99385, None D0120,D0140,D0145,D0150, D0160,D0171,D0180,D0210, D0220,D0230,D0240,D0250, D0260,D0270,D0272,D0273, D0274,D0277,D0290,D0310, D0320,D0321,D0330,D0340, D0350,D0393,D0470,D0502, D0999,D1110,D1120,D1206, D1208,D1351,D1352,D1353, D1354,D1510,D1515,D1520, D1525,D1550,D1555,D1999 None EPSDT Adults age 18, 19, and 20 who had at least one well visit Dental Adults age 18, 19, and 20 who had at least one preventative dental service
5 n atio iz Util The following information is to help guide your understanding of Utilization Measures. These are calculated differently than the standard measures because utilization measures are reported per member months or as a rate, instead of percent compliant. Inpatient and Utilization measures are listed as per 1,000 member months (mm), while the rest of the utilization measures are listed as per 100,000mm. Reporting these measures in this manner is normalizing, meaning the numbers can be compared across different agencies or plans of varying sizes. The charts below identify criteria from the specification requirements that would either include or exclude a member from each measure. For more information regarding specific measures, please refer to previous issues of Harry s H Hints! Inpatient Utilization (days/1,000 member months) This measure is the number of total inpatient days. Unspecified Emergency Department () Utilization (visits/1,000 member months) This measure is the number of emergency department visits Unspecified Plan All-Cause Hospital (readmissions within 30 days of discharge) This measure is the number of hospital discharges that were followed by a readmission for any diagnosis within 30 days The member died during the stay A principal diagnosis of pregnancy A principal diagnosis of a condition originating in the perinatal period Adult Asthma Admission Rate (discharges/1,000 member months) This measure is members who had a hospital stay due to asthma Transfer from a hospital (different facility) Transfer from a Skilled Nursing Facility (SNF) or Intermediate Care Facility (ICF) Transfer from another health care facility Pregnancy, childbirth, and puerperium With any diagnosis code of cystic fibrosis and anomalies of the respiratory system
6 Utilization Use of Appropriate Medications for People with Asthma (ASM) This measure is the number of members identified as having persistent Asthma and were appropriately prescribed medication Exclude members who had any diagnosis from any of the following groups, any time during the member s history through the measurement year: Emphysema Other Emphysema COPD Obstructive Chronic Bronchitis Chronic Respiratory Conditions Due To Fumes/Vapors Cystic Fibrosis Follow-up After Hospitalization (all cause within 7 days) This measure is the number of members who were hospitalized and received a 7 day follow up after discharge with their provider Follow-up After Hospitalization (all cause within 30 days) This measure is the number of members who were hospitalized and received a 30 follow up after discharge with their provider Acute Respiratory Failure Exclude discharges followed by readmission or direct transfer to a non-acute inpatient care setting within the 30-day follow-up period, regardless of principal diagnosis for the readmission. To identify readmissions to a nonacute inpatient care setting: Identify all acute and non-acute inpatient stays Confirm the stay was for non-acute care based on the presence of a non-acute code on the claim Identify the admission date for the stay Exclude discharges followed by readmission or direct transfer to a non-acute inpatient care setting within the 30-day follow-up period, regardless of principal diagnosis for the readmission. To identify readmissions to a non-acute inpatient care setting: Identify all acute and non-acute inpatient stays Confirm the stay was for non-acute care based on the presence of a non-acute code on the claim Identify the admission date for the stay
7 n atio iz Util Diabetes Admissions, Short-Term Complications (discharges/100,000 member months) This measure is the number of inpatient hospital admissions for diabetes short-term complications (ketoacidosis, hyperosmolarity, or coma) Transfer from a hospital (different facility), a Skilled Nursing Facility (SNF) or Intermediate Care Facility (ICF), or another health care facility Obstetric admissions Chronic Obstructive Pulmonary Disease (COPD) Admissions (discharges/100,000 member months) This measure is the number of members with COPD (including chronic bronchitis or emphysema) who go to the ER or are hospitalized with a primary diagnosis of COPD Preventative measure only Congestive Heart Failure Admissions (discharges/100,000 member months) This measure is the number of discharges of members with a diagnosis of Congestive Heart Failure Transfer from a hospital (different facility), a Skilled Nursing Facility (SNF) or Intermediate Care Facility (ICF), or another health care facility Obstetric admissions
8 y Harr SEZ Harry SEZ (Frequently Asked Questions) Please send your questions about H to Tony DeQuinzio, our H contact. Call ( x84452) or Tony (ADeQuinzio@Cenpatico.com) with your question and we ll post it and his answer under the next edition of HARRY S H HINTS in the Harry SEZ section. We look forward to responding to your questions in the newsletter! Q. Why are there members that qualify for a H measure but are not on the non-compliant list? A. There are 2 reasons why a qualified member would not show up on the non-compliant list. The first reason would be that the member is compliant with the measure. The second reason would be that the member is not assigned to the correct agency and could be listed on a different agency s non-compliant list or is not assigned. If a member is showing on your non-compliant list and is not enrolled with your agency, verify demographic information and contact Cenpatico-IC Member Services to report the discrepancy at CAZmembership@cenpatico.com. Q. How many times should our agency do outreach to a member for a H service? Is one outreach attempt all that is needed? A. Your agency should have an outreach plan and goals for members with gaps in H care services. Outreach attempts continue until the member has received the required services. All outreach attempts must be recorded in the EHR or logged for quarterly reporting to Cenpatico-IC. Q. Does Cenpatico-IC require that member outreach be completed by a RC/DRC? A. Member outreach can be completed by anyone on the integrated care team. Receptionists, peers, medical assistants, community health workers, RNs/LPNs and anyone on the team who communicates directly with member can be effective in completing outreach. Q. Do denied claims count toward meeting my agency s H score targets? What about claims billed by other agencies or specialists? A. Pended, denied and approved claims all count toward a positive H score for the measures that are currently reported on. All claims that Cenpatico-IC receives count towards the measure for the member regardless of who initiated the claim.
9 Harry s Health Highlights Minority Health Determines the Health of the Nation The United States is increasingly diverse: 36 percent of the population belongs to a racial or ethnic minority group (2010 census). Life expectancy and infant mortality have improved for most Americans. However, minorities experience a disproportionate burden of preventable diseases, deaths, and disabilities compared with non-minorities. The overarching goal of CDC Healthy People 2020 is to achieve health equity, eliminate disparities, and improve the health of all groups.
10 Harry s Health Highlights What is Health Equity? All people have an opportunity to attain full health potential regardless of their social position or other socially determined circumstances. What are Social Determinants of Health? Poverty, unemployment, education, urban/rural, race, ethnicity and other determinants shaped by social distribution of money, power and resources. What is Health Disparity? A difference in presence of disease, health outcomes, or access to health care between populations. This can include a different race, ethnicity, socioeconomic status, gender, sexual orientation, mental health, sexual orientation, geographic location or cognitive, sensory or physical disability As a result of social or economic disadvantage stemming from historical discrimination or exclusion
11 Harry s Health Highlights How does Quality of Care affect Health Disparities? Communication is critical for the delivery of appropriate and effective treatment and care o It is linked with improved patient satisfaction which can lead to improved health outcomes o Miscommunication can lead to incorrect diagnosis, improper use of medications, and failure to receive follow-up care. This can result in poor medical compliance, poor health outcomes, and greater medical expenditures. o 19% of the time minority patients have problems understanding the doctor, feeling the doctor listened, and had questions but did not ask o 33% of the time the Hispanic population had problems communicating with their provider o Less than half of non-english speakers who say they need an interpreter during clinical visits report having one o Inability of providers to communicate with Limited English Proficiency (LEP) patients leads to more diagnostic procedures, more invasive procedures, and over prescribing of medications o Providers need to assess patients health beliefs and practices to understand a patients view of health and disease for improved diagnosis and treatment o Patient health decisions (screening and medication compliance) are influenced by religious beliefs, mistrust of Western medicine, and familial and hierarchical roles Provider discrimination (unconsciously or consciously) occurs when health care providers treat certain patients differently from other patients using stereotypes o Racial/ethnic group stereotypes; heterosexist attitude towards LGBT patients and lack of understanding Lack of access to preventive care: o Limited English Proficiency (LEP) patients are less likely to receive preventive health services such as mammograms o Use of professional interpreters significantly reduces disparities in the rates of fecal occult testing, flu immunizations and pap smears How to achieve Health Equity Advocacy: Promote policy change that supports provider knowledge transfer and uptake and targets the specific population and social context Increase provider awareness: Recognize health disparities in ethnic and minority populations and teach on how to reduce it Use AIM ability, incentives, and management feedback: Successfully reduce care disparity in providers through (1) training to enhance ability, (2) monetary incentives to enhance motivation, and (3) management feedback to enhance accountability
HEDIS TOOLKIT FOR PROVIDER OFFICES. A Guide to Understanding Medicaid Measure Compliance
 HEDIS TOOLKIT FOR PROVIDER OFFICES A Guide to Understanding Medicaid Measure Compliance TABLE OF CONTENTS WHAT IS HEDIS 1?... 1 ANNUAL HEDIS TIMELINE... 2 HEDIS MEDICAL RECORD REQUEST PROCESS:... 2 TIPS
HEDIS TOOLKIT FOR PROVIDER OFFICES A Guide to Understanding Medicaid Measure Compliance TABLE OF CONTENTS WHAT IS HEDIS 1?... 1 ANNUAL HEDIS TIMELINE... 2 HEDIS MEDICAL RECORD REQUEST PROCESS:... 2 TIPS
and HEDIS Measures
 1 SC Medicaid Managed Care Initiative and HEDIS Measures - 2009 Ana Lòpez De Fede, PhD Institute for Families in Society University of South Carolina Regina Young, RNC SC Department of Health and Human
1 SC Medicaid Managed Care Initiative and HEDIS Measures - 2009 Ana Lòpez De Fede, PhD Institute for Families in Society University of South Carolina Regina Young, RNC SC Department of Health and Human
Oregon's Health System Transformation
 Oregon's Health System Transformation MEASUREMENT PERIOD Baseline Year 2011 and Calendar Year 2013 JUNE 24, 2014 TABLE OF CONTENTS Executive Summary...iii 2013 CCO Performance and Quality Pool Distribution...1
Oregon's Health System Transformation MEASUREMENT PERIOD Baseline Year 2011 and Calendar Year 2013 JUNE 24, 2014 TABLE OF CONTENTS Executive Summary...iii 2013 CCO Performance and Quality Pool Distribution...1
At the start of each HEDIS season, you will receive a fax from L.A. Care. Each fax request will stipulate what documents need to be faxed back.
 Office Manager s Guide to HEDIS 2018 L.A. CARE MEDICAL RECORD REQUESTS At the start of each HEDIS season, you will receive a fax from L.A. Care. Each fax request will stipulate what documents need to be
Office Manager s Guide to HEDIS 2018 L.A. CARE MEDICAL RECORD REQUESTS At the start of each HEDIS season, you will receive a fax from L.A. Care. Each fax request will stipulate what documents need to be
Enhancing Outcomes with Quality Improvement (QI) October 29, 2015
 Enhancing Outcomes with Quality Improvement (QI) October 29, 2015 Learning Objectives! Introduce Quality Improvement (QI)! Explain Clinical Performance Person-Centered Medical Home (PCMH) Measures! Implement
Enhancing Outcomes with Quality Improvement (QI) October 29, 2015 Learning Objectives! Introduce Quality Improvement (QI)! Explain Clinical Performance Person-Centered Medical Home (PCMH) Measures! Implement
Instructions for Accessing the Secure Portal and the Verification Process
 Instructions for Accessing the Secure Portal and the Verification Process Community Checkup report: www.wacommunitycheckup.org More about the Alliance: www.wahealthalliance.org 1 Contents Overview... 3
Instructions for Accessing the Secure Portal and the Verification Process Community Checkup report: www.wacommunitycheckup.org More about the Alliance: www.wahealthalliance.org 1 Contents Overview... 3
Community Analysis Summary Report for Clinical Care
 Community Analysis Summary Report for Clinical Care BACKGROUND ABOUT THE HEALTHY COMMUNITY STUDY The Rockford Health Council (RHC) exists to build and improve community health in the region. To address
Community Analysis Summary Report for Clinical Care BACKGROUND ABOUT THE HEALTHY COMMUNITY STUDY The Rockford Health Council (RHC) exists to build and improve community health in the region. To address
QUALITY IMPROVEMENT. Molina Healthcare has defined the following goals for the QI Program:
 QUALITY IMPROVEMENT Molina Healthcare maintains an active Quality Improvement (QI) Program. The QI program provides structure and key processes to carry out our ongoing commitment to improvement of care
QUALITY IMPROVEMENT Molina Healthcare maintains an active Quality Improvement (QI) Program. The QI program provides structure and key processes to carry out our ongoing commitment to improvement of care
Fast Facts 2018 Clinical Integration Performance Measures
 IMPORTANT: LHP providers who do not achieve a minimum CI Score in 2018 will not be eligible for incentive distribution and will be placed on a monitoring plan for the 2019 performance year. For additional
IMPORTANT: LHP providers who do not achieve a minimum CI Score in 2018 will not be eligible for incentive distribution and will be placed on a monitoring plan for the 2019 performance year. For additional
PROVIDER NEWSLETTER Spring 2016
 PROVIDER NEWSLETTER Spring 2016 IN THIS ISSUE: Recover Wellness Program Overview Integrated Care Success Stories HEDIS Measures Respite Care Policy Updates Health Choice Integrated Care Becomes the Regional
PROVIDER NEWSLETTER Spring 2016 IN THIS ISSUE: Recover Wellness Program Overview Integrated Care Success Stories HEDIS Measures Respite Care Policy Updates Health Choice Integrated Care Becomes the Regional
QUALITY IMPROVEMENT. Articles of Importance to Read: Quality Improvement Program. Winter Pages 1, 2, 3, 4 and 5 Quality Improvement
 Important information for physicians and other health care professionals and facilities serving UnitedHealthcare Medicaid members Winter 2009 QUALITY IMPROVEMENT Quality Improvement Program The Quality
Important information for physicians and other health care professionals and facilities serving UnitedHealthcare Medicaid members Winter 2009 QUALITY IMPROVEMENT Quality Improvement Program The Quality
Gateway to Practitioner Excellence GPE 2017 Medicaid & Medicare
 Gateway to Practitioner Excellence GPE 2017 Medicaid & Medicare Recognizing and Rewarding Excellent Practices Improving the Health of Gateway Members PRACTICE ELIGIBILITY (see PCMH slide #27 for separate
Gateway to Practitioner Excellence GPE 2017 Medicaid & Medicare Recognizing and Rewarding Excellent Practices Improving the Health of Gateway Members PRACTICE ELIGIBILITY (see PCMH slide #27 for separate
ALL NEW ALOHACARE WEBSITE
 NEWS FOR PHYSICIANS AND PROVIDERS QUARTER 4 2017 NEW STREAMLINED PRIOR AUTHORIZATION PROCESS AlohaCare will implement a simplified and reduced list of services requiring Prior Authorization effective January
NEWS FOR PHYSICIANS AND PROVIDERS QUARTER 4 2017 NEW STREAMLINED PRIOR AUTHORIZATION PROCESS AlohaCare will implement a simplified and reduced list of services requiring Prior Authorization effective January
Communicator. the JUST A THOUGHT. Ensuring HEDIS-Compliant Preventive Health Services. Provider Portal Features. Peer-to-Peer Review BY DR.
 WINTER 2016 MHS NEWSLETTER FOR PHYSICIANS Ensuring HEDIS-Compliant Preventive Health Services Here are a few best practice strategies for raising HEDIS and EPSDT onsite review scores, as demonstrated by
WINTER 2016 MHS NEWSLETTER FOR PHYSICIANS Ensuring HEDIS-Compliant Preventive Health Services Here are a few best practice strategies for raising HEDIS and EPSDT onsite review scores, as demonstrated by
2015 Member Incentive. Program Evaluation. Our mission is to improve the health and quality of life of our members
 25 Member Incentive Program Evaluation Our mission is to improve the health and quality of life of our members 25 Member Incentive Program Evaluation Annual Participation Rate Program Title: Member Incentive
25 Member Incentive Program Evaluation Our mission is to improve the health and quality of life of our members 25 Member Incentive Program Evaluation Annual Participation Rate Program Title: Member Incentive
2016 Member Incentive. Program Descriptions. Our mission is to improve the health and quality of life of our members
 2016 Member Incentive Program Descriptions Our mission is to improve the health and quality of life of our members Member Incentive Program Descriptions I. Purpose Passport Health Plan (Passport) has developed
2016 Member Incentive Program Descriptions Our mission is to improve the health and quality of life of our members Member Incentive Program Descriptions I. Purpose Passport Health Plan (Passport) has developed
Kaiser Permanente Group Plan 301 Benefit and Payment Chart
 301 Kaiser Permanente Group Plan 301 Benefit and Payment Chart 10119 CITY AND COUNTY OF SAN FRANCISCO About this chart This benefit and payment chart: Is a summary of covered services and other benefits.
301 Kaiser Permanente Group Plan 301 Benefit and Payment Chart 10119 CITY AND COUNTY OF SAN FRANCISCO About this chart This benefit and payment chart: Is a summary of covered services and other benefits.
Assistance. Improving. Consumer Health. Strategies for
 Assistance Strategies for Improving Consumer Health A resource to help educate consumers about available preventive health incentives and eliminating barriers to receiving care www.bhpi.org www.healthsharesolutions.org
Assistance Strategies for Improving Consumer Health A resource to help educate consumers about available preventive health incentives and eliminating barriers to receiving care www.bhpi.org www.healthsharesolutions.org
Quality Measurement Approaches of State Medicaid Accountable Care Organization Programs
 TECHNICAL ASSISTANCE TOOL September 2014 Quality Measurement Approaches of State Medicaid Accountable Care Organization Programs S tates interested in using an accountable care organization (ACO) model
TECHNICAL ASSISTANCE TOOL September 2014 Quality Measurement Approaches of State Medicaid Accountable Care Organization Programs S tates interested in using an accountable care organization (ACO) model
Practice Improvement Program 2014 Program Guide
 Practice Improvement Program 2014 Program Guide Measure Set for NEMS & CCHCA Application due: January 31, 2014 Contacts: Lauren Baehner, Project Manager, Practice Improvement Program 415 615 4284 Lbaehner@sfhp.org
Practice Improvement Program 2014 Program Guide Measure Set for NEMS & CCHCA Application due: January 31, 2014 Contacts: Lauren Baehner, Project Manager, Practice Improvement Program 415 615 4284 Lbaehner@sfhp.org
Benefits. Benefits Covered by UnitedHealthcare Community Plan
 Benefits Covered by UnitedHealthcare Community Plan As a member of UnitedHealthcare Community Plan, you are covered for the following MO HealthNet Managed Care services. (Remember to always show your current
Benefits Covered by UnitedHealthcare Community Plan As a member of UnitedHealthcare Community Plan, you are covered for the following MO HealthNet Managed Care services. (Remember to always show your current
2015 DUPLIN COUNTY SOTCH REPORT
 2015 DUPLIN COUNTY SOTCH REPORT Reported March 2016 State of the County Health Report The State of the County Health Report provides a review of the current county health statistics and compares them to
2015 DUPLIN COUNTY SOTCH REPORT Reported March 2016 State of the County Health Report The State of the County Health Report provides a review of the current county health statistics and compares them to
2016 Mommy Steps Program Descriptions
 2016 Mommy Steps Program Descriptions Our mission is to improve the health and quality of life of our members Mommy Steps Program Descriptions I. Purpose Passport Health Plan (Passport) has developed approaches
2016 Mommy Steps Program Descriptions Our mission is to improve the health and quality of life of our members Mommy Steps Program Descriptions I. Purpose Passport Health Plan (Passport) has developed approaches
NCQA s Patient-Centered Medical Home (PCMH) 2011 Standards 11/21/11
 NCQA s Patient-Centered Medical Home (PCMH) 2011 Standards 11/21/11 28 PCMH 1: Enhance Access and Continuity PCMH 1: Enhance Access and Continuity 20 points provides access to culturally and linguistically
NCQA s Patient-Centered Medical Home (PCMH) 2011 Standards 11/21/11 28 PCMH 1: Enhance Access and Continuity PCMH 1: Enhance Access and Continuity 20 points provides access to culturally and linguistically
Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION
 Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION 2019 Summary of Important Changes for Contract Renewals for the Kaiser Permanente Group Plan (These changes are subject to regulatory
Kaiser Foundation Health Plan, Inc. A NONPROFIT HEALTH PLAN - HAWAII REGION 2019 Summary of Important Changes for Contract Renewals for the Kaiser Permanente Group Plan (These changes are subject to regulatory
Patient-Centered Specialty Practice (PCSP) Recognition Program
 Patient-Centered Specialty Practice (PCSP) Recognition Program Standards Workshop Part 2 2013 All materials 2013, National Committee for Quality Assurance Agenda Part 1 Content of PCSP Standards and Guidelines
Patient-Centered Specialty Practice (PCSP) Recognition Program Standards Workshop Part 2 2013 All materials 2013, National Committee for Quality Assurance Agenda Part 1 Content of PCSP Standards and Guidelines
2012 QUALITY ASSURANCE ANNUAL REPORT Executive Summary
 2012 QUALITY ASSURANCE ANNUAL REPORT Executive Summary Jai Medical Systems Managed Care Organization, Inc. (JMS) and its providers have closed out their fifteenth full year in the Maryland Medicaid HealthChoice
2012 QUALITY ASSURANCE ANNUAL REPORT Executive Summary Jai Medical Systems Managed Care Organization, Inc. (JMS) and its providers have closed out their fifteenth full year in the Maryland Medicaid HealthChoice
Fact Sheet: Stratifying Quality Measures BY RACE, ETHNICITY, PREFERRED LANGUAGE, AND COUNTRY OF ORIGIN
 MINNESOTA STATEWIDE QUALITY REPORTING AND MEASUREMENT SYSTEM Fact Sheet: Stratifying Quality Measures BY RACE, ETHNICITY, PREFERRED LANGUAGE, AND COUNTRY OF ORIGIN Overview Minnesota s 2008 Health Reform
MINNESOTA STATEWIDE QUALITY REPORTING AND MEASUREMENT SYSTEM Fact Sheet: Stratifying Quality Measures BY RACE, ETHNICITY, PREFERRED LANGUAGE, AND COUNTRY OF ORIGIN Overview Minnesota s 2008 Health Reform
QUALITY IMPROVEMENT PROGRAM
 QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
QUALITY IMPROVEMENT PROGRAM EmblemHealth s mission is to create healthier futures for our customers and communities. We will do this by providing members with a broad range of benefits and conscientious
HHW-HIPP0314 (9/13) MDwise Annual IHCP Seminar. Exclusively serving Indiana families since 1994.
 HHW-HIPP0314 (9/13) MDwise 101 2013 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda Indiana Health Coverage Overview MDwise Overview MDwise Hoosier Healthwise MDwise Healthy
HHW-HIPP0314 (9/13) MDwise 101 2013 Annual IHCP Seminar Exclusively serving Indiana families since 1994. Agenda Indiana Health Coverage Overview MDwise Overview MDwise Hoosier Healthwise MDwise Healthy
2013 Mommy Steps. Program Description. Our mission is to improve the health and quality of life of our members
 2013 Mommy Steps Program Description Our mission is to improve the health and quality of life of our members I. Purpose Passport Health Plan (PHP) has developed approaches to the management of members
2013 Mommy Steps Program Description Our mission is to improve the health and quality of life of our members I. Purpose Passport Health Plan (PHP) has developed approaches to the management of members
Quality Peer Group UDS Best Practices and Data Sharing 9/9/16. ohiochc.org
 1 Quality Peer Group UDS Best Practices and Data Sharing 9/9/16 ohiochc.org Presenters 2 Ashley Ballard Director of Clinical Quality Tiffany Blair Quality Improvement Coordinator Dr. Wymyslo Chief Medical
1 Quality Peer Group UDS Best Practices and Data Sharing 9/9/16 ohiochc.org Presenters 2 Ashley Ballard Director of Clinical Quality Tiffany Blair Quality Improvement Coordinator Dr. Wymyslo Chief Medical
Oregon Health Authority Key Performance Measures Biennium
 Oregon Health Authority Key Performance Measures 2017 2017 Biennium Presented to the Human Services Legislative Subcommittee on Ways and Means April 6, 2015 Leslie Clement, Chief of Policy Lori Coyner,
Oregon Health Authority Key Performance Measures 2017 2017 Biennium Presented to the Human Services Legislative Subcommittee on Ways and Means April 6, 2015 Leslie Clement, Chief of Policy Lori Coyner,
King County City Health Profile Seattle
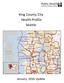 King County City Health Profile Seattle Shoreline Kenmore/LFP Bothell/Woodinville NW Seattle North Seattle Kirkland North Ballard Fremont/Greenlake NE Seattle Kirkland Redmond QA/Magnolia Capitol Hill/E.lake
King County City Health Profile Seattle Shoreline Kenmore/LFP Bothell/Woodinville NW Seattle North Seattle Kirkland North Ballard Fremont/Greenlake NE Seattle Kirkland Redmond QA/Magnolia Capitol Hill/E.lake
HEDIS 101 for Providers 2018
 HEDIS 101 for Providers 2018 Improving Quality of Care HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Author: Commercial & GBD Communication HEDIS Team Document
HEDIS 101 for Providers 2018 Improving Quality of Care HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Author: Commercial & GBD Communication HEDIS Team Document
Partners HealthCare Primary Care Quality and Patient Experience Reports 2017
 Partners HealthCare Primary Care Quality and Patient Experience Reports 2017 North Shore Health System QUALITYANDSAFETY.PARTNERS.ORG 1 INTRODUCTION Dear Patients, Colleagues and members of the Commonwealth
Partners HealthCare Primary Care Quality and Patient Experience Reports 2017 North Shore Health System QUALITYANDSAFETY.PARTNERS.ORG 1 INTRODUCTION Dear Patients, Colleagues and members of the Commonwealth
Reducing Readmissions: Potential Measurements
 Reducing Readmissions: Potential Measurements Avoid Readmissions Through Collaboration October 27, 2010 Denise Remus, PhD, RN Chief Quality Officer BayCare Health System Overview Why Focus on Readmissions?
Reducing Readmissions: Potential Measurements Avoid Readmissions Through Collaboration October 27, 2010 Denise Remus, PhD, RN Chief Quality Officer BayCare Health System Overview Why Focus on Readmissions?
Section IX Special Needs & Case Management
 Section IX Special Needs & Case Management Special Needs and Case Management 181 Integrated Health Care Management (IHCM) The Integrated Health Care Management (IHCM) program is a population-based health
Section IX Special Needs & Case Management Special Needs and Case Management 181 Integrated Health Care Management (IHCM) The Integrated Health Care Management (IHCM) program is a population-based health
ProviderReport. Managing complex care. Supporting member health.
 ProviderReport Supporting member health Managing complex care Do you have patients whose conditions need complex, coordinated care they may not be able to facilitate on their own? A care manager may be
ProviderReport Supporting member health Managing complex care Do you have patients whose conditions need complex, coordinated care they may not be able to facilitate on their own? A care manager may be
March 6, 2016 Cambridge, MA. Health Equity. Amy Reid, MPH
 March 6, 2016 Cambridge, MA Health Equity Amy Reid, MPH Director areid@ihi.org @_amyjreid_ Agenda 1. What is health equity? 2. How does health equity relate to patient safety & health care quality? 3.
March 6, 2016 Cambridge, MA Health Equity Amy Reid, MPH Director areid@ihi.org @_amyjreid_ Agenda 1. What is health equity? 2. How does health equity relate to patient safety & health care quality? 3.
Medical Record Review Tool Standards with Definitions
 WellCare Health Plans, Inc. WellCare of Georgia, Inc The WellCare Group of Companies Medical Record Review Tool Standards with Definitions Item # STANDARD DEFINITION SOURCE All Medical Records: 1 Patient
WellCare Health Plans, Inc. WellCare of Georgia, Inc The WellCare Group of Companies Medical Record Review Tool Standards with Definitions Item # STANDARD DEFINITION SOURCE All Medical Records: 1 Patient
STEUBEN COUNTY HEALTH PROFILE. Finger Lakes Health Systems Agency, 2017
 STEUBEN COUNTY HEALTH PROFILE Finger Lakes Health Systems Agency, 2017 About the Report The purpose of this report is to provide a summary of health data specific to Steuben County. Where possible, benchmarks
STEUBEN COUNTY HEALTH PROFILE Finger Lakes Health Systems Agency, 2017 About the Report The purpose of this report is to provide a summary of health data specific to Steuben County. Where possible, benchmarks
ZIP CODE. Other Zip Codes Unknown Residence
 ZIP CODE Zip Code Other Zip Codes Unknown Residence TOTAL Patients Note: This is a representation of the form; however the actual on line input process will look significantly different, as may the printed
ZIP CODE Zip Code Other Zip Codes Unknown Residence TOTAL Patients Note: This is a representation of the form; however the actual on line input process will look significantly different, as may the printed
Medi-Cal Performance Measurement: Making the Leap to Value-Based Incentives. Dolores Yanagihara IHA Stakeholders Meeting October 3, 2018
 Medi-Cal Performance Measurement: Making the Leap to Value-Based Incentives Dolores Yanagihara IHA Stakeholders Meeting October 3, 2018 Why Standardization? MEDI-CAL CROSS PRODUCT San Francisco Health
Medi-Cal Performance Measurement: Making the Leap to Value-Based Incentives Dolores Yanagihara IHA Stakeholders Meeting October 3, 2018 Why Standardization? MEDI-CAL CROSS PRODUCT San Francisco Health
Big Rapids Hospital Community Health Needs Assessment (CHNA) Implementation Plan July 2015 June 2018
 Big Rapids Hospital Community Health Needs Assessment (CHNA) Implementation Plan July 2015 June 2018 Attachment A Spectrum Health Big Rapids Hospital Community Health Needs Assessment Summary of Significant
Big Rapids Hospital Community Health Needs Assessment (CHNA) Implementation Plan July 2015 June 2018 Attachment A Spectrum Health Big Rapids Hospital Community Health Needs Assessment Summary of Significant
Meaningful Use Measures: Quick Reference Guide Stage 2 (2014 and Beyond)
 Meaningful Use Measures: Quick Reference Guide Stage 2 (2014 and Beyond) Core Measures Required: All 17 objectives Objective: Requirement: Exclusions: Accomplish in Clinical 1. Computerized - Documenting
Meaningful Use Measures: Quick Reference Guide Stage 2 (2014 and Beyond) Core Measures Required: All 17 objectives Objective: Requirement: Exclusions: Accomplish in Clinical 1. Computerized - Documenting
An Introduction to MPCA and Federally Qualified Health Centers~ Partners for Quality Care
 An Introduction to MPCA and Federally Qualified Health Centers~ Partners for Quality Care AIM Partnership Forum June 5, 2014 Lynda C. Meade, MPA Director of Clinical Services Michigan Primary Care Association
An Introduction to MPCA and Federally Qualified Health Centers~ Partners for Quality Care AIM Partnership Forum June 5, 2014 Lynda C. Meade, MPA Director of Clinical Services Michigan Primary Care Association
Chapter 2 Provider Responsibilities Unit 5: Specialist Basics
 Chapter 2 Provider Responsibilities Unit 5: Specialist Basics In This Unit Topic See Page Unit 5: Specialist Basics Participation in the Highmark s Networks as a Specialist 2 Specialist and Personal Physician
Chapter 2 Provider Responsibilities Unit 5: Specialist Basics In This Unit Topic See Page Unit 5: Specialist Basics Participation in the Highmark s Networks as a Specialist 2 Specialist and Personal Physician
Covered (blood, blood components, human blood products, and their administration) Covered (Some restrictions)
 Washington Apple Health Medical Benefits Allergy Services (Antigen/Allergy Serum/Allergy Shots) Ambulance Services (Air Transportation) by FFS* Ambulance Services (Emergency Transportation) Ambulatory
Washington Apple Health Medical Benefits Allergy Services (Antigen/Allergy Serum/Allergy Shots) Ambulance Services (Air Transportation) by FFS* Ambulance Services (Emergency Transportation) Ambulatory
Payment Transformation 2018 Measure Changes and Updates. April 4, 2018
 Payment Transformation 2018 Measure Changes and Updates April 4, 2018 1. 2018 Performance Measures 2. 2018 Engagement Measures 3. Patient Attribution & Panel Management Cozeva 4. Coreo 1. Effectively Manage
Payment Transformation 2018 Measure Changes and Updates April 4, 2018 1. 2018 Performance Measures 2. 2018 Engagement Measures 3. Patient Attribution & Panel Management Cozeva 4. Coreo 1. Effectively Manage
Data Use in Public Health: Challenges, Successes and New Opportunities. Iowa Governor s Conference on Public Health April 14, 2015
 Data Use in Public Health: Challenges, Successes and New Opportunities Iowa Governor s Conference on Public Health April 14, 2015 Learning Objectives Locate and utilize local data for assessment, planning,
Data Use in Public Health: Challenges, Successes and New Opportunities Iowa Governor s Conference on Public Health April 14, 2015 Learning Objectives Locate and utilize local data for assessment, planning,
Community Health Improvement Plan
 Community Health Improvement Plan Methodist Le Bonheur Germantown Hospital Methodist Le Bonheur Healthcare (MLH) is an integrated, not-for-profit healthcare delivery system based in Memphis, Tennessee,
Community Health Improvement Plan Methodist Le Bonheur Germantown Hospital Methodist Le Bonheur Healthcare (MLH) is an integrated, not-for-profit healthcare delivery system based in Memphis, Tennessee,
New Patient Welcome. elrio.org
 New Patient Welcome elrio.org Welcome to EL RIO Your HEALTHCARE HOME A healthcare home is a place where healthcare professionals know your needs, history, and how to help you stay healthy. A healthcare
New Patient Welcome elrio.org Welcome to EL RIO Your HEALTHCARE HOME A healthcare home is a place where healthcare professionals know your needs, history, and how to help you stay healthy. A healthcare
ONTARIO COUNTY HEALTH PROFILE. Finger Lakes Health Systems Agency, 2017
 ONTARIO COUNTY HEALTH PROFILE Finger Lakes Health Systems Agency, 2017 About the Report The purpose of this report is to provide a summary of health data specific to Ontario County. Where possible, benchmarks
ONTARIO COUNTY HEALTH PROFILE Finger Lakes Health Systems Agency, 2017 About the Report The purpose of this report is to provide a summary of health data specific to Ontario County. Where possible, benchmarks
during the EHR reporting period.
 CMS Stage 2 MU Proposed Objectives and Measures for EPs Objective Measure Notes and Queries PUT YOUR COMMENTS HERE CORE SET (EP must meet all 17 Core Set objectives) Exclusion: Any EP who writes fewer
CMS Stage 2 MU Proposed Objectives and Measures for EPs Objective Measure Notes and Queries PUT YOUR COMMENTS HERE CORE SET (EP must meet all 17 Core Set objectives) Exclusion: Any EP who writes fewer
Kaleida Health 2010 One-Year Community Service Plan Update September 2010
 2010 One-Year Community Service Plan Update September 2010 1 2 Kaleida Health 2010 One-Year Community Service Plan Update September 2010 Kaleida Health hospital facilities include the Buffalo General Hospital,
2010 One-Year Community Service Plan Update September 2010 1 2 Kaleida Health 2010 One-Year Community Service Plan Update September 2010 Kaleida Health hospital facilities include the Buffalo General Hospital,
HEDIS Ad-Hoc Public Comment: Table of Contents
 HEDIS 1 2018 Ad-Hoc Public Comment: Table of Contents HEDIS Overview... 1 The HEDIS Measure Development Process... Synopsis... Submitting Comments... NCQA Review of Public Comments... Value Set Directory...
HEDIS 1 2018 Ad-Hoc Public Comment: Table of Contents HEDIS Overview... 1 The HEDIS Measure Development Process... Synopsis... Submitting Comments... NCQA Review of Public Comments... Value Set Directory...
Stage 1 Meaningful Use Objectives and Measures
 Stage 1 Meaningful Use Objectives and Measures Author: Mia Evans About Technosoft Solutions: Technosoft Solutions is a healthcare technology consulting, dedicated to providing software development services
Stage 1 Meaningful Use Objectives and Measures Author: Mia Evans About Technosoft Solutions: Technosoft Solutions is a healthcare technology consulting, dedicated to providing software development services
Benefits are effective January 01, 2018 through December 31, 2018 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY
 PLAN FEATURES Annual Deductible The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Hearing aid reimbursement does not apply to the out-of-pocket
PLAN FEATURES Annual Deductible The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Hearing aid reimbursement does not apply to the out-of-pocket
Total Cost of Care Technical Appendix April 2015
 Total Cost of Care Technical Appendix April 2015 This technical appendix supplements the Spring 2015 adult and pediatric Clinic Comparison Reports released by the Oregon Health Care Quality Corporation
Total Cost of Care Technical Appendix April 2015 This technical appendix supplements the Spring 2015 adult and pediatric Clinic Comparison Reports released by the Oregon Health Care Quality Corporation
Schedule of Benefits - HMO Group - MEDFORD AREA SCHOOL DISTRICT Benefit Year: January 1st through December 31st Effective Date: 01/01/2016
 Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
Security Health Plan certifies that you and any covered dependents have coverage as described in your Certificate and Schedule of Benefits as of the effective date shown on the letter you received with
STEUBEN COUNTY HEALTH PROFILE
 STEUBEN COUNTY HEALTH PROFILE 2017 ABOUT THE REPORT The purpose of this report is to provide a summary of health data specific to Steuben County. Where possible, benchmarks have been given to compare county
STEUBEN COUNTY HEALTH PROFILE 2017 ABOUT THE REPORT The purpose of this report is to provide a summary of health data specific to Steuben County. Where possible, benchmarks have been given to compare county
Health First Wellness Incentive
 Health First Wellness Incentive The Health First Wellness Incentive has been set up as a reward for taking steps to either maintain or obtain a healthy lifestyle. Taking healthy actions and becoming a
Health First Wellness Incentive The Health First Wellness Incentive has been set up as a reward for taking steps to either maintain or obtain a healthy lifestyle. Taking healthy actions and becoming a
Community Health Needs Assessment. Implementation Plan FISCA L Y E AR
 Community Health Needs Assessment Implementation Plan FISCA L Y E AR 2 0 1 5-2 0 1 8 Table of Contents: I. Background 1 II. Areas of Priority 2 a. Preventive Care and Chronic Conditions b. Community Health
Community Health Needs Assessment Implementation Plan FISCA L Y E AR 2 0 1 5-2 0 1 8 Table of Contents: I. Background 1 II. Areas of Priority 2 a. Preventive Care and Chronic Conditions b. Community Health
MEANINGFUL USE STAGE FOR ELIGIBLE PROVIDERS USING CERTIFIED EMR TECHNOLOGY
 MEANINGFUL USE STAGE 2 2014 FOR ELIGIBLE PROVIDERS USING CERTIFIED EMR TECHNOLOGY STAGE 2 REQUIREMENTS EPs must meet or qualify for an exclusion to 17 core objectives. EPs must meet 3 of the 6 menu measures.
MEANINGFUL USE STAGE 2 2014 FOR ELIGIBLE PROVIDERS USING CERTIFIED EMR TECHNOLOGY STAGE 2 REQUIREMENTS EPs must meet or qualify for an exclusion to 17 core objectives. EPs must meet 3 of the 6 menu measures.
HEDIS Measures and the Family Physician Office. Pablo J Calzada DO, MPH, FAAFP, FACOFP
 HEDIS Measures and the Family Physician Office Pablo J Calzada DO, MPH, FAAFP, FACOFP Disclaimer HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). NCQA and payers
HEDIS Measures and the Family Physician Office Pablo J Calzada DO, MPH, FAAFP, FACOFP Disclaimer HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). NCQA and payers
APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS
 Appendix 2 NCQA PCMH 2011 and CMS Stage 1 Meaningful Use Requirements 2-1 APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS CMS Meaningful Use Requirements* All Providers Must Meet
Appendix 2 NCQA PCMH 2011 and CMS Stage 1 Meaningful Use Requirements 2-1 APPENDIX 2 NCQA PCMH 2011 AND CMS STAGE 1 MEANINGFUL USE REQUIREMENTS CMS Meaningful Use Requirements* All Providers Must Meet
What Culture Does Your Patient Hurt In? Cultural Competency in Caring for Diverse Populations
 What Culture Does Your Patient Hurt In? Cultural Competency in Caring for Diverse Populations Fern R. Hauck, MD, MS Department of Family Medicine University of Virginia Health System POM-1, September 10,
What Culture Does Your Patient Hurt In? Cultural Competency in Caring for Diverse Populations Fern R. Hauck, MD, MS Department of Family Medicine University of Virginia Health System POM-1, September 10,
Quality Improvement Program (QIP) Measurement Specifications
 Quality Improvement Program (QIP) 2014 2015 Measurement Specifications Developed by: Marya Choudhry Contributors include: Robert Moore Jess Liu Jennifer Dionisio Carolyn Stewart Melanie Lam Jessica Thatcher
Quality Improvement Program (QIP) 2014 2015 Measurement Specifications Developed by: Marya Choudhry Contributors include: Robert Moore Jess Liu Jennifer Dionisio Carolyn Stewart Melanie Lam Jessica Thatcher
2018 Practice Improvement Program (PIP) Orientation. January 4 th, 2018 San Francisco Health Plan Practice Improvement Program (PIP)
 2018 Practice Improvement Program (PIP) Orientation January 4 th, 2018 San Francisco Health Plan Practice Improvement Program (PIP) Practice Improvement Program (PIP) Leadership Team James Glauber, Chief
2018 Practice Improvement Program (PIP) Orientation January 4 th, 2018 San Francisco Health Plan Practice Improvement Program (PIP) Practice Improvement Program (PIP) Leadership Team James Glauber, Chief
Health and Well-Being
 Health and Well-Being DRAFT REPORT FOR VOTING August 14, 2014 This report is funded by the Department of Health and Human Services under contract HHSM-500-2012-00009I Task 8.0 1 Contents Executive Summary...
Health and Well-Being DRAFT REPORT FOR VOTING August 14, 2014 This report is funded by the Department of Health and Human Services under contract HHSM-500-2012-00009I Task 8.0 1 Contents Executive Summary...
NATIONAL HEALTHCARE AGREEMENT 2011
 NATIONAL HEALTHCARE AGREEMENT 2011 Council of Australian Governments An agreement between the Commonwealth of Australia and the States and Territories, being: the State of New South Wales; the State of
NATIONAL HEALTHCARE AGREEMENT 2011 Council of Australian Governments An agreement between the Commonwealth of Australia and the States and Territories, being: the State of New South Wales; the State of
OPPORTUNITIES FOR DATA INTEGRATION AND BEST PRACTICE INTERVENTIONS TO IMPROVE CLINICAL AND FINANCIAL OUTCOMES
 OPPORTUNITIES FOR DATA INTEGRATION AND BEST PRACTICE INTERVENTIONS TO IMPROVE CLINICAL AND FINANCIAL OUTCOMES Elizabeth S Miller, MPA November 2014 President BPKMiller Associates 1 2 3 HEDIS DATA IMPROVEMENT:
OPPORTUNITIES FOR DATA INTEGRATION AND BEST PRACTICE INTERVENTIONS TO IMPROVE CLINICAL AND FINANCIAL OUTCOMES Elizabeth S Miller, MPA November 2014 President BPKMiller Associates 1 2 3 HEDIS DATA IMPROVEMENT:
Fostering Quality Improvement in the SC Medicaid Program
 Fostering Quality Improvement in the SC Medicaid Program Medicaid Matching Expenditures as a Percent of Total State General Fund Revenue Medicaid is approximately 1/5 2015 2010 2005 2000 1995 $0 $2,000,000,
Fostering Quality Improvement in the SC Medicaid Program Medicaid Matching Expenditures as a Percent of Total State General Fund Revenue Medicaid is approximately 1/5 2015 2010 2005 2000 1995 $0 $2,000,000,
Diversity & Disparities: A Benchmark Study of U.S. Hospitals.
 Diversity & Disparities: A Benchmark Study of U.S. Hospitals http://www.hpoe.org/diversity-disparities Contents Executive Summary...2 Survey Methods...4 Collection and Use of REAL Data...5 Cultural Competency
Diversity & Disparities: A Benchmark Study of U.S. Hospitals http://www.hpoe.org/diversity-disparities Contents Executive Summary...2 Survey Methods...4 Collection and Use of REAL Data...5 Cultural Competency
Florida Medicaid: Performance Measures (HEDIS)
 Florida Medicaid: Performance Measures (HEDIS) Justin M. Senior Florida Medicaid Director Agency for Health Care Administration Senate Health Policy October 20, 2015 Statewide Medicaid Managed Care (SMMC)
Florida Medicaid: Performance Measures (HEDIS) Justin M. Senior Florida Medicaid Director Agency for Health Care Administration Senate Health Policy October 20, 2015 Statewide Medicaid Managed Care (SMMC)
TC LHIN Quality Indicators: Big Dot (System) and Small Dot (Sector Specific) Indicators. November 29, 2013
 TC LHIN Quality Indicators: Big Dot (System) and Small Dot (Sector Specific) Indicators November 29, 2013 1 Contents 1. TC LHIN Quality Framework, Themes and Focus Areas 2. Big Dot System Indicators 3.
TC LHIN Quality Indicators: Big Dot (System) and Small Dot (Sector Specific) Indicators November 29, 2013 1 Contents 1. TC LHIN Quality Framework, Themes and Focus Areas 2. Big Dot System Indicators 3.
Midwife / Physician Agreement
 Midwife / Physician Agreement This agreement between (the midwife) and (Affiliated Physician) executed this date sets forth the agreement between the parties, patterns of care between the parties and patterns
Midwife / Physician Agreement This agreement between (the midwife) and (Affiliated Physician) executed this date sets forth the agreement between the parties, patterns of care between the parties and patterns
Cultural Transformation and the Road to an ACO Lee Sacks, M.D. CEO Mark Shields, M.D., MBA Senior Medical Director
 Cultural Transformation and the Road to an ACO Lee Sacks, M.D. CEO Mark Shields, M.D., MBA Senior Medical Director AMGA Pre-conference Workshop 1 April 14, 2011 Washington, D.C. Disclosure Nothing in Today
Cultural Transformation and the Road to an ACO Lee Sacks, M.D. CEO Mark Shields, M.D., MBA Senior Medical Director AMGA Pre-conference Workshop 1 April 14, 2011 Washington, D.C. Disclosure Nothing in Today
How Do You Operationalize Health Equity? How Do We Tip The Scale?
 1 How Do You Operationalize Health Equity? How Do We Tip The Scale? 2 Why Look Through A Health Equity Lens: A large body of research has been well a established. This research has lead us to understand
1 How Do You Operationalize Health Equity? How Do We Tip The Scale? 2 Why Look Through A Health Equity Lens: A large body of research has been well a established. This research has lead us to understand
CLASSIC BLUE SECURE/BLUE CROSS BLUE SHIELD COMPLEMENTARY Monroe County Benefit Summary/Comparison (Over 65 Retirees)
 WHO IS COVERED Enrollment Requirement Members must be enrolled in both Medicare Parts A and B Members must be enrolled in both Medicare Parts A and B Type of Tier Single only Single only Dependent/Student
WHO IS COVERED Enrollment Requirement Members must be enrolled in both Medicare Parts A and B Members must be enrolled in both Medicare Parts A and B Type of Tier Single only Single only Dependent/Student
2015 MEANINGFUL USE STAGE 2 FOR ELIGIBLE PROVIDERS USING CERTIFIED EMR TECHNOLOGY
 2015 MEANINGFUL USE STAGE 2 FOR ELIGIBLE PROVIDERS USING CERTIFIED EMR TECHNOLOGY STAGE 2 REQUIREMENTS EPs must meet or qualify for an exclusion to 17 core objectives EPs must meet 3 of the 6 menu measures.
2015 MEANINGFUL USE STAGE 2 FOR ELIGIBLE PROVIDERS USING CERTIFIED EMR TECHNOLOGY STAGE 2 REQUIREMENTS EPs must meet or qualify for an exclusion to 17 core objectives EPs must meet 3 of the 6 menu measures.
Covered Benefits Matrix for Children
 Medicaid Managed Care The matrix below lists the available for children (under age 21) enrolled in the West Virginia Mountain Health Trust and s. Ambulance Ambulatory surgical center services Some services
Medicaid Managed Care The matrix below lists the available for children (under age 21) enrolled in the West Virginia Mountain Health Trust and s. Ambulance Ambulatory surgical center services Some services
Managing Patients with Multiple Chronic Conditions
 Best Practices Managing Patients with Multiple Chronic Conditions Dartmouth-Hitchcock Physicians Case Study Organization Profile Headquartered in Bedford, New Hampshire, Dartmouth-Hitchcock is a large
Best Practices Managing Patients with Multiple Chronic Conditions Dartmouth-Hitchcock Physicians Case Study Organization Profile Headquartered in Bedford, New Hampshire, Dartmouth-Hitchcock is a large
Pursuing Equity: The Role of Health Care
 D3/E3 Pursuing Equity: The Role of Health Care Session D: 9:30 10:45am Session E: 11:15 12:30pm Berny Gould Julie Oehlert Amy Reid Michelle Schreiber Agenda 2 15 mins Framing & Overview 10 mins Case Study
D3/E3 Pursuing Equity: The Role of Health Care Session D: 9:30 10:45am Session E: 11:15 12:30pm Berny Gould Julie Oehlert Amy Reid Michelle Schreiber Agenda 2 15 mins Framing & Overview 10 mins Case Study
Date: Illinois Health Connect PCP 6/23/14 Page 1 of 8. Signature:
 Illinois Department of Healthcare and Family Services Illinois Health Connect Primary Care Provider Agreement This Agreement pertains only to the relationship between the Illinois Department of Healthcare
Illinois Department of Healthcare and Family Services Illinois Health Connect Primary Care Provider Agreement This Agreement pertains only to the relationship between the Illinois Department of Healthcare
Benefits and Premiums are effective January 01, 2018 through December 31, 2018 PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY
 The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Primary Care Physician Selection Optional There is no requirement for member pre-certification.
The maximum out-of-pocket limit applies to all covered Medicare Part A and B benefits including deductible. Primary Care Physician Selection Optional There is no requirement for member pre-certification.
RFS-7-62 ATTACHMENT E INDIANA CARE SELECT PROGRAM DESCRIPTION AND COVERED BENEFITS
 The following services are covered by the Indiana Care Select Program. Dual-eligible members, those members eligible for both IHCP and Medicare, will not receive any benefits under Indiana Care Select,
The following services are covered by the Indiana Care Select Program. Dual-eligible members, those members eligible for both IHCP and Medicare, will not receive any benefits under Indiana Care Select,
Achieving Health Equity After the ACA: Implications for cost, quality and access
 Achieving Health Equity After the ACA: Implications for cost, quality and access Michelle Cabrera, Research Director SEIU State Council April 23, 2015 SEIU California 700,000 Members Majority people of
Achieving Health Equity After the ACA: Implications for cost, quality and access Michelle Cabrera, Research Director SEIU State Council April 23, 2015 SEIU California 700,000 Members Majority people of
Part I. New York State Laws and Regulations PRENATAL CARE ASSISTANCE PROGRAM (i.e., implementing regs on newborn testing program)
 Part I. New York State Laws and Regulations PRENATAL CARE ASSISTANCE PROGRAM (i.e., implementing regs on newborn testing program) (SEE NY Public Health Law 2500f for HIV testing of newborns FOR STATUTE)
Part I. New York State Laws and Regulations PRENATAL CARE ASSISTANCE PROGRAM (i.e., implementing regs on newborn testing program) (SEE NY Public Health Law 2500f for HIV testing of newborns FOR STATUTE)
June Thank you for attending today s Webinar. We will begin shortly. June Brian Clark. Diana Charlton. Debbie Barkley Aetna Inc.
 June 2018 Brian Clark Diana Charlton Debbie Barkley Thank you for attending today s Webinar. We will begin shortly. June 2018 1 Brian Clark Diana Charlton Debbie Barkley Welcome Illinois, New Jersey, Florida,
June 2018 Brian Clark Diana Charlton Debbie Barkley Thank you for attending today s Webinar. We will begin shortly. June 2018 1 Brian Clark Diana Charlton Debbie Barkley Welcome Illinois, New Jersey, Florida,
National Survey of Physician Organizations and the Management of Chronic Illness II (Independent Practice Associations)
 If you want to use all or part of this questionnaire, please contact Patty Ramsay (email: pramsay@berkeley.edu; phone: 510/643-8063; mail: Patty Ramsay, University of California, SPH/HPM, 50 University
If you want to use all or part of this questionnaire, please contact Patty Ramsay (email: pramsay@berkeley.edu; phone: 510/643-8063; mail: Patty Ramsay, University of California, SPH/HPM, 50 University
Benchmark Data Sources
 Medicare Shared Savings Program Quality Measure Benchmarks for the 2016 and 2017 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Medicare Shared Savings Program Quality Measure Benchmarks for the 2016 and 2017 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Public Health and Managed Care. December 8 and 16, 2015
 Public Health and Managed Care December 8 and 16, 2015 Where We re Going Structure of Public Health in Illinois What Public Health Brings to Managed Care Some Similarities and Differences Some Public Health
Public Health and Managed Care December 8 and 16, 2015 Where We re Going Structure of Public Health in Illinois What Public Health Brings to Managed Care Some Similarities and Differences Some Public Health
MONROE COUNTY HEALTH PROFILE. Finger Lakes Health Systems Agency, 2017
 MONROE COUNTY HEALTH PROFILE Finger Lakes Health Systems Agency, 2017 About the Report The purpose of this report is to provide a summary of health data specific to Monroe County. Where possible, benchmarks
MONROE COUNTY HEALTH PROFILE Finger Lakes Health Systems Agency, 2017 About the Report The purpose of this report is to provide a summary of health data specific to Monroe County. Where possible, benchmarks
DELAWARE FACTBOOK EXECUTIVE SUMMARY
 DELAWARE FACTBOOK EXECUTIVE SUMMARY DaimlerChrysler and the International Union, United Auto Workers (UAW) launched a Community Health Initiative in Delaware to encourage continued improvement in the state
DELAWARE FACTBOOK EXECUTIVE SUMMARY DaimlerChrysler and the International Union, United Auto Workers (UAW) launched a Community Health Initiative in Delaware to encourage continued improvement in the state
=======================================================================
 ======================================================================= ----------------------------------------------------------------------- DEPARTMENT OF HEALTH AND HUMAN SERVICES Office of the Secretary
======================================================================= ----------------------------------------------------------------------- DEPARTMENT OF HEALTH AND HUMAN SERVICES Office of the Secretary
Technical Specifications Community Checkup Measures About the technical specifications Measures sourced from the Washington Health Alliance Database
 Technical Specifications Community Checkup Measures September 2017 About the technical specifications The 2017 Community Checkup relies on three categories of data to produce results: The Alliance (the
Technical Specifications Community Checkup Measures September 2017 About the technical specifications The 2017 Community Checkup relies on three categories of data to produce results: The Alliance (the
Appendix 4 CMS Stage 1 Meaningful Use Requirements Summary Tables 4-1 APPENDIX 4 CMS STAGE 1 MEANINGFUL USE REQUIREMENTS SUMMARY
 Appendix 4 CMS Stage 1 Meaningful Use Requirements Summary Tables 4-1 APPENDIX 4 CMS STAGE 1 MEANINGFUL USE REQUIREMENTS SUMMARY 1. Use CPOE (computerized physician order entry) for medication orders directly
Appendix 4 CMS Stage 1 Meaningful Use Requirements Summary Tables 4-1 APPENDIX 4 CMS STAGE 1 MEANINGFUL USE REQUIREMENTS SUMMARY 1. Use CPOE (computerized physician order entry) for medication orders directly
1. What is your ethnic origin? (Check one) 2. What is your gender? 3. What is your age? Page 1. nmlkj. nmlkj. nmlkj. nmlkj. nmlkj. nmlkj. nmlkj.
 1. What is your ethnic origin? (Check one) White Asian/Pacfic Island American Indian Black Hispanic 2. What is your gender? Female Male 3. What is your age? 18 to 24 55 to 64 25 to 34 65 to 74 35 to 44
1. What is your ethnic origin? (Check one) White Asian/Pacfic Island American Indian Black Hispanic 2. What is your gender? Female Male 3. What is your age? 18 to 24 55 to 64 25 to 34 65 to 74 35 to 44
