Policy for Patient Access
|
|
|
- Kathlyn Phillips
- 6 years ago
- Views:
Transcription
1 Policy for Patient Access
2 DOCUMENT CONTROL Revision Date Old Version 10/12/ /07/ /04/ Amendment General Management Review General Management Review General Management Review Authored by Michaella Tsikkini Commercial & Legal Officer New Version 1.1 Operation Director 1.2 Jon Dore Director Central Operations 1.3 Introduction This Policy sets out the overall expectations of Newmedica on the management of referrals and admissions into and within the organisation. It also sets out the responsibilities of Newmedica staff. This policy details how patients will be managed administratively at all points of contact within Newmedica. The policy has been developed to ensure Newmedica in conjunction with its commissioners provides a consistent, equitable and fair approach to the management of patient referrals and treatment that meets the requirements of the NHS Operating Framework and the commitments made to patients in the NHS Constitution and Accessible Information Standard. Newmedica will use this policy to demonstrate how rules are applied fairly and with equity in the provision of planned care. Newmedica will work to ensure fair and equal access to services for all patients, and ensure it meets its obligations towards people who have had, or have disabilities under the Equality Act (2010). This places a legal obligation on organisations to make reasonable adjustments to facilitate the care of people with disabilities. The decision as to what adjustments to make is not prescriptive, and must be agreed with the patient, their carer and the team caring for the person. By Law, if the adjustment is reasonable, then it should be made. Examples of reasonable adjustments can be found in the NHS England Guidelines: supporting people with a learning disability and/or autism who have a mental health condition or display behaviour that challenges Objectives This policy aims to inform patients, their relatives and carers of their rights and what they can expect from Newmedica in terms of access to services by outlining relevant rules, responsibilities and actions by which Newmedica will manage patients through their pathways, specifically:
3 The national 18-week Referral to Treatment (RTT) pathway, which is about improving patients experience of the NHS, ensuring all patients receive high quality elective care without any unnecessary delay. National Cancer Waiting Times for all suspected and diagnosed cancers. The national 6-week guidance for diagnostic tests. In accordance with the NHS Constitution everyone has the right to access certain services commissioned by NHS bodies within maximum waiting times, or for the NHS to take all reasonable steps to offer a range of suitable alternative providers if this is not possible. This includes a right to start consultant-led treatment within a maximum of 18 weeks from referral for non-urgent conditions; and This policy sets out the way in which Newmedica will manage patients who are waiting for treatment or on treatment pathways. It covers the management of patients at all sites where Newmedica operates, including community clinics. Every process in the management of patients who are waiting for treatment must be clear and transparent to the patients and to partner organisations and must be open to inspection, monitoring and audit. This policy sets out how Newmedica will manage 18-week RTT pathways and suspected cancer referrals in line with national targets and guidance. Application of the policy where applicable will ensure that each patient s RTT clock starts and stops fairly and consistently in accordance with an agreed structured methodology. Treatment decisions will be fair and transparent and at an operational level this translates into the adoption of the following key principles: The management of patients will be fair, consistent and transparent and communication with patients will be clear and informative and will be consistent with the Human Rights Act 1998 and the Equality Act Patients seen in outpatients, or diagnostics will be seen firstly according to clinical priority and then in chronological order based upon the 18-week RTT pathway. We will attempt wherever possible to agree appointment dates to suit patients personal circumstances. This policy is intended to be used by all those individuals within Newmedica, who are responsible for managing referrals, adding to, and maintaining waiting lists for organising patient access to treatment. The principals of the policy apply to both medical and administrative waiting list management. Responsibility, Accountability & Duties The following are required to instigate appropriate actions to ensure the successful implementation of this policy within their area(s) of control: Patients should keep appointments, or if they must cancel, cancel within a reasonable time in order that the appointment can be re-used for another waiting patient. Receiving treatment within the maximum waiting times may be compromised unless patients try wherever possible to keep their original appointments.
4 Newmedica Medical Advisory Committee Approval & clinical input of this policy. Quality Management Committee - Consultation and input to this policy. Service Managers - Responsible for waiting list and patient access. Director of Operations and Governance - Participate with the Directors in monitoring Newmedica and commissioning, contract, service agreements, national and local standards and strategies, undertaking benchmarking, reporting and review work as necessary. All Directors - Responsible for the overall application and adherence to this policy and procedures within their areas of responsibility. Clinical Staff: Consistent application and adherence of this policy and its principles. Consideration is to be given by clinical staff for cross-cover arrangements during periods of annual leave or other absences. A minimum of 6 weeks notice is necessary for consultant and medical staff planned leave to ensure patient appointment dates are honoured and to reduce the need for changes and cancellations. All leave requests must be authorised by the line manager. All referrals (electronic and paper) into Newmedica should be reviewed and prioritised within contract KPI timelines by the accepting clinician to confirm clinical priority, appropriateness and capacity to treat within the mandated timelines. Head of Governance: Provide professional leadership on all records management issues within Newmedica to ensure an efficient quality case note service to support effective patient care. Initiating, interpreting and implementing changes in response to service developments, risk standards, legislation and to ensure the department is compliant with the Newmedica s strategic objectives. Service Managers: Responsible for the application of this policy at Service level, including the delivery of national and local targets. Responsible for training their staff as it relates to patient access and administration. Responsible for ensuring the minimum 6 weeks notice required for changes to rota s is adhered to in order to reduce the impact on patient experience and the administrative burden this entails if clinics should be cancelled. Responsible for providing information and analysis support to monitor targets and adherence to this
5 policy. Central Operations Director: Responsible for the production of the Patient Access Policy and the associated user guidance and their routine review. Also, responsible for their compliance and setting the standards for training around patient access and administration. Responsible for the provision and accuracy of information, data quality reports and the content of EMMA training. Provide professional leadership on all records management issues within Newmedica to ensure an efficient quality case note service to support effective patient care. Initiating, interpreting and implementing changes in response to service developments, risk standards, legislation and to ensure the department is compliant with the Newmedica s strategic objectives. Responsible for the training and education of administrative operatives as it relates to patient access and administration. Administrators and Secretaries: Responsible for the day-to-day management and application of their responsibilities in line with this policy. Management of the Policy Newmedica recognises the complexity of waiting list and patient access management. National rules are often complex but the procedures contained within this policy for patient access (PPA) give clear direction and expectations of both staff and patients. The routine management and updating of the PPA is led by the Director of Operations & Governance and passed to the policy review group for publication. Consultant Responsibilities Consultants clinically manage the needs of individual patients accessing Newmedica services. Leave and Clinic Cover - A minimum of 6 weeks notice for consultant and medical staff planned leave must be given to ensure patient appointment dates are honoured and that the re-work required when clinics are cancelled is kept to a minimum. All leave requests must be authorised by the Service Manager. Priority treatment for Military Veterans From 1 January 2008, all military veterans should receive priority access to NHS care for any conditions which are likely to be related to their service, subject to the clinical needs of all patients. Veterans are encouraged to tell their General Practitioner about their veteran status in order to benefit from priority treatment.
6 Newmedica Responsibilities for Patients with Learning Disabilities: Where a person is recognised as having a learning disability, the clinician should ensure that the notes are recorded appropriately to support the teams, the patient and their carers/family with access to the appointment and any reasonable adjustments that may be required during subsequent appointments / treatment episodes. Operational Management Responsibilities Patients with a learning disability and their families / carers must be supported with reasonable adjustments to ensure equitable access to treatment. If a service is unable to contact a patient, the Newmedica Discharge protocol should be followed, this is further covered later in this policy. Patients are to be seen within their maximum waiting times allowable. Information reports should be used to actively plan capacity to ensure achievement of waiting time targets and thus incur no breaches. Referrals and booking rules should be actively monitored in order to respond flexibly to demand and to deliver flexible capacity. Changes to booking rules must be authorised by the Central Ops Director and agreed with a Clinical Director. The exceptions are: Ad hoc requests with no reduction to patient booking numbers. Changes to medical staff rotas. Additions of target urgent slots for patients about to breach. Systems should be in place to ensure patients do not breach the 18-week RTT targets. Service Managers will monitor pathways and escalate patients to the appropriate manager where a breach is expected. Staff are to comply with EMMA data quality standards. Reasons for DNAs should be accurately recorded and monitored as should patient cancellations and discharges (particularly discharges without treatment). The content of the Directory of Services on E-Referral should be accurate at all times. Application of the clinical leave policy should be adhered to at all times. Ensure booking rules reflect appropriate levels of capacity for new and follow-up consultations and monitor variances in new-to-follow up ratios. Consultant to Consultant & Consultant to GP Referrals Direct referrals will be appropriate for:
7 Suspected cancer. Urgent problems for which delay would be detrimental to the patient s health. The expectation here would be that the patient needs to be seen within 2 weeks. Referral as part of the same clinical problem. Part of the recognised pathway of care for the condition Transfer of responsibility of care for an on-going condition, when it would be more convenient for the patient to be seen in a different location. Referral back to GP will be appropriate for: Conditions that are unrelated to the presenting problems and do not require urgent referral. Incidental findings. Conditions that can be dealt with by the GP. Those patients who Did Not Attend (DNA) their appointment (subject to the KPIs/local agreements). Those patients who cancel their appointments on multiple occasions (subject to KPIs/local agreements) Referral Queries: If there is any doubt as to whether a patient needs to be managed by Newmedica or whether a patient should be offered another choice of hospital, consultant or treatment option, the responsible Consultant should contact the patient s GP to discuss the case. Patients will only be added to a waiting list if there is an expectation of treating them and they are clinically fit or there is an expectation that they may become fit and ready to undertake the treatment within 18 weeks. With the exception of urgent screening referrals, all referrals (electronic and paper) will be reviewed and prioritised within contract KPI timelines of receipt. Processes around the use of the NHS e-referral Service Advice & Guidance (A&G) service (designed to support GPs with referral queries) must be standardised across Newmedica and, in accordance with contractual requirements. As the NHS e-referral Service system only supports one response, a holding message must not be used. At least 2 weeks notice must be given to the patient when agreeing an appointment date. The only exceptions to this are: Where it is clinically urgent
8 For a diagnostic test/procedure, where a reasonable offer is 10 days or more. Where patients make themselves available at short notice. NHS E-Ref Service NHS e-referral Service is a national electronic referral service which gives patients a choice of place, date and time for their first outpatient appointment in a hospital or clinic. The guidance states that the responsibility for the effective implementation of NHS e-referral Service should be shared between organisations. For example: Providers are responsible for ensuring that services are made available on NHS e-referral Service and that patients can book into appointments using the system Referrers are responsible for using NHS e-referral Service effectively to find suitable services for their patients Commissioners are responsible for ensuring that services available on the system accurately represent the clinical needs of their patient population and that those referrers and providers use the system effectively for the benefit of all patients. Appointment Slot Issues When no clinic appointment is available for patients to book in the NHS e-referral Service, the referral can be forwarded (via the Patient Web Application) or deferred (via the professional application) to the provider to enable the provider to book the patient an appointment. When a referral is forwarded or deferred, it will appear on the provider s Appointment Slot Issues (ASI) worklist. There are two reasons why there may be no clinic appointment available on the NHS e-referral Service. The first is that, in very rare circumstances, a technical issue can prevent an appointment slot from being shown or booked. The second and usual reason is that where we are providing directly bookable services we have not made sufficient appointment slots available to the NHS e-referral Service. If patients are left on the ASI worklist and their referrals are not processed then the following significant patient safety effects can occur: Some patients may not receive appointments within reasonable timescales. In some cases, this delay to care could pose a serious danger to their health and wellbeing. Patients without an appointment will have had no clinical review of their referral, as referral information only becomes visible to the provider once an appointment is booked in the NHS e-referral Service. This means that providers will not have had the opportunity to change the priority of a referral. Patients who have been referred into an inappropriate service will not have been identified and there will have been no opportunity to re-direct them into a more appropriate service.
9 Service managers must ensure that all staff managing the ASI worklists are appropriately trained, are in the correct workgroups, and have the necessary skills and authority to manage these referrals effectively, within the required timescales. Referral to Treatment Rules The NHS Constitution confirms that all patients have the legal right to start NHS consultant-led treatment within a maximum of 18 weeks from referral, unless they choose to wait longer or it is clinically appropriate that they wait longer. The national standard for 18-week RTT is: Those on an incomplete pathway whose clock is still running; 92% of those on the waiting list should not have waited more than 18 weeks. Consultant-led treatment includes treatments where a consultant retains overall clinical responsibility for the treatment. This could include treatments provided by the service or team led by the consultant. The setting of the consultant-led treatment, whether hospital-based or in a communitybased clinic, will not affect a patient s right to start treatment within 18 weeks. RTT Measurement Clock Starts. A clock start is the date that the Unique Booking Reference Number (UBRN) is converted in the case of referrals made via e-referral Service, or when Newmedica receives notice of the referral in to any service (consultant led, interface or assessment service) via FAX. Defer to Provider functionality is used in the NHS e-referral Service. Where a paper referral is sent, the clock start is the date on which the referral is received by Newmedica. Clock Continues The clock continues while tests and investigations are taking place. A clock does not automatically stop when a patient DNAs a follow-up appointment. The clock does not stop when a patient gives more than 24 hours notice that they are unable to attend an appointment. Clock Stops The 18-week clock stops when first definitive treatment is given i.e. treatment given surgically or non-surgically or when the following is communicated without undue delay to the patient and subsequently their GP and/or other referring practitioner: It is clinically appropriate to return the patient to primary care for any non-consultant-led treatment in primary care. A clinical decision is made to start a period of active monitoring. A patient declines treatment having been offered it. A clinical decision is made not to treat. A patient DNAs their first appointment twice following the initial referral that started their 18-week clock, provided that the provider can demonstrate that the appointment was clearly communicated to
10 the patient. A patient DNAs any other appointment twice and is subsequently discharged back to the care of their GP provided that: Newmedica can demonstrate that the appointment was clearly communicated to the patient. Discharging the patient is not contrary to their best clinical interests. Discharging the patient is carried out according to publicly available, policies on DNA s. If there is a delay in booking a further follow-up appointment because the patient preference makes it impossible or unreasonable for 18 weeks to be achieved for that patient, they will be discharged back to their GP. For example, if the patient repeatedly denies treatment or appointments offered or in accordance with Para 9 below. In order to ensure that the above RTT standards are adhered to, this policy confirms that: Service Managers will undertake a review of breaches of the RTT standards in order to identify themes to address to prevent a reoccurrence. This will be supported by the clinical lead responsible for the patient s treatment. The reasons for breaches are to be reviewed regularly by Central Operations and fed in to appropriate forums and / or escalated where appropriate. The Quality Management Committee will receive a regular report detailing the volume of breaches by speciality and reason, together with a supporting document detailing any lessons identified and subsequently learned, from the Service Managers Newmedica will formally document the process for escalation of issues related to RTT delivery. Refusal of Referrals NHS guidance states that providers should accept all clinically appropriate referrals made to them. Patients choosing a particular NHS provider must be treated by that provider as long as this is clinically appropriate and in accordance with the patient s wishes. Patients who DNA and Cancellations by Newmedica and the Patient If a patient DNAs an appointment (local KPIs differ), they should be referred back to their GP, unless the consultant deems it clinically necessary to offer another appointment, and they will be removed from the waiting list (a letter confirming their removal must be sent to the patient and their GP). If a patient cannot make a planned appointment, they should contact their clinic as soon as possible as this may make it possible for the appointment to be offered to somebody else who is waiting. Regarding measurement of RTT times, the national guidance states that: For first appointments on an RTT pathway:
11 If the patient DNAs, their RTT clock can be stopped and nullified on the date of the DNA appointment. If the patient DNAs but Newmedica chooses to rebook the patient, then their original RTT clock would be stopped on the date of the DNA appointment and a new clock will start (at zero) on the date that the Newmedica rebooks the patient. For subsequent appointments on an RTT pathway: If the patient DNAs and the Newmedica returns the patient back to primary care, then their RTT clock would stop on the date of the DNA appointment. If the patient DNAs but the Newmedica chooses to rebook the patient, then their existing RTT clock would continue to tick. If a patient DNAs their appointment in accordance with the policy, the following will occur: Adults - where there are no safeguarding issues, the patient will be discharged back to their GP. Where there are potential safeguarding issues, the patient should be offered another appointment. Children - will automatically be offered another appointment. In DNA cases, all Consultants must identify whether safeguarding issues are a factor and whether the DNA constitutes potential neglect of medical needs. Children who fail to attend a second outpatient appointment will be discharged back to their GP and the Safeguarding Lead should be informed. For missed follow-up appointments, the lead clinician will decide if there is a clinical need for follow-up in the community or whether primary care management would be appropriate. An assessment will be made as to whether the repeated nonattendance of the child could indicate neglect of their health needs and further referrals to safeguard the wellbeing of the child/young person may be made. For patients with a series of planned appointments, DNA s will need to be considered on a case-bycase basis by the lead Consultant. If a patient DNA s where a face-to-face interpreter has been booked, clinic administration staff are authorised to use that interpreter to attempt to make contact with the patient in order to establish a reason why and to offer a new appointment where that is appropriate in order to maximise the use of the translator resource. In the event that an interpreter DNAs a pre-booked appointment, clinics are encouraged to continue with the appointment utilising other methods of communication, including attempting to resource interpretation services via the telephone service. Only if it is deemed clinically unsafe to continue with an appointment should a patient s appointment be cancelled and rescheduled. Patient Tracking Lists (PTL) A PTL is a list of patients who need to be treated by given dates in order to start treatment within maximum waiting times set out in the NHS Constitution. A PTL is an established, forward-looking, management tool that is utilised by Newmedica to help achieve and sustain short Referral to
12 Treatment and diagnostic waits. The PTL provides a prospective viewpoint, and so can act as a planning tool for managing patient waiting lists in a way that a retrospective data collection cannot. Essentially, a PTL contains the data required to manage patients pathways, by showing clearly which patients are approaching the maximum waiting time so referral management centre staff can offer dates according to clinical priority and within maximum waiting times. PTL lists for services can be accessed through Checks and Balances. The NHS Standard Contract requires providers to submit information on referrals and waiting times. Where a CCG requests a PTL data set they are to be provided. Both the CCG and Newmedica should review this information routinely to understand performance. General Booking and Referral Management Principles If the patient was discharged more than 6 months ago, GPs will have to re-refer if an appointment is required for the same condition. Review of referrals must be completed within 7 working days. Referrals are not expected to be routinely rejected. Newmedica can reject a referral that hasn't been accepted (to be seen) in NHS e-referral Service, other rejections are maintained on EMMA post registration. The rejection process sends the patient back onto a work list at their GP surgery and the appointment is automatically cancelled on EMMA and NHS e-referral Service. It is then the GP s responsibility to notify the patient of their appointment cancellation. All inappropriate referrals will be referred back to the GP for them to review the choice of provider prior to the referral being redirected. The Date Request Received in EMMA constitutes a clock start for those patients on an active 18-Week RTT pathway. This is the date an attempt was made to convert a Unique Booking Reference Number into a booking for NHS e-referral Service patients and the date the referral letter was received into the Newmedica for paper referrals. Agreeing the dates of appointments with patients rather than notifying them of an appointment is the preferred option wherever possible in order to avoid the risk of patient cancellations or DNAs. Summary of Guidelines for Managing New Referrals A new referral will be required for: A new condition within the same specialty. Same condition where previous referral was discharged over 6 months ago. An assessment should have been undertaken by the referring clinician to determine any need for special considerations at the next level of care and this should then be recorded on EMMA to alert staff. If any new or changed requirements are identified during any treatment episode, then this information should be captured and EMMA updated.
13 Follow Ups Patients will only be followed up where there is a specific clinical need following the specialty protocol. Changing/Cancelling Appointments at Patient Request Patients may have an additional option to cancel and change their outpatient appointment on line, via NHS e-referral Service appointments must be cancelled and changed using the NHS e-referral Service telephone appointments line or website. If patient requests a rearrangement or cancellation within 24 hours of the appointment time it must be recorded as a patient cancellation and the 18-Week RTT clock will continue ticking and the reason for cancelation must be recorded. If a patient cancels the same appointment twice they must be: As a new patient, be removed from the registered referral list and referred back to their GP subject to clinical agreement. As a follow-up patient, referred to the consultant for discharge to GP. Patients can change NHS e-referral Service appointments at any time; this is out of Newmedica s control. All patient cancellations must be dealt with immediately to ensure they are not recorded as a DNA. If a patient has to leave a clinic prior to being seen (clinic over-running or other circumstance), their appointment must be changed to ensure that they are not penalised in the 18-week cycle as the clock will continue ticking. If a child s appointment is cancelled twice, the issues/concerns associated with this must be reviewed and assessed by the consultant, referring to the Newmedica policy for Safeguarding Children. If a patient cancels an appointment a second time, they should be referred back to their GP unless there is a clinical decision not to do so. Unable to Contact Patient If a service is unable to contact a patient, the following protocol must be followed before the patient is discharged: Patient receives a minimum of two telephone calls. These sets (from first to last) of calls must be at least one week apart on different days and one am and one pm. If there is no response from the patient, the patient must be sent an appointment in the post. This appointment must be at least five days away.
14 If the patient fails to attend this appointment, they will be discharged, depending upon the requirements of each specific contract. The following patients will not be discharged without clinician over read: Children Vulnerable patients Breach patients in accordance with local policies The discharge letter back to the GP will state why the patient has been discharged, should the GP wish to re-refer this patient they will follow the pathway and be seen within four weeks This applies to all clinics. Communication Under the Human Rights Act, the Equal Opportunities Acts and anti-discrimination legislation, Newmedica has a duty to provide interpreters for appointments when requested and to ensure reasonable adjustments are made for those patients and their families. Interpretation can be managed via the telephone interpretation service or face-to-face with an interpreter present. Overseas Visitors Before patients can access any community services, they must have registered with a GP and so will have satisfied eligibility for free NHS care at that time. If the patient bypasses/negates this process then Newmedica will initiate retrieval of NHS costs. Glossary RTT Referral to Treatment PTL Patient Tracking List DNA Patient did not attend Active Monitoring - An 18w clock may be stopped where it is clinically appropriate to start a period of monitoring in secondary care without clinical intervention or diagnostic procedures. A new 18- week clock would start when a decision to treat is made following a period of active monitoring NHS e-referral service - A method of electronically booking a patient into the service of their choice. First Definitive Treatment - An intervention intended to manage a patient s disease, condition or injury and avoid further intervention. What constitutes First Definitive Treatment is a matter for clinical judgement, in consultation with others as appropriate, including the patient.
15 Key References Accessible Information Standard. Available from: < NHS e-referral Service. Available from: < Equality Act Available from: < Guide to NHS Waiting Times. Available from: < to%20waiting%20times.aspx> Human Rights Act Available from: < Referral to treatment consultant-led waiting times - How to Measure. Available from: < Measure-Jan Final.pdf> 2014/15 Choice Framework. Available from: < Links Please see also: Policy for Dignity in Care Policy for Monitoring Patients Views Control of Documents and Records Procedure Policy for Infection Prevention and Control Policy for Safeguarding Vulnerable Adults Policy for Consent & Mental Capacity Policy for Information Management and Access to Health Records Policy for Maintenance of Health CarePremises Policy for Medicines Management Policy for Safeguarding Children
PATIENT ACCESS POLICY
 V 9.1 PATIENT ACCESS POLICY Reference Number: POL- COR/1825/11 (OLD REF NO.COR/2011/002 Version / Amendment History Version: 9.1 Status: Draft Author: Roger McBroom Title: Head of Patient Access and Administration
V 9.1 PATIENT ACCESS POLICY Reference Number: POL- COR/1825/11 (OLD REF NO.COR/2011/002 Version / Amendment History Version: 9.1 Status: Draft Author: Roger McBroom Title: Head of Patient Access and Administration
REFERRAL TO TREATMENT ACCESS POLICY
 Directorate of Strategy & Planning REFERRAL TO TREATMENT ACCESS POLICY Reference: DCP175 Version: 7.0 This version issued: 17/12/15 Result of last review: Major changes Date approved by owner (if applicable):
Directorate of Strategy & Planning REFERRAL TO TREATMENT ACCESS POLICY Reference: DCP175 Version: 7.0 This version issued: 17/12/15 Result of last review: Major changes Date approved by owner (if applicable):
NOTTINGHAM UNIVERSITY HOSPITAL NHS TRUST. PATIENT ACCESS MANAGEMENT POLICY (Previously known as Waiting List Management Policy) Documentation Control
 NOTTINGHAM UNIVERSITY HOSPITAL NHS TRUST PATIENT ACCESS MANAGEMENT POLICY (Previously known as Waiting List Management Policy) Documentation Control Reference CL/CGP/026 Approving Body Senior Management
NOTTINGHAM UNIVERSITY HOSPITAL NHS TRUST PATIENT ACCESS MANAGEMENT POLICY (Previously known as Waiting List Management Policy) Documentation Control Reference CL/CGP/026 Approving Body Senior Management
Author: Kelvin Grabham, Associate Director of Performance & Information
 Trust Policy Title: Access Policy Author: Kelvin Grabham, Associate Director of Performance & Information Document Lead: Kelvin Grabham, Associate Director of Performance & Information Accepted by: RTT
Trust Policy Title: Access Policy Author: Kelvin Grabham, Associate Director of Performance & Information Document Lead: Kelvin Grabham, Associate Director of Performance & Information Accepted by: RTT
Rapid improvement guide to appointment slot issues
 Rapid improvement guide to appointment slot issues October 2017 This guidance provides information to help providers maintain high standards of clinical care by minimising and managing the number of patients
Rapid improvement guide to appointment slot issues October 2017 This guidance provides information to help providers maintain high standards of clinical care by minimising and managing the number of patients
Patient Access Policy
 Patient Access Policy SPONSOR (Information Asset Owner): Chief Operating Officer AUTHOR (Information Asset Administrator): Gina Quantrill Associate Director Elective Care RATIFIED BY: Document Management
Patient Access Policy SPONSOR (Information Asset Owner): Chief Operating Officer AUTHOR (Information Asset Administrator): Gina Quantrill Associate Director Elective Care RATIFIED BY: Document Management
Referral to Treatment (RTT) Access Policy
 General Referral to Treatment (RTT) Access Policy This is a controlled document and whilst this document may be printed, the electronic version posted on the intranet/shared drive is the controlled copy.
General Referral to Treatment (RTT) Access Policy This is a controlled document and whilst this document may be printed, the electronic version posted on the intranet/shared drive is the controlled copy.
Quick Reference Sheet for Elective Access Policy: EDM006 V5.1
 Quick Reference Sheet for Elective Access Policy: EDM006 V5.1 Sets out how Trust staff manage patients referred for elective assessment and treatment including: o o o o Outpatient appointments Elective
Quick Reference Sheet for Elective Access Policy: EDM006 V5.1 Sets out how Trust staff manage patients referred for elective assessment and treatment including: o o o o Outpatient appointments Elective
18 Weeks Referral to Treatment Guidance (Access Policy)
 18 Weeks Referral to Treatment Guidance (Access Policy) CATEGORY: Guidelines CLASSIFICATION: Clinical PURPOSE: To provide guidance on the management of the 18 week referral to treatment pathway Controlled
18 Weeks Referral to Treatment Guidance (Access Policy) CATEGORY: Guidelines CLASSIFICATION: Clinical PURPOSE: To provide guidance on the management of the 18 week referral to treatment pathway Controlled
Document Management Section (if applicable) Previous policy number NA Previous version
 Policy Title Patient Access Policy Version Policy Number 0059 5 number All administrative / clerical / managerial staff Applicable to involved in the administration of patient pathway. All medical and
Policy Title Patient Access Policy Version Policy Number 0059 5 number All administrative / clerical / managerial staff Applicable to involved in the administration of patient pathway. All medical and
SWH Patient Access Policy
 Information and Performance The Trust s Intranet holds the current approved guidance documents. Notice to staff using a paper copy of this document. Staff must ensure that they are using the most up-to-date
Information and Performance The Trust s Intranet holds the current approved guidance documents. Notice to staff using a paper copy of this document. Staff must ensure that they are using the most up-to-date
BNSSG Elective Care Access Policy
 BNSSG Elective Care Access Policy North Bristol Hospitals NHS Trust University Hospitals Bristol NHS Foundation Trust Weston Area Health NHS Trust NHS Bristol CCG NHS North Somerset CCG NHS South Gloucestershire
BNSSG Elective Care Access Policy North Bristol Hospitals NHS Trust University Hospitals Bristol NHS Foundation Trust Weston Area Health NHS Trust NHS Bristol CCG NHS North Somerset CCG NHS South Gloucestershire
PATIENT ACCESS POLICY
 PATIENT ACCESS POLIC Document Reference No. CORP002v9.9 Version No. 9.9 Issue Date June 2017 Review Date March 2020 Document Author Head of Access, Booking & Choice Document Owner Accountable Executive
PATIENT ACCESS POLIC Document Reference No. CORP002v9.9 Version No. 9.9 Issue Date June 2017 Review Date March 2020 Document Author Head of Access, Booking & Choice Document Owner Accountable Executive
PATIENT RIGHTS ACT (SCOTLAND) 2011 ACCESS POLICY FOR TREATMENT TIME GUARANTEE
 NHS Board Meeting Tuesday 16 October 2012 Chief Operating Officer (Acute Services Division) Board Paper No. 12/45 PATIENT RIGHTS ACT (SCOTLAND) 2011 ACCESS POLICY FOR TREATMENT TIME GUARANTEE Recommendation:
NHS Board Meeting Tuesday 16 October 2012 Chief Operating Officer (Acute Services Division) Board Paper No. 12/45 PATIENT RIGHTS ACT (SCOTLAND) 2011 ACCESS POLICY FOR TREATMENT TIME GUARANTEE Recommendation:
Patient Access Policy
 Version Date Purpose of Issue/Description of Change Review Date 2.0 3.0 4.0 4.1 Status August 2009 December 2011 November 2014 November 2015 Interim Review Full review to ensure policy is up to date and
Version Date Purpose of Issue/Description of Change Review Date 2.0 3.0 4.0 4.1 Status August 2009 December 2011 November 2014 November 2015 Interim Review Full review to ensure policy is up to date and
Commissioning Policy
 Commissioning Policy Consultant to Consultant Referrals Version 6.0 December 2017 Name of Responsible Board / Committee for Ratification: North Staffordshire CCG Stoke on Trent CCG Date Issued: November
Commissioning Policy Consultant to Consultant Referrals Version 6.0 December 2017 Name of Responsible Board / Committee for Ratification: North Staffordshire CCG Stoke on Trent CCG Date Issued: November
NHS BOLTON CLINICAL COMMISSIONING GROUP Public Board Meeting AGENDA ITEM NO: 12. Date of Meeting: 30 th March 2016
 NHS BOLTON CLINICAL COMMISSIONING GROUP Public Board Meeting AGENDA ITEM NO: 12 Date of Meeting: 30 th March 2016 TITLE OF REPORT: AUTHOR: PRESENTED BY: PURPOSE OF PAPER: (Linking to Strategic Objectives)
NHS BOLTON CLINICAL COMMISSIONING GROUP Public Board Meeting AGENDA ITEM NO: 12 Date of Meeting: 30 th March 2016 TITLE OF REPORT: AUTHOR: PRESENTED BY: PURPOSE OF PAPER: (Linking to Strategic Objectives)
Understanding the 18 week elective pathway and referral process, your rights and responsibilities
 Understanding the 18 week elective pathway and referral process, your rights and responsibilities Buckinghamshire Healthcare NHS Trust is committed to providing timely access to services and treatment
Understanding the 18 week elective pathway and referral process, your rights and responsibilities Buckinghamshire Healthcare NHS Trust is committed to providing timely access to services and treatment
Managing Waiting Lists and Handling Referrals Nickie Yates, Head of Information & Contracting
 Trust Policy and Procedure Document Ref. No: PP(13)138 Patient Access Policy For use in: For use by: For use for: Document owner: Other Contributors Status: Trust Wide All Staff Managing Waiting Lists
Trust Policy and Procedure Document Ref. No: PP(13)138 Patient Access Policy For use in: For use by: For use for: Document owner: Other Contributors Status: Trust Wide All Staff Managing Waiting Lists
Trust Operational Policy. Elective Access
 Trust Operational Policy Elective Access Document Control Author/Contact Jo Henshaw, General Manager and Divisional Head of Performance, Scheduled Care Division. Document Reference 2077 Impact Assessment
Trust Operational Policy Elective Access Document Control Author/Contact Jo Henshaw, General Manager and Divisional Head of Performance, Scheduled Care Division. Document Reference 2077 Impact Assessment
Patient Access Policy
 Post holder responsible for Procedural Document Author of Policy Division /Department responsible for Procedural Document Operations Director Principal Access Analyst Operations Support Unit Contact details:
Post holder responsible for Procedural Document Author of Policy Division /Department responsible for Procedural Document Operations Director Principal Access Analyst Operations Support Unit Contact details:
Access Management Policy
 Access Management Policy Document Type: Policy Version: 3.1 Date of Issue: April 2014 Review Date: April 2016 Lead Director: Post Responsible for Update: Ratifying Committee: Ratified by them in the minutes
Access Management Policy Document Type: Policy Version: 3.1 Date of Issue: April 2014 Review Date: April 2016 Lead Director: Post Responsible for Update: Ratifying Committee: Ratified by them in the minutes
Access, Booking and Choice Policy and Operational Procedures
 Access, Booking and Choice Policy and Operational Procedures Date Approved Ratifying Body Related Documents Author Owner (Executive Director) Directorate Superseded Documents Subject Access Improvement
Access, Booking and Choice Policy and Operational Procedures Date Approved Ratifying Body Related Documents Author Owner (Executive Director) Directorate Superseded Documents Subject Access Improvement
Date Completed 23 April 2015 Final Document. Policy Approval Group Approval. Date Approved 23 March 2015 Other Specialist committee(s) recommending
 Elective Care Access Policy - HH(1)/CO/723/15 Previous document(s) being replaced Location Policy No Policy Name HHFT HH/CO/520/12 Access Policy Document Summary This policy provides an overview of the
Elective Care Access Policy - HH(1)/CO/723/15 Previous document(s) being replaced Location Policy No Policy Name HHFT HH/CO/520/12 Access Policy Document Summary This policy provides an overview of the
Clinical Assessment Services
 NHS e-referral Service Clinical Assessment Services What is a Clinical Assessment Service? A Clinical Assessment Service (CAS) is an intermediate service that allows for a greater level of clinical expertise
NHS e-referral Service Clinical Assessment Services What is a Clinical Assessment Service? A Clinical Assessment Service (CAS) is an intermediate service that allows for a greater level of clinical expertise
Elective Access Policy
 Elective Access Policy Version: 1.0 Date Effective: January 2014 Author: Assistant Director of Clinical Services (Access and Performance) Equality Impact 31 st December 2013 Assessment: Consultation: Divisional
Elective Access Policy Version: 1.0 Date Effective: January 2014 Author: Assistant Director of Clinical Services (Access and Performance) Equality Impact 31 st December 2013 Assessment: Consultation: Divisional
Local Health Economy Elective Care Access Policy
 The Shrewsbury and Telford Hospital NHS Trust Shropshire Clinical Commissioning Group Telford and Wrekin Clinical Commissioning Group Local Health Economy Elective Care Access Policy Author Andrena Weston
The Shrewsbury and Telford Hospital NHS Trust Shropshire Clinical Commissioning Group Telford and Wrekin Clinical Commissioning Group Local Health Economy Elective Care Access Policy Author Andrena Weston
Countess of Chester Hospital NHS Foundation Trust Access Policy
 Countess of Chester Hospital NHS Foundation Trust Access Policy Written by: Supported by: Matt Butcher - BPM Access Gena Rothwell Access Hayley Carey Access Rena Erskine Access Denise Wood IMT Joe O Grady
Countess of Chester Hospital NHS Foundation Trust Access Policy Written by: Supported by: Matt Butcher - BPM Access Gena Rothwell Access Hayley Carey Access Rena Erskine Access Denise Wood IMT Joe O Grady
ACCESS POLICY FOR ELECTIVE CARE PATHWAYS
 ACCESS POLICY FOR ELECTIVE CARE PATHWAYS Policy Reference Number Version November 2014 Ratified By Trust Executive committee Date Ratified 19 November 2014 Name/title of originator/policy author(s) Jackie
ACCESS POLICY FOR ELECTIVE CARE PATHWAYS Policy Reference Number Version November 2014 Ratified By Trust Executive committee Date Ratified 19 November 2014 Name/title of originator/policy author(s) Jackie
PATIENT ACCESS POLICY & USER MANUAL
 PATIENT ACCESS POLICY & USER MANUAL Controlled document This document is uncontrolled when downloaded or printed. Reference number Version 16 Author & Job Title WHHT: C056 Jane Shentall, Director of Performance
PATIENT ACCESS POLICY & USER MANUAL Controlled document This document is uncontrolled when downloaded or printed. Reference number Version 16 Author & Job Title WHHT: C056 Jane Shentall, Director of Performance
Elective Services Access Policy Access to Elective Care Pathways
 SH CP 152 Elective Services Access Policy Access to Elective Care Pathways Version: 2 Summary: Keywords (minimum of 5): (To assist policy search engine) Target Audience: The policy reflects current national
SH CP 152 Elective Services Access Policy Access to Elective Care Pathways Version: 2 Summary: Keywords (minimum of 5): (To assist policy search engine) Target Audience: The policy reflects current national
Did Not Attend (DNA) and Cancellation Policy and Operational Guidelines
 Did Not Attend (DNA) and Cancellation Policy and Operational Guidelines Document Number Version Ratified By & Date Name of Approving Body(s) & Date(s) FPE-004 V1 Safety and Effectiveness Sub-Committee
Did Not Attend (DNA) and Cancellation Policy and Operational Guidelines Document Number Version Ratified By & Date Name of Approving Body(s) & Date(s) FPE-004 V1 Safety and Effectiveness Sub-Committee
RTT Assurance Paper. 1. Introduction. 2. Background. 3. Waiting List Management for Elective Care. a. Planning
 RTT Assurance Paper 1. Introduction The purpose of this paper is to provide assurance to Trust Board in relation to the robust management of waiting lists and timely delivery of elective patient care within
RTT Assurance Paper 1. Introduction The purpose of this paper is to provide assurance to Trust Board in relation to the robust management of waiting lists and timely delivery of elective patient care within
Trust-wide Policy. For. Access Policy
 Trust-wide Policy For Access Policy A document recommended for use In: All departments / Divisions By: All staff For: Managing patients care pathways & compliance to NHS constitution and Care Quality Commission
Trust-wide Policy For Access Policy A document recommended for use In: All departments / Divisions By: All staff For: Managing patients care pathways & compliance to NHS constitution and Care Quality Commission
Patient Access to Treatment. Policy and Procedure (RTT 18 weeks)
 MAIDSTONE AND TUNBRIDGE WELLS NHS TRUST Patient Access to Treatment Policy and Procedure (RTT 18 weeks) Requested/ Required by: Main author: Other contributors: Document lead: Directorate: Specialty: Directorates
MAIDSTONE AND TUNBRIDGE WELLS NHS TRUST Patient Access to Treatment Policy and Procedure (RTT 18 weeks) Requested/ Required by: Main author: Other contributors: Document lead: Directorate: Specialty: Directorates
18 Weeks Referral to Treatment (RTT) Waiting times
 Patient Access Policy 18 Weeks Referral to Treatment (RTT) Waiting times King s College Hospital NHS Foundation Trust is committed to providing timely access to services and treatment for all patients
Patient Access Policy 18 Weeks Referral to Treatment (RTT) Waiting times King s College Hospital NHS Foundation Trust is committed to providing timely access to services and treatment for all patients
PATIENT ACCESS POLICY
 PATIENT ACCESS POLICY Version 6 DOCUMENT NUMBER APPROVING COMMITTEE STHK0075 Executive Team DATE APPROVED 01 August 2016 DATE IMPLEMENTED 01 August 2016 NEXT REVIEW DATE 01 August 2017 ACCOUNTABLE DIRECTOR
PATIENT ACCESS POLICY Version 6 DOCUMENT NUMBER APPROVING COMMITTEE STHK0075 Executive Team DATE APPROVED 01 August 2016 DATE IMPLEMENTED 01 August 2016 NEXT REVIEW DATE 01 August 2017 ACCOUNTABLE DIRECTOR
NHS standard contract letter templates for practice use
 1 Use the hyperlinks to quickly reach each appendix. Appendix 1 Template response for missed appointment Letter to Trust requesting that the hospital liaises directly with a patient who has missed an outpatient
1 Use the hyperlinks to quickly reach each appendix. Appendix 1 Template response for missed appointment Letter to Trust requesting that the hospital liaises directly with a patient who has missed an outpatient
62 days from referral with urgent suspected cancer to initiation of treatment
 Appendix-2012-87 Borders NHS Board PATIENT ACCESS POLICY Aim In preparation for the introduction of the Patients Rights (Scotland) Act 2011, NHS Borders has produced a Patient Access Policy governing the
Appendix-2012-87 Borders NHS Board PATIENT ACCESS POLICY Aim In preparation for the introduction of the Patients Rights (Scotland) Act 2011, NHS Borders has produced a Patient Access Policy governing the
How to write and review an access policy in line with best practice for referral to treatment and cancer pathways. July 2018
 How to write and review an access policy in line with best practice for referral to treatment and cancer pathways July 2018 What is covered? Why is an access policy important? What is the purpose of an
How to write and review an access policy in line with best practice for referral to treatment and cancer pathways July 2018 What is covered? Why is an access policy important? What is the purpose of an
NHS BORDERS PATIENT ACCESS POLICY
 NHS BORDERS PATIENT ACCESS POLICY 1. BACKGROUND NHS Borders is required by Scottish Government to deliver a consistent, safe, equitable and patient centred service to Borders patients within national waiting
NHS BORDERS PATIENT ACCESS POLICY 1. BACKGROUND NHS Borders is required by Scottish Government to deliver a consistent, safe, equitable and patient centred service to Borders patients within national waiting
Corporate. Visitors & VIP s Standard Operating Procedure. Document Control Summary. Contents
 Corporate Visitors & VIP s Standard Operating Procedure Document Control Summary Status: Version: Author/Owner: Approved by: Ratified: Related Trust Strategy and/or Strategic Aims Implementation Date:
Corporate Visitors & VIP s Standard Operating Procedure Document Control Summary Status: Version: Author/Owner: Approved by: Ratified: Related Trust Strategy and/or Strategic Aims Implementation Date:
ELECTIVE CARE PATIENT ACCESS POLICY
 Index No: W10a ELECTIVE CARE PATIENT ACCESS POLICY Version: 5.1 Date ratified: 25 th April 2017 Ratified by: (Name of Committee) Name of originator/author, job title and department: Director Lead (Trust-wide
Index No: W10a ELECTIVE CARE PATIENT ACCESS POLICY Version: 5.1 Date ratified: 25 th April 2017 Ratified by: (Name of Committee) Name of originator/author, job title and department: Director Lead (Trust-wide
NHS FORTH VALLEY. Access Policy Version 2.9
 NHS FORTH VALLEY Access Policy Version 2.9 Date of First Issue 01/06/2012 Approved 01/09/2012 Current Issue Date 01/04/2017 Review Date 01/04/2019 Version 2.9 EQIA Yes 16/01/2013 Author / Contact Roslyn
NHS FORTH VALLEY Access Policy Version 2.9 Date of First Issue 01/06/2012 Approved 01/09/2012 Current Issue Date 01/04/2017 Review Date 01/04/2019 Version 2.9 EQIA Yes 16/01/2013 Author / Contact Roslyn
Implementation of the right to access services within maximum waiting times
 Implementation of the right to access services within maximum waiting times Guidance for strategic health authorities, primary care trusts and providers DH INFORMATION READER BOX Policy HR / Workforce
Implementation of the right to access services within maximum waiting times Guidance for strategic health authorities, primary care trusts and providers DH INFORMATION READER BOX Policy HR / Workforce
NORTH EAST ESSEX CLINICAL COMMISSIONING GROUP CONSULTANT TO CONSULTANT REFERRAL POLICY
 PLEASE NOTE POLICY IS UNDER REVIEW NORTH EAST ESSEX CLINICAL COMMISSIONING GROUP CONSULTANT TO CONSULTANT REFERRAL POLICY Target Audience Brief Description (max 50 words) Action Required Providers, Commissioners
PLEASE NOTE POLICY IS UNDER REVIEW NORTH EAST ESSEX CLINICAL COMMISSIONING GROUP CONSULTANT TO CONSULTANT REFERRAL POLICY Target Audience Brief Description (max 50 words) Action Required Providers, Commissioners
Managing Community Access and the management of appointments
 TRUST-WIDE CLINICAL POLICY DOCUMENT Managing Community Access and the management of appointments Policy Number: Scope of this Document: Recommending Committee: Approving Committee: SD08 All Staff Trust
TRUST-WIDE CLINICAL POLICY DOCUMENT Managing Community Access and the management of appointments Policy Number: Scope of this Document: Recommending Committee: Approving Committee: SD08 All Staff Trust
Elective Access Policy
 Seamless Delivery and Excellence in Health Care and Outcomes Elective Access Policy April 2016 CG585 April 2016 Produced by RBFT Head of Access and Performance Target Audience Referrers, Patients, Commissioners
Seamless Delivery and Excellence in Health Care and Outcomes Elective Access Policy April 2016 CG585 April 2016 Produced by RBFT Head of Access and Performance Target Audience Referrers, Patients, Commissioners
NHS e-referral Service (e-rs) Frequently Asked Questions for Referrers
 NHS e-referral Service (e-rs) Frequently Asked Questions for Referrers Purpose Primary Care colleagues are sometimes faced with situations regarding referrals and may not necessarily know the correct action
NHS e-referral Service (e-rs) Frequently Asked Questions for Referrers Purpose Primary Care colleagues are sometimes faced with situations regarding referrals and may not necessarily know the correct action
National Waiting List Management Protocol
 National Waiting List Management Protocol A standardised approach to managing scheduled care treatment for in-patient, day case and planned procedures January 2014 an ciste náisiúnta um cheannach cóireála
National Waiting List Management Protocol A standardised approach to managing scheduled care treatment for in-patient, day case and planned procedures January 2014 an ciste náisiúnta um cheannach cóireála
Committee is requested to action as follows: Richard Walker. Dylan Williams
 BetsiCadwaladrUniversityHealthBoard Committee Paper 17.11.14 Item IG14_60 NameofCommittee: Subject: Summary or IssuesofSignificance StrategicTheme/Priority / Valuesaddressedbythispaper Information Governance
BetsiCadwaladrUniversityHealthBoard Committee Paper 17.11.14 Item IG14_60 NameofCommittee: Subject: Summary or IssuesofSignificance StrategicTheme/Priority / Valuesaddressedbythispaper Information Governance
Healthwatch England Escalation Guidance
 Healthwatch England Escalation Guidance This guidance provides information on how to do four things: 1) Collating people s views and experiences of care services from local Healthwatch 2) Highlighting
Healthwatch England Escalation Guidance This guidance provides information on how to do four things: 1) Collating people s views and experiences of care services from local Healthwatch 2) Highlighting
Hospital Generated Inter-Speciality Referral Policy Supporting people in Dorset to lead healthier lives
 NHS Dorset Clinical Commissioning Group Hospital Generated Inter-Speciality Referral Policy Supporting people in Dorset to lead healthier lives PREFACE This Document outlines the CCG s policy in respect
NHS Dorset Clinical Commissioning Group Hospital Generated Inter-Speciality Referral Policy Supporting people in Dorset to lead healthier lives PREFACE This Document outlines the CCG s policy in respect
Clinical Sub Category Review date February 2016 Distribution Who the policy will be Distributed to senior staff as defined by directors
 Document Details Title Patient Access Policy Incorporating the management of appointments and Did Not Attend (DNA) Trust Ref No 1613-24356 Local Ref (optional) Main points the document To ensure the effective
Document Details Title Patient Access Policy Incorporating the management of appointments and Did Not Attend (DNA) Trust Ref No 1613-24356 Local Ref (optional) Main points the document To ensure the effective
Waiting List Management and Patient Access Policy
 Waiting List Management and Patient Access Policy Document Reference Document status Target Audience OP.WL.V5.0 Final Clinical Directors, Consultants, Nurses, Directorate Managers, Waiting List Managers,
Waiting List Management and Patient Access Policy Document Reference Document status Target Audience OP.WL.V5.0 Final Clinical Directors, Consultants, Nurses, Directorate Managers, Waiting List Managers,
The interface between primary and secondary care Key messages for NHS clinicians and managers
 The interface between primary and secondary care Key messages for NHS clinicians and managers In partnership with: NHS England and NHS Improvement 2 Good organisation of care across the interface between
The interface between primary and secondary care Key messages for NHS clinicians and managers In partnership with: NHS England and NHS Improvement 2 Good organisation of care across the interface between
Patient Access Policy for Elective Treatment
 Patient Access Policy for Elective Treatment This document is uncontrolled once printed. Please check on the Trust s Intranet site for the most up-to-date version. Policy number: LNWHT/CQR/030/2017 Name
Patient Access Policy for Elective Treatment This document is uncontrolled once printed. Please check on the Trust s Intranet site for the most up-to-date version. Policy number: LNWHT/CQR/030/2017 Name
This procedural document supersedes the previous procedural documents for Policy for the Management of Patients/Clients Access to Services
 Patient Access Policy November 2013 This procedural document supersedes the previous procedural documents for Policy for the Management of Patients/Clients Access to Services Version: 1.0 Policy reference
Patient Access Policy November 2013 This procedural document supersedes the previous procedural documents for Policy for the Management of Patients/Clients Access to Services Version: 1.0 Policy reference
ALLOCATION OF RESOURCES POLICY FOR CONTINUING HEALTHCARE FUNDED INDIVIDUALS
 ALLOCATION OF RESOURCES POLICY FOR CONTINUING HEALTHCARE FUNDED INDIVIDUALS APPROVED BY: South Gloucestershire Clinical Commissioning Group Quality and Governance Committee DATE Date of Issue:- Version
ALLOCATION OF RESOURCES POLICY FOR CONTINUING HEALTHCARE FUNDED INDIVIDUALS APPROVED BY: South Gloucestershire Clinical Commissioning Group Quality and Governance Committee DATE Date of Issue:- Version
Quality Accounts: Corroborative Statements from Commissioning Groups. Nottingham NHS Treatment Centre - Corroborative Statement
 Quality Accounts: Corroborative Statements from Commissioning Groups Quality Accounts are annual reports to the public from providers of NHS healthcare about the quality of services they deliver. The primary
Quality Accounts: Corroborative Statements from Commissioning Groups Quality Accounts are annual reports to the public from providers of NHS healthcare about the quality of services they deliver. The primary
Access Policy. Scheduled Care
 Access Policy Scheduled Care Name of Author and Job Title: Name of Review/Development Body: Ratification Body: Date of Ratification/Effective from: Luigi Federico RTT Lead ELT Clinical Quality Governance
Access Policy Scheduled Care Name of Author and Job Title: Name of Review/Development Body: Ratification Body: Date of Ratification/Effective from: Luigi Federico RTT Lead ELT Clinical Quality Governance
Medicines Governance Service to Care Homes (Care Home Service)
 Medicines Governance Service to Care Homes (Care Home Service) Locally Enhanced Service Authors: Ruth Buchan, Senior Pharmacist Medicines Management 4th Floor F Mill Dean Clough Halifax HX3 5AX Tel-01422
Medicines Governance Service to Care Homes (Care Home Service) Locally Enhanced Service Authors: Ruth Buchan, Senior Pharmacist Medicines Management 4th Floor F Mill Dean Clough Halifax HX3 5AX Tel-01422
NHS Dumfries and Galloway Patient Access Policy
 NHS Dumfries and Galloway Patient Access Policy Printed copies must not be considered the definitive version DOCUMENT CONTROL POLICY NO. Policy Group Author Version no. 1.3 Reviewer Waiting Times Group
NHS Dumfries and Galloway Patient Access Policy Printed copies must not be considered the definitive version DOCUMENT CONTROL POLICY NO. Policy Group Author Version no. 1.3 Reviewer Waiting Times Group
The non-executive director s guide to NHS data Part one: Hospital activity, data sets and performance
 Briefing October 2017 The non-executive director s guide to NHS data Part one: Hospital activity, data sets and performance Key points As a non-executive director, it is important to understand how data
Briefing October 2017 The non-executive director s guide to NHS data Part one: Hospital activity, data sets and performance Key points As a non-executive director, it is important to understand how data
Job Description. CNS Clinical Lead
 Job Description CNS Clinical Lead POST: BASE: ACCOUNTABLE TO: REPORTS TO: RESPONSIBLE FOR: CNS Clinical Lead St John s Hospice Head of Nursing and Quality Head of Nursing and Quality Community Clinical
Job Description CNS Clinical Lead POST: BASE: ACCOUNTABLE TO: REPORTS TO: RESPONSIBLE FOR: CNS Clinical Lead St John s Hospice Head of Nursing and Quality Head of Nursing and Quality Community Clinical
DRAFT CONTINUING HEALTHCARE (CHC) CHOICE & EQUITY POLICY. Version 2
 DRAFT CONTINUING HEALTHCARE (CHC) CHOICE & EQUITY POLICY Version 2 1 Subject and version number of document: Continuing Healthcare (CHC) and Funded Nursing Care (FNC) Choice and Equity Policy Serial number:
DRAFT CONTINUING HEALTHCARE (CHC) CHOICE & EQUITY POLICY Version 2 1 Subject and version number of document: Continuing Healthcare (CHC) and Funded Nursing Care (FNC) Choice and Equity Policy Serial number:
OFFICIAL. NHS e-referral Service: guidance for managing referrals
 NHS e-referral Service: guidance for managing referrals April 2018 1 NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops.
NHS e-referral Service: guidance for managing referrals April 2018 1 NHS England INFORMATION READER BOX Directorate Medical Operations and Information Specialised Commissioning Nursing Trans. & Corp. Ops.
PATIENT ACCESS POLICY (ELECTIVE CARE) UHB 033 Version No: 1 Previous Trust / LHB Ref No: Senior Manager, Performance and Compliance.
 Reference No: PATIENT ACCESS POLICY (ELECTIVE CARE) UHB 033 Version No: 1 Previous Trust / LHB Ref No: Trust 364 Documents to read alongside this Policy. Ministerial Letter EH/ML/004/09 WAG Rules for Managing
Reference No: PATIENT ACCESS POLICY (ELECTIVE CARE) UHB 033 Version No: 1 Previous Trust / LHB Ref No: Trust 364 Documents to read alongside this Policy. Ministerial Letter EH/ML/004/09 WAG Rules for Managing
CHAPTER TWO: WAITING LISTS AND BOOKING
 TWO: INTRODUCTION Managing waiting lists 2.1 Sometimes it seems that the NHS is primarily about waiting lists. Public perception focuses on waiting lists. Waiting lists provide media headlines. For those
TWO: INTRODUCTION Managing waiting lists 2.1 Sometimes it seems that the NHS is primarily about waiting lists. Public perception focuses on waiting lists. Waiting lists provide media headlines. For those
Offering Advice & Guidance: Supplementary Guidance for CQUIN Indicator 6. August 2017
 Offering Advice & Guidance: Supplementary Guidance for CQUIN Indicator 6 August 2017 This information can be made available in alternative formats, such as easy read or large print, and may be available
Offering Advice & Guidance: Supplementary Guidance for CQUIN Indicator 6 August 2017 This information can be made available in alternative formats, such as easy read or large print, and may be available
NHS LANARKSHIRE PATIENT ACCESS POLICY
 NHS LANARKSHIRE PATIENT ACCESS POLICY 1. BACKGROUND NHS Lanarkshire is required by Scottish Government to deliver a consistent, safe, equitable and patient centred service to Lanarkshire patients within
NHS LANARKSHIRE PATIENT ACCESS POLICY 1. BACKGROUND NHS Lanarkshire is required by Scottish Government to deliver a consistent, safe, equitable and patient centred service to Lanarkshire patients within
Assessment Framework for Designated Centres for Persons (Children and Adults) with Disabilities
 Assessment Framework for Designated Centres for Persons (Children and Adults) with Disabilities January, 2015 1 About the The (HIQA) is the independent Authority established to drive high quality and safe
Assessment Framework for Designated Centres for Persons (Children and Adults) with Disabilities January, 2015 1 About the The (HIQA) is the independent Authority established to drive high quality and safe
Patient Access and Waiting Times Management. NHS Tayside Access Policy
 Tayside NHS Board Report 25 th October 2012 APPENDIX 1 Patient Access and Waiting Times Management NHS Tayside Access Policy Policy Manager Kerry Wilson Policy Group Policy Established September 2012 Policy
Tayside NHS Board Report 25 th October 2012 APPENDIX 1 Patient Access and Waiting Times Management NHS Tayside Access Policy Policy Manager Kerry Wilson Policy Group Policy Established September 2012 Policy
Performance. Improvement in Scheduled Care Waiting List Management TOOLKIT. An Roinn Sláinte DEPARTMENT OF HEALTH. January 2013
 Performance TOOLKIT in Scheduled Care January 2013 Patient Toolkit Pathways Performance in Scheduled Care Setting the context and initiating whole systems change for the delivery of scheduled care and
Performance TOOLKIT in Scheduled Care January 2013 Patient Toolkit Pathways Performance in Scheduled Care Setting the context and initiating whole systems change for the delivery of scheduled care and
Policy on the Commissioning of NHS Continuing Healthcare for Adults: Assuring Equity, Choice and Value for Money
 Policy Statement No. Salford Clinical Commissioning Group Policy on the Commissioning of NHS Continuing Healthcare for Adults: Assuring Equity, Choice and Value for Money Lead for development & revisions
Policy Statement No. Salford Clinical Commissioning Group Policy on the Commissioning of NHS Continuing Healthcare for Adults: Assuring Equity, Choice and Value for Money Lead for development & revisions
Diagnostics FAQs. Frequently Asked Questions on completing the Diagnostic Waiting Times & Activity monthly data collection
 Diagnostics FAQs Frequently Asked Questions on completing the Diagnostic Waiting Times & Activity monthly data collection First published: October 2006 Updated: 02 February 2015 Prepared by Analytical
Diagnostics FAQs Frequently Asked Questions on completing the Diagnostic Waiting Times & Activity monthly data collection First published: October 2006 Updated: 02 February 2015 Prepared by Analytical
Referral to Treatment (RTT) Validation and Assurance Standard Operating Procedure (SOP) Contents
 Referral to Treatment (RTT) Validation and Assurance Standard Operating Procedure (SOP) Classification: Standard Operating Procedure Lead Author: Toni Coyle, Senior Manager, Access, Booking & Choice Additional
Referral to Treatment (RTT) Validation and Assurance Standard Operating Procedure (SOP) Classification: Standard Operating Procedure Lead Author: Toni Coyle, Senior Manager, Access, Booking & Choice Additional
Performance and Quality Report Sean Morgan Director of Performance and Delivery Mary Hopper Director of Quality Dino Pardhanani, Clinical Director
 Sutton CCG Clinical Commissioning Group Governing Body Date Thursday, 06 September 2018 Document Title Lead Director (Name and Role) Clinical Sponsor (Name and Role) Performance and Quality Report Sean
Sutton CCG Clinical Commissioning Group Governing Body Date Thursday, 06 September 2018 Document Title Lead Director (Name and Role) Clinical Sponsor (Name and Role) Performance and Quality Report Sean
CONTINUING HEALTHCARE (CHC) CHOICE & EQUITY POLICY
 CONTINUING HEALTHCARE (CHC) CHOICE & EQUITY POLICY Ref: Version: Supersedes: Author (inc Job Title): Ratified by: (Name of responsible Committee) Date ratified: To be completed by Corporate Team To be
CONTINUING HEALTHCARE (CHC) CHOICE & EQUITY POLICY Ref: Version: Supersedes: Author (inc Job Title): Ratified by: (Name of responsible Committee) Date ratified: To be completed by Corporate Team To be
This paper aims to provide the Board with a clear picture of how Waiting Lists are managed within NHS Borders.
 Appendix-2012-45 Borders NHS Board MANAGEMENT OF WAITING TIMES Aim This paper aims to provide the Board with a clear picture of how Waiting Lists are managed within NHS Borders. Background NHS Borders
Appendix-2012-45 Borders NHS Board MANAGEMENT OF WAITING TIMES Aim This paper aims to provide the Board with a clear picture of how Waiting Lists are managed within NHS Borders. Background NHS Borders
Action required: To agree the process by which Governors will meet with the inspection team.
 Airedale NHS Foundation Trust Council of Governors: 28 th January 2016 Title: CQC Inspection Briefing Author: Jane Downes, Company Secretary As you will be aware, the Care Quality Commission ( CQC ) have
Airedale NHS Foundation Trust Council of Governors: 28 th January 2016 Title: CQC Inspection Briefing Author: Jane Downes, Company Secretary As you will be aware, the Care Quality Commission ( CQC ) have
DRAFT - NHS CHC and Complex Care Commissioning Policy.
 DRAFT - NHS CHC and Complex Care Commissioning Policy. 1. Introduction 1.1 This policy describes the way the following Clinical Commissioning Groups (CCGs) NHS Wirral Clinical Commissioning Group, NHS
DRAFT - NHS CHC and Complex Care Commissioning Policy. 1. Introduction 1.1 This policy describes the way the following Clinical Commissioning Groups (CCGs) NHS Wirral Clinical Commissioning Group, NHS
Policies, Procedures, Guidelines and Protocols
 Policies, Procedures, Guidelines and Protocols Document Details Title Complaints and Compliments Policy Trust Ref No 1353-29025 Local Ref (optional) N/A Main points the document This policy and procedure
Policies, Procedures, Guidelines and Protocols Document Details Title Complaints and Compliments Policy Trust Ref No 1353-29025 Local Ref (optional) N/A Main points the document This policy and procedure
Staffordshire and Stoke on Trent Adult Safeguarding Partnership Board Safeguarding Adult Reviews (SAR) Protocol
 Staffordshire and Stoke on Trent Adult Safeguarding Partnership Board Safeguarding Adult Reviews (SAR) Protocol SAR Process July 2014 (revised August 2017) Page 1 Contents 1. Introduction 2. Criteria 3.
Staffordshire and Stoke on Trent Adult Safeguarding Partnership Board Safeguarding Adult Reviews (SAR) Protocol SAR Process July 2014 (revised August 2017) Page 1 Contents 1. Introduction 2. Criteria 3.
Creating and Maintaining Services on the Directory of Services
 Creating and Maintaining Services on the Directory of Services A guide for Service Providers Published August 2017 Copyright 2017 Health and Social Care Information Centre. The Health and Social Care Information
Creating and Maintaining Services on the Directory of Services A guide for Service Providers Published August 2017 Copyright 2017 Health and Social Care Information Centre. The Health and Social Care Information
SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY REPORT TO THE TRUST BOARD HELD ON 18 NOVEMBER 2015
 SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY REPORT TO THE TRUST BOARD HELD ON 18 NOVEMBER 2015 Subject: Supporting TEG Member: Authors: Status 1 Data Quality Baseline Assessment
SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY REPORT TO THE TRUST BOARD HELD ON 18 NOVEMBER 2015 Subject: Supporting TEG Member: Authors: Status 1 Data Quality Baseline Assessment
Information for patients
 Information for patients 18-Weeks Maximum Waiting Time from Referral to Treatment (RTT): What does this mean for you? Your rights under the NHS Constitution You have the right to access NHS services within
Information for patients 18-Weeks Maximum Waiting Time from Referral to Treatment (RTT): What does this mean for you? Your rights under the NHS Constitution You have the right to access NHS services within
How CQC monitors, inspects and regulates independent doctors and clinics providing primary care
 How CQC monitors, inspects and regulates independent doctors and clinics providing primary care October 2017 CONTENTS MONITORING AND INFORMATION SHARING... 2 How we monitor independent doctors and clinics
How CQC monitors, inspects and regulates independent doctors and clinics providing primary care October 2017 CONTENTS MONITORING AND INFORMATION SHARING... 2 How we monitor independent doctors and clinics
Continuing Healthcare Policy
 Continuing Healthcare Policy 1 SUMMARY This policy describes the way in which Haringey Clinical Commissioning Group (HCCG) will make provision for the care of people who have been assessed as eligible
Continuing Healthcare Policy 1 SUMMARY This policy describes the way in which Haringey Clinical Commissioning Group (HCCG) will make provision for the care of people who have been assessed as eligible
The Trainee Doctor. Foundation and specialty, including GP training
 Foundation and specialty, including GP training The duties of a doctor registered with the General Medical Council Patients must be able to trust doctors with their lives and health. To justify that trust
Foundation and specialty, including GP training The duties of a doctor registered with the General Medical Council Patients must be able to trust doctors with their lives and health. To justify that trust
The Code Standards of conduct, performance and ethics for chiropractors. Effective from 30 June 2016
 The Code Standards of conduct, performance and ethics for chiropractors Effective from 30 June 2016 2 The Code Standards of conduct, performance and ethics for chiropractors Effective from 30 June 2016
The Code Standards of conduct, performance and ethics for chiropractors Effective from 30 June 2016 2 The Code Standards of conduct, performance and ethics for chiropractors Effective from 30 June 2016
CREATING EFFICIENT OUTPATIENT SERVICES
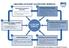 1 CREATING EFFICIENT OUTPATIENT SERVICES Measuring the Demand on the Service How many entry points are there into the service? Who manages the service entry points? Are all of them needed? 6 How can a
1 CREATING EFFICIENT OUTPATIENT SERVICES Measuring the Demand on the Service How many entry points are there into the service? Who manages the service entry points? Are all of them needed? 6 How can a
18 Weeks Referral to Treatment (RTT) Standard Recovery Planning and Assurance Framework
 18 Weeks Referral to Treatment (RTT) Standard Recovery Planning and Assurance Framework Vicky Scott Head of Delivery & Development (North West London) NHS Trust Development Authority Lyndsay Pendegrass
18 Weeks Referral to Treatment (RTT) Standard Recovery Planning and Assurance Framework Vicky Scott Head of Delivery & Development (North West London) NHS Trust Development Authority Lyndsay Pendegrass
We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards.
 Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Sussex Health Care Audiology Ltd Dorking Hospital, Horsham Road,
Inspection Report We are the regulator: Our job is to check whether hospitals, care homes and care services are meeting essential standards. Sussex Health Care Audiology Ltd Dorking Hospital, Horsham Road,
Document Details Clinical Audit Policy
 Title Document Details Clinical Audit Policy Trust Ref No 1538-31104 Main points this document covers This policy details the responsibilities and processes associated with the Clinical Audit process within
Title Document Details Clinical Audit Policy Trust Ref No 1538-31104 Main points this document covers This policy details the responsibilities and processes associated with the Clinical Audit process within
Patient Registration Standard Operating Principles for Primary Medical Care (General Practice)
 Patient Registration Standard Operating Principles for Primary Medical Care (General Practice) NHS England INFORMATION READER BOX Directorate Medical Commissioning Operations Patients and Information Nursing
Patient Registration Standard Operating Principles for Primary Medical Care (General Practice) NHS England INFORMATION READER BOX Directorate Medical Commissioning Operations Patients and Information Nursing
Trust Policy Access Policy For Planned Care Services
 Trust Policy Access Policy For Planned Care Services Purpose Date Version July 2015 2 To inform staff of the key principles for managing patients on an Elective waiting List. Who should read this document?
Trust Policy Access Policy For Planned Care Services Purpose Date Version July 2015 2 To inform staff of the key principles for managing patients on an Elective waiting List. Who should read this document?
QOF Quality and Productivity (QP) Indicators. Supplementary Guidance and Frequently Asked Questions for PCTs and Practices in England
 QOF Quality and Productivity (QP) Indicators Supplementary Guidance and Frequently Asked Questions for PCTs and Practices in England May 2011 Contents Introduction 2 Summary of QP indicators 3 Prescribing
QOF Quality and Productivity (QP) Indicators Supplementary Guidance and Frequently Asked Questions for PCTs and Practices in England May 2011 Contents Introduction 2 Summary of QP indicators 3 Prescribing
NHS Continuing Healthcare and Joint Packages of Health and Social Care Services Commissioning Policy
 NHS Continuing Healthcare and Joint Packages of Health and Social Care Services Commissioning Policy Version History: Version Date Author Reason for change 0.1 3.4.17 Rosa Waddingham based on West Suffolk
NHS Continuing Healthcare and Joint Packages of Health and Social Care Services Commissioning Policy Version History: Version Date Author Reason for change 0.1 3.4.17 Rosa Waddingham based on West Suffolk
NHS ISLE OF WIGHT CLINICAL COMMISSIONING GROUP CLINICAL FUNDING AUTHORISATION POLICY
 NHS ISLE OF WIGHT CLINICAL COMMISSIONING GROUP CLINICAL FUNDING AUTHORISATION POLICY AUTHOR/ APPROVAL DETAILS & VERSION CONTROL Author Version Reason for Change Date Status IW CCG Acute V1 New policy Sept
NHS ISLE OF WIGHT CLINICAL COMMISSIONING GROUP CLINICAL FUNDING AUTHORISATION POLICY AUTHOR/ APPROVAL DETAILS & VERSION CONTROL Author Version Reason for Change Date Status IW CCG Acute V1 New policy Sept
