POLICIES & PROCEDURES ENDOTRACHEAL TUBE (ADULT, PEDIATRIC) ASSISTING WITH INTUBATION. I.D. Number: Authorization
|
|
|
- Stanley Jefferson
- 6 years ago
- Views:
Transcription
1 POLICIES & PROCEDURES Title: ENDOTRACHEAL TUBE (ADULT, PEDIATRIC) ASSISTING WITH INTUBATION I.D. Number: 1039 Authorization [X] SHR Nursing Practice Committee Source: Nursing/Respiratory Therapy Date Revised:October,2017 Date Effective: March 2004 Scope: SHR Acute Care Any PRINTED version of this document is only accurate up to the date of printing 1-Dec-17. Saskatoon Health Region (SHR) cannot guarantee the currency or accuracy of any printed policy. Always refer to the Policies and Procedures site for the most current versions of documents in effect. SHR accepts no responsibility for use of this material by any person or organization not associated with SHR. No part of this document may be reproduced in any form for publication without permission of SHR. Definition Health Care Professional (HCP) - Physician-Assistant, RN, RN (NP), LPN working in the OR with Perioperative Advanced Certification, RRT, student RT under direct supervision of RRT may assist with intubation. Two personnel must be present to perform intubation one qualified in intubation and one to assist 1. PURPOSE 1.1 Endotracheal intubation usually requires two qualified Health Care Professionals (HCP), one to insert the endotracheal tube (ETT) into the trachea and another person to assist. This procedure outlines the responsibilities of the assistant who may prepare and monitor the patient, assemble the equipment required under direction of practitioner intubating, act as an extra set of hands (especially when the vocal cords are being visualized and immediately following tube placement), and ensure patient safety. A third HCP may be needed for medication administration or other tasks as directed. 2. POLICY 2.1 Who may assist: Health Care Professional 2.2 Physician order required: Yes 2.3 Special considerations 3. PROCEDURE At least two personnel must be present to perform intubation one qualified in intubation and one to assist Ensure all equipment is in working order before beginning procedure 3.1 Supplies Airway Management Kit ( SKU # ) / Tray (SKU # ) or Pediatric Intubation Tray (SKU # ) Page 1 of 6
2 Suction equipment including Yankauer tip and straight suction catheter of appropriate size Laryngoscope handles curved & straight blades of appropriate sizes. Glidescope may also be requested. 12 ml syringe Appropriate size and style of endotracheal tube (ETT): cuffed for adults and cuffed or un-cuffed for children. NOTE: for Pediatrics, assemble ETT 0.5mm larger and smaller than size anticipated. ETT tapes, ties, or commercially available holder Scissors McGill forceps Stylet adult or child depending on size of ETT Xylocaine spray and nozzle (optional) Water-soluble lubricating jelly (optional) Bag-valve-mask (BVM) device and appropriate size mask and PEEP valve as appropriate. NOTE: Neonatal BVM do not have a PEEP valve Stethoscope Personal Protective Equipment: mask with attached visor and sterile/non-sterile gloves as required by the situation ((based on a point-of-care risk assessment, the use of other appropriate PPE such as a gown may be considered). Direct ECG rhythm, SpO2, and ETCO2 monitoring Refer to Cardiac( ECG) monitoring ( Adults and Pediatrics) #1142 Medications (as ordered) Vascular access supplies if medications being used Oropharyngeal airway Cuff pressure monitor for cuffed ETT ( if available) Gastric tube of appropriate size for decompression, if necessary 3.2 Perform hand hygiene and don appropriate PPE. 3.3 Ensure that equipment is in working order while maintaining cleanliness of equipment Test endotracheal cuff for proper inflation with appropriate syringe Test for proper function of laryngoscope Test suction equipment 3.4 Explain procedure and risks to patient / family and obtain consent as appropriate for situation. 3.5 Obtain patient history and NPO status as appropriate. 3.6 Prepare for ETT insertion: Ensure direct ECG rhythm and SpO2 monitoring is in place and patient has patent IV access. In event of cardiorespiratory arrest, IV/IO access will be addressed as soon as possible Perform hand hygiene. Prepare medication as ordered Position patient so HCP that is intubating has access to the head of the patient. Remove headboard from bed or lower crib rail and position the bed/crib away from the wall to allow access for 2 HCPs and assembled equipment. The assistant should Page 2 of 6
3 be positioned ideally to the right of the person inserting the ETT and have ready access to appropriate intubating supplies Place patient supine unless otherwise directed or contraindicated Perform hand hygiene. Don clean gloves. Remove any false teeth, bridges or foreign objects, such as body piercings, from the mouth and perform hand hygiene Slightly extend head and flex neck ( sniff position ), unless contraindicated (e.g. C- spine precaution). To assist in maintaining sniff position, a small roll under shoulders in pediatrics or under the head in adults, maybe useful. NOTE: if the sniff position is contraindicated, HCP assisting will provide jaw thrust maneuver. 3.6 Assist with procedure Perform hand hygiene. Hyper-oxygenate as directed by supplying 100% oxygen (2 3 minutes for adults and 3 5 minutes for pediatrics) if spontaneously breathing. If not spontaneously breathing, provide 3 4 hyperoxygenation, hyperinflation breaths using BVM device and oral airway (if necessary) or head tilt/jaw thrust maneuvers to optimize SpO2 as much as possible Pre-medicate patient as directed Suction oropharynx as requested by HCP intubating. After suctioning is complete, remove gloves and perform hand hygiene and don a new pair of clean gloves Apply cricoid pressure as requested by HCP intubating. This is done by applying and maintaining firm pressure downward on cricoid cartilage / thyroid to assist in visualizing the vocal cords. Do not remove cricoid pressure until directed to do so by HCP intubating or the ETT placement is confirmed in trachea and cuff is inflated (if cuffed ETT utilized). Release of pressure prematurely may result in emesis / aspiration Intubation attempts Adults: should be limited to 30 seconds. Pediatrics: should be limited to 20 seconds depending on patient s stability. The patient is manually ventilated with BVM device using 100% oxygen between attempts Monitor SpO2 and/or ECG for deterioration during attempts. Notify HCP intubating if SpO2 drops to below 90% or ordered levels, heart rate is below age appropriate norm or rhythm changes Once the ETT has been inserted into the trachea, it will be held in place by the HCP who intubated. The assistant, upon direction from the HCP intubating, will then a take firm hold of the proximal part of the ETT and remove the stylet, or other insertion device used (i.e. Bougies) being careful not to move the tube itself. The assistant will then remove gloves, perform hand hygiene and don a new pair of gloves. NOTE: if patient is biting on the ETT, a bite block may be inserted The ETCO2 adapter is placed onto the ETT, positive pressure breaths are provided, and the cuff is quickly inflated using the minimal occlusive volume technique by Page 3 of 6
4 slowly injecting air into the cuff and listening with a stethoscope over the trachea until no air leak can be heard. 3.7 Immediately assesses ETT placement following intubation ETCO2 device (Capnography) with CO2 levels and waveform, or by color change on color-metric device Person inserting ETT reports sees the tube pass through vocal cords Auscultate over right and left lung apices and epigastrium. Breath sounds should be heard over both lungs and no sounds from epigastrium. ADULTS: Bilateral, equal breath sounds should be heard. If air is heard entering stomach and there is no ETCO2 confirmation and or breath sounds in peripheral lung fields, the ETT should be removed immediately and BVM ventilation provided until patient is stabilized prior to next intubation attempt. PEDIATRICS: Auscultate peripheral lung fields (under axilla) for equal breath sounds. If air is heard entering stomach and there is no ETCO2 confirmation and or breath sounds in peripheral lung fields, the ETT should be removed immediately and BVM ventilation provided until patient is stabilized prior to next intubation attempt. NOTE: air entry to one lung only may be indicative of ETT placement into a main stem bronchus. Notify intubating HCP for readjustment of ETT depth and reassess Observe for clinical improvement (heart rate, SpO2, color). Inspect for bilateral, symmetrical chest expansion. NOTE: observation for condensation on the inside of the tube during exhalation is not a primary confirmation technique. 3.8 Firmly secure ETT with tape, twill ties or commercially available ETT securement device. See Policy: Endotracheal Tubes Care Of #1176. Secure across, unless contraindicated. Once ETT is secured, auscultate lung fields to ensure bilateral air entry. Remove gloves and perform hand hygiene. 3.9 Connect patient to humidified oxygen source or mechanical ventilator. Pediatrics; continue to manually ventilate until connected to mechanical ventilator Perform hand hygiene and remove PPE Ensure that chest x-ray is ordered and obtained (optional in PACU and OR for short-term intubations). Adults: ETT tip should lie at least 2 cm above carina. Pediatrics: ETT tip should be 1-2 cm above carina. NOTE: May not be done in a rural setting where portable chest x-ray may not be an option. If placement has been verified clinically and patient stability has improved, then transfer maybe undertaken Document on appropriate record: Name of HCP performing intubation. Page 4 of 6
5 4. REFERENCES ETT size, type, level of insertion in cm (to gums / teeth in adults, and upper lip in pediatrics), route of insertion, person performing intubation, volume or pressure used to inflate ETT cuff, presence of air leak Methods used to confirm tube placement, including capnography reading, waveform or color changes Patient's tolerance before, during, and after procedure including vital signs (heart rate, BP, SpO2, ETCO2) Assess patient s respiratory status (i.e. rate, rhythm, lung sounds, need for suctioning / presence of secretions,) If CXR done On medication record, medications used, including double signatures for checking high alert medications. SHR Policy; High Alert Medications Identification, Double Check and Labeling # Oxygen percentage and ventilator parameters if patient mechanically ventilated following intubation on appropriate record If patient was a difficult intubation: NOTE: An Assessment of Patient Airway Alert (form # ) should be completed by the HCP that performed the intubation and placed in the patient s chart. Post an Airway Alert sign (form # ) at head of bed. Place an Airway Alert sticker (form # /06) on front of patient s chart. Goodrich, C., (2017). Endotracheal Intubation (Assist) in AACN Procedure Manual for High Acuity, Progressive, and Critical Care - E-Book 7 th ed. Seventh edition. Saunders: St. Louis. Pg Grzeskowiak, M. (2015). Protecting the Airway, Protecting the Patient. RT: The Journal For Respiratory Care Practitioners. 28(3): ect=true&db=rzh&an= &site=ehost-live Hazinski, M.F. (2013). Bioinstrumentation: Prinicples and Techniques. Nursing Care of the Critically Ill Child, (3 rd ed). St. Louis, MI, Elsevier, Krug, L., Machan, M., Villalba, J. (2014). Securing the Endotracheal Tube with Adhesive Tape: An Integrative Literature Review. AANA Journal. 82(6): ect=true&db=rzh&an= &site=ehost-live Mayo, P.H., Hegde, A., Eisen, L.A., Kory, P., Doelken, P. (2011) A Program to Improve the Quality of Emergency Endotracheal Intubation. Journal of Intensive Care Medicine. 26(1):50-6. Morton, P. G., Fontaine, D. K. (2013). Endotracheal Tubes in Critical Care Nursing. 10 th ed. Philadelphia: Wolters Kluwer. Pg Miller, K. A., Kimia, A., Monuteaux M. C. & Magler, J. (2016). Factors associated with misplaced endotracheal tubes during itnubation in pediatric patients. Journal of Emergency Medicine, 51(1), Pediatric Advanced Life Support: Provider Manual. (2016). Heart and Stroke Foundation Page 5 of 6
6 Perry, A. G., Potter, P.A., Ostendorf, W. R. (2014).Care of Endotracheal Tubes. 8 th ed. St. Louis: Elsevier. Pg Securing Endotracheal Tube in Neonatal / Pediatric Areas. UTMB Respiratory Care Services. Effective 10/30/14. Smith S. (2016). Ask the Experts. Best Method for Securing an Endotracheal Tube. Critical Care Nurse. 36(2): ect=true&db=rzh&an= &site=ehost-live Urden, L. D., Stacy, K. M., Lough, M. E. (2014). Endotracheal Tubes in Critical Care Nursing; Diagnosis and Management. 7 th ed. St. Louis: Elsevier. pg Vollman, K., Sole, M. L., Quinn, B (2017). Endotracheal Tube Care and Oral Care Practices For Ventilated And Non-Ventilated Patients. in AACN Procedure Manual for High Acuity, Progressive, and Critical Care - E-Book 7 th ed. Seventh edition. Saunders: St. Louis. Pg Page 6 of 6
POLICIES & PROCEDURES. RNSP: RN Procedure. I.D. Number: 1176
 POLICIES & PROCEDURES Title: ENDOTRACHEAL TUBES (ADULT, PEDIATRIC) SECURING, CARE OF RNSP: RN Procedure I.D. Number: 1176 Authorization [X] SHR Nursing Practice Committee Source: Nursing /Respiratory Therapy
POLICIES & PROCEDURES Title: ENDOTRACHEAL TUBES (ADULT, PEDIATRIC) SECURING, CARE OF RNSP: RN Procedure I.D. Number: 1176 Authorization [X] SHR Nursing Practice Committee Source: Nursing /Respiratory Therapy
Policies & Procedures
 Policies & Procedures Title: ENTERAL FEEDING TUBE WITH A STYLET: ASSISTING WITH INSERTION OF: CARE OF, REMOVAL OF Authorization [X] SHR Nursing Practice Committee ID Number: 1109 Source: Nursing Date Reaffirmed:
Policies & Procedures Title: ENTERAL FEEDING TUBE WITH A STYLET: ASSISTING WITH INSERTION OF: CARE OF, REMOVAL OF Authorization [X] SHR Nursing Practice Committee ID Number: 1109 Source: Nursing Date Reaffirmed:
Curriculum For The LMA Supreme
 Curriculum For The LMA Supreme Course Description This course is designed to provide instruction in a procedure for the use of the LMA Supreme by the EMT-Intermediate `99 and Paramedic. Prerequisites 1.
Curriculum For The LMA Supreme Course Description This course is designed to provide instruction in a procedure for the use of the LMA Supreme by the EMT-Intermediate `99 and Paramedic. Prerequisites 1.
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Effective: September, 2011 Revised: August 17, 2016 TRACHEOSTOMY TUBE REPLACEMENT
 TRACHEOSTOMY TUBE REPLACEMENT Purpose: Emergency tracheostomy tube replacement occurs when the tube becomes blocked, dislodged or has been unintentionally removed. Additional Authority: Nevada Revised
TRACHEOSTOMY TUBE REPLACEMENT Purpose: Emergency tracheostomy tube replacement occurs when the tube becomes blocked, dislodged or has been unintentionally removed. Additional Authority: Nevada Revised
A AIRWAY Open the Airway B BREATHING Deliver two (2) Breaths. Code Blue Policy. Indications for Calling A Code Blue
 Code Blue Policy Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in a patient s status (e.g. unresponsiveness, absence of blood pressure, status epilepticus)
Code Blue Policy Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in a patient s status (e.g. unresponsiveness, absence of blood pressure, status epilepticus)
VANDERBILT UNIVERSITY MEDICAL CENTER MULTIDISCIPLINARY SURGICAL CRITICAL CARE PERCUTANEOUS TRACHEOSTOMY MANAGEMENT GUIDELINE
 PERCUTANEOUS TRACHEOSTOMY MANAGEMENT GUIDELINE I. PURPOSE: - To standardize the steps and processes involved in the performance of bedside percutaneous tracheostomies in the SICU. - This document should
PERCUTANEOUS TRACHEOSTOMY MANAGEMENT GUIDELINE I. PURPOSE: - To standardize the steps and processes involved in the performance of bedside percutaneous tracheostomies in the SICU. - This document should
Effective: Revised: April 15, 2016 SUCTIONING, MODIFIED STERILE TRACHEAL
 SUCTIONING, MODIFIED STERILE TRACHEAL Purpose: Tracheal suctioning is performed to remove secretions and maintain a patent airway. Additional Authority: Nevada Revised Statute, Nevada Nurse Practice Act,
SUCTIONING, MODIFIED STERILE TRACHEAL Purpose: Tracheal suctioning is performed to remove secretions and maintain a patent airway. Additional Authority: Nevada Revised Statute, Nevada Nurse Practice Act,
PICU tracheostomy protocol
 PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
PICU tracheostomy protocol This protocol is based on the joint Royal Brompton & Harefield NHS Trust and Great Ormond Street Hospital for Children NHS Trust, Great Ormond Street Hospital Manual of Children
Effective Date: August 31, 2006 SUBJECT: TRACHEOSTOMY CARE: CLEANING OF INNER CANNULA
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 418 Effective Date: August 31, 2006 SUBJECT: TRACHEOSTOMY CARE: CLEANING OF INNER CANNULA 1. PURPOSE: To
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 418 Effective Date: August 31, 2006 SUBJECT: TRACHEOSTOMY CARE: CLEANING OF INNER CANNULA 1. PURPOSE: To
HAWAII HEALTH SYSTEMS CORPORATION
 All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
Please provide us with the following information, in case we need to contact you to clarify any of your responses: Name: Title/Position: Phone number:
 Please provide us with the following information, in case we need to contact you to clarify any of your responses: Name: Title/Position: Phone number: Email: These first few questions will tell us about
Please provide us with the following information, in case we need to contact you to clarify any of your responses: Name: Title/Position: Phone number: Email: These first few questions will tell us about
North York General Hospital Policy Manual
 ORIGINATOR: Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: May, 2002 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012 Page
ORIGINATOR: Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: May, 2002 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012 Page
Medication Aide Skills Assessment Review Guide
 Medication Aide Skills Assessment Review Guide Provided by Clarkson College Office of Professional Development professionaldevelopment@clarksoncollege.edu Medication Aide Skills Assessment Study Guide
Medication Aide Skills Assessment Review Guide Provided by Clarkson College Office of Professional Development professionaldevelopment@clarksoncollege.edu Medication Aide Skills Assessment Study Guide
September 2007 Replaces: October 2001
 Inova Fairfax Hospital - Critical Care CRITICAL CARE STANDARD: 4.020 Passy-Muir Tracheostomy Speaking Valve September 2007 Replaces: October 2001 Sonia Astle, RN, MS, CCNS Chair Critical Care Standards
Inova Fairfax Hospital - Critical Care CRITICAL CARE STANDARD: 4.020 Passy-Muir Tracheostomy Speaking Valve September 2007 Replaces: October 2001 Sonia Astle, RN, MS, CCNS Chair Critical Care Standards
CLINICAL SKILLS ASSESSMENT (CSA)
 CLINICAL SKILLS ASSESSMENT (CSA) Applicant Guide INTRODUCTION The College of Respiratory Therapists of Ontario s (CRTO s) entry-topractice assessment process provides a mechanism for applicants for registration
CLINICAL SKILLS ASSESSMENT (CSA) Applicant Guide INTRODUCTION The College of Respiratory Therapists of Ontario s (CRTO s) entry-topractice assessment process provides a mechanism for applicants for registration
Policies & Procedures. Title: TRACHEOSTOMY CARE Adult, Pediatric & Neonate. I.D. Number: Authorization:
 Authorization: [ ] Board of Directors [ ] MAC Motion #: [x] SHR Nursing Practice Committee Policies & Procedures Title: TRACHEOSTOMY CARE Adult, Pediatric & Neonate I.D. Number: 1184 Source: Nursing/Respiratory
Authorization: [ ] Board of Directors [ ] MAC Motion #: [x] SHR Nursing Practice Committee Policies & Procedures Title: TRACHEOSTOMY CARE Adult, Pediatric & Neonate I.D. Number: 1184 Source: Nursing/Respiratory
Description of Essential Criteria for PREPARED Emergency Department
 Description of Essential Criteria for PREPARED Emergency Department Access to optimal emergency care for children is affected by the lack of availability of equipment, appropriately trained staff to care
Description of Essential Criteria for PREPARED Emergency Department Access to optimal emergency care for children is affected by the lack of availability of equipment, appropriately trained staff to care
North York General Hospital Policy Manual
 ORIGINATOR: Code Blue/Pink Committee APPROVED By: Operations Committee Medical Advisory Committee ORIGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012
ORIGINATOR: Code Blue/Pink Committee APPROVED By: Operations Committee Medical Advisory Committee ORIGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29, 2012
North York General Hospital Policy Manual
 ORIGINTATOR: Chair Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29,
ORIGINTATOR: Chair Code Blue/Pink Committee APPROVED BY: Operations Committee Medical Advisory Committee ORGINAL DATE APPROVED: September, 1999 DATE REVIEWED: April, 2012 DATE OF IMPLEMENTATION: June 29,
Department of Emergency Medical Services
 MIAMI DADE COLLEGE MEDICAL CENTER CAMPUS SCHOOL OF HEALTH SCIENCES Department of Emergency Medical Services CLINICAL COURSE OUTLINE EMS 1431 EMERGENCY MEDICAL TECHNICIAN BASIC 1 EMS 1431 EMERGENCY MEDCIAL
MIAMI DADE COLLEGE MEDICAL CENTER CAMPUS SCHOOL OF HEALTH SCIENCES Department of Emergency Medical Services CLINICAL COURSE OUTLINE EMS 1431 EMERGENCY MEDICAL TECHNICIAN BASIC 1 EMS 1431 EMERGENCY MEDCIAL
does staff intervene; used? If not, describe.
 Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
ADC ED/TRAUMA POLICY AND PROCEDURE Policy 221. I. Title Trauma team Activation Protocol/Roles & Responsibilities of the Trauma Team
 Section: ADC Trauma ADC ED/TRAUMA POLICY AND PROCEDURE Policy 221 Subject: Trauma Team Activation Protocol/Roles & Responsibilities of the Trauma Team Trauma Coordinator UTMB respects the diverse culture
Section: ADC Trauma ADC ED/TRAUMA POLICY AND PROCEDURE Policy 221 Subject: Trauma Team Activation Protocol/Roles & Responsibilities of the Trauma Team Trauma Coordinator UTMB respects the diverse culture
393 PICC INSERTION USING ULTRASONOGRAPHY AND MICRO INTRODUCER TECHNIQUE 06/10/03 1
 393 ULTRASONOGRAPHY AND MICRO INTRODUCER TECHNIQUE 06/10/03 1 POLICY: General Information: 1. RN s validated to insert PICCs with the additional training in the use of ultrasonography (U/S) and microintroduction
393 ULTRASONOGRAPHY AND MICRO INTRODUCER TECHNIQUE 06/10/03 1 POLICY: General Information: 1. RN s validated to insert PICCs with the additional training in the use of ultrasonography (U/S) and microintroduction
Policy and Procedures. RNSP: RN Procedure. I.D. Number: 1142
 Policy and Procedures RNSP: RN Procedure Title: CARDIAC (ECG) MONITORING (Adults and Pediatrics) I.D. Number: 1142 Authorization: [X] SHR Nursing Practice Committee Source: Nursing Date Revised: November
Policy and Procedures RNSP: RN Procedure Title: CARDIAC (ECG) MONITORING (Adults and Pediatrics) I.D. Number: 1142 Authorization: [X] SHR Nursing Practice Committee Source: Nursing Date Revised: November
Prone Positioning Protocol
 Prone Positioning Protocol Objectives To illustrate patient criteria for prone positioning as an adjunct therapy in the treatment of Acute Respiratory Distress Syndrome (ARDS) To review the exclusion and
Prone Positioning Protocol Objectives To illustrate patient criteria for prone positioning as an adjunct therapy in the treatment of Acute Respiratory Distress Syndrome (ARDS) To review the exclusion and
About the Critical Care Center
 Patient and Family Education Section 2 About the Critical Care Center The 5-Southeast and 5-East units 5-Southeast and 5-East When You Arrive for a Visit Patient Services Specialist Waiting Rooms Patient
Patient and Family Education Section 2 About the Critical Care Center The 5-Southeast and 5-East units 5-Southeast and 5-East When You Arrive for a Visit Patient Services Specialist Waiting Rooms Patient
Title Oropharyngeal & Oral Yankauer Suction Standard Operating Procedure
 Document Control Title Oropharyngeal & Oral Yankauer Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health & Social Care Community Services Date
Document Control Title Oropharyngeal & Oral Yankauer Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health & Social Care Community Services Date
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES
 UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
UNIVERSITY OF MASSACHUSETTS MEDICAL SCHOOL ANESTHESIOLOGY RESIDENCY PROGRAM GOALS AND OBJECTIVES CA-2/CA-3 REQUIRED ROTATIONS IN PEDIATRIC ANESTHESIOLOGY The Department of Anesthesiology has established
Feedback from Anesthesia clinicians. 2.1 Intubate Patient Workflow
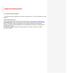 Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Indications for Calling A Code Blue or Pediatric Medical Emergency
 Code Blue/Pediatric Medical Emergency Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in an individual s status (e.g. unresponsiveness, absence of blood
Code Blue/Pediatric Medical Emergency Code Blue is a term used to alert the Code Team and hospital staff of the significant deterioration in an individual s status (e.g. unresponsiveness, absence of blood
St. Vincent s Health System Page 1 of 8. Nursing Administration HOSPITAL SHARED POLICY?
 St. Vincent s Health System Page 1 of 8 TITLE: Rapid Response Team FACILITY: St. Vincent s East FUNCTION: ORIGINATING DEPT: Nursing Administration HOSPITAL SHARED POLICY? EFFECTIVE DATE: _X_ Yes No DOCUMENT
St. Vincent s Health System Page 1 of 8 TITLE: Rapid Response Team FACILITY: St. Vincent s East FUNCTION: ORIGINATING DEPT: Nursing Administration HOSPITAL SHARED POLICY? EFFECTIVE DATE: _X_ Yes No DOCUMENT
GAMUT QI Collaborative Consensus Quality Metrics (v. 05/16/2016)
 1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
1) Ventilator use in patients 1 with advanced airways reported as Percent of patient transport contacts with an advanced airway 2 supported by a mechanical ventilator. 2) Scene and bedside times for STEMI
STANDARDIZED PROCEDURE NEONATAL / PEDIATRIC THORACENTESIS (NEEDLE ASPIRATION) (Neonatal, Pediatric)
 I. Definition To insert a needle into the chest in order to evacuate air or fluid II. Background Information A. Setting: Inpatient neonatal / pediatric patients or outpatient during Emergency Transport
I. Definition To insert a needle into the chest in order to evacuate air or fluid II. Background Information A. Setting: Inpatient neonatal / pediatric patients or outpatient during Emergency Transport
RECOMMENDATION FOR CONSIDERATION
 Board Meeting Date: June 15, 2016 RECOMMENDATION FOR CONSIDERATION Subject: Critical Care Transfer of Care Data Elements and Form VTR#: 0616-04 Committee/Task Force: Critical Care Transport Task Force
Board Meeting Date: June 15, 2016 RECOMMENDATION FOR CONSIDERATION Subject: Critical Care Transfer of Care Data Elements and Form VTR#: 0616-04 Committee/Task Force: Critical Care Transport Task Force
MEDICINES CONTROL COUNCIL
 MEDICINES CONTROL COUNCIL EMERGENCY PROCEDURES FOR CLINICAL TRIAL SITES This document highlights the importance of having emergency standard operating procedures in place during the conduct of clinical
MEDICINES CONTROL COUNCIL EMERGENCY PROCEDURES FOR CLINICAL TRIAL SITES This document highlights the importance of having emergency standard operating procedures in place during the conduct of clinical
RECTAL DIAZEPAM MEDICATION ORDERS IN SCHOOL PURPOSE, INFORMATION, GUIDELINES AND SAMPLE PROCEDURE
 RECTAL DIAZEPAM MEDICATION ORDERS IN SCHOOL PURPOSE, INFORMATION, GUIDELINES AND SAMPLE PROCEDURE PURPOSE: To ensure student safety when recta! diazepam (RD) is administered in the educational setting.
RECTAL DIAZEPAM MEDICATION ORDERS IN SCHOOL PURPOSE, INFORMATION, GUIDELINES AND SAMPLE PROCEDURE PURPOSE: To ensure student safety when recta! diazepam (RD) is administered in the educational setting.
PLACEMENT. Disclaimer
 1 TITLE: GUIDELINE FOR PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE Disclaimer PLACEMENT The Canadian Society of Gastroenterology Nurses and Associates (CSGNA) presents this guideline to be used as a reference
1 TITLE: GUIDELINE FOR PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE Disclaimer PLACEMENT The Canadian Society of Gastroenterology Nurses and Associates (CSGNA) presents this guideline to be used as a reference
Medical Simulation Orientation
 Medical Simulation Orientation Familiarization with IMSE s METI ECS Simulation Manikin Getting to know the Simulator Aims and Goals of Orientation To allow participants to familiarize themselves with the
Medical Simulation Orientation Familiarization with IMSE s METI ECS Simulation Manikin Getting to know the Simulator Aims and Goals of Orientation To allow participants to familiarize themselves with the
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: HEMODIALYSIS TEMPORARY CATHETER (INSERTION, DRESSING CHANGE, REMOVAL, MEDICATION AND BLOOD DRAWS, DISCONTINUATION OF MEDS AND IV FLUIDS)
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: HEMODIALYSIS TEMPORARY CATHETER (INSERTION, DRESSING CHANGE, REMOVAL, MEDICATION AND BLOOD DRAWS, DISCONTINUATION OF MEDS AND IV FLUIDS)
Simulation Scenario Management of obstructed tracheostomy
 INTRODUCTION: Scenario Goals and Objectives: Simulation Scenario Management of obstructed tracheostomy Simulation objectives By the end of this simulation participants will have: 1. Practiced the recognition
INTRODUCTION: Scenario Goals and Objectives: Simulation Scenario Management of obstructed tracheostomy Simulation objectives By the end of this simulation participants will have: 1. Practiced the recognition
Minimum equipment and drug lists for cardiopulmonary resuscitation. Mental health Inpatient care
 Minimum equipment and drug lists for cardiopulmonary resuscitation Mental health Inpatient care Resuscitation Council (UK) 5th Floor Tavistock House North Tavistock Square London WC1H 9HR Published by
Minimum equipment and drug lists for cardiopulmonary resuscitation Mental health Inpatient care Resuscitation Council (UK) 5th Floor Tavistock House North Tavistock Square London WC1H 9HR Published by
SPECIAL MEMORANDUM. All Fresno/Kings/Madera/Tulare EMS Providers, Hospitals, First Responder Agencies, and Interested Parties
 Central California Emergency Medical Services Agency A Division of Fresno County Department of Public Health SPECIAL MEMORANDUM FILE #: F/K/M/T #05-2018 TO: FROM: All Fresno/Kings/Madera/Tulare EMS Providers,
Central California Emergency Medical Services Agency A Division of Fresno County Department of Public Health SPECIAL MEMORANDUM FILE #: F/K/M/T #05-2018 TO: FROM: All Fresno/Kings/Madera/Tulare EMS Providers,
Replacement Of Balloon Retained Gastrostomy (BRG) Procedure Introduction and Aim
 Reference Number: UHB 189 Version Number: 2 Date of Next Review: 10 th Dec 2018 Previous Trust/LHB Reference Number: Replacement Of Balloon Retained Gastrostomy (BRG) Procedure Introduction and Aim The
Reference Number: UHB 189 Version Number: 2 Date of Next Review: 10 th Dec 2018 Previous Trust/LHB Reference Number: Replacement Of Balloon Retained Gastrostomy (BRG) Procedure Introduction and Aim The
A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES. By Maureen Kroning EdD, RN
 A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES By Maureen Kroning EdD, RN Dedication This handbook is dedicated to patients, families, communities and the nurses that touch their lives
A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES By Maureen Kroning EdD, RN Dedication This handbook is dedicated to patients, families, communities and the nurses that touch their lives
Sedation/Analgesia by Non-Anesthesiologists. THE UNIVERSITY OF TOLEDO Approving Officer:
 Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Case 1 Standard of Care. Disclosures. Defending Critical Care: Navigating Through the Malpractice Maze 5/9/2015. Defending Critical Care:
 Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
N: Emergency Nursing. Alberta Licensed Practical Nurses Competency Profile 135
 N: Emergency Nursing Alberta Licensed Practical Nurses Competency Profile 135 Competency: N-1 Multi-Systems Assessment N-1-1 N-1-2 N-1-3 N-1-4 Demonstrate knowledge and ability to apply critical thinking
N: Emergency Nursing Alberta Licensed Practical Nurses Competency Profile 135 Competency: N-1 Multi-Systems Assessment N-1-1 N-1-2 N-1-3 N-1-4 Demonstrate knowledge and ability to apply critical thinking
Reducing the Harm Caused by Misplaced Nasogastric & Orogastric Feeding Tubes Policy April 2017
 Reducing the Harm Caused by Misplaced Nasogastric & Orogastric Feeding Tubes Policy April 2017 Page 1 of 12 Title Author(s) Reducing the Harm Caused by Misplaced Nasogastric & Orogastric Feeding Tubes
Reducing the Harm Caused by Misplaced Nasogastric & Orogastric Feeding Tubes Policy April 2017 Page 1 of 12 Title Author(s) Reducing the Harm Caused by Misplaced Nasogastric & Orogastric Feeding Tubes
PROCEDURAL SEDATION AND ANALGESIA: HOSPITAL-WIDE POLICY
 CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
CLINICAL PRACTICE POLICY PAGE: 1 OF 6 PURPOSE: These policies will allow clinicians to provide their patients with the benefits of procedural sedation and analgesia while minimizing the associated risks.
Family/Caregiver Education Checklist Return Demonstration of Knowledge FIRST 24 HOURS
 of Knowledge FIRST 24 HOURS The following checklists will be completed by a PDN RN or LPN to ensure family/caregiver s skill level is adequate to safely take care of their child independently Teaching
of Knowledge FIRST 24 HOURS The following checklists will be completed by a PDN RN or LPN to ensure family/caregiver s skill level is adequate to safely take care of their child independently Teaching
Subacute Care. 1. Define important words in the chapter. 2. Discuss the types of residents who are in a subacute setting
 175 26 Subacute Care 1. Define important words in this chapter 2. Discuss the types of residents who are in a subacute setting 3. List care guidelines for pulse oximetry 4. Describe telemetry and list
175 26 Subacute Care 1. Define important words in this chapter 2. Discuss the types of residents who are in a subacute setting 3. List care guidelines for pulse oximetry 4. Describe telemetry and list
Prone Ventilation of the Critically Ill Patient
 Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Respirator. Prerequisit. ive review to. Comprehensi. exam success C5, C6, C7, C8, C16) C7,C12,C15,C16, ,C18) C19, C20) C15, C18, C19, C20)
 Respirator ry Care Examinationn Preparation (RSPT 2230) Capstone Course Credit: 2 semester credit hours (2 hours lecture, 1 hour lab) Prerequisit te/co-requisite: RSPT 1113, RSPT 1207, RSPT 1261, RSPT
Respirator ry Care Examinationn Preparation (RSPT 2230) Capstone Course Credit: 2 semester credit hours (2 hours lecture, 1 hour lab) Prerequisit te/co-requisite: RSPT 1113, RSPT 1207, RSPT 1261, RSPT
ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE
 ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE Rotation Contacts and Scheduling Details Rotation Director: Kelly Yeh, MD Director of Pediatric Anesthesia Santa Clara Valley Medical Center kelly.yeh@hhs.sccgov.org.,
ROTATION SUMMARY PEDIATRIC ANESTHESIA ELECTIVE Rotation Contacts and Scheduling Details Rotation Director: Kelly Yeh, MD Director of Pediatric Anesthesia Santa Clara Valley Medical Center kelly.yeh@hhs.sccgov.org.,
PROCEDURAL SAFETY CHECKLIST
 PROCEDURAL SAFETY CHECKLIST Before any medical or patient care procedure, review checklist together with the other members of the procedural team. This checklist can be used by any health professional
PROCEDURAL SAFETY CHECKLIST Before any medical or patient care procedure, review checklist together with the other members of the procedural team. This checklist can be used by any health professional
Iowa Department of Public Health BUREAU OF EMERGENCY MEDICAL SERVICES. Promoting and Protecting the Health of Iowans through EMS
 Iowa Department of Public Health BUREAU OF EMERGENCY MEDICAL SERVICES Iowa Emergency Medical Care Provider Scope of Practice April 2012 Promoting and Protecting the Health of Iowans through EMS LUCAS STATE
Iowa Department of Public Health BUREAU OF EMERGENCY MEDICAL SERVICES Iowa Emergency Medical Care Provider Scope of Practice April 2012 Promoting and Protecting the Health of Iowans through EMS LUCAS STATE
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: (crc15-nursing) (crc.02-respiratory) Nursing Respiratory Care Services DATE: REVIEWED: PAGES: 02/93 9/17 1 of 8 RESPONSIBILITY: RN, LPN II
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: (crc15-nursing) (crc.02-respiratory) Nursing Respiratory Care Services DATE: REVIEWED: PAGES: 02/93 9/17 1 of 8 RESPONSIBILITY: RN, LPN II
A. Administration and Coordination of the Emergency Department (ED) for the Care of Children.
 Note: Pediatric Emergency Care (PEC) recognition does not reflect a hospital s trauma capabilities. Trauma designation is a separate stand-alone program. Criteria for Emergency Department Pediatric Readiness
Note: Pediatric Emergency Care (PEC) recognition does not reflect a hospital s trauma capabilities. Trauma designation is a separate stand-alone program. Criteria for Emergency Department Pediatric Readiness
Title: ED Management of Trauma Patient Protocol
 Title: ED Management of Trauma Patient Protocol Document Category: Clinical Document Type: Protocol Department/Committee Owner: Emergency Department Original Date: August 2009 Approver(s) last review:
Title: ED Management of Trauma Patient Protocol Document Category: Clinical Document Type: Protocol Department/Committee Owner: Emergency Department Original Date: August 2009 Approver(s) last review:
ROUGE VALLEY HEALTH SYSTEM PRACTICE STANDARDS MANUAL
 ISSUED BY: PPL, CRITICAL CARE COMMITTEE PAGE: 1 of 5 PURPOSE To ensure standardized practice in the care of Arterial line Catheters To provide guidelines for care, maintenance, monitoring, troubleshooting,
ISSUED BY: PPL, CRITICAL CARE COMMITTEE PAGE: 1 of 5 PURPOSE To ensure standardized practice in the care of Arterial line Catheters To provide guidelines for care, maintenance, monitoring, troubleshooting,
Functional Abilities / Core Performance Standards
 Functional Abilities / Core Performance Standards Please Review the list of skills below. If you unable to meet the standard/s even with correction (example: eyeglasses, hearing aids) on any of the items
Functional Abilities / Core Performance Standards Please Review the list of skills below. If you unable to meet the standard/s even with correction (example: eyeglasses, hearing aids) on any of the items
OVERVIEW OF THE QUICK RESPONSE SERVICE
 OVERVIEW OF THE QUICK RESPONSE SERVICE Pennsylvania Department of Health Bureau of Emergency Medical Services Revised March 01, 2012 TABLE OF CONTENTS Page # Introduction 3 Application Process 3 Inspection
OVERVIEW OF THE QUICK RESPONSE SERVICE Pennsylvania Department of Health Bureau of Emergency Medical Services Revised March 01, 2012 TABLE OF CONTENTS Page # Introduction 3 Application Process 3 Inspection
MIAMI DADE COLLEGE MEDICAL CAMPUS BENJAMIN LEON SCHOOL OF NURSING RN-BSN PROGRAM MANUAL OF CLINICAL PERFORMANCE
 MIAMI DADE COLLEGE MEDICAL CAMPUS BENJAMIN LEON SCHOOL OF NURSING RN-BSN PROGRAM MANUAL OF CLINICAL PERFORMANCE 1 INTRODUCTION Welcome to Miami Dade College Bachelor of Science in Nursing Program. The
MIAMI DADE COLLEGE MEDICAL CAMPUS BENJAMIN LEON SCHOOL OF NURSING RN-BSN PROGRAM MANUAL OF CLINICAL PERFORMANCE 1 INTRODUCTION Welcome to Miami Dade College Bachelor of Science in Nursing Program. The
RNSP: Advanced RN Intervention
 Policies and Procedures RNSP: Advanced RN Intervention Title: CHEST TUBES: IRRIGATION AND/OR ADMINISTRATION OF A MEDICATION TO THE PLEURAL SPACE I.D. Number: 1016 Authorization: [X] SHR Nursing Practice
Policies and Procedures RNSP: Advanced RN Intervention Title: CHEST TUBES: IRRIGATION AND/OR ADMINISTRATION OF A MEDICATION TO THE PLEURAL SPACE I.D. Number: 1016 Authorization: [X] SHR Nursing Practice
Event Orientation Competition
 Gotta-Have-It Chart One area of heartbreak at state and national HOSA competitive events is a failure to bring the needed supplies/materials to an event for orientation or competition. Every year competitors
Gotta-Have-It Chart One area of heartbreak at state and national HOSA competitive events is a failure to bring the needed supplies/materials to an event for orientation or competition. Every year competitors
Marianne Chulay is a critical care nursing/clinical research consultant in Chapel Hill, NC. The author has no financial relationships to disclose.
 VAP is a common and potentially fatal complication of ventilator care. Following the latest CDC recommendations is the best defense you can offer your patients. Marianne Chulay, RN, DNSC, FAAN Marianne
VAP is a common and potentially fatal complication of ventilator care. Following the latest CDC recommendations is the best defense you can offer your patients. Marianne Chulay, RN, DNSC, FAAN Marianne
HenryE.Wang,MD,MPH,RobertM.Domeier,MD,DouglasF.Kupas,MD, MarkJ.Greenwood,DO,JD,RobertE.O Connor,MD,MPH
 POSITION PAPER NATIONAL ASSOCIATION OF EMS PHYSICIANS RECOMMENDED GUIDELINES FOR UNIFORM REPORTING OF DATA FROM OUT-OF-HOSPITAL AIRWAY MANAGEMENT: POSITION STATEMENT OF THE NATIONAL ASSOCIATION OF EMS
POSITION PAPER NATIONAL ASSOCIATION OF EMS PHYSICIANS RECOMMENDED GUIDELINES FOR UNIFORM REPORTING OF DATA FROM OUT-OF-HOSPITAL AIRWAY MANAGEMENT: POSITION STATEMENT OF THE NATIONAL ASSOCIATION OF EMS
CLINICAL SKILLS & OBSERVATION CHECKLIST
 CLINICAL SKILLS & OBSERVATION CHECKLIST Employee: Please check Yes or No at time of hire and annually for Adult and/or Pediatric experience RN Supervisor: Please date and initial after observation & demonstration
CLINICAL SKILLS & OBSERVATION CHECKLIST Employee: Please check Yes or No at time of hire and annually for Adult and/or Pediatric experience RN Supervisor: Please date and initial after observation & demonstration
Course Outline and Assignments
 Course Outline and Assignments WEEK ONE 10-16-12 Instructional In Class-Learning to be completed prior to class 10-17-12 Total Hours Assessment 1. proper hand washing techniques 2. donning and removing
Course Outline and Assignments WEEK ONE 10-16-12 Instructional In Class-Learning to be completed prior to class 10-17-12 Total Hours Assessment 1. proper hand washing techniques 2. donning and removing
TEXAS FACILITY READINESS PROGRAM CHECK LIST
 TEXAS FACILITY READINESS PROGRAM CHECK LIST PEDIATRIC READY Official Completing Form (please print): Date: Initials: Instructions: The requirements and acceptable documentation are detailed for each item
TEXAS FACILITY READINESS PROGRAM CHECK LIST PEDIATRIC READY Official Completing Form (please print): Date: Initials: Instructions: The requirements and acceptable documentation are detailed for each item
Advanced Cardiovascular Life Support (ACLS) Study assistance for employees of Lake EMS
 Advanced Cardiovascular Life Support (ACLS) Study assistance for employees of Lake EMS Situation Much of the great care we perform relies on our protocols Our protocols are primarily based initially on
Advanced Cardiovascular Life Support (ACLS) Study assistance for employees of Lake EMS Situation Much of the great care we perform relies on our protocols Our protocols are primarily based initially on
SURGICAL SAFETY CHECKLISTS
 1 SURGICAL SAFETY CHECKLISTS Power Play: Managing the Forces that Impact Implementation The Experience of a small isolated community hospital Presentation by: Mark Balcaen. March 8-9, 2010 2 Background
1 SURGICAL SAFETY CHECKLISTS Power Play: Managing the Forces that Impact Implementation The Experience of a small isolated community hospital Presentation by: Mark Balcaen. March 8-9, 2010 2 Background
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: TRACHEOSTOMY SPEAKING VALVE EFFECTIVE DATE: REVISED DATE: POLICY TYPE: 135.008 (Respiratory Therapy) (Patient Care) 134.900 (Rehab) 10/93
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: TRACHEOSTOMY SPEAKING VALVE EFFECTIVE DATE: REVISED DATE: POLICY TYPE: 135.008 (Respiratory Therapy) (Patient Care) 134.900 (Rehab) 10/93
Goals & Objectives 4/17/2014 UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN. Why would someone need to do this?
 UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN Goals & Objectives Participants will increase their knowledge about AHCD Review AHCD documents used at the hospital Role
UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN Goals & Objectives Participants will increase their knowledge about AHCD Review AHCD documents used at the hospital Role
DETERIORATING PATIENT & RESUSCITATION POLICY
 DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
DETERIORATING PATIENT & RESUSCITATION POLICY Version Number: 2.3 Version date: December 2015 Policy Owner Author First approval or date last reviewed Staff/Groups Consultant Discussed by Policy Group Director
Routine Practices. Infection Prevention and Control
 Routine Practices Infection Prevention and Control Routine Practices Elements of Routine Practices: Risk assessment + hand hygiene + personal protective equipment Environmental controls (patient placement,
Routine Practices Infection Prevention and Control Routine Practices Elements of Routine Practices: Risk assessment + hand hygiene + personal protective equipment Environmental controls (patient placement,
Endotracheal Intubation Adult (April 2013)
 Endotracheal Intubation Adult (April 2013) Placement of tube into patient s trachea in order to provide pulmonary ventilation. Advanced Life Support procedure Specified in existing regulations. Not authorized
Endotracheal Intubation Adult (April 2013) Placement of tube into patient s trachea in order to provide pulmonary ventilation. Advanced Life Support procedure Specified in existing regulations. Not authorized
Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients
 UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
UNM Trauma & EM Operational Policies Subject: Trauma Team Roles and Responsibilities for TRAUMA ACTIVATION patients Purpose: To define the roles and responsibilities of personnel responding to trauma activations,
@ncepod #tracheostomy
 @ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
@ncepod #tracheostomy 1 Introduction Tracheostomy: Remedy upper airway obstruction Avoid complications of prolonged intubation Protection & maintenance of airway The number of temporary tracheostomies
1. Communicate to the UAP any special information needed prior to the administration of the medication.
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by intradermal injection. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by intradermal injection. 2. document medication administration in the client
Simulation Design Template. Date: May 7, 2008 File Name: Group 4
 Simulation Design Template Date: May 7, 2008 File Name: Group 4 Discipline: Nursing, medicine, radiology, EMT, possible consultant (specialist ie neurosurgeon via conference call), possible social work/pastoral
Simulation Design Template Date: May 7, 2008 File Name: Group 4 Discipline: Nursing, medicine, radiology, EMT, possible consultant (specialist ie neurosurgeon via conference call), possible social work/pastoral
Title Nasopharyngeal Suction Standard Operating Procedure
 Document Control Title Nasopharyngeal Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health and Social Care Community Services Date Version Status
Document Control Title Nasopharyngeal Suction Standard Operating Procedure Author s job title Community Respiratory Physiotherapist Directorate Health and Social Care Community Services Date Version Status
BAYTOWN FIRE DEPARTMENT 201 E. Wye Drive Baytown, TX
 Shon Blake Fire Chief Rick Davis City Manager Permitting Procedure for Private Ambulance Service The proposed ambulance permitting procedure is essentially a form of registration for private ambulances
Shon Blake Fire Chief Rick Davis City Manager Permitting Procedure for Private Ambulance Service The proposed ambulance permitting procedure is essentially a form of registration for private ambulances
Review of Clinical Practice Guidelines in Suction Therapy. Disclaimer. Suctioning the Patient in the Home Types of Suction Therapy
 Review of Clinical Practice Guidelines in Suction Therapy Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Dave Henry RRT Name of employer: DeVilbiss Healthcare Definition:
Review of Clinical Practice Guidelines in Suction Therapy Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Dave Henry RRT Name of employer: DeVilbiss Healthcare Definition:
EMS Service Inspection Policy
 EMS Service Inspection Policy Approved 04/01/2016 The Kansas Board of EMS 900 SW Jackson, Room 1031 Landon State Office Building Topeka, KS 66612 (785) 296-7296 www.ksbems.org Contents Inspection Procedures/Corrective
EMS Service Inspection Policy Approved 04/01/2016 The Kansas Board of EMS 900 SW Jackson, Room 1031 Landon State Office Building Topeka, KS 66612 (785) 296-7296 www.ksbems.org Contents Inspection Procedures/Corrective
Z: Perioperative Nursing Specialty
 Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Z: Perioperative Nursing Specialty Alberta Licensed Practical Nurses Competency Profile 263 Major Competency Area: Z Perioperative Nursing Specialty Priority: One Competency: Z-1 HPA Authorizations and
Activation of the Rapid Response Team
 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool
 Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Nursing. Lab Name Location Person in Charge Programs Served Courses Served. M Muna Al -Tamimi Nursing Department
 Central Laboratories Catalog Nursing Laboratories Nursing Lab Name Location Person in Charge Programs Served Courses Served Maternity & Child Health Nursing & Basic Life Support (BLS) Skills Lab Fundamentals
Central Laboratories Catalog Nursing Laboratories Nursing Lab Name Location Person in Charge Programs Served Courses Served Maternity & Child Health Nursing & Basic Life Support (BLS) Skills Lab Fundamentals
Appendix B: Departments / Programs
 1 Appendix B: Departments / Programs The Guide to Conduct Hand Hygiene Reviews contains important information that applies to hand hygiene reviews performed in all areas across the continuum of care. Appendix
1 Appendix B: Departments / Programs The Guide to Conduct Hand Hygiene Reviews contains important information that applies to hand hygiene reviews performed in all areas across the continuum of care. Appendix
Policies and Procedures. RNSP: RN Procedure. I.D. Number: 1067
 Policies and Procedures RNSP: RN Procedure Title: CHEMOTHERAPY BLADDER INSTILLATION (INTRAVESICAL) CARE OF CLIENT I.D. Number: 1067 Authorization: [] SHR Nursing Practice Committee Source: Nursing Date
Policies and Procedures RNSP: RN Procedure Title: CHEMOTHERAPY BLADDER INSTILLATION (INTRAVESICAL) CARE OF CLIENT I.D. Number: 1067 Authorization: [] SHR Nursing Practice Committee Source: Nursing Date
Vanderbilt University Medical Center. Division of Trauma and Surgical Critical Care. Clinical Management Guideline: Standard Trauma Resuscitation
 Introduction Vanderbilt University Medical Center Division of Trauma and Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Good communication and leadership are the keys
Introduction Vanderbilt University Medical Center Division of Trauma and Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Good communication and leadership are the keys
Teaching Methods. Responsibilities
 Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
Avera McKennan Critical Care Medicine Rotation Goals and Objectives Pulmonary/Critical Care Medicine Fellowship Program University of Nebraska Medical Center Written: May 2011 I) Rotation Goals A) To manage
ASEPTIC TECHNIQUE LEARNING PACKAGE
 ASEPTIC TECHNIQUE LEARNING PACKAGE Staff Name:... Date:... Table of Contents What is Aseptic technique? 3 Core infection control components 3 Key parts 5 References 6 Aseptic technique questionnaire 7
ASEPTIC TECHNIQUE LEARNING PACKAGE Staff Name:... Date:... Table of Contents What is Aseptic technique? 3 Core infection control components 3 Key parts 5 References 6 Aseptic technique questionnaire 7
Policies and Procedures. RNSP: RN Procedure. ID Number: 1105 Source: Nursing Date Effective: February, 2017 Scope: SHR and Affiliates
 Policies and Procedures RNSP: RN Procedure Title: GASTROSTOMY TUBE (Balloon Type): Adult and Pediatric: Authorization [x] SHR Nursing Practice Committee ID Number: 1105 Source: Nursing Date Effective:
Policies and Procedures RNSP: RN Procedure Title: GASTROSTOMY TUBE (Balloon Type): Adult and Pediatric: Authorization [x] SHR Nursing Practice Committee ID Number: 1105 Source: Nursing Date Effective:
STANDARDIZED PROCEDURE CENTRAL LINE PLACEMENT and TEMPORARY NONTUNNELLED CENTRAL VENOUS DIALYSIS CATHETER INSERTION (Adult, Peds)
 I. Definition: This protocol covers the task of central (venous) catheter placement and temporary nontunnelled central venous dialysis catheters by the Advanced Health Practitioner. The purpose of this
I. Definition: This protocol covers the task of central (venous) catheter placement and temporary nontunnelled central venous dialysis catheters by the Advanced Health Practitioner. The purpose of this
Commercial Ambulance Services. Annual Renewal & Inspection Application Packet NEONATAL SERVICE INFORMATION
 Maryland Institute for Emergency Medical Services Systems Office of Commercial Ambulance Licensing & Regulation 653 West Pratt Street Baltimore, MD 21201-1536 Office: (410) 706-8511 - Fax: (410) 706-8552
Maryland Institute for Emergency Medical Services Systems Office of Commercial Ambulance Licensing & Regulation 653 West Pratt Street Baltimore, MD 21201-1536 Office: (410) 706-8511 - Fax: (410) 706-8552
S T A N D A R D O P E R A T I N G G U I D E L I N E
 C H AR L O T T E S V I L L E A L B E M A R L E R E S C U E S Q U A D S T A N D A R D O P E R A T I N G G U I D E L I N E TOPIC: Special Events Scott Stadium - Operations S.O.P. # 4.5a Approved by: Lair
C H AR L O T T E S V I L L E A L B E M A R L E R E S C U E S Q U A D S T A N D A R D O P E R A T I N G G U I D E L I N E TOPIC: Special Events Scott Stadium - Operations S.O.P. # 4.5a Approved by: Lair
