Adapting to the worsening of the LTMV patient. Mike J. Kampelmacher Home Ventilation Service UMC Utrecht Utrecht, The Netherlands
|
|
|
- Herbert Nelson
- 6 years ago
- Views:
Transcription
1 Adapting to the worsening of the LTMV patient Mike J. Kampelmacher Home Ventilation Service UMC Utrecht Utrecht, The Netherlands
2 Agenda 1. Adaptations in care 2. Education and training 3. Organizational aspects and responsibilities 4. Palliative care + end-of-life issues 5. Conclusion
3 Case 1 Male, 25 yrs, lives with parents Duchenne muscular dystrophy Started 6 yrs earlier with nocturnal NPPV and AS Needs to commence with MPPV and MIE Adaptation needed: more help, care and supervision Family and friends At home and during outside activities At activity center During admissions
4 Adaptations in care for worsening LTMV patients Higher demand for care by family and health care services Greater level of ventilatory dependency Medical complexity Increase in physical assistance Prerequisites for management at home Adequate resources for home care: financial and personnel Adequate numbers of competent caregivers Adequate respite for care givers
5 Adaptations in care (2) Quality of life of family caregivers is negatively influenced by: Tremendous responsibility Sense of duty and obligation to be a caregiver Physical, emotional, financial and social impact of providing care Restrictions on personal time Disturbance of routines Diminished leisure time and outside activities Inability to advance or maintain a job Hudson Med J Austr; Rabkin Amyotroph Lateral Scler; Gelinas J Neurol Sci
6 Adaptations in care (3) Caregiver burden: significant moral issue in care of LTMV patients Major causes of burden for carers looking after LTMV patients: 1. Underlying disease 2. Level op dependency 3. Hours spent under HMV 4. Presence of tracheostomy 5. Home distance from hospital 6. Frequent hospitalisations Caregivers of LTMV patients are potentially at risk for depression (33%), burden, overload and declining health. Practical and effective support for both patients and their families is crucial if LTMV is to be successful. Scott Home Health Care Management & Practice; ACI Respiratory Network consensus statement
7 Adaptations in care (4) Approaches to lessen the burden of informal caregivers: Stability in patient s health Greater affective reward from patients Balanced life style Self-support groups Sufficient support from family members, friends or volunteers Respite care Ready accessibility of community service providers Home visits or home care (telemedicine) Improved professional support: personal assistant and/or skilled nursing care Residential care, nursing home or hospice Huang J Clin Nurs; Evans Can Respir J; ACI Respiratory Network consensus statement
8 Case 2 Male 53, living at home with wife and 3 children ALS, tetraplegic Swallowing problems with pulmonary infections Needs and wants TPPV instead of NPPV Adaptations needed: Increase of (professional) care Organizational aspects: timing, support, safety Education and training Informal care Skilled nursing care Respite care
9 Education and training for worsening LTMV patients Maintaining and developing knowledge, skills and competence Ongoing assessment of skilled nursing care and ongoing education of home care nurses Clinical competence is more than adequate, baseline performance. Essential characteristics of nurse competency required in LTMV: Knowledge Superior technical skills Interpersonal skills Prioritizing Multitasking Autonomous clinical decision making Patient outcomes Boroughs Home Healthcare Nurse
10 Education and training (2) The best prevention of ventilator and tracheostomy emergencies is a vigilant, well-trained caregiver Viligance includes: Anticipating what might be Calculating the risk Monitoring results and outcome Staying ready to act Boroughs Home Healthcare Nurse
11 Education and training (3) Structures that foster clinical competency: Educational training Patient care review sessions Application of evidence-based best practices during training Although simulation training has shown to be superior to using CD-ROM, the value of experiental learning with patients cannot be replaced. Schmalenberg Crit Care Nurse
12 Case 3 Male 64, no spouse SCI, tetraplegic, admitted to ICU TPPV for 18 hrs/day Wants to stay at home Organizational adaptations needed: Inform patient about possibilities, risks and responsibilities Search for a nursing home that may fit all demands Check for safety: alarms, electrical current, personnel Intake visit by care provider on ICU Supply of two ventilators which can be connected to central alarm system Wait for definitive acception by care provider
13 Organizational aspects and responsibilities Stieglitz Chron Respir Dis
14 Organizational aspects and responsibilities (2) No literature on staffing in residential or nursing homes Care provider is responsible for deployment and planning of adequate numbers of competent personnel Factors which may play a role in determing minimal staffing: Ventilator free time Hand function Ability to communicate Cognition and ability to manage Length and frequency of care Distance to patient Possibility to alert a caregiver
15 Organizational aspects and responsibilities (3) 1. HVS recommends patient on support and care based on risk profile and gears this with care provider 2. Care provider informs patient and HVS about care package and repsonse times (urgent and non-urgent) 3. Care provider discusses quality and quantity of care with patient in connecton with the risks and desires of that patient 4. Care provider determines if patient will be accepted given the care which is needed according to the HVS 5. HVS informs patient, care givers and/or care provider about health changes which are relevant for quantity and quality of care
16 Organizational aspects and responsibilities (4) Detection of worsening the of the LTMV patient by: Home visits by HMV-nurse and HMV-technician Home visits by HMV-physician Daily office hours 9-13h HMV-outpatients clinic Consultation by telephone 24/7 Company support 24 h/7 Assessments of HMV effectiveness at home
17 Organizational aspects and responsibilities (5) Technical issues while adapting to the worsening in LTMV: 1. Replacement of BiPAP-ventilators by more sophisticated ones 2. Ventilator with internal and external batteries 3. Ventilator with appropriate alarms (LP, LV, discon, power failure) 4. Ventilator which may be connnected to alarm system 5. Supplying an (identical) back-up ventilator >16 hrs/day 6. Wheelchair adaptation (construction, stability, power, safety) 7. A plan for power failure and calamities 8. Emergency support by medical equipment company 9. Routine equipment maintenance and quality control 10. Continued caregiver training and support
18 Organizational aspects and responsibilities (6) Other safety measures while adapting to the worsening: Written information for the patient explaining the implications of surgery, sedative procedures and uncontrolled oxygen therapy Preferably, performing procedures in hospital with experience in LTMV and LVR-techniques as well as access to high level monitoring or an ICU Supplying the patient with a medical letter for journeys and holidays Organizing multidisciplinary review and management including: Ø Cardiologist Ø Chest phyisician Ø Dietician Ø ENT-physician Ø Occupational therapist Ø Physiotherapist Ø Rehab physician Ø Social worker Ø Speech therapist
19 Organizational aspects and responsibilities (7) Guidelines may assist to organize (worsening of) LTMV in a safe manner National practice standard developed by care providers Operational since Criteria for professional performance Status: weighty recommendations
20 Case 4 Female 42, living at home with husband and child ALS, tetraplegic, only able to sit Uses morphine for severe back pain Swallowing problems with pulmonary infections Does not want TPPV (living will) instead of NPPV 24/24 Adaptations and actions needed: Home visit by physician and nurse of HVS to discuss end of life Determination of date, place and way of ending life Withdrawal of LTMV at home: GP, palliative team Instruction of GP: technique of withdrawal and symptom management Continuous availability for consultation
21 Palliative care and end-of-life issues In European respiratory intermediate care and high dependency units, an end-of-life decision is taken by the physician for 21.5% of patients admitted Neurologists in different countries reported that >20% ALS patients received TPPV on an emergency basis without an advanced directive Shared decision making (SDM) and advance care planning (ACP) are crucial in proactively determining what treatment and care decisions will be most appropriate for the patient over time, given his/ her values, beliefs and preferences. Nava Eur Respir J; Rabkin Amyotroph Lateral Scler Frontotemporal Degener
22 Palliative care and end-of-life issues (2) ACP should be sought from all patients at risk of LTMV, in particular those with rapidly progressive diseases ACP should result in document to be used when patient is unable to express preferences ACP-themes, which ought to be re-visited regularly, may include: Resuscitation Endotracheal intubation LTMV, including treatment end points Artificial nutrition Artificial hydration Treatment for infections Kidney failure Nava Eur Respir J
23 Palliative care and end-of-life issues (3) A good death : Free from avoidable distress and suffering In general accord with patient s and families wishes Reasonably consistent with clinical, cultural and ethical standards Strong communication between patient and clinicians and carers Failure of physicians to discuss disease progression in the context of LTMV, symptom management and initiate end-of-life discussions is a significant barrier to determining patient preferences Discussing sensitive end-of-life care issues: not too soon and not too late Successful palliative and end-of-life care requires a multi-disciplinary team ACI Respiratory Network consensus statement
24 Palliative care and end-of-life issues (4) Accepted in most countries Withholding Controversial in most countries Withdrawal Terminal sedation Rejected in most countries Physician-assisted suicide Euthanasia
25 Palliative care and end-of-life issues (5) Termination of LTMV: shared decision-making (SDM) Often well-considered and on time Sometimes denial: wellbeing-paradox (5% FTD) Correct information on course of disease and way of dying SDM = emotional process Termination of LTMV: implementation At home, hospice, nursing home Responsibility: GP or institutional physician Advisors: counsellor on palliative care, hospice-physician, HVS S.c. opioids (morfine), benzodiazepines (midazolam), oxygen
26 Palliative care and end-of-life issues (6) Withdrawal of LTMV: terminal weaning or disconnection The intention is not to facilitate or hasten death but to prevent further disproportionate burdens. Time until death depends on: Preferences patients and family Ventilator free time Continuous NPPV: minutes? Continuous TPPV: median time to die 28 min (5 min-18 hrs) No correlation between opiate dose and duration of survival off ventilator Especially as opiates and benzodiazepines do not seem to hasten death, there is no medical, ethical or legal justification for withholding doses necessary to control distressing symptoms Dreyer. J Palliat Med 2012; Campbell. AACN Adv Clin Care 2007
27 Conclusions Adapting to the worsening of the LTMV patient does involve: Strong communication between patient and clinicians and carers Shared decision-making and advanced care planning Role adaptation of patient, family and caregivers Pro-active attitude of professionals Technical and medical adjustments Organizational and professional capacity and compentency These requirements are best met with a practice guideline
28 Thank you for your attention
If patient is 24 hour dependent on NIV and decides to discontinue it, support and forward planning are essential
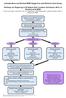 Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Palliative Care Competencies for Occupational Therapists
 Principles of Palliative Care Demonstrates an understanding of the philosophy of palliative care Demonstrates an understanding that a palliative approach to care starts early in the trajectory of a progressive
Principles of Palliative Care Demonstrates an understanding of the philosophy of palliative care Demonstrates an understanding that a palliative approach to care starts early in the trajectory of a progressive
End of Life Care in the ICU
 End of Life Care in the ICU C.M. Stafford, MD, FCCP Medical Director, Intensive Care Unit Chairman, Healthcare Ethics Committee Naval Medical Center San Diego The views expressed in this presentation are
End of Life Care in the ICU C.M. Stafford, MD, FCCP Medical Director, Intensive Care Unit Chairman, Healthcare Ethics Committee Naval Medical Center San Diego The views expressed in this presentation are
Unit 301 Understand how to provide support when working in end of life care Supporting information
 Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Communication with Surrogate Decision Makers. Shannon S. Carson, MD Associate Professor University of North Carolina
 Communication with Surrogate Decision Makers Shannon S. Carson, MD Associate Professor University of North Carolina Role of Communication with Families in the ICU Sharing information about illness and
Communication with Surrogate Decision Makers Shannon S. Carson, MD Associate Professor University of North Carolina Role of Communication with Families in the ICU Sharing information about illness and
Objectives. Integrating Palliative Care Principles into Critical Care Nursing
 1 Integrating Palliative Care Principles into Critical Care Nursing It s the Caring, Compassionate, Holistic, Patient and Family Centered, Better Communication, Keeping my patient comfortable amidst the
1 Integrating Palliative Care Principles into Critical Care Nursing It s the Caring, Compassionate, Holistic, Patient and Family Centered, Better Communication, Keeping my patient comfortable amidst the
Moral Conversations with ICU Patients and Families
 Moral Conversations with ICU Patients and Families Barb Supanich,RSM, MD,FAAHPM Medical Director, Palliative Care and Senior Services Holy Cross Hospital March 11, 2010 Learner Objectives Describe three
Moral Conversations with ICU Patients and Families Barb Supanich,RSM, MD,FAAHPM Medical Director, Palliative Care and Senior Services Holy Cross Hospital March 11, 2010 Learner Objectives Describe three
Criteria and Guidance for referral to Specialist Palliative Care Services
 Criteria and Guidance for referral to Specialist Palliative Care Services FEBRUARY 2007 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
Criteria and Guidance for referral to Specialist Palliative Care Services FEBRUARY 2007 Introduction This guidance is for health professionals caring for patients who may need referral to specialist palliative
TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee
 TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee Advance Directives Living Wills Power of Attorney The Values History: A Worksheet for Advanced Directives
TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee Advance Directives Living Wills Power of Attorney The Values History: A Worksheet for Advanced Directives
Caring for me Advanced Care Planning
 Caring for me Advanced Care Planning Supporting guidance for Healthcare Professionals and Administrative Staff This care plan is aimed as a guide to treatment and intended to aid the documentation of patient
Caring for me Advanced Care Planning Supporting guidance for Healthcare Professionals and Administrative Staff This care plan is aimed as a guide to treatment and intended to aid the documentation of patient
End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces.
 End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces. Terms Definitions End of Life Care To assist persons who
End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces. Terms Definitions End of Life Care To assist persons who
6: What care is available?
 6: What care is available? This section identifies and explains the types of care on offer at end of life and who is involved. The following information is an extracted section from our full guide End
6: What care is available? This section identifies and explains the types of care on offer at end of life and who is involved. The following information is an extracted section from our full guide End
The Principle of Double Effect in the Palliative Administration of Opioids. Kristin Abbott. University of Kansas School of Nursing
 The Principle of Double Effect in the Palliative Administration of Opioids Kristin Abbott University of Kansas School of Nursing 1 The Principle of Double Effect in the Palliative Administration of Opioids
The Principle of Double Effect in the Palliative Administration of Opioids Kristin Abbott University of Kansas School of Nursing 1 The Principle of Double Effect in the Palliative Administration of Opioids
NHS RightCare scenario: The variation between standard and optimal pathways
 NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 1: Summary slide pack January 2018 Sarah s story This is the story of Sarah s experience
NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 1: Summary slide pack January 2018 Sarah s story This is the story of Sarah s experience
Complex Decision-Making Around the Use of Extreme Technologies at the Edges of Medicine in the Pediatric ICU: The Case of Extracorporeal Life Support
 Complex Decision-Making Around the Use of Extreme Technologies at the Edges of Medicine in the Pediatric ICU: The Case of Extracorporeal Life Support Mithya Lewis-Newby, MD MPH Assistant Professor, Division
Complex Decision-Making Around the Use of Extreme Technologies at the Edges of Medicine in the Pediatric ICU: The Case of Extracorporeal Life Support Mithya Lewis-Newby, MD MPH Assistant Professor, Division
HealthStream Regulatory Script
 HealthStream Regulatory Script Advance Directives Version: [May 2006] Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney Lesson 5: Other Advance
HealthStream Regulatory Script Advance Directives Version: [May 2006] Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney Lesson 5: Other Advance
ADVANCE DIRECTIVE FOR HEALTH CARE
 ADVANCE DIRECTIVE FOR HEALTH CARE This document includes a list of definitions and the two types of Advance Directives (together called a Combined Directive). Some people choose to fill out only one portion.
ADVANCE DIRECTIVE FOR HEALTH CARE This document includes a list of definitions and the two types of Advance Directives (together called a Combined Directive). Some people choose to fill out only one portion.
Home Respiratory Care Norwegian model
 Home Respiratory Care Norwegian model Heidi Markussen Nurse, PhD candidate Tiina Andersen Physiotherapist, PhD candidate Norwegian Centre of Excellence for Home Mechanical Ventilation / Haukeland University
Home Respiratory Care Norwegian model Heidi Markussen Nurse, PhD candidate Tiina Andersen Physiotherapist, PhD candidate Norwegian Centre of Excellence for Home Mechanical Ventilation / Haukeland University
TAKING A STANCE ON PHYSICIAN AID IN DYING
 TAKING A STANCE ON PHYSICIAN AID IN DYING Constance Dahlin, MSN, ANP-BC, ACHPN, FPCN, FAAN Palliative Care Specialist Director of Professional Practice, HPNA Consultant, CAPC Palliative NP, NSMC Disclosures
TAKING A STANCE ON PHYSICIAN AID IN DYING Constance Dahlin, MSN, ANP-BC, ACHPN, FPCN, FAAN Palliative Care Specialist Director of Professional Practice, HPNA Consultant, CAPC Palliative NP, NSMC Disclosures
Long-term Ventilation Service Inventory Program. Final Summary Report July 31, 2008
 Long-term Ventilation Service Inventory Program Final Summary Report July 31, 2008 Table of Contents EXECUTIVE SUMMARY... I 1.0 INTRODUCTION...1 1.1 BACKGROUND...1 1.2 LTV ACTION PLAN...2 1.3 LTV INFORMATION
Long-term Ventilation Service Inventory Program Final Summary Report July 31, 2008 Table of Contents EXECUTIVE SUMMARY... I 1.0 INTRODUCTION...1 1.1 BACKGROUND...1 1.2 LTV ACTION PLAN...2 1.3 LTV INFORMATION
ABOUT THE ADVANCE DIRECTIVE FOR RECEIVING ORAL FOOD AND FLUIDS IN DEMENTIA. Introduction
 ABOUT THE ADVANCE DIRECTIVE FOR RECEIVING ORAL FOOD AND FLUIDS IN DEMENTIA Introduction There are two purposes to completing an Advance Directive for Receiving Oral Food and Fluids In Dementia. The first
ABOUT THE ADVANCE DIRECTIVE FOR RECEIVING ORAL FOOD AND FLUIDS IN DEMENTIA Introduction There are two purposes to completing an Advance Directive for Receiving Oral Food and Fluids In Dementia. The first
My Voice - My Choice
 My Voice - My Choice My Advance Directive Table of Contents Introduction... 2 Words You Need to Know... 3 Legal Document... 4 Helpful Information about your Advance Directive... 10 What makes your life
My Voice - My Choice My Advance Directive Table of Contents Introduction... 2 Words You Need to Know... 3 Legal Document... 4 Helpful Information about your Advance Directive... 10 What makes your life
MEDICAL ASSISTANCE IN DYING
 CMA POLICY MEDICAL ASSISTANCE IN DYING RATIONALE The legalization of medical assistance in dying (MAiD) raises a host of complex ethical and practical challenges that have implications for both policy
CMA POLICY MEDICAL ASSISTANCE IN DYING RATIONALE The legalization of medical assistance in dying (MAiD) raises a host of complex ethical and practical challenges that have implications for both policy
Challenging The 2015 PH Guidelines - comments from the Nurses. Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust
 Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
Challenging The 2015 PH Guidelines - comments from the Nurses Wendy Gin-Sing RN MSc Pulmonary Hypertension CNS Imperial College Healthcare NHS Trust Recommendations for pulmonary hypertension expert referral
DURABLE POWER OF ATTORNEY FOR HEALTH CARE (Rhode Island Version) You must be at least eighteen (18) years of age.
 MASSASOIT INTERNAL MEDICINE (401) 434-2704 massasoitmed.com DURABLE POWER OF ATTORNEY FOR HEALTH CARE (Rhode Island Version) THE DURABLE POWER OF ATTORNEY FOR HEALTH CARE DOCUMENT lets you appoint someone
MASSASOIT INTERNAL MEDICINE (401) 434-2704 massasoitmed.com DURABLE POWER OF ATTORNEY FOR HEALTH CARE (Rhode Island Version) THE DURABLE POWER OF ATTORNEY FOR HEALTH CARE DOCUMENT lets you appoint someone
We need to talk about Palliative Care. The Care Inspectorate
 We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
We need to talk about Palliative Care The Care Inspectorate Introduction The Care Inspectorate is the official body responsible for inspecting standards of care in Scotland. That means we regulate and
Palliative Care. Care for Adults With a Progressive, Life-Limiting Illness
 Palliative Care Care for Adults With a Progressive, Life-Limiting Illness Summary This quality standard addresses palliative care for people who are living with a serious, life-limiting illness, and for
Palliative Care Care for Adults With a Progressive, Life-Limiting Illness Summary This quality standard addresses palliative care for people who are living with a serious, life-limiting illness, and for
PATIENT RIGHTS, PRIVACY, AND PROTECTION
 REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
NHS RightCare scenario: The variation between standard and optimal pathways
 NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 2: Short summary slide pack January 2018 Sarah and the sub-optimal pathway Sarah, a 70-year-old
NHS RightCare scenario: The variation between standard and optimal pathways Sarah s story: Parkinson s Appendix 2: Short summary slide pack January 2018 Sarah and the sub-optimal pathway Sarah, a 70-year-old
Aid in Dying. Ethically Appropriate? History of Physician Assisted Suicide. Compatible with the professional obligation of the physician?
 Aid in Dying The process by which a capable, terminally ill person voluntarily self ingests prescribed medication to hasten death Distinguish from: Withdrawal or withholding of lifesustaining treatment
Aid in Dying The process by which a capable, terminally ill person voluntarily self ingests prescribed medication to hasten death Distinguish from: Withdrawal or withholding of lifesustaining treatment
TOWARDS A CONSENSUS-BUILDING APPROACH
 SAFEGUARDING THE UNCONSCIOUS PATIENTS OVERALL BENEFIT TOWARDS A CONSENSUS-BUILDING APPROACH Endcare An Erasmus+2015 Project 17 th /18 th March, 2016 Prof Emmanuel Agius Dean, Faculty of Theology, University
SAFEGUARDING THE UNCONSCIOUS PATIENTS OVERALL BENEFIT TOWARDS A CONSENSUS-BUILDING APPROACH Endcare An Erasmus+2015 Project 17 th /18 th March, 2016 Prof Emmanuel Agius Dean, Faculty of Theology, University
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Greater Manchester Neuro-Rehabilitation Services information for patients and carers
 THIS BOOKLET IS BEING TRIALLED Greater Manchester Neuro-Rehabilitation Services information for patients and carers Greater Manchester Neuro-Rehabilitation Services gmnrodn@srft.nhs.uk All Rights Reserved
THIS BOOKLET IS BEING TRIALLED Greater Manchester Neuro-Rehabilitation Services information for patients and carers Greater Manchester Neuro-Rehabilitation Services gmnrodn@srft.nhs.uk All Rights Reserved
ALLINA HOME & COMMUNITY SERVICES ALLINA HEALTH. Advance Care Planning. Discussion guide. Discussion Guide. Advance care planning
 ALLINA HOME & COMMUNITY SERVICES ALLINA HEALTH Advance Care Planning Discussion guide Discussion Guide Advance care planning Advance care planning Any of us could think of a time when we might be too sick
ALLINA HOME & COMMUNITY SERVICES ALLINA HEALTH Advance Care Planning Discussion guide Discussion Guide Advance care planning Advance care planning Any of us could think of a time when we might be too sick
HOSPICE IN MINNESOTA: A RURAL PROFILE
 JUNE 2003 HOSPICE IN MINNESOTA: A RURAL PROFILE Background Numerous national polls have found that when asked, most people would prefer to die in their own homes. 1 Contrary to these wishes, 75 percent
JUNE 2003 HOSPICE IN MINNESOTA: A RURAL PROFILE Background Numerous national polls have found that when asked, most people would prefer to die in their own homes. 1 Contrary to these wishes, 75 percent
1. Guidance notes. Social care (Adults, England) Knowledge set for end of life care. (revised edition, 2010) What are knowledge sets?
 Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Social care (Adults, England) Knowledge set for end of life care (revised edition, 2010) Part of the sector skills council Skills for Care and Development 1. Guidance notes What are knowledge sets? Knowledge
Policy Review Sheet. Review Date: 14/10/16 Policy Last Amended: 19/10/17. Next planned review in 12 months, or sooner as required.
 Category: Care Management Sub-category: Care Practice Page: 1 of 10 Policy Review Sheet Review Date: 14/10/16 Policy Last Amended: 19/10/17 Next planned review in 12 months, or sooner as required. Note:
Category: Care Management Sub-category: Care Practice Page: 1 of 10 Policy Review Sheet Review Date: 14/10/16 Policy Last Amended: 19/10/17 Next planned review in 12 months, or sooner as required. Note:
 NEW YORK STATE DEPARTMENT OF HEALTH Medical Orders for Life Sustaining Treatment (MOLST) THE PATIENT KEEPS THE ORIGINAL MOLST FORM DURING TRAVEL TO DIFFERENT CARE SETTINGS. THE PHYSICIAN KEEPS A COPY.
NEW YORK STATE DEPARTMENT OF HEALTH Medical Orders for Life Sustaining Treatment (MOLST) THE PATIENT KEEPS THE ORIGINAL MOLST FORM DURING TRAVEL TO DIFFERENT CARE SETTINGS. THE PHYSICIAN KEEPS A COPY.
Kuban Naidoo Department of Critical Care Chris Hani Baragwanath Academic Hospital SAMA Conference, Johannesburg, 2016
 Kuban Naidoo Department of Critical Care Chris Hani Baragwanath Academic Hospital SAMA Conference, Johannesburg, 2016 No financial conflict of interests I am a paediatrician Food for thought Intensive
Kuban Naidoo Department of Critical Care Chris Hani Baragwanath Academic Hospital SAMA Conference, Johannesburg, 2016 No financial conflict of interests I am a paediatrician Food for thought Intensive
Common Questions Asked by Patients Seeking Hospice Care
 Common Questions Asked by Patients Seeking Hospice Care C o m i n g t o t e r m s w i t h the fact that a loved one may need hospice care to manage his or her pain and get additional social and psychological
Common Questions Asked by Patients Seeking Hospice Care C o m i n g t o t e r m s w i t h the fact that a loved one may need hospice care to manage his or her pain and get additional social and psychological
European Recommendations for End-of-Life Care for Adults in Departments of Emergency Medicine
 European Recommendations for End-of-Life Care for Adults in Departments of Emergency Medicine September 2017 European Recommendations for End-of-Life Care in Departments of Emergency Medicine * Summary
European Recommendations for End-of-Life Care for Adults in Departments of Emergency Medicine September 2017 European Recommendations for End-of-Life Care in Departments of Emergency Medicine * Summary
Vermont Advance Directive for Health Care
 Vermont Advance Directive for Health Care Prepared by the Vermont Ethics Network Explanation and Instructions You have the right to give instructions about what types of health care you want or do not
Vermont Advance Directive for Health Care Prepared by the Vermont Ethics Network Explanation and Instructions You have the right to give instructions about what types of health care you want or do not
Advance Care Planning Conversations and Goals of Care Discussions: Understanding the Difference
 March 16, 2017 Advance Care Planning Conversations and Goals of Care Discussions: Understanding the Difference Jeff Myers MD, MSEd, CCFP(PC) Nadia Incardona MD, MHSc, CCFP(EM) WHY this is timely JAMA,
March 16, 2017 Advance Care Planning Conversations and Goals of Care Discussions: Understanding the Difference Jeff Myers MD, MSEd, CCFP(PC) Nadia Incardona MD, MHSc, CCFP(EM) WHY this is timely JAMA,
We would like to Welcome You to Martin Health System s Intensive Care Unit (ICU)
 We would like to Welcome You to Martin Health System s Intensive Care Unit (ICU) The ICU is a specialized unit for the very ill or those who need special care and observation. Enclosed is information that
We would like to Welcome You to Martin Health System s Intensive Care Unit (ICU) The ICU is a specialized unit for the very ill or those who need special care and observation. Enclosed is information that
MY CHOICES. Information on: Advance Care Directive Living Will POLST Orders
 MY CHOICES Information on: Advance Care Directive Living Will POLST Orders My Choices Adults have the right to accept or refuse medical care. As long as you can make health care decisions for yourself,
MY CHOICES Information on: Advance Care Directive Living Will POLST Orders My Choices Adults have the right to accept or refuse medical care. As long as you can make health care decisions for yourself,
Deciding About. Health Care A GUIDE FOR PATIENTS AND FAMILIES. New York State Department of Health
 Deciding About Health Care A GUIDE FOR PATIENTS AND FAMILIES New York State Department of Health 2 Introduction Who should read this guide? This guide is for New York State patients and for those who will
Deciding About Health Care A GUIDE FOR PATIENTS AND FAMILIES New York State Department of Health 2 Introduction Who should read this guide? This guide is for New York State patients and for those who will
What Are Advance Medical Directives?
 What Are Advance Medical Directives? UAMS would like you to know there are ways to let others know what decisions you would want to make about your medical treatments, even when you are unable to speak
What Are Advance Medical Directives? UAMS would like you to know there are ways to let others know what decisions you would want to make about your medical treatments, even when you are unable to speak
McKinley T34 Ambulatory syringe pump Used in the provision of adult palliative and end of life care
 Health Guidance McKinley T34 Ambulatory syringe pump Used in the provision of adult palliative and end of life care Publication Code: HCR-0214-083 Publication date: 26 February 2014 Page 1 of 7 Health
Health Guidance McKinley T34 Ambulatory syringe pump Used in the provision of adult palliative and end of life care Publication Code: HCR-0214-083 Publication date: 26 February 2014 Page 1 of 7 Health
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee
 Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
Woking & Sam Beare Hospices
 Woking & Sam Beare Hospices Introduction Woking Hospice was set up 20 years ago. From that early beginning, it has developed to become a local centre of excellence, as is the case with all Hospices in
Woking & Sam Beare Hospices Introduction Woking Hospice was set up 20 years ago. From that early beginning, it has developed to become a local centre of excellence, as is the case with all Hospices in
Overview of Presentation
 End-of-Life Issues: The Role of Hospice in The Nursing Home Susan C. Miller, Ph.D. Center for Gerontology & Health Care Research BROWN MEDICAL SCHOOL Overview of Presentation The rationale for the Medicare
End-of-Life Issues: The Role of Hospice in The Nursing Home Susan C. Miller, Ph.D. Center for Gerontology & Health Care Research BROWN MEDICAL SCHOOL Overview of Presentation The rationale for the Medicare
A guide for people considering their future health care
 A guide for people considering their future health care foreword Recently, Catholic Health Australia has been approached for guidance over the issue of advance care planning for patients and residents
A guide for people considering their future health care foreword Recently, Catholic Health Australia has been approached for guidance over the issue of advance care planning for patients and residents
Improving family experiences in ICU. Pamela Scott Senior Charge Nurse Forth Valley Royal Hospital ICU
 Improving family experiences in ICU Pamela Scott Senior Charge Nurse Forth Valley Royal Hospital ICU Family Burden in icu:- Incidence of anxiety symptoms range from 21% to 60.4% (median 40%) from ICU admission
Improving family experiences in ICU Pamela Scott Senior Charge Nurse Forth Valley Royal Hospital ICU Family Burden in icu:- Incidence of anxiety symptoms range from 21% to 60.4% (median 40%) from ICU admission
Symptoms and stress in family caregivers of ICU patients. Hanne Birgit Alfheim RN, CCN, PhD student Photo:
 Symptoms and stress in family caregivers of ICU patients Hanne Birgit Alfheim RN, CCN, PhD student Photo: oystein.horgmo@medisin.uio.no Why are the family caregivers so important for the patients? Family
Symptoms and stress in family caregivers of ICU patients Hanne Birgit Alfheim RN, CCN, PhD student Photo: oystein.horgmo@medisin.uio.no Why are the family caregivers so important for the patients? Family
Path to Transformation Concept Paper Comments and Recommendations. Palliative Care Community Partners (PCCP)
 Path to Transformation Concept Paper Comments and Recommendations Palliative Care Community Partners (PCCP) c/o Hospice Care of America, Inc., 3815 N Mulford Rd, Rockford, IL / (815)316-2697 As part of
Path to Transformation Concept Paper Comments and Recommendations Palliative Care Community Partners (PCCP) c/o Hospice Care of America, Inc., 3815 N Mulford Rd, Rockford, IL / (815)316-2697 As part of
Nursing Role in Renal Supportive Care.
 Nursing Role in Renal Supportive Care. How far have we come and where to from here? Renal Supportive Care Symposium 2015 Elizabeth Josland Renal Supportive Care CNC St George Hospital Content Definition
Nursing Role in Renal Supportive Care. How far have we come and where to from here? Renal Supportive Care Symposium 2015 Elizabeth Josland Renal Supportive Care CNC St George Hospital Content Definition
Ethical Issues: advance directives, nutrition and life support
 Ethical Issues: advance directives, nutrition and life support December 12, 2013 2013 LegalHealth Objectives Discuss parameters of consent for medical treatment and legal issues that arise Provide overview
Ethical Issues: advance directives, nutrition and life support December 12, 2013 2013 LegalHealth Objectives Discuss parameters of consent for medical treatment and legal issues that arise Provide overview
Colorado CPR Directives. Colorado Department of Public Health and Environment Emergency Medical and Trauma Services Section
 Colorado CPR Directives Colorado Department of Public Health and Environment Emergency Medical and Trauma Services Section Course Objectives Upon completion of this class, you should be able to: Identify
Colorado CPR Directives Colorado Department of Public Health and Environment Emergency Medical and Trauma Services Section Course Objectives Upon completion of this class, you should be able to: Identify
L e g a l I s s u e s i n H e a l t h C a r e
 Page 1 L e g a l I s s u e s i n H e a l t h C a r e Tutorial #6 January 2008 Introduction Patients have the right to accept or refuse health care treatment. For a patient to exercise that right, he or
Page 1 L e g a l I s s u e s i n H e a l t h C a r e Tutorial #6 January 2008 Introduction Patients have the right to accept or refuse health care treatment. For a patient to exercise that right, he or
(f) Department means the New Hampshire department of health and human services.
 Adopted Rule 6/16/10. Effective: 7/1/10 1 Adopt He-W 544.01 544.16, cited and to read as follows: CHAPTER He-W 500 MEDICAL ASSISTANCE PART He-W 544 HOSPICE SERVICES He-W 544.01 Definitions. (a) Agent means
Adopted Rule 6/16/10. Effective: 7/1/10 1 Adopt He-W 544.01 544.16, cited and to read as follows: CHAPTER He-W 500 MEDICAL ASSISTANCE PART He-W 544 HOSPICE SERVICES He-W 544.01 Definitions. (a) Agent means
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
National Standards Assessment Program. Quality Report
 National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
National Standards Assessment Program Quality Report - March 2016 1 His Excellency General the Honourable Sir Peter Cosgrove AK MC (Retd), Governor-General of the Commonwealth of Australia, Patron Palliative
Palliative and Hospice Care In the United States Jean Root, DO
 Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
Palliative and Hospice Care In the United States Jean Root, DO Hello. My name is Jean Root. I am an Osteopathic Physician who specializes in Geriatrics, or care of the elderly. I teach and practice Geriatric
DNACPR. Maire O Riordan 14 th January 2015
 DNACPR Maire O Riordan 14 th January 2015 Objectives NHS Scotland DNACPR policy Decision making framework and the forms DNACPR within ACP context Communicationwith patients, relatives and colleagues Background
DNACPR Maire O Riordan 14 th January 2015 Objectives NHS Scotland DNACPR policy Decision making framework and the forms DNACPR within ACP context Communicationwith patients, relatives and colleagues Background
Hospice Residences. in Fraser Health
 Hospice Residences in Fraser Health Options for End of Life Care As a person s life draws to a close, the time comes when the focus changes from working towards a cure to loving care and comfort. Paying
Hospice Residences in Fraser Health Options for End of Life Care As a person s life draws to a close, the time comes when the focus changes from working towards a cure to loving care and comfort. Paying
Continuing Healthcare - should the NHS be paying for your care?
 Continuing Healthcare - should the NHS be paying for your care? This factsheet explains when it is the duty of the NHS to pay for your social care. It covers what NHS Continuing Healthcare is, who is eligible,
Continuing Healthcare - should the NHS be paying for your care? This factsheet explains when it is the duty of the NHS to pay for your social care. It covers what NHS Continuing Healthcare is, who is eligible,
Withdrawal of active treatment in intensive care: what is stopped comparison between belief and practice
 Withdrawal of active treatment in intensive care: what is stopped comparison between belief and practice Alex J Psirides and Shawn Sturland Most deaths in intensive care units in the Western world are
Withdrawal of active treatment in intensive care: what is stopped comparison between belief and practice Alex J Psirides and Shawn Sturland Most deaths in intensive care units in the Western world are
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool
 Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
End of Life PSP Module. Case Study: Mr. James Lee
 Case Study: Mr. James Lee Mr. James Lee is a 74 yr old retired electrician. He is married to Mary with two children in their 30 s. They have been in Canada for 35 years and are fluent in English and Cantonese.
Case Study: Mr. James Lee Mr. James Lee is a 74 yr old retired electrician. He is married to Mary with two children in their 30 s. They have been in Canada for 35 years and are fluent in English and Cantonese.
Exploring Your Options for Palliative Care
 Exploring Your Options for Palliative Care A guide for patients and families Inside this booklet Question Page What is palliative care? 1 When should I receive palliative care? 2 Where can I receive palliative
Exploring Your Options for Palliative Care A guide for patients and families Inside this booklet Question Page What is palliative care? 1 When should I receive palliative care? 2 Where can I receive palliative
PRIORITIES FOR CARE OF THE DYING PERSON
 PRIORITIES FOR CARE OF THE DYING PERSON Core and other useful sessions to support education and training across health and social care Fig.1 The 5 Priorities for Care of the Dying Person INTRODUCTION One
PRIORITIES FOR CARE OF THE DYING PERSON Core and other useful sessions to support education and training across health and social care Fig.1 The 5 Priorities for Care of the Dying Person INTRODUCTION One
PSYCHOSOCIAL ASPECTS OF PALLIATIVE CARE IN MENTAL HEALTH SETTINGS. Dawn Chaitram BSW, RSW, MA Psychosocial Specialist
 PSYCHOSOCIAL ASPECTS OF PALLIATIVE CARE IN MENTAL HEALTH SETTINGS Dawn Chaitram BSW, RSW, MA Psychosocial Specialist WRHA Palliative Care Program April 19, 2017 OUTLINE Vulnerability and Compassion Addressing
PSYCHOSOCIAL ASPECTS OF PALLIATIVE CARE IN MENTAL HEALTH SETTINGS Dawn Chaitram BSW, RSW, MA Psychosocial Specialist WRHA Palliative Care Program April 19, 2017 OUTLINE Vulnerability and Compassion Addressing
MAKING YOUR WISHES KNOWN: Advance Care Planning Guide
 MAKING YOUR WISHES KNOWN: Advance Care Planning Guide ADVANCE CARE PLANNING The process of learning about the type of medical decisions that may need to be made, considering those decisions ahead of time
MAKING YOUR WISHES KNOWN: Advance Care Planning Guide ADVANCE CARE PLANNING The process of learning about the type of medical decisions that may need to be made, considering those decisions ahead of time
The Palliative Care Program MISSION STATEMENT
 The Palliative Care Program MISSION STATEMENT believes in providing compassionate, comprehensive, multidisciplinary care to residents living with a life threatening illness and their families to relieve
The Palliative Care Program MISSION STATEMENT believes in providing compassionate, comprehensive, multidisciplinary care to residents living with a life threatening illness and their families to relieve
JOB DESCRIPTION & PERSON SPECIFICATION JOB DESCRIPTION. Highly Specialist Psychological Therapist
 JOB DESCRIPTION & PERSON SPECIFICATION JOB DESCRIPTION JOB TITLE: GRADE: Highly Specialist Psychological Therapist Band 7 and 8a HOURS OF WORK: 37.5 RESPONSIBLE TO: (Line manager) ACCOUNTABLE TO: Clinical
JOB DESCRIPTION & PERSON SPECIFICATION JOB DESCRIPTION JOB TITLE: GRADE: Highly Specialist Psychological Therapist Band 7 and 8a HOURS OF WORK: 37.5 RESPONSIBLE TO: (Line manager) ACCOUNTABLE TO: Clinical
What You Need To Know About Palliative Care
 www.hrh.ca Medical Program What You Need To Know About Palliative Care What s Inside: Who are your team members?... 2 Care Needs of Your Loved One: Information for the Family... 4 Options for Discharge...
www.hrh.ca Medical Program What You Need To Know About Palliative Care What s Inside: Who are your team members?... 2 Care Needs of Your Loved One: Information for the Family... 4 Options for Discharge...
2
 1 2 3 4 Designation of Health Care Surrogate I, (please print) want Phone Address to be my Health Care Surrogate and make health care decisions for me as indicated by my initials below: Effective only
1 2 3 4 Designation of Health Care Surrogate I, (please print) want Phone Address to be my Health Care Surrogate and make health care decisions for me as indicated by my initials below: Effective only
Equality Impact. Version Control Sheet. Version: V1.0. Date Ratified August 2014 Name of author. Date Published on Intranet Review Date August 2017
 Clinical Guidance for the End-of-Life Care of Patients who are Receiving n-invasive Ventilation for Respiratory Failure Associated with Motor Neurone Disease Version: V1.0 Ratifying Committee: Schedule/Unscheduled
Clinical Guidance for the End-of-Life Care of Patients who are Receiving n-invasive Ventilation for Respiratory Failure Associated with Motor Neurone Disease Version: V1.0 Ratifying Committee: Schedule/Unscheduled
Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For. Patients And Their Families
 Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For Patients And Their Families The goal of this pamphlet is to help you participate in the decision about whether or not to have cardio-pulmonary resuscitation
Cardio-Pulmonary Resuscitation (CPR): A Decision Aid For Patients And Their Families The goal of this pamphlet is to help you participate in the decision about whether or not to have cardio-pulmonary resuscitation
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert
 For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
Course Materials & Disclosure
 E L N E C End-of-Life Nursing Education Consortium Module 7 Loss, Grief, & Bereavement Course Materials & Disclosure Course materials including handout(s) and conflict of interest disclosure statement
E L N E C End-of-Life Nursing Education Consortium Module 7 Loss, Grief, & Bereavement Course Materials & Disclosure Course materials including handout(s) and conflict of interest disclosure statement
MY ADVANCE CARE PLANNING GUIDE
 MY DVNCE CRE PLNNING GUIDE Let s TLK! Tell us your values and beliefs about your healthcare. Take time to have the conversation with your physician and your family. lways be open and honest. Leave no doubt
MY DVNCE CRE PLNNING GUIDE Let s TLK! Tell us your values and beliefs about your healthcare. Take time to have the conversation with your physician and your family. lways be open and honest. Leave no doubt
SDMs and Health Decision Making
 1 SDMs and Health Decision Making Judith Wahl Wahl Elder Law wahlelderlaw@gmail.com 416-209-3407 2 Disclaimer This presentation and any material provided for this presentation is not legal advice but is
1 SDMs and Health Decision Making Judith Wahl Wahl Elder Law wahlelderlaw@gmail.com 416-209-3407 2 Disclaimer This presentation and any material provided for this presentation is not legal advice but is
A Guide to Compassionate Decisions
 A Guide to Compassionate Decisions At Companion Hospice We Are Dedicated to Enhancing the Quality of Life Enhancing the Quality of Life A Guide to Compassionate Decisions Throughout most of our lives,
A Guide to Compassionate Decisions At Companion Hospice We Are Dedicated to Enhancing the Quality of Life Enhancing the Quality of Life A Guide to Compassionate Decisions Throughout most of our lives,
Scottish Palliative Care Guidelines Rapid Transfer Home in the Last Days of Life
 Rapid Transfer Home in the Last Days of Life Management Follow five steps below to: facilitate a peaceful death in the patient s preferred place facilitate seamless transfer from hospital or hospice to
Rapid Transfer Home in the Last Days of Life Management Follow five steps below to: facilitate a peaceful death in the patient s preferred place facilitate seamless transfer from hospital or hospice to
AARC Clinical Practice Guideline
 AARC Clinical Practice Guideline Discharge Planning for the Respiratory Care Patient DPRP 1.0 PROCEDURE: Development and implementation of a comprehensive plan for the safe discharge of the respiratory
AARC Clinical Practice Guideline Discharge Planning for the Respiratory Care Patient DPRP 1.0 PROCEDURE: Development and implementation of a comprehensive plan for the safe discharge of the respiratory
One Chance to Get it Right:
 One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
One Chance to Get it Right: Implementing the new priorities of Care for the Dying Person Dr Susan Salt, Medical Director Trinity Hospice, Blackpool Outline of the talk Brief look at what led to this point..
The POLST Conversation POLST Script
 The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes realistic
The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes realistic
Hospice Care for the Person with Cancer
 Hospice Care for the Person with Cancer Hospice is a special type of care designed to provide comfort, support and dignity to patients with a lifelimiting or terminal illness. For hospice purposes, a life-limiting
Hospice Care for the Person with Cancer Hospice is a special type of care designed to provide comfort, support and dignity to patients with a lifelimiting or terminal illness. For hospice purposes, a life-limiting
ADVANCE DIRECTIVE PACKET Question and Answer Section
 ADVANCE DIRECTIVE PACKET Question and Answer Section Please review the following facts regarding what an Advance Directive is, as well as your right as an adult to create one. If you decide to complete
ADVANCE DIRECTIVE PACKET Question and Answer Section Please review the following facts regarding what an Advance Directive is, as well as your right as an adult to create one. If you decide to complete
Advance Health Care Planning: Making Your Wishes Known. MC rev0813
 Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Many who are interested in medicine, palliative care and hospice and bioethics have been
 NEW "DNR" RULES WENT INTO EFFECT MAY 20, 1999 Many who are interested in medicine, palliative care and hospice and bioethics have been carefully following the progress of the legislation on "portable DNR"
NEW "DNR" RULES WENT INTO EFFECT MAY 20, 1999 Many who are interested in medicine, palliative care and hospice and bioethics have been carefully following the progress of the legislation on "portable DNR"
Advance Directives The Missing Conversation Why Our Patients Children Are Left Holding The Bag. End of Life Planning Barriers 10/7/2014
 Advance Directives The Missing Conversation Why Our Patients Children Are Left Holding The Bag SC Chapter American College of Physicians October 29, 2014 Sewell I. Kahn, MD FACP End of Life Planning Barriers
Advance Directives The Missing Conversation Why Our Patients Children Are Left Holding The Bag SC Chapter American College of Physicians October 29, 2014 Sewell I. Kahn, MD FACP End of Life Planning Barriers
Countess Mountbatten House. Information for patients, families and carers
 Countess Mountbatten House Information for patients, families and carers Contents About the service 3 The inpatient unit 5 The Hazel Centre 7 The chaplaincy service 9 The hospital palliative care team
Countess Mountbatten House Information for patients, families and carers Contents About the service 3 The inpatient unit 5 The Hazel Centre 7 The chaplaincy service 9 The hospital palliative care team
Supporting people who need Palliative and End of Life Care in the Community. Giving people a choice
 Supporting people who need Palliative and End of Life Care in the Community Giving people a choice Introduction People who are terminally ill or at the end of their life need excellent nursing and medical
Supporting people who need Palliative and End of Life Care in the Community Giving people a choice Introduction People who are terminally ill or at the end of their life need excellent nursing and medical
9: Advance care planning and advance decisions
 9: Advance care planning and advance decisions This section explains how advance care planning and Advance Decisions to Refuse Treatment (ADRT) can support your future care. The following information is
9: Advance care planning and advance decisions This section explains how advance care planning and Advance Decisions to Refuse Treatment (ADRT) can support your future care. The following information is
ADVANCE CARE PLANNING DOCUMENTS
 ADVANCE CARE PLANNING DOCUMENTS Legal Documents to Assure Your Future Health Care Choices Distributed as a Public Service by THE NEVADA CENTER FOR ETHICS & HEALTH POLICY University of Nevada, Reno Revised
ADVANCE CARE PLANNING DOCUMENTS Legal Documents to Assure Your Future Health Care Choices Distributed as a Public Service by THE NEVADA CENTER FOR ETHICS & HEALTH POLICY University of Nevada, Reno Revised
Commentary on the guidance
 Annex A Withholding and Withdrawing Life-Prolonging Treatments: Good Practice in Decision-Making Commentary on the guidance Introduction (paragraphs 1-5) 1. This section explains the professional and public
Annex A Withholding and Withdrawing Life-Prolonging Treatments: Good Practice in Decision-Making Commentary on the guidance Introduction (paragraphs 1-5) 1. This section explains the professional and public
YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE
 YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE Communicating Your Health Care Choices In 1990, Congress passed the Patient Self-Determination Introduction Act. It requires
YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE Communicating Your Health Care Choices In 1990, Congress passed the Patient Self-Determination Introduction Act. It requires
Physician s Guide to OHIP billing for Palliative Care Services
 Physician s Guide to OHIP billing for Palliative Care Services Based on the May 1, 2014 OHIP Schedule of Benefits Dedicated to Doctors. Committed to Patients. Guide to OHIP Billing for Palliative Care
Physician s Guide to OHIP billing for Palliative Care Services Based on the May 1, 2014 OHIP Schedule of Benefits Dedicated to Doctors. Committed to Patients. Guide to OHIP Billing for Palliative Care
