Staff Acceptance of Tele-ICU Coverage
|
|
|
- Daniel Watkins
- 6 years ago
- Views:
Transcription
1 CHEST Original Research Staff Acceptance of Tele-ICU Coverage A Systematic Review Lance Brendan Young, PhD, MBA ; Paul S. Chan, MD, MSc ; and Peter Cram, MD, MBA CRITICAL CARE Background: Remote coverage of ICUs is increasing, but staff acceptance of this new technology is incompletely characterized. We conducted a systematic review to summarize existing research on acceptance of tele-icu coverage among ICU staff. Methods: We searched for published articles pertaining to critical care telemedicine systems (aka, tele-icu) between January 1950 and March 2010 using PubMed, Cumulative Index to Nursing and Allied Health Literature, Global Health, Web of Science, and the Cochrane Library and s and presentations delivered at national conferences. Studies were included if they provided original qualitative or quantitative data on staff perceptions of tele-icu coverage. Studies were imported into content analysis software and coded by tele-icu configuration, methodology, participants, and findings (eg, positive and negative staff evaluations). Results: Review of 3,086 citations yielded 23 eligible studies. Findings were grouped into four categories of staff evaluation: overall acceptance level of tele-icu coverage (measured in 70% of studies), impact on patient care (measured in 96%), impact on staff (measured in 100%), and organizational impact (measured in 48%). Overall acceptance was high, despite initial ambivalence. Favorable impact on patient care was perceived by. 82% of participants. Staff impact referenced enhanced collaboration, autonomy, and training, although scrutiny, malfunctions, and contradictory advice were cited as potential barriers. Staff perceived the organizational impact to vary. An important limitation of available studies was a lack of rigorous methodology and validated instruments in many studies. Conclusions: Initial reports suggest high levels of staff acceptance of tele-icu coverage, but more rigorous methodologic study is required. CHEST 2011; 139(2): Although intensivist care is associated with lower ICU and hospital mortality and with reduced length of stay, 1 only one-third of critically ill patients receive intensivist care, and the shortfall is projected Manuscript received July 14, 2010; revision accepted October 13, Affiliations: From the Iowa City VA Medical Center (Drs Young and Cram), Iowa City, IA; Mid America Heart Institute and the University of Missouri (Dr Chan), Kansas City, MO; and Division of General Internal Medicine (Dr Cram), Department of Internal Medicine, University of Iowa Carver College of Medicine, Iowa City, IA. Funding/Support: Dr Young is supported by a postdoctoral fellowship from the Department of Veterans Affairs. Dr Chan is supported by a K23 career development award [HL102224] from the National Heart, Lung, and Blood Institute. Dr Cram is supported by a K23 career development award [RR ] from the National Center for Research Resources at the National Institutes of Health and by the Robert Wood Johnson Physician Faculty Scholars Program. This work is also funded by the Veterans Administration Health Services Research and Development Service [grant IIR ] and the National Heart, Lung, and Blood Institute at the National Institutes of Health [R01 HL085347]. to worsen. 2 As a result, hospitals increasingly rely on tele-icu coverage. 3 For the purposes of this article, we define tele-icu coverage as the application of telemedicine 4 to in-hospital critical care units, thereby encompassing an array of technologies of varying complexity 5,6 that allow physical ICUs to access critical care experts in real time. At the present time, it is estimated that 10% of US hospitals use some form of tele-icu coverage, This material is based on work supported by the Department of Veterans Affairs, Veterans Health Administration, Office of Research and Development, Health Services Research and Development, and the VA Midwest Rural Health Resource Center. Correspondence to: Lance Brendan Young, PhD, MBA, Center for Research in the Implementation of Innovative Strategies in Practice, Iowa City VA Medical Center, Mail Stop 152, Iowa City, IA 52242; Lance.Young@va.gov. Reproduction of this article is prohibited without written permission from the American College of Chest Physicians ( site/misc/reprints.xhtml ). DOI: /chest CHEST / 139 / 2 / FEBRUARY,
2 and expansion seems likely. 7 Despite rapid adoption, reported effectiveness of tele-icu coverage has varied across studies, 8-11 and studies often have neglected to address tele-icu impact on staff. Staff impact is important as evidenced by a report of one hospital system that dropped tele-icu coverage after 2 years. 12 Not only do monitoring and intervention by specialists likely influence the interpersonal dynamics of the ICU staff but also that same staff is responsible for implementing and operating the new system. The objective of the present study was to systematically evaluate the published and unpublished literature addressing acceptance of tele-icu coverage by ICU staff with a focus on benefits and challenges seen by frontline providers adopting this new technology. Literature Search Materials and Methods Our literature review was conducted in accordance with guidelines for the conduct of systematic reviews Reliance on deidentified published data precluded the need for institutional review board approval. With the assistance of a medical research librarian, we searched for studies evaluating staff acceptance of critical care telemedicine systems published between January 1, 1950, and March 31, 2010, using PubMed, Cumulative Index to Nursing and Allied Health Literature, Global Health, Web of Science, and Cochrane Library. Because terminology for tele-icu has not been standardized, our search used several terms to describe tele-icu systems (eg, eicu, remote ICU, virtual ICU) alone and in combination with relevant medical subject heading terms (eg, critical care AND telemedicine). We supplemented this search with a keyword search and review of s presented at relevant major scientific conferences between 2006 and Inclusion Criteria Studies were considered eligible for inclusion if they met each of the following criteria: (1) addressed real-time telemedicine within an ICU, (2) presented original quantitative or qualitative data on the impact of tele-icu coverage, and (3) assessed staff acceptance of tele-icu coverage. We defined staff acceptance as any objective or subjective evaluation, recognizing that our broad inclusion criteria would result in studies that included both moreand less-rigorous assessments. Staff included in these studies might include physicians, nurses, and administrators working in either the ICU or the monitoring center. Two authors (P. C. and L. B. Y.) independently reviewed each study, and discrepancies were resolved through discussion. Data Abstraction and Analysis Staff acceptance was a primary focus in some studies but of ancillary interest in others. Formal meta-analysis was not possible given the variation in methodology used in individual studies. We therefore relied on a standard content analytic method 16,17 that integrated both quantitative and qualitative findings within categories describing tele-icu impact. 18,19 After importing the studies into NVivo 8 content analysis software (QSR International, Pty, Ltd; Doncaster, Victoria, Australia), 20 one of the investigators with formal training in content analysis (L. B. Y.) ed data on the tele-icu configuration investigated, including type of technology involved (bedside monitors for each patient, a single mobile camera, or a remote-controlled robot), coverage level (scheduled telerounds, on-call consultation, or ongoing monitoring and consultation), and tele-icu structure. Structure was coded as hub and spoke (single monitoring center covering multiple ICUs), parent-child (one hospital extending existing intensivist coverage remotely to another), or collaborative/network (mobile intensivists offering services from home, hospital, or any other location). Also coded were study method (quantitative, qualitative, interview, or case study), participants (physician, nurse, administrator, or unidentified staff), and findings. Analysis of study findings were guided by our research question: How do staff members view tele-icu coverage? We began by open coding 17 the quantitative studies and then applying those codes to the qualitative data, which fit them well. Participants introduced few issues or processes unaddressed in researcherdefined s. One code represented overall acceptance (eg, satisfaction), and three codes represented staff evaluations of tele-icu impact on quality of patient care, on staff, and on the organization. Description of Studies Results Study Selection: We identified 3,086 studies that focused on critical care telemedicine and subsequently excluded 2,904 studies that did not focus on tele-icu coverage or that contained no original data ( Fig 1 ). The remaining 182 studies were given full review, and 23 met the inclusion criteria. 5,21-42 When data from a single tele-icu was reported in multiple articles or s, the article with the most comprehensive results was used Table 1 summarizes the included studies; 10 (43%) were unpublished s. Staff acceptance was the primary focus of 10 studies, 23,26,29,30,34,36-38,40,41 whereas it was a secondary focus of the remaining 13. 5,21,22,24,25,27,28,31-33,35,39,42 Tele-ICU Configuration: There was significant variation in how tele-icu was defined, used, and structured ( Table 2 ). In 12 studies (52%), tele-icu involved bedside monitors and cameras, 5,24,29-32,34,36-38,40,41 whereas the remaining 11 (48%) used mobile cameras or robots ,25-28,33,35,39,42 Likewise, 12 (52%) studies described systems using around-the-clock telemonitoring,5,21,24,29,30,32,34,36-38,40,41 whereas seven (30%) entailed only on-call consultation, 22,23,31,33,35,39,42 and four (17%) used a system of regularly scheduled telerounds Thirteen (57%) studies included tele-icus structured on a hub-and-spoke model, 5,21,24,29,30,32,34,36-38,40-42 whereas 10 (43%) evaluated ICUs using parent-child or collaborative/network set-ups. 22,23,25-28,31,33,35,39 Study Methodology: Eighteen studies assessed acceptance using Likert or simple yes/no questions, 21-23,25-30,32-35,37-39,41,42 and two of these included a qualitative component. 28,34 Only two (11%) studies 280 Original Research
3 In two studies evaluating preimplementation views of staff, there were significant misgivings about tele-icu coverage. Initial resistance was most pronounced among nursing staff, but acceptance may improve over time. 28 Another study that evaluated nurses preimplementation perceptions of tele-icu coverage found that on a five-point Likert scale (1 5 not favorable, 5 5 favorable), perceived usefulness averaged 2.8 and attitude, Figure 1. Tele-ICU acceptance literature search flow diagram. used validated instruments to assess acceptability. 34,41 Among the five (22%) studies relying exclusively on qualitative methods, two reported interview findings, 5,40 and three provided summaries of case studies. 24,31,36 Participants: Acceptance was examined among physicians in 16 (70%) studies, 21-28,30,32,33,35,37,39-41 nurses in 13 (57%), 21-25,27-29,34,36,38,40,42 and hospital administrators in one (4%). 5 Five (22%) studies included data on clinicians providing teleservices. 21,27,32,33,40 Findings Sixteen (70%) studies provided staff members overall acceptance of tele-icu coverage, 21,22,24-29, (96%) assessed impact on patient care, 5,21-37,39-42 all assessed impact on staff; and 11 (48%) assessed impact on the organization. 5,21-24,31,32,34,35,40,41 Table 3 summarizes findings in each category and identifies potential implementation barriers mentioned by participants. Overall Acceptance: Studies assessing overall acceptance generally were favorable. Studies used a variety of terms in describing acceptance, including acceptance,34,36 perception,27,29,30,37 experience,32 buy-in,38 receptiveness,23 and attitudes.41 Among the four studies using a five-point Likert scale (15 poor acceptance, 55 high acceptance), mean satisfaction with tele-icu coverage ranged from to Among residents training in ICUs equipped with tele-icu, 66.7% wanted tele-icu postresidency. 37 Evaluations of Impact on Quality of Patient Care: Participants had positive views of the impact of tele-icu coverage on patient care. Prior to implementation, 67% of the ICU physicians and nurses believed that tele-icu coverage would enhance ICU quality of care 23 ; postimplementation, between 82.3% and 100% of respondents reported tele-icu coverage had successes in enhancing quality. 28,32,33,37,45 Studies focusing exclusively on nursing perspectives were similarly favorable. 21,27,42 Most ICU nurses believed that tele-icu coverage increased patient survival (72%), but fewer thought it prevented medical errors (47%). 29 Studies reported two potential negative consequences of tele-icu coverage related to patient care. Two suggested that nurses in physical ICUs might not take advice from the monitoring center nurses. 28,34 Four suggested that patient care might suffer if tele-icu staffing diminished the quantity or quality of nurses in the ICU. 5,34,36,40 Evaluations of Staff Impact: Evaluations of how tele-icu coverage affects an individual s work were nuanced and complex. Before implementation, 67% of ICU staff believed that tele-icu coverage would facilitate collaboration with intensivists 23 ; after implementation, communication between the ICU and tele-icu was rated good or very good by 94% of teleintensivists and by 98% of bedside physicians. 33 Collaboration was perhaps more important to parentchild than to hub-and-spoke relationships, 21,22,49,50 and compared with telephone contact, audiovisual interaction was associated with more intensivist suggestions and more-frequent implementation of those suggestions.22,28 Participants also cited potential barriers to acceptance of tele-icu coverage. Nurses reported conflict arising when advice offered remotely conflicted with treatment prescribed by ICU attending physicians. 34 Furthermore, some nurses practiced avoidance behaviors 24 or simply waited until a consulting telephysician was on duty before seeking advice. 40 Monitoring could foster resentment of the oversight process. 5,22,29,31,34,40 Other challenges reported by staff included complaints that the tele-icu coverage increased interruptions 34 and workload, 28,31 whereas other studies CHEST / 139 / 2 / FEBRUARY,
4 Table 1 Design of Studies Evaluating Staff Acceptance of TICU Coverage Study/Year Publication Status Study Method Participants Evaluation Point Summary of Findings Berenson et al 5 /2009 Published Interview Administrators (n 5453 pre and 581 post) Coletti et al 30 /2008 Published Crawley 31 /2008 Meeting DiMartino et al 29 /2009 Meeting Faiz et al 32 /2006 Meeting Medical ICU residents (n 5 35) Pre/ Pre: Perception that substantial costs are not justified by potential benefit, that current staffing was adequate, and that onsite was preferable to off-site staff. : Broad perception that TICU improves quality and safety, but no objective data support those beliefs. Frustration with IT interface problems. 77% reported improved patient safety. 63% reported improved ability to focus on urgent patient issues. 51% reported increase in uninterrupted periods of rest. 37% reported that TICU held educational value. Case study Staff (n 5 NR) Reports of enhanced training of physician staff, high system reliability, and enhanced Army-Navy cooperation. Perceived workload increase, big-brother concerns, lack of need, failure to recognize when help is needed, and IT interface/security challenges. Grundy et al 28 /1977 Published and qualitative Heath et al 33 /2009 Published Nurses (n 591) 72% believed that TICU increases patient survival. 47% believed that TICU prevents errors. 42% believed that TICU improves family satisfaction. 13% felt spied upon. 11% believed that TICU was intrusive. 9% believed that TICU interrupted workflow. 79% believed that knowing the telephysician was important, and 61% were more likely to contact the consultant if they knew the physician on call. Telephysicians (n 5 16) Physicians and nurses (n 5 NR) Physicians (n 5 41 consultations), Teleintensivists (n 5 63 consultations) Of 16 fellows rotating through the eicu remote site, 14 of 16 would want to work in a place with TICU, and 13 of 16 believed that it protected against liability. All believed that TICU improved patient care. 88% of nurses believed that TICU benefited patients, and 70% believed that it enhanced education. Nurses reported positive attitudes toward TICU on 40 occasions and negative attitudes on 21. Over time, resistance was replaced by enthusiasm. Physicians reported positive attitudes toward TICU on 17 occasions and negative attitudes on 4. Although acceptance increased over time, physicians implemented only 46% of consultant suggestions in the last 84 d of the program. Some physicians resented the consultant. Unit of analysis was the consultation. In 88% of pediatric consultations to rural EDs, the physician agreed that consultation improved care. In 89% of consultations, the consulting intensivist agreed that the consultation improved care. (Continued) 282 Original Research
5 Table 1 (Continued) Study/Year Publication Status Study Method Participants Evaluation Point Summary of Findings Kowitlawakul34 /2008 Published and qualitative Marcin et al 35 /2004 Published Marttos et al 27 /2008 Meeting Nurses (n quantitative and n 5 34 qualitative) Physicians (n 5 53), nurses, respiratory therapists (n 5 17) Clinicians (physicians and nurses, n 571 combined), both bedside and telepresence Pre On a five-point Likert scale, the item mean was 3.3 on the 21-item Nurse Attitudes Toward eicu. The item mean was 3.2 on the six-item Intention to Use scale. Nurses believed that TICU would benefit units without adequate physician coverage and might benefit new nurses. Nurses believed that it was unnecessary in some units, that conflicts between on- and off-site staff could undermine patient outcomes, and that it could lead to extra work and staff cuts. On a five-point Likert scale, overall satisfaction averaged 4.56 for referring physicians and 4.53 for nurses and respiratory therapists. Among aspects of TICU consultations, the physicians scored audiovisual quality lowest (mean, 4.31), and the nurses and respiratory therapists scored ease of equipment use lowest (mean, 3.59). Results were very positive on the basis of means of a five-point Likert scale: overall experience, 4.29; user satisfaction, 4.22; technical issues, 4.31; and clinical application, No significant variation over time suggested positive attitudes toward TICU from first use. Mathews et al 36 /2007 Published Case study Nurses (n 5 NR) Pre/ Prior to implementation, nurses were apprehensive and resistant, fearing repercussions from constant monitoring, increased workload, and increased nurse to patient ratios. A work team was able to decrease apprehension and increase acceptance of TICU staff. McNelis et al 26 /2008 Meeting Mora et al 37 /2007 Meeting Poropatich et al 25,45,46 /2008 Roberts and Dewoody 38 /2008 Meeting Published Physicians (n 5 NR) Staff intensivists communicated with surgical ICU staff during off hours through robot or telephone. Satisfaction with the robot (mean, 6.5) was significantly greater than satisfaction with the telephone (mean, 4.5). Residents (n 596) Of the residents with TICU experience, 82.3% believed that it improves patient care, and 73.8% believed that it improves the care they deliver to patients; 66.7% desired telemonitoring postresidency. Of events potentially benefiting from telemonitoring, ventilator management was mentioned by the most (70%), and supervision of online placement was mentioned the least (42%). Physicians (n 5 8), residents (n 5 22), nurses (n 5 45) On a 10-point scale, overall satisfaction averaged 8.5 for physicians, 8.1 for residents, and 8.3 for nurses. A majority of physicians and residents believed that the robot saved time. Measured collectively, no clinicians believed that the telephone was better than the robot or that the video or audio quality was poor. 95% believed that remote telepresence improves care. There was high satisfaction with no difference in support between types of providers. Nurses (n 5 NR) Pre/ The development of an orientation program for eicu care staff was associated with increased staff satisfaction with eicu and increased number of assistance calls and interactions with teleclinicians. (Continued) CHEST / 139 / 2 / FEBRUARY,
6 Table 1 (Continued) Study/Year Publication Status Study Method Participants Evaluation Point Summary of Findings Rogove et al 39 /2009 Meeting Siek et al 24 /2008 Meeting Case study Physicians (n 5 NR) Physicians, nurses (n 5 NR) Stafford et al 40 /2008 Published Interview Telephysicians (n 526), telenurses (n 544) Sucher et al 23 /2009 Meeting Thomas et al 41 /2007 Published Westbrook et al 22,47-49 /2008 Published Interviews, quantitative Youn 42 /2006 Published Zawada et al 21,43,50 /2009 Published Physicians, nurses (n 5 NR) Pre Physician satisfaction by was excellent. Pulmonary and critical care physicians appreciated consultations with colleagues, but the cardiovascular surgeon would not use the eicu resource. Nurses believed that the system was great and provided resources for the night shift, but they noted manipulation of physicians. Physical stress and boredom were challenges, but the telecenter fosters teamwork with a focus on improved patient care. Telestaff can become frustrated by the inability to directly intervene and by the resistance encountered from ICU staff. Calls from ICU nurses increase when (they learn) consulting physicians are on duty. 67% agreed that the robot would facilitate patient care between intensivists and bedside clinicians, and 72% agreed that the robot would assist bedside clinicians in managing emergencies. Physicians (n 5 NR) Pre/ The Safety Attitudes Questionnaire revealed that a significant increase in the mean teamwork score (from 69.7 to 78.8) and safety climate score (from 66.4 to 73.4) after TICU was implemented. Item scores also revealed a decrease in perceived interruptions, an increase in confidence that patients are adequately covered, and an increase in belief that a physician can be accessed in an emergency. Physicians (n 5 6), nurses (n 5 12), telephysicians (n 5 13) Following implementation of a virtual critical care unit in Australia, all consulting physicians reported that they were able to increase decision support to ED clinicians, and this had improved patient management. Many also noted increased workload and responsibility; 71% were satisfied with TICU design. ED physicians perceived greater support, and nurses reported increased autonomy and less stress. 65% of ED clinicians were satisfied with TICU design. The majority of all respondents reported improved interhospital relationships. Nurses (n 5 NR) Nursing satisfaction averaged 4.7 to 5.0 (on a five-point scale) for improved communication and collaboration and better patient outcomes. Physicians, nurse, telephysicians (n 5 NR) eicu 5 electronic ICU; IT 5 information technology; NR 5 not reported; TICU 5 tele-icu. Ten of 11 community hospitals responded. Using a five-point scale, 90% of hospital administrators and lead clinical staff agreed that tele-icu improved patient care, was easy to use, and should be available to every small or critical access hospital. More than 90% of telephysicians indicated that the TICU improved critical care in tertiary and community ICUs. All of them agreed better, safer care can be delivered by a telecritical care team. 284 Original Research
7 Table 2 Characteristics of TICUs Study/Year Technology Coverage Structure Berenson et al 5 /2009 Bedside Monitoring Hub and spoke (eicu) Coletti et al 30 /2008 Bedside Monitoring Hub and spoke (eicu) Crawley31 /2008 Bedside Consultation Parent and child (eicu) DiMartino et al 29 /2009 Bedside Monitoring Hub and spoke Faiz et al 32 /2006 Bedside Monitoring Hub and spoke (eicu) Grundy et al 28 /1977 Single mobile camera ICU rounds Parent and child Heath et al 33 /2009 Single mobile camera Consultation Parent and child Kowitlawakul 34 /2008 Bedside Monitoring Hub and spoke (eicu) Marcin et al 35 /2004 Single mobile camera Consultation Parent and child Marttos et al 27 /2008 Robot ICU rounds Collaborative/network Mathews et al 36 /2007 Bedside Monitoring Hub and spoke (eicu) McNelis et al 26 /2008 Robot ICU rounds Collaborative/network Mora et al 37 /2007 Bedside Monitoring Hub and spoke (eicu) Poropatich et al 25,45,46 /2008 Robot ICU rounds Collaborative/network Roberts and Dewoody 38 /2008 Bedside Monitoring Hub and spoke (eicu) Rogove et al 39 /2009 Robot Consultation Collaborative/network Siek et al 24 /2008 Bedside Monitoring Hub and spoke (eicu) Stafford et al 40 /2008 Bedside Monitoring Hub and spoke (eicu) Sucher et al 23 /2009 Robot Consultation Collaborative/network Thomas et al 41 /2007 Bedside Monitoring Hub and spoke Westbrook et al 22,47-49 /2008 Single mobile camera Consultation Parent and child Youn 42 /2006 Robot Consultation Hub and spoke Zawada et al 21,43,50 /2009 Hybrid Monitoring Hub and spoke (eicu) See Table 1 legend for expansion of abbreviations. reported that the tele-icu coverage may decrease interruptions 41 and workload. 5,25,30 Additionally, equipment shortcomings and malfunctions were reported in several studies. 5,28,31,33-35 Evaluations of Organizational Impact: Staff consistently indicated that tele-icu coverage should be tailored to the specific needs or capabilities of a particular ICU. In fact, preimplementation resistance Table 3 Summary of Acceptance and Potential Barriers Reported by Staff Evaluation Category Summary Potential Barriers Overall acceptance of staff Staff evaluation of patient care impact Staff evaluation of staff impact Staff evaluation of organizational impact See Table 1 for expansion of abbreviation. High satisfaction TICU desired by residents Anticipated enhancements to patient care Positive evaluations of patient care impact Better off-shift coverage and reductions in patient transfers Anticipated fruitful collaboration between ICU and telecenter Communication between the ICU and telecenter highly rated Better relationships in parent-child setups than in hub-and-spoke setups Enhanced autonomy Enhanced clinical training Reduced workload Coverage unnecessary in all ICUs (eg, highly effective ICUs) Needs and resources of the ICU should determine type of telecoverage TICU benefits underperforming ICUs and those with new nurses or physician gaps Leveraged intensivist services Enhanced hospital reputation Ambivalence among nurses prior to implementation Preimplementation questions about usefulness of TICU Nurse refusal to take good advice from teleclinicians Poaching of ICU clinicians in order to staff the telecenter Conflicting recommendations from ICU and teleclinicians Suspicion ICU nurses avoided or deferred consultations to receive desired advice from a preferred source Concerns that big brother was watching and scrutinizing work Increased workload, particularly when equipment malfunctions Interruptions Benefits unjustified by cost to hospital Concerns about legal liability and vulnerability CHEST / 139 / 2 / FEBRUARY,
8 often centered on concerns that the ICU was already functioning adequately and that external supervision would not be helpful. 5,31,34 Even after implementation, some ICU staff saw little need for telecoverage at hospitals with a low volume of critically ill patients, 31 although staff also recognized that tele-icu coverage might allow certain higher complexity patients to be treated locally. 21 Tele-ICU coverage also was perceived as more beneficial for ICUs with poorer baseline performance.5 Finally, ICUs with staffing challenges (eg, newly graduated nurses, gaps in physician coverage on nights and weekends) were thought to benefit more than others. 34 In interviews with hospital administrators conducted by Berenson et al, 5 three additional assessments emerged related to the tele-icu impact on the organization. The first was a negative perception that the substantial cost did not justify the potential benefits. The second was a positive perception that tele-icu coverage would leverage intensivist services, thereby enhancing patient care outside the hospital and facilitating partnerships with other hospitals and clinicians. The third was a positive perception that tele-icu coverage would enhance the reputation of the hospital. Discussion In a systematic review of staff acceptance of tele-icu coverage, we found that this technology generally was viewed favorably by physicians and nurses across an array of settings. In particular, staff generally viewed tele-icu coverage as improving ICU quality despite initial reservations regarding the implementation of these systems. Staff also expressed the strong belief that the benefit of tele-icu coverage would be greater for ICUs with specific quality issues (eg, difficulty in obtaining staffing) that could be affected. Our review also revealed important limitations in the methodologic rigor of many studies, highlighting the need for better evaluation of this costly new technology. A number of our findings merit further discussion. First, it is important to address the quality and rigor of the available data. Although we identified 23 studies meeting our inclusion criteria, only seven were peer-reviewed studies that focused primarily on staff acceptance,30,33,34,36,38,40,41 and validated instruments were used in only two studies. 34,41 This lack of rigorous data places hospital administrators and intensivists contemplating implementation of tele-icu coverage in a difficult situation. Second, our results suggest that staff acceptance of tele-icu coverage is generally high. Although staff members have appropriate concerns about the impact of this technology ahead of implementation, most studies suggest that those who have worked in an ICU with tele-monitoring view the technology favorably. Third, our review suggests that context matters. In other words, staff members seem to appreciate the fact that the benefit of tele-icu coverage depends on the baseline performance of the ICU where coverage is initiated. In particular, ICUs with poorer baseline performance or more-significant challenges might benefit more, whereas ICUs with better baseline performance might benefit less. One could argue that this assumption is intuitive, but at the present time, it is actually quite uncertain which hospitals are choosing to implement tele-icu coverage. Indeed, it is possible that ICUs with highly engaged intensivist leaders and high baseline quality may be the facilities choosing to purchase these systems. Fourth, our review highlights several specific strategies that might facilitate tele-icu acceptance by staff. ICU clinicians should participate early in the design and implementation of the tele-icu. 34 Physicians and hospital administrators should build support for tele-icu coverage among the ICU staff prior to rollout. 22,34 Clinicians from the monitoring center should visit the bedside teams in order to build trust on both sides of the camera. 29,40 Audiovisual contact with the teleconsultant is better than audio contact alone. 22,28 Hiring monitoring center physicians and nurses skilled in interpersonal communication is important for reducing the threat perceived by bedside teams. 40 The findings allow us to speculate on additional ways to facilitate integration of the tele-icu. Uncertain and conflicting treatment approaches undermine patient care, so hospital administrators must establish absolute agreement between the ICU staff and the monitoring center on best practices for operation. Procedures for physician-to-physician sign-out should be explicit so that ICU nurses know at all times the scope of the tele-icu consultants authority. Administrators should encourage nurses to identify conflicting treatment directives and provide clear instructions for resolving those conflicts for the best care of the patient. Administrators also could enhance acceptance and decrease suspicion by arranging periodic face-to-face meetings or site visits for bedside and consulting clinicians. Our review has several limitations. First, most of the included studies addressed staff acceptance only as a secondary consideration, so the level of detail reported often was deficient. Second, the heterogeneity of study designs and measures prevented us from conducting meta-analyses of the reported quantitative data. Nevertheless, the reporting of qualitative results was a strength of this review. Third, all but one study neglected to evaluate tele-icu acceptance among administrators. This omission is important because administrators were typically the ones who determined whether tele-icu coverage was purchased and implemented. Finally, acceptance by 286 Original Research
9 patients and families was not examined in the studies in this review and merits further investigation. In conclusion, we found that although tele-icu coverage was initially viewed with trepidation, after implementation, staff viewed this technology as improving ICU functioning in a number of diverse ways. This study highlights the need for careful planning and staff involvement prior to implementation of what can be viewed as a threatening and disruptive technology. Acknowledgments Author contributions: Dr Young had full access to the data and vouches for the integrity of the data analysis. Dr Young: contributed to the conduct of the literature search and the analysis and wrote the original draft of the manuscript. Dr Chan: contributed to the analysis and multiple revisions of the manuscript. Dr Cram: contributed independent evaluation of the studies, to the analysis, and to the revision of subsequent drafts of the manuscript. Financial/nonfinancial disclosures: The authors have reported to CHEST to following conflicts: Dr Cram has received grant funding from the Veterans Administration for the research presented in this article and has given talks on tele-icu but has not received or ever received funding from any corporate entities or other entities with a financial stake in tele-icu care. Drs Young and Chan report that no potential conflicts of interest exist with any companies/organizations whose products or services may be discussed in this article. Role of sponsors: The views expressed in this article are those of the authors and do not necessarily represent the views of the Department of Veterans Affairs. The funding sources had no role in the analyses or drafting of this manuscript. References 1. Pronovost PJ, Angus DC, Dorman T, Robinson KA, Dremsizov TT, Young TL. Physician staffing patterns and clinical outcomes in critically ill patients: a systematic review. JAMA ;288(17): Duke EM. Report to Congress: The Critical Care Workforce: A Study of the Supply and Demand for Critical Care Physicians. Washington, DC : US Department of Health and Human Services HRSA ; Gutsche JT, Kohl BA. Who should care for intensive care unit patients? Crit Care Med ;35(2 suppl ):S18-S National Library of Medicine. National Library of Medicine: Medical Subject Headings. Bethesda, MD : National Library of Medicine ; Berenson RA, Grossman JM, November EA. Does telemonitoring of patients the eicu improve intensive care? Health Aff (Millwood) ;28(5):w937-w Breslow MJ. Remote ICU care programs: current status. J Crit Care ;22(1): Society of Critical Care Medicine. Tele-ICU Monitoring and Care. Mount Prospect, IL : Society of Critical Care Medicine ; Thomas EJ, Lucke JF, Wueste L, Weavind L, Patel B. Association of telemedicine for remote monitoring of intensive care patients with mortality, complications, and length of stay. JAMA ;302(24): Morrison JL, Cai Q, Davis N, et al. Clinical and economic outcomes of the electronic intensive care unit: Results from two community hospitals. Crit Care Med ;38(1): Rosenfeld BA, Dorman T, Breslow MJ, et al. Intensive care unit telemedicine: alternate paradigm for providing continuous intensivist care. Crit Care Med ;28 (12 ): Kohl BA, Gutsche JT, Kim P, et al. Effect of telemedicine on mortality and length of stay in a university ICU. Crit Care Med ;35 (12 ):A Stern L. Care from afar: small hospitals use technology to run remote ICUs. Newsweek, 2007 :150 (12 ):E Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA ;283 (15 ): Centre for Reviews and Dissemination. Systematic Reviews: CRD s Guidance for Undertaking Reviews in Healthcare. York, England : CRD, University of York ; Agency for Healthcare Research and Quality. Systems To Rate the Strength of Scientific Evidence. In: Services UDoHaH. Rockville, MD : Public Health Service ; 2002 : Krippendorff K. Content Analysis: An Introduction to Its Methodology. 2nd ed. Thousand Oaks, CA : Sage ; Baxter LA, Babbie E. The Basics of Communication Research. Belmont, CA : Wadsworth ; Creswell JW. Research Design: Qualitative,, and Mixed Methods Approaches. Thousand Oaks, CA : Sage ; Tashakkori A, Teddlie C. Mixed Methodology: Combining Qualitative and Approaches. Thousand Oaks, CA : Sage ; NVivo Qualitative Data Analysis Software [computer program]. Victoria, Australia: QSR International Pty Ltd; Zawada ET Jr, Herr P, Larson D, Fromm R, Kapaska D, Erickson D. Impact of an intensive care unit telemedicine program on a rural health care system. grad Med ; 121 (3 ): Westbrook JI, Coiera EW, Brear M, et al. Impact of an ultrabroadband emergency department telemedicine system on the care of acutely ill patients and clinicians work. Med J Aust ;188 (12 ): Sucher J, Jones S, Montoya I, et al. ICU staff receptiveness to remote telepresence. Paper presented at: American Telemedicine Association Fourteenth Annual Meeting and Exposition; April 2009; Las Vegas, NV. 24. Siek T, Cox R, Schmidt J. eicu impact in a rural community hospital. Paper presented at: American Telemedicine Association Thirteenth Annual Meeting and Exposition; April 2008; Seattle, WA. 25. Poropatich RK, Barrigan C, Chung KK, et al. Deployment of a robotic tele-presence capability in the US Army. Paper presented at: American Telemedicine Association Thirteenth Annual Meeting and Exposition. April 2008; Seattle, WA. 26. McNelis J, Spector R, Kiley M, et al. Off hours remote presence technology (RPT) enhances communication between intensivists and staff. Crit Care Med ;36 (12 ):A Marttos A, Wilson K, Krauthamer S, et al. Telerounds in a trauma ICU dept. Crit Care Med ;36 (12 ):A Grundy BL, Crawford P, Jones PK, et al. Telemedicine in critical care: an experiment in health care delivery. JACEP ;6 (10 ): DiMartino J, Fortino-Mullen M, Entrikin L, et al. Bedside nurse perceptions of intensive care unit telemedicine. Crit Care Med ;37 (12 ):A Coletti C, Elliott D, Zubrow M. Resident perceptions of an integrated remote ICU monitoring system. Crit Care Med ;36 (12 ): Crawley EA. eicu impact in the military. Paper presented at: American Telemedicine Association Thirteenth Annual Meeting and Exposition; April 2008; Seattle, WA. CHEST / 139 / 2 / FEBRUARY,
10 32. Faiz SA, Zachria A, Weavind L, et al. Fellowship education in remote telemonitoring units. Chest ; 130 ( 4 suppl ): 112S-113S. 33. Heath B, Salerno R, Hopkins A, Hertzig J, Caputo M. Pediatric critical care telemedicine in rural underserved emergency departments. Pediatr Crit Care Med ;10 (5 ): Kowitlawakul Y. The Technology Acceptance Model: predicting nurses acceptance of telemedicine technology (eicu). Comput Inform Nurs. In press. doi: /ncn.0b013e3181f9dd4a. 35. Marcin JP, Nesbitt TS, Kallas HJ, Struve SN, Traugott CA, Dimand RJ. Use of telemedicine to provide pediatric critical care inpatient consultations to underserved rural Northern California. J Pediatr ;144 (3 ): Mathews S, Wood C, Kagel E. Smile you re on EICU: A collaborative critical care team to enhance patient outcomes. Crit Care Nurse ;27 (2 ): Mora A, Faiz SA, Kelly T, et al. Resident perception of the educational and patient care value from remote telemonitoring in a medical intensive care unit. Chest ;132 (4 ):443a. 38. Roberts G, Dewoody S. Lights, camera, collaboration: implementation of an eicu orientation program. Crit Care Nurse ;28 :e Rogove H, Atkins C, Kramer J, et al. Enhanced access to neurointensivists through a telemedicine program. Crit Care Med ;37 (12 suppl ):A Stafford TB, Myers MA, Young A, Foster JG, Huber JT. Working in an eicu unit: life in the box. Crit Care Nurs Clin North Am ;20 (4 ): Thomas EJ, Chu-Weininger MYL, Lucke J, et al. The impact of a tele-icu on provider attitudes about teamwork and safety climate. Crit Care Med ;35 (12 suppl ):A Youn BA. Utilizing robots and an ICU telemedicine program to provide intensivist support for rapid response teams. Chest ;130 (Suppl ):102S. 43. Zawada ET, Herr P. ICU telemedicine improves care to rural hospitals reducing costly transports. Crit Care Med ;36 (4 ): Grundy BL, Jones PK, Lovitt A. Telemedicine in critical care: problems in design, implementation, and assessment. Crit Care Med ;10 (7 ): Chung KK, Grathwohl KW, Poropatich RK, et al. Bedside nurse perceptions of intensive care unit telemedicine. Crit Care Med ;37 (12 ):A Chung KK, Grathwohl KW, Poropatich RK, Wolf SE, Holcomb JB. Robotic telepresence: past, present, and future. J Cardiothorac Vasc Anesth ;21 (4 ): Murphy M, Stapleton S, Cregan P, et al. Using remote critical care units in Australia. Paper presented at: American Telemedicine Association Twelfth Annual Meeting and Tradeshow; May 2007; Nashville, TN. 48. Wilson L, Hansen SK, Li J, et al. A broadband telemedicine application for critical care in Australia. Paper presented at: American Telemedicine Association Twelfth Annual Meeting and Tradeshow; May 2007; Nashville, TN. 49. Wilson L, Hansen SK, Skinner MW. Design and evaluation of a broadband telemedicine system for supporting ICUs in regional hospitals. Paper presented at: American Telemedicine Association Thirteenth Annual Meeting and Exposition; April 2008; Seattle, WA. 50. Herr P. eicu impact in a rural health system. Paper presented at: American Telemedicine Association Thirteenth Annual Meeting and Exposition; April 2008; Seattle, WA. 288 Original Research
TeleICU And What It Means To You
 Vanderbilt Department of Anesthesiology TeleICU And What It Means To You Dr. L. Weavind MBBCh Associate Professor Anesthesia and Surgery Director Critical Care Fellowship Vanderbilt University Former Director
Vanderbilt Department of Anesthesiology TeleICU And What It Means To You Dr. L. Weavind MBBCh Associate Professor Anesthesia and Surgery Director Critical Care Fellowship Vanderbilt University Former Director
Quality health care in intensive
 Clinical outcomes after telemedicine intensive care unit implementation* Beth Willmitch, RN, BSN; Susan Golembeski, PhD, RN, CHRC; Sandy S. Kim, MA, MEd; Loren D. Nelson, MD, FACS, FCCM; Louis Gidel, MD,
Clinical outcomes after telemedicine intensive care unit implementation* Beth Willmitch, RN, BSN; Susan Golembeski, PhD, RN, CHRC; Sandy S. Kim, MA, MEd; Loren D. Nelson, MD, FACS, FCCM; Louis Gidel, MD,
2017 LEAPFROG TOP HOSPITALS
 2017 LEAPFROG TOP HOSPITALS METHODOLOGY AND DESCRIPTION In order to compare hospitals to their peers, Leapfrog first placed each reporting hospital in one of the following categories: Children s, Rural,
2017 LEAPFROG TOP HOSPITALS METHODOLOGY AND DESCRIPTION In order to compare hospitals to their peers, Leapfrog first placed each reporting hospital in one of the following categories: Children s, Rural,
The Costs of Critical Care Telemedicine Programs. A Systematic Review and Analysis
 CHEST Original Research The Costs of Critical Care Telemedicine Programs A Systematic Review and Analysis Gaurav Kumar, MD ; Derik M. Falk, MD ; Robert S. Bonello, MD ; Jeremy M. Kahn, MD ; Eli Perencevich,
CHEST Original Research The Costs of Critical Care Telemedicine Programs A Systematic Review and Analysis Gaurav Kumar, MD ; Derik M. Falk, MD ; Robert S. Bonello, MD ; Jeremy M. Kahn, MD ; Eli Perencevich,
ORGANIZATIONAL AND TEAMWORK FACTORS OF TELE INTENSIVE CARE UNITS. Critical Care Management
 Critical Care Management ORGANIZATIONAL AND TEAMWORK FACTORS OF TELE INTENSIVE CARE UNITS By Michael S. Wilkes, MD, MPH, PhD, James P. Marcin, MD, MPH, Lois A. Ritter, EdD, and Sherilyn Pruitt, MPH 06
Critical Care Management ORGANIZATIONAL AND TEAMWORK FACTORS OF TELE INTENSIVE CARE UNITS By Michael S. Wilkes, MD, MPH, PhD, James P. Marcin, MD, MPH, Lois A. Ritter, EdD, and Sherilyn Pruitt, MPH 06
Assessing competence during professional experience placements for undergraduate nursing students: a systematic review
 University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2012 Assessing competence during professional experience placements for
University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2012 Assessing competence during professional experience placements for
PG snapshot Nursing Special Report. The Role of Workplace Safety and Surveillance Capacity in Driving Nurse and Patient Outcomes
 PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
PG snapshot news, views & ideas from the leader in healthcare experience & satisfaction measurement The Press Ganey snapshot is a monthly electronic bulletin freely available to all those involved or interested
Neurocritical Care Fellowship Program Requirements
 Neurocritical Care Fellowship Program Requirements I. Introduction A. Definition The medical subspecialty of Neurocritical Care is devoted to the comprehensive, multisystem care of the critically-ill neurological
Neurocritical Care Fellowship Program Requirements I. Introduction A. Definition The medical subspecialty of Neurocritical Care is devoted to the comprehensive, multisystem care of the critically-ill neurological
National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI)
 October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
The impact of nighttime intensivists on medical intensive care unit infection-related indicators
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 The impact of nighttime intensivists on medical intensive care unit infection-related indicators Abhaya Trivedi
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 The impact of nighttime intensivists on medical intensive care unit infection-related indicators Abhaya Trivedi
Wired to Save Lives: A Virtual Hospital Experience
 Wired to Save Lives: A Virtual Hospital Experience Donald J. Kosiak, MD, MBA, FACEP, CPE Vice President for Medical Development Thursday, March 3 rd -- 11:30am Conflict of Interest Donald Kosiak, MD Has
Wired to Save Lives: A Virtual Hospital Experience Donald J. Kosiak, MD, MBA, FACEP, CPE Vice President for Medical Development Thursday, March 3 rd -- 11:30am Conflict of Interest Donald Kosiak, MD Has
Emergency admissions to hospital: managing the demand
 Report by the Comptroller and Auditor General Department of Health Emergency admissions to hospital: managing the demand HC 739 SESSION 2013-14 31 OCTOBER 2013 4 Key facts Emergency admissions to hospital:
Report by the Comptroller and Auditor General Department of Health Emergency admissions to hospital: managing the demand HC 739 SESSION 2013-14 31 OCTOBER 2013 4 Key facts Emergency admissions to hospital:
Telemedicine Enhances Communication in the Intensive Care Unit
 University of Vermont ScholarWorks @ UVM Graduate College Dissertations and Theses Dissertations and Theses 2016 Telemedicine Enhances Communication in the Intensive Care Unit Prema Ramachandran Menon
University of Vermont ScholarWorks @ UVM Graduate College Dissertations and Theses Dissertations and Theses 2016 Telemedicine Enhances Communication in the Intensive Care Unit Prema Ramachandran Menon
MUSC Critical Care Outreach Program. Dee W. Ford, MD, MSCR Associate Professor of Medicine
 MUSC Critical Care Outreach Program Dee W. Ford, MD, MSCR Associate Professor of Medicine Disclosures * Funding from the NIH, Department of Defense, and the National Palliative Care Research Center * No
MUSC Critical Care Outreach Program Dee W. Ford, MD, MSCR Associate Professor of Medicine Disclosures * Funding from the NIH, Department of Defense, and the National Palliative Care Research Center * No
JULY 2012 RE-IMAGINING CARE DELIVERY: PUSHING THE BOUNDARIES OF THE HOSPITALIST MODEL IN THE INPATIENT SETTING
 JULY 2012 RE-IMAGINING CARE DELIVERY: PUSHING THE BOUNDARIES OF THE HOSPITALIST MODEL IN THE INPATIENT SETTING About The Chartis Group The Chartis Group is an advisory services firm that provides management
JULY 2012 RE-IMAGINING CARE DELIVERY: PUSHING THE BOUNDARIES OF THE HOSPITALIST MODEL IN THE INPATIENT SETTING About The Chartis Group The Chartis Group is an advisory services firm that provides management
The Nature of Emergency Medicine
 Chapter 1 The Nature of Emergency Medicine In This Chapter The ED Laboratory The Patient The Illness The Unique Clinical Work Sense Making Versus Diagnosing The ED Environment The Role of Executive Leadership
Chapter 1 The Nature of Emergency Medicine In This Chapter The ED Laboratory The Patient The Illness The Unique Clinical Work Sense Making Versus Diagnosing The ED Environment The Role of Executive Leadership
Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care
 Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care April 29, 2011 Waltham, MA Presented by Lisa Payne Simon, MPH Cheryl H. Dunnington, RN, MS 1 FAST Initiative Overview 2004-2010
Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care April 29, 2011 Waltham, MA Presented by Lisa Payne Simon, MPH Cheryl H. Dunnington, RN, MS 1 FAST Initiative Overview 2004-2010
Improving Hospital Performance Through Clinical Integration
 white paper Improving Hospital Performance Through Clinical Integration Rohit Uppal, MD President of Acute Hospital Medicine, TeamHealth In the typical hospital, most clinical service lines operate as
white paper Improving Hospital Performance Through Clinical Integration Rohit Uppal, MD President of Acute Hospital Medicine, TeamHealth In the typical hospital, most clinical service lines operate as
Does Robotic Telerounding Enhance Nurse Physician Collaboration Satisfaction About Care Decisions?
 Does Robotic Telerounding Enhance Nurse Physician Collaboration Satisfaction About Care Decisions? Michele Bettinelli, RN, 1 Yuxiu Lei, PhD, 2 Matt Beane, MS, 3 Caleb Mackey, MD, 4 and Timothy N. Liesching,
Does Robotic Telerounding Enhance Nurse Physician Collaboration Satisfaction About Care Decisions? Michele Bettinelli, RN, 1 Yuxiu Lei, PhD, 2 Matt Beane, MS, 3 Caleb Mackey, MD, 4 and Timothy N. Liesching,
Lakota Health System: eicu Pilot for Pine Ridge Indian Health Services Hospital
 Lakota Health System: eicu Pilot for Pine Ridge Indian Health Services Hospital MMI 404 Health Enterprise Operations Group 1 Rhona Banayat Ralph Garcia Nicole Hawkins Mike Nowak November 20, 2011 Presentation
Lakota Health System: eicu Pilot for Pine Ridge Indian Health Services Hospital MMI 404 Health Enterprise Operations Group 1 Rhona Banayat Ralph Garcia Nicole Hawkins Mike Nowak November 20, 2011 Presentation
"Nurse Staffing" Introduction Nurse Staffing and Patient Outcomes
 "Nurse Staffing" A Position Statement of the Virginia Hospital and Healthcare Association, Virginia Nurses Association and Virginia Organization of Nurse Executives Introduction The profession of nursing
"Nurse Staffing" A Position Statement of the Virginia Hospital and Healthcare Association, Virginia Nurses Association and Virginia Organization of Nurse Executives Introduction The profession of nursing
Nursing skill mix and staffing levels for safe patient care
 EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
EVIDENCE SERVICE Providing the best available knowledge about effective care Nursing skill mix and staffing levels for safe patient care RAPID APPRAISAL OF EVIDENCE, 19 March 2015 (Style 2, v1.0) Contents
Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence
 CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
CADTH RAPID RESPONSE REPORT: SUMMARY WITH CRITICAL APPRAISAL Disposable, Non-Sterile Gloves for Minor Surgical Procedures: A Review of Clinical Evidence Service Line: Rapid Response Service Version: 1.0
BEDSIDE NURSES PERCEPTIONS OF INTENSIVE CARE UNIT TELEMEDICINE. Innovative Approaches. 1.0 Hour
 Innovative Approaches BEDSIDE NURSES PERCEPTIONS OF INTENSIVE CARE UNIT TELEMEDICINE By Margaret Mullen-Fortino, RN, MSN, Joseph DiMartino, RN, MSN, Lorraine Entrikin, RN, BSN, Sophia Mulliner, RN, BSN,
Innovative Approaches BEDSIDE NURSES PERCEPTIONS OF INTENSIVE CARE UNIT TELEMEDICINE By Margaret Mullen-Fortino, RN, MSN, Joseph DiMartino, RN, MSN, Lorraine Entrikin, RN, BSN, Sophia Mulliner, RN, BSN,
How Allina Saved $13 Million By Optimizing Length of Stay
 Success Story How Allina Saved $13 Million By Optimizing Length of Stay EXECUTIVE SUMMARY Like most large healthcare systems throughout the country, Allina Health s financial health improves dramatically
Success Story How Allina Saved $13 Million By Optimizing Length of Stay EXECUTIVE SUMMARY Like most large healthcare systems throughout the country, Allina Health s financial health improves dramatically
THE NEED FOR CLEAR team communication
 QUALITY CORNER Improving Communication in the ICU Using Daily Goals Peter Pronovost, Sean Berenholtz, Todd Dorman, Pam A. Lipsett, Terri Simmonds, and Carol Haraden OBJECTIVES The specific aims of this
QUALITY CORNER Improving Communication in the ICU Using Daily Goals Peter Pronovost, Sean Berenholtz, Todd Dorman, Pam A. Lipsett, Terri Simmonds, and Carol Haraden OBJECTIVES The specific aims of this
Exploring Socio-Technical Insights for Safe Nursing Handover
 Context Sensitive Health Informatics: Redesigning Healthcare Work C. Nøhr et al. (Eds.) 2017 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under
Context Sensitive Health Informatics: Redesigning Healthcare Work C. Nøhr et al. (Eds.) 2017 The authors and IOS Press. This article is published online with Open Access by IOS Press and distributed under
Version 1.0 (posted Aug ) Aaron L. Leppin. Background. Introduction
 Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
Describing the usefulness and efficacy of discharge interventions: predicting 30 day readmissions through application of the cumulative complexity model (protocol). Version 1.0 (posted Aug 22 2013) Aaron
Exploring the Impact of Medicaid Expansion on West Virginia s Primary Care System
 Exploring the Impact of Medicaid Expansion on West Virginia s Primary Care System Jessica L. Thayer, BA Medical Student West Virginia University School of Medicine Thomas K. Bias, PhD* Assistant Professor
Exploring the Impact of Medicaid Expansion on West Virginia s Primary Care System Jessica L. Thayer, BA Medical Student West Virginia University School of Medicine Thomas K. Bias, PhD* Assistant Professor
Student-Led Clinics: Building Placement Capacity and Filling Service Gaps
 Student-Led Clinics: Building Placement Capacity and Filling Service Gaps MADELYN NICOLE MICHELE FAIRBROTHER SRIVALLI VILAPAKKAM NAGARAJAN JULIA BLACKFORD LINDY MCALLISTER University of Sydney, Sydney,
Student-Led Clinics: Building Placement Capacity and Filling Service Gaps MADELYN NICOLE MICHELE FAIRBROTHER SRIVALLI VILAPAKKAM NAGARAJAN JULIA BLACKFORD LINDY MCALLISTER University of Sydney, Sydney,
Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010)
 Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010) Completed November 30, 2010 Ryan Spaulding, PhD Director Gordon Alloway Research Associate Center for
Medicaid HCBS/FE Home Telehealth Pilot Final Report for Study Years 1-3 (September 2007 June 2010) Completed November 30, 2010 Ryan Spaulding, PhD Director Gordon Alloway Research Associate Center for
Keep watch and intervene early
 IntelliVue GuardianSoftware solution Keep watch and intervene early The earlier, the better Intervene early, by recognizing subtle signs Clinical realities on the general floor and in the emergency department
IntelliVue GuardianSoftware solution Keep watch and intervene early The earlier, the better Intervene early, by recognizing subtle signs Clinical realities on the general floor and in the emergency department
Impact of Financial and Operational Interventions Funded by the Flex Program
 Impact of Financial and Operational Interventions Funded by the Flex Program KEY FINDINGS Flex Monitoring Team Policy Brief #41 Rebecca Garr Whitaker, MSPH; George H. Pink, PhD; G. Mark Holmes, PhD University
Impact of Financial and Operational Interventions Funded by the Flex Program KEY FINDINGS Flex Monitoring Team Policy Brief #41 Rebecca Garr Whitaker, MSPH; George H. Pink, PhD; G. Mark Holmes, PhD University
Asking Questions: Information Needs in a Surgical Intensive Care Unit
 Asking Questions: Information Needs in a Surgical Intensive Care Unit Madhu C. Reddy M.S. 1, Wanda Pratt Ph.D. 2, Paul Dourish Ph.D. 1, M. Michael Shabot M.D. 3 2 1 Information and Computer Science Department,
Asking Questions: Information Needs in a Surgical Intensive Care Unit Madhu C. Reddy M.S. 1, Wanda Pratt Ph.D. 2, Paul Dourish Ph.D. 1, M. Michael Shabot M.D. 3 2 1 Information and Computer Science Department,
More than 60% of elective surgery
 Benefits of Preoperative Education for Adult Elective Surgery Patients NANCY KRUZIK, MSN, RN, CNOR More than 60% of elective surgery procedures in the United States were being performed as outpatient procedures
Benefits of Preoperative Education for Adult Elective Surgery Patients NANCY KRUZIK, MSN, RN, CNOR More than 60% of elective surgery procedures in the United States were being performed as outpatient procedures
WHITE PAPER #2: CASE STUDY ON FRONTIER TELEHEALTH
 WHITE PAPER #2: CASE STUDY ON FRONTIER TELEHEALTH I. CURRENT LEGISLATION AND REGULATIONS Telehealth technology has the potential to improve access to a broader range of health care services in rural and
WHITE PAPER #2: CASE STUDY ON FRONTIER TELEHEALTH I. CURRENT LEGISLATION AND REGULATIONS Telehealth technology has the potential to improve access to a broader range of health care services in rural and
Improving medical handover at the weekend: a quality improvement project
 BMJ Quality Improvement Reports 2015; u207153.w2899 doi: 10.1136/bmjquality.u207153.w2899 Improving medical handover at the weekend: a quality improvement project Emma Michael, Chandni Patel Broomfield
BMJ Quality Improvement Reports 2015; u207153.w2899 doi: 10.1136/bmjquality.u207153.w2899 Improving medical handover at the weekend: a quality improvement project Emma Michael, Chandni Patel Broomfield
Essential Skills for Evidence-based Practice: Strength of Evidence
 Essential Skills for Evidence-based Practice: Strength of Evidence Jeanne Grace Corresponding Author: J. Grace E-mail: Jeanne_Grace@urmc.rochester.edu Jeanne Grace RN PhD Emeritus Clinical Professor of
Essential Skills for Evidence-based Practice: Strength of Evidence Jeanne Grace Corresponding Author: J. Grace E-mail: Jeanne_Grace@urmc.rochester.edu Jeanne Grace RN PhD Emeritus Clinical Professor of
ORIGINAL RESEARCH ABSTRACT
 ORIGINAL RESEARCH Assessing call demand and utilization of a secondary triage emergency communication nurse system for low acuity calls transferred from an emergency dispatch system Mark Conrad Fivaz,
ORIGINAL RESEARCH Assessing call demand and utilization of a secondary triage emergency communication nurse system for low acuity calls transferred from an emergency dispatch system Mark Conrad Fivaz,
TELEHEALTH FOR HEALTH SYSTEMS: GUIDE TO BEST PRACTICES
 TELEHEALTH FOR HEALTH SYSTEMS: GUIDE TO BEST PRACTICES Overview Telemedicine delivers care that s convenient and cost effective letting physicians and patients avoid unnecessary travel and wait time. Health
TELEHEALTH FOR HEALTH SYSTEMS: GUIDE TO BEST PRACTICES Overview Telemedicine delivers care that s convenient and cost effective letting physicians and patients avoid unnecessary travel and wait time. Health
The Role of Health Information Technology on Critical Care Services in Thailand
 Special Article The Role of Health Information Technology on Critical Care Services in Thailand Petch Wacharasint MD* * Department of Anesthesiology, Phramongkutklao Hospital, Bangkok, Thailand Health
Special Article The Role of Health Information Technology on Critical Care Services in Thailand Petch Wacharasint MD* * Department of Anesthesiology, Phramongkutklao Hospital, Bangkok, Thailand Health
MEDICAL POLICY No R2 TELEMEDICINE
 Summary of Changes Clarifications: Page 1, Section I. A 6, additional language added for clarification. Deletions: Additions Page 4, Section IV, Description, additional language added in regards to telemedicine.
Summary of Changes Clarifications: Page 1, Section I. A 6, additional language added for clarification. Deletions: Additions Page 4, Section IV, Description, additional language added in regards to telemedicine.
Postacute care (PAC) cost variation explains a large part
 INNOVATIVE GERIATRIC PRACTICE MODELS: PRELIMINARY DATA Creating a Network of High-Quality Skilled Nursing Facilities: Preliminary Data on the Postacute Care Quality Improvement Experiences of an Accountable
INNOVATIVE GERIATRIC PRACTICE MODELS: PRELIMINARY DATA Creating a Network of High-Quality Skilled Nursing Facilities: Preliminary Data on the Postacute Care Quality Improvement Experiences of an Accountable
Reviewing Telemetry Monitoring Practices at Mount Saint Joseph Hospital
 Reviewing Telemetry Monitoring Practices at Mount Saint Joseph Hospital Jennifer Beer, Mihaela Rozor, Ngai In (Ginny) Ho The purpose of this study is to examine the current telemetry monitoring practices
Reviewing Telemetry Monitoring Practices at Mount Saint Joseph Hospital Jennifer Beer, Mihaela Rozor, Ngai In (Ginny) Ho The purpose of this study is to examine the current telemetry monitoring practices
A systematic review of the literature: executive summary
 A systematic review of the literature: executive summary October 2008 The effectiveness of interventions for reducing ambulatory sensitive hospitalisations: a systematic review Arindam Basu David Brinson
A systematic review of the literature: executive summary October 2008 The effectiveness of interventions for reducing ambulatory sensitive hospitalisations: a systematic review Arindam Basu David Brinson
CHSD. Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary. Centre for Health Service Development
 CHSD Centre for Health Service Development Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary Centre for Health Service Development UNIVERSITY OF WOLLONGONG April,
CHSD Centre for Health Service Development Encouraging Best Practice in Residential Aged Care Program: Evaluation Framework Summary Centre for Health Service Development UNIVERSITY OF WOLLONGONG April,
Clinical and Financial Successes at Advocate Health Care Utilizing our
 Clinical and Financial Successes at Advocate Health Care Utilizing our Tele-ICU Program June 2, 2016 Cindy Welsh, RN, MBA, FACHE VP for Critical Care and Medical Professional Affairs Advocate Health Care
Clinical and Financial Successes at Advocate Health Care Utilizing our Tele-ICU Program June 2, 2016 Cindy Welsh, RN, MBA, FACHE VP for Critical Care and Medical Professional Affairs Advocate Health Care
The Role of the Hospice Medical Director as Observed in Interdisciplinary Team Case Reviews
 JOURNAL OF PALLIATIVE MEDICINE Volume 13, Number 3, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=jpm.2009.0247 The Role of the Hospice Medical Director as Observed in Interdisciplinary Team Case Reviews
JOURNAL OF PALLIATIVE MEDICINE Volume 13, Number 3, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=jpm.2009.0247 The Role of the Hospice Medical Director as Observed in Interdisciplinary Team Case Reviews
Improving the patient experience through nurse leader rounds
 Patient Experience Journal Volume 1 Issue 2 Article 10 2014 Improving the patient experience through nurse leader rounds Judy C. Morton Providence Health & Services, Judy.morton@providence.org Jodi Brekhus
Patient Experience Journal Volume 1 Issue 2 Article 10 2014 Improving the patient experience through nurse leader rounds Judy C. Morton Providence Health & Services, Judy.morton@providence.org Jodi Brekhus
A Business Case for Tele-Intensive Care Units
 Marshall University Marshall Digital Scholar Management Faculty Research Management, Marketing and MIS Fall 2014 Alberto Coustasse Marshall University, coustassehen@marshall.edu Stacie Deslich Deanna Bailey
Marshall University Marshall Digital Scholar Management Faculty Research Management, Marketing and MIS Fall 2014 Alberto Coustasse Marshall University, coustassehen@marshall.edu Stacie Deslich Deanna Bailey
Integrated Leadership for Hospitals and Health Systems: Principles for Success
 Integrated Leadership for Hospitals and Health Systems: Principles for Success In the current healthcare environment, there are many forces, both internal and external, that require some physicians and
Integrated Leadership for Hospitals and Health Systems: Principles for Success In the current healthcare environment, there are many forces, both internal and external, that require some physicians and
NHS 111: London Winter Pilots Evaluation. Executive Summary
 NHS 111: London Winter Pilots Evaluation Qualitative research exploring staff experiences of using and delivering new programmes in NHS 111 Executive Summary A report prepared for Healthy London Partnership
NHS 111: London Winter Pilots Evaluation Qualitative research exploring staff experiences of using and delivering new programmes in NHS 111 Executive Summary A report prepared for Healthy London Partnership
Georgia Regents University: Evolution of One of the Country s Longest-Running Telestroke Programs
 Telemedicine Case Study Georgia Regents University: Evolution of One of the Country s Longest-Running Telestroke Programs Successes and Future Plans Each year, close to 800,000 people in the U.S. suffer
Telemedicine Case Study Georgia Regents University: Evolution of One of the Country s Longest-Running Telestroke Programs Successes and Future Plans Each year, close to 800,000 people in the U.S. suffer
Final Report ALL IRELAND. Palliative Care Senior Nurses Network
 Final Report ALL IRELAND Palliative Care Senior Nurses Network May 2016 FINAL REPORT Phase II All Ireland Palliative Care Senior Nurse Network Nursing Leadership Impacting Policy and Practice 1 Rationale
Final Report ALL IRELAND Palliative Care Senior Nurses Network May 2016 FINAL REPORT Phase II All Ireland Palliative Care Senior Nurse Network Nursing Leadership Impacting Policy and Practice 1 Rationale
Patient Safety: 10 Years Later Why is Improvement So Hard? Patient Safety: Strong Beginnings
 Patient Safety: 10 Years Later Why is Improvement So Hard? G. Ross Baker, Ph.D. Institute of Health Policy, Management & Evaluation University of Toronto 3 November 2014 Patient Safety: Strong Beginnings
Patient Safety: 10 Years Later Why is Improvement So Hard? G. Ross Baker, Ph.D. Institute of Health Policy, Management & Evaluation University of Toronto 3 November 2014 Patient Safety: Strong Beginnings
Evidence-Informed ICU Rounds. Critical Care Canada Forum October 26, 2015
 Evidence-Informed ICU Rounds Critical Care Canada Forum October 26, 2015 No disclosures or conflicts of interest Many acknowledgements Objectives 1. Summarize why we round 2. Describe current rounding
Evidence-Informed ICU Rounds Critical Care Canada Forum October 26, 2015 No disclosures or conflicts of interest Many acknowledgements Objectives 1. Summarize why we round 2. Describe current rounding
Data, analysis and evidence
 1 New Congenital Heart Disease Review Data, analysis and evidence Joanna Glenwright 2 New Congenital Heart Disease Review Evidence for standards Joanna Glenwright Evidence to inform the service standards
1 New Congenital Heart Disease Review Data, analysis and evidence Joanna Glenwright 2 New Congenital Heart Disease Review Evidence for standards Joanna Glenwright Evidence to inform the service standards
Getting the right case in the right room at the right time is the goal for every
 OR throughput Are your operating rooms efficient? Getting the right case in the right room at the right time is the goal for every OR director. Often, though, defining how well the OR suite runs depends
OR throughput Are your operating rooms efficient? Getting the right case in the right room at the right time is the goal for every OR director. Often, though, defining how well the OR suite runs depends
Telemedicine and Business Efficiency: Improving Patient Outcomes. White Paper April 2011
 Telemedicine and Business Efficiency: Improving Patient Outcomes White Paper April 2011 Clinicians, Business Efficiency and Patient Outcomes As a healthcare professional, you must efficiently and consistently
Telemedicine and Business Efficiency: Improving Patient Outcomes White Paper April 2011 Clinicians, Business Efficiency and Patient Outcomes As a healthcare professional, you must efficiently and consistently
Clinical and Financial Evidence for Improving Quality and Efficiency in the ICU
 Clinical and Financial Evidence for Improving Quality and Efficiency in the ICU eicu is a registered trademark of Philips VISICU. All rights reserved. All other brand names, product names, company names,
Clinical and Financial Evidence for Improving Quality and Efficiency in the ICU eicu is a registered trademark of Philips VISICU. All rights reserved. All other brand names, product names, company names,
Institute of Medicine Standards for Systematic Reviews
 Institute of Medicine Standards for Systematic Reviews Christopher H Schmid Tufts University ILSI 23 January 2012 Phoenix, AZ Disclosures Member of Tufts Evidence-Based Practice Center Member, External
Institute of Medicine Standards for Systematic Reviews Christopher H Schmid Tufts University ILSI 23 January 2012 Phoenix, AZ Disclosures Member of Tufts Evidence-Based Practice Center Member, External
RURAL TRAUMA. Bianchi JD, Collin GR. Management of splenic trauma at a rural, level I trauma center. The American Surgeon 1997;63(6):
 RURAL TRAUMA Bianchi JD, Collin GR. Management of splenic trauma at a rural, level I trauma center. The American Surgeon 1997;63(6):490-495. The purpose of this project was to examine the operative and
RURAL TRAUMA Bianchi JD, Collin GR. Management of splenic trauma at a rural, level I trauma center. The American Surgeon 1997;63(6):490-495. The purpose of this project was to examine the operative and
Preventing In-Facility Falls
 Preventing In-Facility Falls Presented by Paul Shekelle, M.D., Ph.D. RAND Corporation Evidence-based Practice Center Introduction: Making Health Care Safer II: An Updated Critical Analysis of the Evidence
Preventing In-Facility Falls Presented by Paul Shekelle, M.D., Ph.D. RAND Corporation Evidence-based Practice Center Introduction: Making Health Care Safer II: An Updated Critical Analysis of the Evidence
Assessing and Increasing Readiness for Patient-Centered Medical Home Implementation 1
 EVALUATION Assessing and Increasing Readiness for Patient-Centered Medical Home Implementation 1 Research Summary No. 9 March 2012 Introduction The current model of primary care in the United States is
EVALUATION Assessing and Increasing Readiness for Patient-Centered Medical Home Implementation 1 Research Summary No. 9 March 2012 Introduction The current model of primary care in the United States is
5/9/2015. Disclosures. Improving ICU outcomes and cost-effectiveness. Targets for improvement. A brief overview: ICU care in the United States
 Disclosures Improving ICU outcomes and cost-effectiveness CHQI grant, UC Health Travel support, Moore Foundation J. Matthew Aldrich, MD Associate Clinical Professor Interim Director, Critical Care Medicine
Disclosures Improving ICU outcomes and cost-effectiveness CHQI grant, UC Health Travel support, Moore Foundation J. Matthew Aldrich, MD Associate Clinical Professor Interim Director, Critical Care Medicine
Clinical and Financial Successes at Advocate Health Care Utilizing our Tele-ICU Program
 Clinical and Financial Successes at Advocate Health Care Utilizing our Tele-ICU Program April 30, 2016 Michael Ries, MD, MBA, FCCM, FCCP, FACP Medical Director Adult Critical Care and eicu Advocate Health
Clinical and Financial Successes at Advocate Health Care Utilizing our Tele-ICU Program April 30, 2016 Michael Ries, MD, MBA, FCCM, FCCP, FACP Medical Director Adult Critical Care and eicu Advocate Health
Comparison of ACP Policy and IOM Report Graduate Medical Education That Meets the Nation's Health Needs
 IOM Recommendation Recommendation 1: Maintain Medicare graduate medical education (GME) support at the current aggregate amount (i.e., the total of indirect medical education and direct graduate medical
IOM Recommendation Recommendation 1: Maintain Medicare graduate medical education (GME) support at the current aggregate amount (i.e., the total of indirect medical education and direct graduate medical
A Publication for Hospital and Health System Professionals
 A Publication for Hospital and Health System Professionals S U M M E R 2 0 0 8 V O L U M E 6, I S S U E 2 Data for Healthcare Improvement Developing and Applying Avoidable Delay Tracking Working with Difficult
A Publication for Hospital and Health System Professionals S U M M E R 2 0 0 8 V O L U M E 6, I S S U E 2 Data for Healthcare Improvement Developing and Applying Avoidable Delay Tracking Working with Difficult
Outcome data and quality: The critical role of policy
 1 of 6 3/07/2008 11:44 AM HIMJ: Reviewed articles HIMJ HOME Outcome data and quality: The critical role of policy Russell Renhard CONTENTS GUIDELINES MISSION CONTACT US HIMAA Locked Bag 2045 North Ryde,
1 of 6 3/07/2008 11:44 AM HIMJ: Reviewed articles HIMJ HOME Outcome data and quality: The critical role of policy Russell Renhard CONTENTS GUIDELINES MISSION CONTACT US HIMAA Locked Bag 2045 North Ryde,
SC Telehealth All 2017
 SC Telehealth Alliance QUARTERLY REPORT 2017 QUARTER THREE PAGE 1 Executive Summary In the third quarter of 2017, the South Carolina Telehealth Alliance (SCTA) continued its work executing the tactics
SC Telehealth Alliance QUARTERLY REPORT 2017 QUARTER THREE PAGE 1 Executive Summary In the third quarter of 2017, the South Carolina Telehealth Alliance (SCTA) continued its work executing the tactics
FULL TEAM AHEAD: UNDERSTANDING THE UK NON-SURGICAL CANCER TREATMENTS WORKFORCE
 FULL TEAM AHEAD: UNDERSTANDING THE UK NON-SURGICAL CANCER TREATMENTS WORKFORCE DECEMBER 2017 Publication date 04/12/17 Registered Charity in England and Wales (1089464), Scotland (SC041666) and the Isle
FULL TEAM AHEAD: UNDERSTANDING THE UK NON-SURGICAL CANCER TREATMENTS WORKFORCE DECEMBER 2017 Publication date 04/12/17 Registered Charity in England and Wales (1089464), Scotland (SC041666) and the Isle
AETNA FOUNDATION AETNA 2001 QUALITY CARE RESEARCH FUND EXECUTIVE SUMMARY
 Department of Family Medicine AETNA FOUNDATION AETNA 2001 QUALITY CARE RESEARCH FUND EXECUTIVE SUMMARY Project Title: "Assessing the Impact of Cultural Competency Training Using Participatory Quality Improvement
Department of Family Medicine AETNA FOUNDATION AETNA 2001 QUALITY CARE RESEARCH FUND EXECUTIVE SUMMARY Project Title: "Assessing the Impact of Cultural Competency Training Using Participatory Quality Improvement
Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC
 Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC Objectives History of the RRT/ERT teams National Statistics Criteria of activating
Rapid Response Team and Patient Safety Terrence Shenfield BS, RRT-RPFT-NPS Education Coordinator A & T respiratory Lectures LLC Objectives History of the RRT/ERT teams National Statistics Criteria of activating
The PCT Guide to Applying the 10 High Impact Changes
 The PCT Guide to Applying the 10 High Impact Changes This Guide has been produced by the NHS Modernisation Agency. For further information on the Agency or the 10 High Impact Changes please visit www.modern.nhs.uk
The PCT Guide to Applying the 10 High Impact Changes This Guide has been produced by the NHS Modernisation Agency. For further information on the Agency or the 10 High Impact Changes please visit www.modern.nhs.uk
Older people and human rights in home care: Local authority responses to the Close to home inquiry report
 Equality and Human Rights Commission Research report 89 Older people and human rights in home care: Local authority responses to the Close to home inquiry report Lorna Adams, Christoph Koerbitz, Liz Murphy
Equality and Human Rights Commission Research report 89 Older people and human rights in home care: Local authority responses to the Close to home inquiry report Lorna Adams, Christoph Koerbitz, Liz Murphy
Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W
 Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W Record Status This is a critical abstract of an economic evaluation
Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W Record Status This is a critical abstract of an economic evaluation
Telehealth Integration at Baptist Health South Florida
 Telehealth Integration at Baptist Health South Florida Philip Ludwig, MS, MBA Vice President, Operations Baptist Health South Florida Not-for-profit, community health system 7 acute adult care hospitals
Telehealth Integration at Baptist Health South Florida Philip Ludwig, MS, MBA Vice President, Operations Baptist Health South Florida Not-for-profit, community health system 7 acute adult care hospitals
Cardiovascular Disease Prevention and Control: Interventions Engaging Community Health Workers
 Cardiovascular Disease Prevention and Control: Interventions Engaging Community Health Workers Community Preventive Services Task Force Finding and Rationale Statement Ratified March 2015 Table of Contents
Cardiovascular Disease Prevention and Control: Interventions Engaging Community Health Workers Community Preventive Services Task Force Finding and Rationale Statement Ratified March 2015 Table of Contents
Writing Manuscripts About Quality Improvement: SQUIRE 2.0 and Beyond
 Writing Manuscripts About Quality Improvement: SQUIRE 2.0 and Beyond Author Marilyn H. Oermann, PhD, RN, ANEF, FAAN Thelma M. Ingles Professor of Nursing, Duke University School of Nursing Editor, Journal
Writing Manuscripts About Quality Improvement: SQUIRE 2.0 and Beyond Author Marilyn H. Oermann, PhD, RN, ANEF, FAAN Thelma M. Ingles Professor of Nursing, Duke University School of Nursing Editor, Journal
Milton Keynes University Hospital NHS Foundation Trust
 Milton Keynes University Hospital NHS Foundation Trust Enter and View Review of Staff/ Patient Communication Ward 17 and 18 September 2017 Contents Contents... 2 1 Introduction... 3 1.1 Details of the
Milton Keynes University Hospital NHS Foundation Trust Enter and View Review of Staff/ Patient Communication Ward 17 and 18 September 2017 Contents Contents... 2 1 Introduction... 3 1.1 Details of the
A Systematic Review of the Liaison Nurse Role on Patient s Outcomes after Intensive Care Unit Discharge
 Review Article A Systematic Review of the Liaison Nurse Role on Patient s Outcomes after Intensive Care Unit Discharge Zeinab Tabanejad, MSc; Marzieh Pazokian, PhD; Abbas Ebadi, PhD Behavioral Sciences
Review Article A Systematic Review of the Liaison Nurse Role on Patient s Outcomes after Intensive Care Unit Discharge Zeinab Tabanejad, MSc; Marzieh Pazokian, PhD; Abbas Ebadi, PhD Behavioral Sciences
Essential Skills for Evidence-based Practice: Evidence Access Tools
 Essential Skills for Evidence-based Practice: Evidence Access Tools Jeanne Grace Corresponding author: J. Grace E-mail: Jeanne_Grace@urmc.rochester.edu Jeanne Grace RN PhD Emeritus Clinical Professor of
Essential Skills for Evidence-based Practice: Evidence Access Tools Jeanne Grace Corresponding author: J. Grace E-mail: Jeanne_Grace@urmc.rochester.edu Jeanne Grace RN PhD Emeritus Clinical Professor of
Nurse Practitioner Impact on Patient Health Outcomes A P R IL N. KAPU, D NP, A P R N, ACNP - B C, FA A NP, F CCM
 Nurse Practitioner Impact on Patient Health Outcomes A P R IL N. KAPU, D NP, A P R N, ACNP - B C, FA A NP, F CCM NORTH CAROLINA NURSES ASSOCIAT ION NP SPRING SYMPOSIUM 20 17 Objectives Value Outcomes Strategies
Nurse Practitioner Impact on Patient Health Outcomes A P R IL N. KAPU, D NP, A P R N, ACNP - B C, FA A NP, F CCM NORTH CAROLINA NURSES ASSOCIAT ION NP SPRING SYMPOSIUM 20 17 Objectives Value Outcomes Strategies
Online Data Supplement: Process and Methods Details
 Online Data Supplement: Process and Methods Details ACC/AHA Special Report: Clinical Practice Guideline Implementation Strategies: A Summary of Systematic Reviews by the NHLBI Implementation Science Work
Online Data Supplement: Process and Methods Details ACC/AHA Special Report: Clinical Practice Guideline Implementation Strategies: A Summary of Systematic Reviews by the NHLBI Implementation Science Work
emja: Measuring patient-reported outcomes: moving from clinical trials into clinical p...
 Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
Página 1 de 5 emja Australia The Medical Journal of Home Issues emja shop My account Classifieds Contact More... Topics Search From the Patient s Perspective Editorial Measuring patient-reported outcomes:
The number of patients admitted to acute care hospitals
 Hospitalist Organizational Structures in the Baltimore-Washington Area and Outcomes: A Descriptive Study Christine Soong, MD, James A. Welker, DO, and Scott M. Wright, MD Abstract Background: Hospitalist
Hospitalist Organizational Structures in the Baltimore-Washington Area and Outcomes: A Descriptive Study Christine Soong, MD, James A. Welker, DO, and Scott M. Wright, MD Abstract Background: Hospitalist
A Primer on Activity-Based Funding
 A Primer on Activity-Based Funding Introduction and Background Canada is ranked sixth among the richest countries in the world in terms of the proportion of gross domestic product (GDP) spent on health
A Primer on Activity-Based Funding Introduction and Background Canada is ranked sixth among the richest countries in the world in terms of the proportion of gross domestic product (GDP) spent on health
Measure what you treasure: Safety culture mixed methods assessment in healthcare
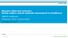 BUSINESS ASSURANCE Measure what you treasure: Safety culture mixed methods assessment in healthcare DNV GL Healthcare Presenter: Tita A. Listyowardojo 1 SAFER, SMARTER, GREENER Declaration of interest
BUSINESS ASSURANCE Measure what you treasure: Safety culture mixed methods assessment in healthcare DNV GL Healthcare Presenter: Tita A. Listyowardojo 1 SAFER, SMARTER, GREENER Declaration of interest
Improving teams in healthcare
 Improving teams in healthcare Resource 1: Building effective teams Developed with support from Health Education England NHS Improvement Background In December 2016, the Royal College of Physicians (RCP)
Improving teams in healthcare Resource 1: Building effective teams Developed with support from Health Education England NHS Improvement Background In December 2016, the Royal College of Physicians (RCP)
Clinical audit: a guide
 Clinical audit: a guide All nurses are expected to take part in clinical audits. Stephen Ashmore and Tracy Ruthven explain how it should be done HEALTHCARE PROFESSIONALS across the NHS are being encouraged
Clinical audit: a guide All nurses are expected to take part in clinical audits. Stephen Ashmore and Tracy Ruthven explain how it should be done HEALTHCARE PROFESSIONALS across the NHS are being encouraged
ROLE OF OUT-OF-HOURS NURSE CO-ORDINATORS IN A CHILDREN S HOSPITAL
 Art & science The synthesis of art and science is lived by the nurse in the nursing act JOSEPHINE G PATERSON ROLE OF OUT-OF-HOURS NURSE CO-ORDINATORS IN A CHILDREN S HOSPITAL Amy Hensman and colleagues
Art & science The synthesis of art and science is lived by the nurse in the nursing act JOSEPHINE G PATERSON ROLE OF OUT-OF-HOURS NURSE CO-ORDINATORS IN A CHILDREN S HOSPITAL Amy Hensman and colleagues
Pay-for-Performance: Approaches of Professional Societies
 Pay-for-Performance: Approaches of Professional Societies CCCF 2011 Damon Scales MD PhD University of Toronto Disclosures 1.I currently hold a New Investigator Award from the Canadian Institutes for Health
Pay-for-Performance: Approaches of Professional Societies CCCF 2011 Damon Scales MD PhD University of Toronto Disclosures 1.I currently hold a New Investigator Award from the Canadian Institutes for Health
A mental health brief intervention in primary care: Does it work?
 A mental health brief intervention in primary care: Does it work? Author Taylor, Sarah, Briggs, Lynne Published 2012 Journal Title The Journal of Family Practice Copyright Statement 2011 Quadrant HealthCom.
A mental health brief intervention in primary care: Does it work? Author Taylor, Sarah, Briggs, Lynne Published 2012 Journal Title The Journal of Family Practice Copyright Statement 2011 Quadrant HealthCom.
October 2015 TEACHING STANDARDS FRAMEWORK FOR NURSING & MIDWIFERY. Final Report
 October 2015 TEACHING STANDARDS FRAMEWORK FOR NURSING & MIDWIFERY Final Report Support for this activity has been provided by the Australian Government Office for Learning and Teaching. The views expressed
October 2015 TEACHING STANDARDS FRAMEWORK FOR NURSING & MIDWIFERY Final Report Support for this activity has been provided by the Australian Government Office for Learning and Teaching. The views expressed
Disclosure. SwedishAmerican Hospital A Division of UW Health. Learning Objectives. Medication History. Medication History 2/2/2017
 Disclosure Pharmacy Technician- Acquired Medication Histories in the ED: A Path to Higher Quality of Care David Huhtelin, PharmD Emergency Medicine Clinical Pharmacist SwedishAmerican Hospital A Division
Disclosure Pharmacy Technician- Acquired Medication Histories in the ED: A Path to Higher Quality of Care David Huhtelin, PharmD Emergency Medicine Clinical Pharmacist SwedishAmerican Hospital A Division
THE TRANSFORMATIVE MODEL IN MEDICAL EDUCATION AND CARE DELIVERY
 THE TRANSFORMATIVE MODEL IN MEDICAL EDUCATION AND CARE DELIVERY Project ECHO (Extension for Community Healthcare Outcomes) helps democratize medical knowledge and develops specialty care capacity in underserved
THE TRANSFORMATIVE MODEL IN MEDICAL EDUCATION AND CARE DELIVERY Project ECHO (Extension for Community Healthcare Outcomes) helps democratize medical knowledge and develops specialty care capacity in underserved
Delivering surgical services: options for maximising resources
 Delivering surgical services: options for maximising resources THE ROYAL COLLEGE OF SURGEONS OF ENGLAND March 2007 2 OPTIONS FOR MAXIMISING RESOURCES The Royal College of Surgeons of England Introduction
Delivering surgical services: options for maximising resources THE ROYAL COLLEGE OF SURGEONS OF ENGLAND March 2007 2 OPTIONS FOR MAXIMISING RESOURCES The Royal College of Surgeons of England Introduction
Worsening Shortages and Growing Consequences: CNO Survey on Nurse Supply and Demand
 Worsening Shortages and Growing Consequences: CNO Survey on Nurse Supply and Demand INTRODUCTION Healthcare organizations face growing challenges in finding the nurses they need, according to nurse leaders,
Worsening Shortages and Growing Consequences: CNO Survey on Nurse Supply and Demand INTRODUCTION Healthcare organizations face growing challenges in finding the nurses they need, according to nurse leaders,
Title:The impact of physician-nurse task-shifting in primary care on the course of disease: a systematic review
 Author's response to reviews Title:The impact of physician-nurse task-shifting in primary care on the course of disease: a systematic review Authors: Nahara Anani Martínez-González (Nahara.Martinez@usz.ch)
Author's response to reviews Title:The impact of physician-nurse task-shifting in primary care on the course of disease: a systematic review Authors: Nahara Anani Martínez-González (Nahara.Martinez@usz.ch)
Organizational Communication in Telework: Towards Knowledge Management
 Association for Information Systems AIS Electronic Library (AISeL) PACIS 2001 Proceedings Pacific Asia Conference on Information Systems (PACIS) December 2001 Organizational Communication in Telework:
Association for Information Systems AIS Electronic Library (AISeL) PACIS 2001 Proceedings Pacific Asia Conference on Information Systems (PACIS) December 2001 Organizational Communication in Telework:
