Open School IHI Open School Online Courses: Curriculum Overview
|
|
|
- Vincent Barber
- 6 years ago
- Views:
Transcription
1 Open School IHI Open School Online Courses: Curriculum Overview Improvement Capability... 3 QI 101: Introduction to Health Care Improvement... 3 QI 102: How to Improve with the Model for Improvement... 4 QI 103: Testing and Measuring Changes with PDSA Cycles... 5 QI 104: Interpreting Data: Run Charts, Control Charts, and other Measurement Tools... 6 QI 105: Leading Quality Improvement... 7 QI 201: Planning for Spread: From Local Improvements to System-Wide Change... 8 QI 202: Achieving Breakthrough Quality, Access, and Affordability... 9 QI 301: Guide to the IHI Open School Quality Improvement Practicum Patient Safety PS 101: Introduction to Patient Safety PS 102: From Error to Harm PS 103: Human Factors and Safety PS 104: Teamwork and Communication in a Culture of Safety PS 105: Responding to Adverse Events PS 201: Root Cause and Systems Analysis PS 202: Building a Culture of Safety PS 203: Partnering to Heal: Teaming Up Against Healthcare-Associated Infections PS 204: Preventing Pressure Ulcers Leadership L 101: Introduction to Health Care Leadership Person- and Family-Centered Care PFC 101: Introduction to Person- and Family-Centered Care PFC 102: Dignity and Respect PFC 103: Incorporating Mindfulness into Clinical Practice PFC 201: A Guide to Shadowing: Seeing Care through the Eyes of Patients and Families PFC 202: Having the Conversation: Basic Skills for Conversations about End-of-Life Care... 26
2 Triple Aim for Populations TA 101: Introduction to the Triple Aim for Populations TA 102: Improving Health Equity TA 103: Quality, Cost, and Value in Health Care Graduate Medical Education GME 201: Why Engage Trainees in Quality and Safety? GME 202: A Guide to the Clinical Learning Environment Review (CLER) Program GME 203: The Faculty Role: Understanding & Modeling Fundamentals of Quality & Safety GME 204: The Role of Didactic Learning in Quality Improvement GME 205: A Roadmap for Facilitating Experiential Learning in Quality Improvement GME 206: Aligning Graduate Medical Education with Organizational Quality & Safety Goals. 35 GME 207: Faculty Advisor Guide to the IHI Open School Quality Improvement Practicum Key 100 = Introductory concepts for all health care audiences 200 = Intermediate concepts and specialized topic areas 300 = Project-based learning *Basic Certificate in Quality and Safety = The Open School offers a certificate of completion to learners who complete 13 essential courses: QI , PS , TA 101, PFC 101, & L 101 About Us The IHI Open School s multimedia online courses cover a range of topics in quality improvement, patient safety, system design, leadership, and population management. Through narrative, video, and interactive discussion, the courses offer a dynamic learning environment to inspire students and health professionals of all levels. Courses are broken into digestible 15- to 40-minute lessons each focused on practical learning around a narrow topic designed for busy learners and educators. Institutional faculty and organizational leaders around the world rely on the courses as an easy way to bring essential training to students and staff. Visit ihi.org/education/ihiopenschool/courses to learn more about how the Open School can help improve your interactions with patients, the safety within your organization, or any of the systems in which you live and work. 2
3 Improvement Capability QI 101: Introduction to Health Care Improvement As the Institute of Medicine (IOM) declared in 2001, in words that still ring true, Between the health care we have and the care we could have lies not just a gap, but a chasm. This course launches you on your journey to becoming a health care change agent. First, it presents a high-level picture of the current quality of health care. Then, we ll share how six aims for improvement from the IOM are driving improvement efforts all over the world. Finally, we ll introduce you to Walter Shewhart, W. Edwards Deming, and a special type of science the science of improvement. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: Health and Health Care Today Lesson 2: The Institute of Medicine s Aims for Improvement Lesson 3: Changing Systems with the Science of Improvement 1. Describe common challenges for health care systems around the world. 2. List the six dimensions of health care, and the aims for each, outlined by the Institute of Medicine in Explain the value of improvement science in health care. Robert Lloyd, PhD, Vice President, Institute for Healthcare Improvement Sandy Murray, MA, Improvement Advisor, CT Concepts Lloyd Provost, MS, Statistician, Associates in Process Improvement 3
4 QI 102: How to Improve with the Model for Improvement This course will teach you how to use the Model for Improvement, developed by a group called Associates in Process Improvement, to improve everything from your tennis game to your hospital s infection rate. You ll learn the basic steps for introducing change in any system: setting an aim, selecting measures, developing ideas for changes, and testing changes using Plan-Do-Study-Act (PDSA) cycles. As you go along, you ll have the opportunity to use the same methodology to start your own personal improvement project. Estimated Time of Completion: 1 hour 30 minutes Lesson 1: An Overview of the Model for Improvement Lesson 2: Setting an Aim Lesson 3: Choosing Measures Lesson 4: Developing Changes Lesson 5: Testing Changes 1. List the three questions you must ask to apply the Model for Improvement. 2. Identify the key elements of an effective aim statement. 3. Identify three kinds of measures: process measures, outcome measures, and balancing measures. 4. Use change concepts and critical thinking tools to come up with good ideas for changes to test. 5. Test changes on a small scale using the Plan-Do-Study-Act (PDSA) cycle. Robert Lloyd, PhD, Vice President, Institute for Healthcare Improvement Sandy Murray, MA, Improvement Advisor, CT Concepts Lloyd Provost, MS, Statistician, Associates in Process Improvement 4
5 QI 103: Testing and Measuring Changes with PDSA Cycles In this course, we ll take you through basic concepts you need to know to run successful PDSA (Plan-Do-Study-Act) cycles in a clinical setting. First, we ll teach you how to plan and conduct small-scale tests of change. We ll discuss how you can establish a helpful set of measures and how to design a data collection plan that facilitates rapid learning, using techniques such as sampling. Next, we ll focus on studying the data you ve collected, and we ll explain why a run chart is such a valuable tool at this stage of the process. Finally, we ll show you how to act on your learning, possibly by increasing the size or scope of your next test cycle. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: How to Define Measures and Collect Data Lesson 2: How to Use Data for Improvement Lesson 3: How to Build Your Degree of Belief over Time 1. Describe how to establish and track measures of improvement during the plan and do phase of PDSA. 2. Explain how to learn from data during the study phase of PDSA. 3. Explain how to increase the size and scope of subsequent test cycles based on what you re learning during the act phase of PDSA. Kevin Little, PhD, Principal, Informing Ecological Design, LLC Robert Lloyd, PhD, Vice President, Institute for Healthcare Improvement Sandy Murray, MA, Improvement Advisor, CT Concepts Lloyd Provost, MS, Statistician, Associates in Process Improvement 5
6 QI 104: Interpreting Data: Run Charts, Control Charts, and other Measurement Tools In this course, we ll delve into how to draw an effective run chart. We ll show you how adding helpful elements such as a baseline median, goal line, and annotations of your tests of change can create a compelling picture of your progress toward improvement. We ll teach you the difference between common cause and special cause variation. And we ll show you how to detect signs of special cause variation by applying four rules to a standard run chart or by drawing a control chart. Once you ve got that down, we ll introduce you to three more excellent tools for displaying data and learning from the variation you re seeing. Estimated Time of Completion: 1 hour 30 minutes Lesson 1: How to Display Data on a Run Chart Lesson 2: How to Learn from Run Charts and Control Charts Lesson 3: Histograms, Pareto Charts, and Scatter Plots 1. Draw a run chart that includes a baseline median, a goal line, and annotations. 2. Describe the difference between common and special cause variation. 3. Explain the purpose of a Shewhart (or control) chart. 4. Apply four rules to identify non-random patterns on a run chart. 5. Explain when and how to use the following tools for understanding variation in data: histograms, Pareto charts, and scatter plots. Kevin Little, Ph.D, Principal, Informing Ecological Design, LLC David Williams, Ph.D., Executive Director, Institute for Healthcare Improvement 6
7 QI 105: Leading Quality Improvement The first four IHI Open School quality improvement courses taught you basic improvement methodology, which you can apply to improve health care processes and make care safer. But when you assume a leadership role in a clinical improvement project, you ll need more than just technical knowledge. In the real world, you ll need to know the steps for managing the project through to completion. You ll need to understand the psychology of change, and you ll need skills in interdisciplinary teamwork. In the real world, the human side of quality improvement that is, the ability to rally a group around a cause is every bit as important as having a good idea for a change. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: The Four Phases of a Quality Improvement Project Lesson 2: Change Psychology and the Human Side of Quality Improvement Lesson 3: Working with Interdisciplinary Team Members 1. Describe how to lead an improvement project through four key phases. 2. Identify and describe the components of IHI s Framework for Spread. 3. Apply strategies to assess and overcome resistance to change. 4. Apply strategies to work effectively with interprofessional colleagues. Sue Butts, Improvement Advisor, Butts-Dion Consulting, Inc. Mary Dolansky, RN, PhD, Associate Professor, Louis Stokes VA Medical Center Chris Grant, MD, Health Foundation & IHI Fellow/Consultant in Critical Care, Aintree University Hospital Holly Oh, MD, Chief Medical Officer, Dimock Community Health Center David Williams, Ph.D., Executive Director, Institute for Healthcare Improvement 7
8 QI 201: Planning for Spread: From Local Improvements to System-Wide Change Previous courses in the Quality Improvement catalog focused on testing and implementing a change in one location. This advanced course is about the next logical step: spreading the change. You ll learn about the theory of how change spreads, according to the foundational work of psychologist Kurt Lewin and sociologist Everett Rogers. Then you ll learn how to help a new idea spread across a population, both by motivating the people within the population to adopt the change and by developing new ideas that are inherently more likely to spread. Finally, we ll introduce IHI s Framework for Spread, and you ll follow a detailed case study about how an organization used the methodologies you re studying to improve patient care at the bedside throughout Central Texas. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: How Change Spreads Lesson 2: Tactics for Spreading Change Lesson 3: Case Study in Spreading Innovations: Transforming Care at the Bedside 1. Describe how change spreads according to Kurt Lewin and Everett Rogers. 2. Assess the likelihood that a new idea will spread. 3. Apply IHI s Framework for Spread to spread an innovation across an organization. Sue Butts, Improvement Advisor, Butts-Dion Consulting, Inc. David Williams, Ph.D., Executive Director, Institute for Healthcare Improvement 8
9 QI 202: Achieving Breakthrough Quality, Access, and Affordability How does an organization go from providing ho-hum, average care to providing breakthrough quality, access, and affordability to patients? In this course, you ll learn to apply a basic framework for designing, operating, and improving complex systems of care that can lead to rapid gains in performance. First, you ll learn that while advances in technology have led to much better patient outcomes over the past few decades, they ve also made for a much more complex health care system. That complexity makes it impossible to predict exactly how the system will perform dynamically, which in turn means that constant, broad-based innovation is absolutely required as staff members discover weak signals of system failure. Improving big clinical problems such as central line infections, you ll learn, requires that staff members report tiny, apparently harmless problems as they occur and it requires that senior leaders actually do something about those problems. By the end of this course, you ll identify the weak signals of system failure all around you, and you ll also figure out exactly what your organization needs in order to respond effectively. Estimated Time of Completion: 1 hour 45 minutes Lesson 1: Two Mustangs Lesson 2: How to Make Complex Systems Fail Lesson 3: Solving Problems in Complex Systems 1. Explain why system complexity requires us to take a methodical approach to system design, operation, and improvement. 2. Explain how the absence of this methodical approach will cause complex systems to fail predictably. 3. Propose specific applications of this methodical approach to the design, operation, and improvement of health care. Steven Spear, DBA, SM, SM, Senior Fellow, Massachusetts Institute of Technology Tom Downes, MB BS, MRCP, MBA, MPH (Harvard), Consultant Geriatrician and IHI Fellow, Sheffield Teaching Hospitals 9
10 QI 301: Guide to the IHI Open School Quality Improvement Practicum This course is designed to walk you through the process of conducting a quality improvement project. It will call on your knowledge and learning from many other IHI Open School courses, and help you apply quality improvement skills in a real-world setting. Unlike other courses in our catalog, you will submit documents after several of the lessons. To help make sure your project is headed in the right direction, we will review the project charter you submit after Lesson 2 and provide written feedback. Then, at the end, after you turn in your summary report, we will provide additional feedback about your project. (Note: We will provide feedback and award the Practicum Certificate only on student projects. Professionals are welcome to participate, but we aren t able to offer direct feedback at this time.) Estimated Time of Completion: 1 hour 15 minutes + project time Lesson 1: Putting Quality Improvement into Practice Lesson 2: Starting Your Project Lesson 3: Looking for Changes? Try Cause and Effect Diagrams Lesson 4: Spell Improvement with P-D-S-A Lesson 5: Data: Collect and Display Lesson 6: Summarizing Your Project 1. Use the Model for Improvement to plan and carry out a quality improvement project in your local health care setting. 2. Develop a charter to guide you through a clinical quality improvement project. 4. Develop a cause and effect diagram to help you understand your theories for accomplishing your aim. 5. Use multiple Plan-Do-Study-Act (PDSA) cycles to test changes in a health care setting. 6. Construct a run chart that tracks measures over time for your improvement project. 7. Create a summary report that summarizes the learning from your project. James Moses, MD, Director of Safety and Quality, Boston Medical Center Michael Briddon, MA, Editorial Director, Institute for Healthcare Improvement 10
11 Patient Safety PS 101: Introduction to Patient Safety No one embarks on a health care career intending to harm patients. But much too often, patients die or suffer injuries from the care they receive. In this course, you ll learn why becoming a student of patient safety is critical for everyone involved in health care today. First, you ll learn about the human and financial toll of medical error and adverse events around the world. Next, you ll learn why blame is rarely the appropriate (or helpful) response to error. Finally, you ll learn four essential behaviors that any health care professional can adopt right away to improve the safety of patients. Estimated Time of Completion: 1 hour 30 minutes Lesson 1: Understanding Medical Error and Patient Safety Lesson 2: Responding to Errors and Harm Lesson 3: A Call to Action What YOU Can Do 1. Summarize the scope of medical errors and preventable harm to patients in health care. 2. Describe the impact of medical errors on patients, families, and providers. 3. Explain why blaming and punishing individuals for errors rarely improves patient safety. 4. Identify four ways any provider can improve safety for patients in his or her direct care. Doug Bonacum, MBA, CSP, Vice President for Safety Management, Kaiser Permanente Fran Griffin, RRT, MPA, Owner, Fran Griffin & Associates LLC 11
12 PS 102: From Error to Harm This course provides an overview of the key concepts in the field of patient safety. You ll learn the relationship between error and harm, and how unsafe conditions and human error lead to harm through something called the Swiss cheese model. You ll learn how to classify different types of unsafe acts that humans commit, including error, and how the types of unsafe acts relate to harm. Finally, you ll learn about how the field of patient safety has expanded its focus from reducing error to also encompass efforts to reduce harm. Estimated Time of Completion: 1 hour Lesson 1: The Swiss Cheese Model Lesson 2: Understanding Unsafe Acts Lesson 3: A Closer Look at Harm 1. Explain the Swiss cheese model of error. 2. Define active failures and latent error and discuss their roles in causing harm. 3. List the main types of unsafe acts utilizing James Reason s classification system. 4. Identify at least one example of how health care has reduced harm. Fran Griffin, RRT, MPA, Director, The Institute for Healthcare Improvement Doug Bonacum, MBA, CSP, Vice President for Safety Management, Kaiser Permanente 12
13 PS 103: Human Factors and Safety This course is an introduction to the field of human factors: how to incorporate knowledge of human behavior in the design of safe systems. You ll explore case studies to analyze the human factors issues involved in health care situations. And you ll learn how to use human factors principles to design safer systems of care including the most effective strategies to prevent errors and mitigate their effects. Finally, you ll learn how technology can reduce errors even as, in some cases, it can introduce new opportunities for errors. Estimated Time of Completion: 1 hour Lesson 1: Understanding the Science of Human Factors Lesson 2: Changes Based on Human Factors Design Principles Lesson 3: Using Technology to Mitigate the Impact of Error 1. Explain how human factors principles apply to health care. 2. Describe how changes to processes can mitigate the effects of factors that contribute to error. 3. Define simplification, standardization, constraints, forcing functions, and redundancies. 4. Discuss the risks and benefits of using technology to improve patient safety. Frank Federico, RPh, Vice President, Senior Expert Patient Safety, Institute for Healthcare Improvement 13
14 PS 104: Teamwork and Communication in a Culture of Safety Effective teamwork and communication are critical parts of the design of safe systems. In this course, you ll learn what makes an effective team through case studies from health care and elsewhere. You ll analyze the effects of individual behavior for promoting teamwork, communication, and a culture safety. Finally, you ll learn several essential communication tools, such as briefings, SBAR, and critical language. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: Why Are Teamwork and Communication Important? Lesson 2: How Can You Contribute to a Culture of Safety? Lesson 3: Basic Tools and Techniques for Effective Communication 1. Explain why effective teamwork is essential for promoting patient safety. 2. Define a culture of safety and discuss the features of a strong safety culture. 3. Identify four behaviors anyone can use to promote teamwork, communication, and a culture of safety. 4. Use structured communication techniques to improve communication within health care. Allan Frankel, MD, Patient Safety and Reliability Expert, Safe and Reliable Healthcare Michael Leonard, MD, Principal, Safe & Reliable Healthcare, Safe & Reliable Healthcare 14
15 PS 105: Responding to Adverse Events In this course, we re going to describe and advocate a patient-centered approach to use when things go wrong. This approach to adverse events and medical error centers on the needs of the patient, but it is also the best way to address the needs of a caregiver in the wake of an adverse event. Finally, we ll introduce a systematic response to error called root cause analysis, the goal of which is to learn from adverse events and prevent them from happening in the future. Estimated Time of Completion: 1 hour 45 minutes Lesson 1: Responding to an Adverse Event: A Step-by-Step Approach Lesson 2: When and How to Apologize to Patients Lesson 3: The Impact of Adverse Events on Caregivers: The Second Victim Lesson 4: Learning From Errors through Root Cause Analysis 1. Describe four steps to take in the immediate aftermath of an adverse event. 2. Explain when you should apologize to a patient and how to apologize effectively. 3. Discuss the impact of adverse events on providers. 4. Explain how you can use root cause analysis to address system problems in health care. Frank Federico, RPh, Executive Director, Strategic Partners, Institute for Healthcare Improvement Allan Frankel, MD, Principal, Pascal Metrics Inc. 15
16 PS 201: Root Cause and Systems Analysis The goal of a root causes analysis (RCA) is to learn from adverse events and prevent them from happening in the future. The three lessons in this course explain RCAs in detail, using case studies and examples from both industry and health care. By the end, you ll learn a step-by-step approach to completing a RCA after an error and improving the process that led to the error. Estimated Time of Completion: 1 hour 30 minutes Lesson 1: Root Cause Analysis Helps Us Learn from Errors Lesson 2: How a Root Cause Analysis Works Lesson 3: How a Root Cause Analysis Can Help Improve Health Care 1. Explain how to use adverse events as learning opportunities. 2. Determine which adverse events are appropriate for a root cause analysis. 3. Describe how RCA works. 4. Explain how you can use RCA to address system problems in health care. Samuel Huber, MD, Associate CMO for Patient Safety and Quality, Rochester Regional Health System Greg Ogrinc, MD, Physician, White River Junction VA Medical Center 16
17 PS 202: Building a Culture of Safety As long as human beings provide health care, mistakes and errors will occur. However, health care providers can reduce the likelihood of such occurrences, and limit their impact, by fostering a culture of safety. This is an environment that encourages people to speak up about safety concerns, makes it safe to talk about mistakes and errors, and encourages learning from these events. How providers can create and foster a culture of safety is the focus of this advanced course. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: Leading Health Systems through Adverse Events Lesson 2: What Does a Culture of Safety Look Like? Lesson 3: Tactics for Leading Cultural Change 1. Discuss your opinions on one hospital s response to a serious adverse event. 2. Explain the four components of a culture of safety: psychological safety, fairness, transparency, and effective leadership. 3. Describe the process of culture change and identify at least three tactics to accelerate it. Allan Frankel, MD, Patient Safety and Reliability Expert, Safe and Reliable Healthcare Michael Leonard, MD, Principal, Safe & Reliable Healthcare, Safe & Reliable Healthcare Robert Lloyd, PhD, Vice President, Institute for Healthcare Improvement Sandy Murray, MA, Improvement Advisor, CT Concepts Lloyd Provost, MS, Statistician, Associates in Process Improvement David Williams, Ph.D., Executive Director, Institute for Healthcare Improvement 17
18 PS 203: Partnering to Heal: Teaming Up Against Healthcare-Associated Infections Partnering to Heal: Teaming Up Against Healthcare-Associated Infections is a computerbased, interactive learning tool for early-career clinicians, health professional students, patients, and visitors on preventing healthcare-associated infections. The training video was created by the U.S. Department of Health & Human Services (HHS), in consultation with subject matter experts from various disciplines and sectors, as well as patient advocates, as part of a wider effort that works closely with public and private sector partners to improve the quality, safety, and affordability of healthcare for all Americans. The dramatization is intended to increase awareness of the risks of healthcare-associated infections and the opportunities for preventing such infections. It is not intended to reflect common clinical care. Certain scenes demonstrate a worst-case scenario of how lapses in medical judgment, communication, teamwork, and attention to infection control practices might impact patient outcomes. The intent is to provide a training tool for use by health professionals, students, patients, and their families about patient safety concepts, rather than provide an accurate or comprehensive depiction of conditions caused by specific pathogens. This interactive video, authored in part by Vet-Work Learning Solutions, Inc., was funded in whole or in part by the U.S. Department of Health and Human Services under U.S. Government contract HHSP A. Department of Health and Human Services (HHS) hosted materials are available free of charge on the HHS website at Estimated Time of Completion: 2 hours Lesson 1: Partnering to Heal 1. Identify when and how to speak to colleagues and other providers about safety practices and improvement efforts. 2. Explain the role of the patient and family in preventing healthcare-associated infections. 3. Identify effective methods to communicate the importance of safety practices. 4. List at least three approaches to working with those skeptical about the importance of safety practices and improvement efforts. United States Department of Health and Human Services 18
19 PS 204: Preventing Pressure Ulcers Pressure ulcers, or bed sores, continue to be a significant problem in health care today. They cause unnecessary harm to patients, increase length of stay, and cost organizations millions of dollars every year. They are also preventable. In the four lessons of this course, we ll quickly explain the basics of pressure ulcers, and then spend the bulk of our time talking about how to prevent them and treat them. We ll highlight exemplary organizations, share the latest research, and provide video tips that you can put to use in your local setting. Estimated Time of Completion: 1 hour 30 minutes Lesson 1: Why Work on Preventing Pressure Ulcers? Lesson 2: Assessing Patients Lesson 3: Responding to Patients Lesson 4: How to Implement a Pressure Ulcer Prevention Program 1. Explain the importance of preventing pressure ulcers. 2. Define the key elements in pressure ulcer assessment. 3. Define the key elements in pressure ulcer prevention. 4. Apply a range of tools and methods for responding to at-risk patients. 5. Outline how to implement a reliable pressure ulcer prevention program. Kathleen Vega, BA, Freelance Writer, Kathleen B. Vega, Inc. Kathy Duncan, RN, Faculty, Institute for Healthcare Improvement Editor(s): Michael Briddon, MA, Editorial Director, Institute for Healthcare Improvement 19
20 Leadership L 101: Introduction to Health Care Leadership When you think of a leader, who comes to mind? A president? A CEO? This course will teach you a different idea of leadership: No matter your position or formal title, you can be a leader. In this course, you ll learn about a hospital that s having some trouble with infection control. As you grapple with the case, you ll learn that leadership isn t a position of authority it s an action. You ll learn how to persuade different types of people and build enough unity to move forward. Finally, you ll learn some strategies for sustaining your leadership journey over time. Estimated Time of Completion: 1 hour 15 minutes Lesson 1: What Makes a Leader? Lesson 2: Practical Skills for Leading Teams Lesson 3: Strategies to Sustain Your Health Care Leadership Journey 1. Describe several characteristics of leaders, who may or may not have formal positions of authority. 2. Describe different techniques for persuading different types of people. 3. Explain why achieving a workable level of unity among teammates is essential for effective team functioning. 4. List several ways to help sustain your health care leadership journey over time. Jonathan Finkelstein, MD, MPH, Professor, Harvard University Medical School Chris Grant, MD, Health Foundation & IHI Fellow/Consultant in Critical Care, Aintree University Hospital Holly Oh, MD, Chief Medical Officer, Dimock Community Health Center James Reinertsen, MD, President, The Reinertsen Group 20
21 Person- and Family-Centered Care PFC 101: Introduction to Person- and Family-Centered Care The relationship between patient and provider is changing. Many health care systems aim to provide not only high-quality services, but also patient-centered care that advances the unique health goals of each person and family. In this course, you ll learn about the ideal relationship to promote health especially for underserved people who face the greatest barriers to health as well as some practical skills to make the relationship a reality. Estimated Time of Completion: 1 hours 30 minutes Lesson 1: Patient-Provider Partnerships for Health Lesson 2: Understanding Patients as People Lesson 3: Skills for Patient-Provider Partnerships 1. Describe the partnership model of patient-provider relationships. 2. Explain why the partnership model can improve health. 3. Discuss how social conditions, faith, culture, and trust affect the patient-provider relationship. 4. Identify at least four skills to improve clinical interactions with patients. Nia Zalamea, MD, Church Health Center Kendra Hotz, PhD, Assistant Professor of Religious Studies, Rhodes College 21
22 PFC 102: Dignity and Respect What does it mean to treat patients and families with dignity and respect? It means that health care providers listen to and honor patient and family perspectives and choices. Providers incorporate patient and family knowledge, values, beliefs, and cultural background into the planning and delivery of care. Providers anticipate patient and family needs, and meet those needs in a clean, safe environment. The health care team provides emotional support to patients and families, and strives to alleviate their fear and anxiety. How can providers accomplish all of this? By learning and then practicing the specific skills described and illustrated in this course. Estimated Time of Completion: 2 hours Lesson 1: An Introduction to Patient- and Family-Centered Care Lesson 2: First Impressions Lesson 3: Privacy and Confidentiality Lesson 4: Culture and Belief Systems Lesson 5: Creating a Restful and Healing Environment 1. Explain why patient- and family-centered care is an essential component of safe care. 2. Describe and use specific skills for treating patients and their families with dignity and respect, especially when first meeting patients and their families. 3. Describe and use specific skills for ensuring patients privacy and confidentiality. 4. Describe and use specific skills for respecting patients and families cultures, languages, and belief systems. 5. Describe and use specific skills for creating a restful and healing environment for patients. Children s Hospital of Philadelphia 22
23 PFC 103: Incorporating Mindfulness into Clinical Practice Clinicians juggle many tasks all day long: assessing patients, making critical decisions, administering medications, documenting care, admitting and discharging patients, and much more. But when the clinician is able to embrace an aware, focused, and present state that transcends the execution of tasks that is practicing mindfulness. This course will show you how to incorporate mindfulness into your practice. You'll learn how it can improve patient safety, quality of care, the patient experience, and joy in work in any health care setting. This content was made possible through grant funding awarded to the primary author, Kate FitzPatrick, DNP, RN, ACNP, NEA-BC, FAAN, by the Robert Wood Johnson Foundation (Executive Nurse Fellowship Program, 2014 Cohort). Estimated Time of Completion: 1 hour Lesson 1: Incorporating Mindfulness into Clinical Practice 1. Describe the need for mindfulness practices in the health care setting, including how these practices relate to quality of care, patient safety, patient experience, and joy in work. 2. Explain the difference between informal and formal mindfulness practice. 3. List several examples of mindfulness exercises for the health care setting. 4. List four situations in health care when mindfulness is especially important. 5. Conduct a body scan. Author: Kate Fitzpatrick, Senior Vice President and Chief Nursing Officer, University of Vermont Medical Center Arnie Kozak, Psychotherapist and Clinical Assistant Professor in Psychiatry, University of Vermont Medical Center Lindsay Foreman, Mindfulness Program Coordinator, University of Vermont Medical Center Mary Streeter, Advance Practice Provider, Department of Radiology, University of Vermont Medical Center Sanchit Maruti, Psychiatrist and Assistant Professor, University of Vermont Medical Center Teri Pipe, Dean of College of Nursing and Health Innovation and Chief Well-being Officer, Arizona State University 23
24 Editors Kate Fitzpatrick, Senior Vice President and Chief Nursing Officer, University of Vermont Medical Center Laura Fink, Senior Managing Editor, Institute for Healthcare Improvement Reviewers Kara Penfield, Senior Faculty Member and Coaching Talent Leader, Center for Creative Leadership Michael Posencheg, Associate Chief Medical Officer, Value Improvement, Penn Medicine Medical Director, Intensive Care Nursery Hospital of the University of Pennsylvania, University of Pennsylvania Hospital Rosalyn Grossman, Health Educator, University of Vermont Medical Center 24
25 PFC 201: A Guide to Shadowing: Seeing Care through the Eyes of Patients and Families In this one-lesson course, we ll introduce you to patient and family shadowing, a valuable exercise for health professions students and health care professionals at any stage of their career. You ll learn five steps for using shadowing to better empathize with patients and families. You ll see how empathy can help you in your daily work, and how it can drive a sense of urgency to start testing and spreading changes to improve care. Estimated Time of Completion: 30 minutes Lesson 1: A Guide to Shadowing: Seeing Care through the Eyes of Patients and Families 1. Define patient and family shadowing. 2. List five steps for conducting a successful shadowing project. 3. Describe how to interact with patients, families, and clinical staff involved in a shadowing project. 4. Discuss how you can use your shadowing experience to create a care experience flow map, observational summary, and final report. 5. Explain how shadowing can help you come up with ideas for changes to improve care. Author: Anthony Digioia, MD, Medical Director, The Bone and Joint Center at Magee-Womens Hospital and the PFCC Innovation Center of the University of Pittsburgh Medical Center 25
26 PFC 202: Having the Conversation: Basic Skills for Conversations about End-of-Life Care In conjunction with the Boston University School of Medicine and The Conversation Project, the IHI Open School offers this course to introduce students and health professionals to basic skills for having conversations with patients and their families about end-of-life care wishes. This course will also help you develop skills to have conversations with patients and their families about their preferences for care at the end of life. As part of developing these skills, the course invites you to have the conversation yourself, with a family member or other loved one. Estimated Time of Completion: 2 hours Lesson 1: Conversation: An Essential Element of Good End-of-Life Care Lesson 2: The Conversation Begins with You Lesson 3: Understanding and Respecting Your Patients Wishes Lesson 4: Changing the Culture: Better Ways to Care for Patients Nearing the End of Life 1. Conduct conversations with patients and families to learn their wishes for end-of-life care. 2. Explain available treatment options to patients and families in terms they can understand. 3. Demonstrate how to answer difficult questions related to end-of-life care. 4. Facilitate conversations with patients and families to help them make decisions about end-of-life care, based on an understanding of what matters most to them. Author: Eric Hardt, MD, Associate Professor of Medicine, Boston University School of Medicine Jessica McCannon, MD, Assistant in Medicine, Massachusetts General Hospital Lisa Norton, MD, Clinical Assistant Professor of Medicine, Boston University Medicine Jane Roessner, PhD, Writer, Institute for Healthcare Improvement Winnie Suen, MD, Adjunct Assistant Professor of Medicine, Boston University Medicine 26
27 Triple Aim for Populations TA 101: Introduction to the Triple Aim for Populations You might think we do a pretty good job of providing care to individuals with illnesses and diseases. But it s important to take a step back and consider the factors contributing to illness. It s important to realize that things like education, the environment, and wealth (and how it s distributed) play an enormous role in health outcomes, too. In this course, you ll learn that to make progress against many of the most important threats to human health, it s not enough to improve clinical care for one patient at a time. We also have to focus on improving the health of entire populations. The Triple Aim for populations is a three-part aim: better care for individuals, better health for populations, all at a lower cost. This course will explore why each dimension is an essential part of improving health and health care, and how you can promote the Triple Aim in your organization and daily work. Estimated Time of Completion: 2 hours Lesson 1: Improving Population Health Lesson 2: Providing Better Care Lesson 3: Lowering Costs of Care 1. Describe the three components of the IHI Triple Aim for populations. 2. Explain the responsibilities of clinicians and health care systems in optimizing population-level outcomes with available resources. 3. Understand medical care as one determinant of the overall health of a population, and the relationship of health care quality and safety to population health. 4. Provide examples of population-level interventions designed to improve overall health and reduce costs of care. Jonathan Finkelstein, MD, MPH, Associate Professor, Harvard University Medical School Donald M. Berwick, MD, MPP, President Emeritus and Senior Fellow, Institute for Healthcare Improvement 27
28 TA 102: Improving Health Equity This three-lesson course will explore health disparities what they are, why they occur, and how you can help reduce them in your local setting. After discussing the current (and alarming) picture in Lesson 1, we ll dive into Lesson 2 and learn about some of the promising work that is reducing disparities in health and health care around the world. Then, in Lesson 3, we ll suggest how you can start improving health equity in your health system and community. Estimated Time of Completion: 2 hours Lesson 1: Understanding Health Disparities Lesson 2: Initiatives to Improve Health Equity Lesson 3: Your Role in Improving Health Equity 1. Recognize at least two causes of health disparities in the US and around the world. 2. Describe at least three initiatives to reduce disparities in health and health care. 3. Identify several ways you can help reduce health disparities. Alex Anderson, Research, Innovation Co-Chair, IHI Diversity/Inclusion Council, Institute for Healthcare Improvement Nigel Deen, Research, Innovation Team Lead, IHI Diversity/Inclusion Council, Institute for Healthcare Improvement 28
29 TA 103: Quality, Cost, and Value in Health Care This course will provide you with an overview of value in health care. We ll start by distinguishing between cost and value, and understanding how both of these concepts relate to quality. We ll introduce you to the growing problem of health care spending, as well as the health care practitioner s role in managing these costs. Finally, we ll explain how to identify and overcome barriers to providing high-value, cost-effective care. Estimated Time of Completion: 45 minutes Lesson 1: Quality, Cost, and Value in Health Care 1. Explain the potential harm of low-value tests and procedures. 2. Distinguish between cost and value in health care. 3. Define resource stewardship in health care. 4. Describe the ethical case for resource stewardship in health care. 5. Identify common barriers to resource stewardship and enablers of inappropriate resource use. Marisa Leon-Carlyle, Medical Student, University of Toronto Raman Srivastava, BMSc(h), MBT, MD(c), Medical Student, University of Toronto Brian Wong, MD, Assistant Professor, Department of Medicine, University of Toronto 29
30 Graduate Medical Education GME 201: Why Engage Trainees in Quality and Safety? In this course, we ll discuss several reasons why organizations should strive to incorporate trainees (medical residents and fellows) in quality and safety work. You will hear from faculty and residents about why this effort is so important and how it can enhance the overall quality and safety of health care delivery. Estimated Time of Completion: 30 minutes Lesson 1: Why Engage Trainees in Quality and Safety? 1. List at least two reasons why it is important to engage medical residents and fellows in quality and safety work. 2. Describe the benefits of starting quality and safety training during a residency or fellowship. 3. Identify at least three barriers to engaging residents and fellows in quality and safety work. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 30
31 GME 202: A Guide to the Clinical Learning Environment Review (CLER) Program This course will introduce you to the Accreditation Council for Graduate Medical Education (ACGME) Clinical Learning Environment Review (CLER) program. We ll describe how CLER works, and demonstrate how different organizations are responding to the call for better learning environments in graduate medical education. This course will help you become more prepared to take part in a CLER site visit and to engage trainees (medical residents and fellows) in your institution s work in quality improvement and patient safety. Estimated Time of Completion: 30 minutes Lesson 1: A Guide to the Clinical Learning Environment Review (CLER) Program 1. Describe the primary goal of the CLER program. 2. List the six focus areas within the CLER program. 3. Explain the steps involved in a CLER program site visit. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 31
32 GME 203: The Faculty Role: Understanding & Modeling Fundamentals of Quality & Safety Just because you agree that quality and safety are priorities doesn t mean you will feel well prepared to lead the charge in these complex areas. You may be at the very beginning of your own journey toward becoming proficient in quality improvement and patient safety (QI/PS) and that s okay. In this course, you ll gain a better understanding of your current knowledge of QI/PS, and then have the opportunity to expand your knowledge where it may be lacking. Even if you haven t received formal training in these areas, we ll show you that teaching QI/PS skills to the next generation relies on faculty like you. Estimated Time of Completion: 30 minutes Lesson 1: The Faculty Role: Understanding & Modeling Fundamentals of Quality & Safety 1. Explain why it is important for faculty members to engage trainees in meaningful QI/PS work that is tied to everyday clinical care. 2. Describe four principles for designing educational experiences in QI/PS. 3. List the core competencies in QI/PS that every faculty member should possess. 4. List several ways faculty can model the use of improvement principles in everyday work. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 32
33 GME 204: The Role of Didactic Learning in Quality Improvement In this course, we ll discuss several reasons why organizations should strive to incorporate trainees (medical residents and fellows) in quality and safety work. You will hear from faculty and residents about why this effort is so important and how it can enhance the overall quality and safety of health care delivery. Estimated Time of Completion: 30 minutes Lesson 1: The Role of Didactic Learning in Quality Improvement 1. Explain what kinds of topics are important to include in a didactic curriculum on QI/PS for trainees. 2. Give examples of available QI/PS training materials, and explain how they could be integrated into a curriculum. 3. Describe the characteristics of a successful QI/PS curriculum for adult learners. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 33
34 GME 205: A Roadmap for Facilitating Experiential Learning in Quality Improvement In this course, we ll provide a roadmap that will help you engage trainees in experiential learning at the point of care. We ll cover three different models of experiential learning within an adaptable framework. Based on your setting, role, and evolving comfort with quality improvement and patient safety (QI/PS) concepts and tools, you ll choose the best approach for you. Estimated Time of Completion: 60 minutes Lesson 1: A Roadmap for Facilitating Experiential Learning in Quality Improvement 1. Explain the importance of supplementing didactic instruction with experiential training. 2. Describe three different models for experiential learning, and list several pros and cons of each. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 34
35 GME 206: Aligning Graduate Medical Education with Organizational Quality & Safety Goals In this course, we ll present innovative strategies that training programs around the country are using to engage residents in institution-wide quality improvement and patient safety (QI/PS) efforts. This toolbox of change ideas will help you or your institution s quality leaders build successful collaborations between existing QI/PS infrastructures and graduate medical education (GME) programs. Estimated Time of Completion: 1 hour Lesson 1: Aligning Graduate Medical Education with Organizational Quality & Safety Goals 1. List and describe four change ideas that are being implemented in training programs around the country to accelerate QI/PS education at the graduate medical education level. 2. Discuss the cultural shift that is occurring, in which organizations are focusing on root cause analysis and systemic improvement as opposed to placing individual blame. 3. Suggest at least two reasons why trainee participation in institutional QI/PS activities and committees is critical. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 35
36 GME 207: Faculty Advisor Guide to the IHI Open School Quality Improvement Practicum Are you ready to see your students and residents put their improvement knowledge into action? The IHI Open School has a unique offering, the IHI Open School Quality Improvement Practicum, that helps new improvers through the process of setting up and conducting a real-world quality improvement (QI) project but they can t do it without you. For your trainees, we ve created a six-lesson course, QI 301: Guide to the IHI Open School Quality Improvement Practicum, that takes them step by step through a health care improvement project. For you, we ve created this companion guide. In this one-lesson course, you ll receive all the knowledge and tools you need to be a Faculty Advisor for the IHI Open School Practicum. With your help, students and residents can use the Practicum to improve the quality of patient care. Estimated Time of Completion: 1 hour Lesson 1: Faculty Advisor Guide to the IHI Open School Quality Improvement Practicum 1. Explain the value of using the IHI Open School Quality Improvement Practicum to help clinical trainees conduct quality improvement projects. 2. Describe each of the components of the IHI Open School Quality Improvement Practicum: teacher-learner agreement, project charter, cause and effect diagram, PDSA forms, run charts, and summary report. 3. Describe your role as a Faculty Advisor for a Practicum project, including several specific responsibilities you will have. 4. Describe the qualities of an appropriately focused Practicum project. 5. Suggest improvements to trainees Practicum documents, including project charters, cause and effect diagrams, PDSA forms, and summary reports. Laura Johnson Faherty, MD, MPH, Robert Wood Johnson Foundation Clinical Scholar, University Of Pennsylvania Kedar Mate, MD, Senior Vice President, Institute for Healthcare Improvement James Moses, MD, Medical Director of Quality Improvement, Boston Medical Center 36
Course Catalog. L 101: Becoming a Leader in Health Care Quality, Cost, and Value
 Course Catalog Improvement Capability QI 101: Fundamentals of Improvement... 2 QI 102: The Model for Improvement: Your Engine for Change... 3 QI 103: Measuring for Improvement... 4 QI 104: The Life Cycle
Course Catalog Improvement Capability QI 101: Fundamentals of Improvement... 2 QI 102: The Model for Improvement: Your Engine for Change... 3 QI 103: Measuring for Improvement... 4 QI 104: The Life Cycle
Improvement Capability QI 101: Introduction to Health Care Improvement* QI 102: How to Improve with the Model for Improvement*...
 Open School IHI Open School Online Courses: Course Summary Sheets Improvement Capability... 3 QI 101: Introduction to Health Care Improvement*... 3 QI 102: How to Improve with the Model for Improvement*...
Open School IHI Open School Online Courses: Course Summary Sheets Improvement Capability... 3 QI 101: Introduction to Health Care Improvement*... 3 QI 102: How to Improve with the Model for Improvement*...
ABMS Organizational QI Forum Links QI, Research and Policy Highlights of Keynote Speakers Presentations
 ABMS Organizational QI Forum Links QI, Research and Policy Highlights of Keynote Speakers Presentations When quality improvement (QI) is done well, it can improve patient outcomes and inform public policy.
ABMS Organizational QI Forum Links QI, Research and Policy Highlights of Keynote Speakers Presentations When quality improvement (QI) is done well, it can improve patient outcomes and inform public policy.
Continuous Value Improvement in Health Care
 webinar summary Continuous Value Improvement in Health Care Featuring Kedar Mate Chief Innovation and Education Officer Institute for Healthcare Improvement October 26, 2017 sponsored by webinar summary
webinar summary Continuous Value Improvement in Health Care Featuring Kedar Mate Chief Innovation and Education Officer Institute for Healthcare Improvement October 26, 2017 sponsored by webinar summary
Leadership for Transforming Health Care
 Presenters have nothing to disclose. Leadership for Transforming Health Care Partnerships with Patients and Families Barbara Balik, RN, EdD Kris White, RN, MBA November 4, 2014 This presenter has nothing
Presenters have nothing to disclose. Leadership for Transforming Health Care Partnerships with Patients and Families Barbara Balik, RN, EdD Kris White, RN, MBA November 4, 2014 This presenter has nothing
Massachusetts General Hospital Nursing & Patient Care Services Strategic Plan
 Massachusetts General Hospital Nursing & Patient Care Services 2017 Strategic Plan January 2017 Mission Guided by the needs of our patients and their families, we aim to deliver the very best health care
Massachusetts General Hospital Nursing & Patient Care Services 2017 Strategic Plan January 2017 Mission Guided by the needs of our patients and their families, we aim to deliver the very best health care
A S S E S S M E N T S
 A S S E S S M E N T S Community Design Assessment This process was developed to aid healthcare organizations in taking the pulse of their community prior to the start of capital improvement projects. A
A S S E S S M E N T S Community Design Assessment This process was developed to aid healthcare organizations in taking the pulse of their community prior to the start of capital improvement projects. A
Engaging Learners Across Health Professions in Improving Care Together
 Session A17 / B17 These presenters have nothing to disclose Engaging Learners Across Health Professions in Improving Care Together Tuesday December 11, 2012 Objectives After this session, participants
Session A17 / B17 These presenters have nothing to disclose Engaging Learners Across Health Professions in Improving Care Together Tuesday December 11, 2012 Objectives After this session, participants
A Quiz. I am comfortable going to any healthcare provider or hospital in my city/town.
 A Quiz I am comfortable going to any healthcare provider or hospital anywhere in the country. I am comfortable going to any healthcare provider or hospital in my city/town. I am comfortable going to my
A Quiz I am comfortable going to any healthcare provider or hospital anywhere in the country. I am comfortable going to any healthcare provider or hospital in my city/town. I am comfortable going to my
Josie King Foundation.
 www.josieking.org INTRODUCTION TO PATIENT SAFETY Session author: Victoria S. Kaprielian, MD Josie s Story: A Patient safety curriculum Victoria S. Kaprielian, MD, FAAFP Dori T. Sullivan, PhD, RN, NE-BC,
www.josieking.org INTRODUCTION TO PATIENT SAFETY Session author: Victoria S. Kaprielian, MD Josie s Story: A Patient safety curriculum Victoria S. Kaprielian, MD, FAAFP Dori T. Sullivan, PhD, RN, NE-BC,
A Comprehensive Framework for Patient Safety
 These presenters have nothing to disclose A Comprehensive Framework for Patient Safety Allan Frankel, MD and Carol Haraden, PhD 8 October 2015 A Framework for a System of Safety Objectives 1. Link safety
These presenters have nothing to disclose A Comprehensive Framework for Patient Safety Allan Frankel, MD and Carol Haraden, PhD 8 October 2015 A Framework for a System of Safety Objectives 1. Link safety
THE AMERICAN BOARD OF PATHOLOGY PATIENT SAFETY COURSE APPLICATION
 THE AMERICAN BOARD OF PATHOLOGY PATIENT SAFETY COURSE APPLICATION Requirements: Component I Patient Safety Self-Assessment Program Programs must meet the following criteria to be an ABP approved Patient
THE AMERICAN BOARD OF PATHOLOGY PATIENT SAFETY COURSE APPLICATION Requirements: Component I Patient Safety Self-Assessment Program Programs must meet the following criteria to be an ABP approved Patient
Patient Safety Competency An Imperative for the Nursing Profession ( and everyone else in health care)
 Patient Safety Competency An Imperative for the Nursing Profession ( and everyone else in health care) Diane C. Pinakiewicz, MBA President, National Patient Safety Foundation 2012 NCSBN Attorney / Investigator
Patient Safety Competency An Imperative for the Nursing Profession ( and everyone else in health care) Diane C. Pinakiewicz, MBA President, National Patient Safety Foundation 2012 NCSBN Attorney / Investigator
Quality Improvement Strategy 2017/ /21
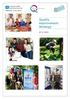 Quality Improvement Strategy 2017/18-2020/21 Contents Section Title Page Number Foreword from Chair and Chief Executive 2 Section 1 Introduction What does Quality mean to us? What do we want to achieve
Quality Improvement Strategy 2017/18-2020/21 Contents Section Title Page Number Foreword from Chair and Chief Executive 2 Section 1 Introduction What does Quality mean to us? What do we want to achieve
Foundations of Patient Safety and Interprofessional Practice Syllabus
 Foundations of Patient Safety and Interprofessional Practice Syllabus ACADEMIC YEAR 2015-2016 COURSE DESCRIPTION This 1 credit course is designed for early health care learners from all OHSU schools and
Foundations of Patient Safety and Interprofessional Practice Syllabus ACADEMIC YEAR 2015-2016 COURSE DESCRIPTION This 1 credit course is designed for early health care learners from all OHSU schools and
5D QAPI from an Operational Approach. Christine M. Osterberg RN BSN Senior Nursing Consultant Pathway Health Pathway Health 2013
 5D QAPI from an Operational Approach Christine M. Osterberg RN BSN Senior Nursing Consultant Pathway Health Objectives Review the post-acute care data agenda. Explain QAPI principles Describe leadership
5D QAPI from an Operational Approach Christine M. Osterberg RN BSN Senior Nursing Consultant Pathway Health Objectives Review the post-acute care data agenda. Explain QAPI principles Describe leadership
Communication and Teamwork for Patient Safety 1.0 Contact Hour Presented by: CEU Professor
 Communication and Teamwork for Patient Safety 1.0 Contact Hour Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2008 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution
Communication and Teamwork for Patient Safety 1.0 Contact Hour Presented by: CEU Professor 7 www.ceuprofessoronline.com Copyright 8 2008 The Magellan Group, LLC All Rights Reserved. Reproduction and distribution
Putting the Patient at the Center of Care
 CMMI Innovation Advisor Paula Suter, Sutter Care at Home: Putting the Patient at the Center of Care Paula Suter, of Sutter Care at Home, joins the Alliance for a discussion of her work with the Center
CMMI Innovation Advisor Paula Suter, Sutter Care at Home: Putting the Patient at the Center of Care Paula Suter, of Sutter Care at Home, joins the Alliance for a discussion of her work with the Center
Expanding Improvement Science Competencies: Successes & Challenges Terry L. Jones RN, PhD. utexas.edu/nursing
 Expanding Improvement Science Competencies: Successes & Challenges Terry L. Jones RN, PhD Objectives Review literature related to educational preparation for IS competencies. Describe an exemplar course
Expanding Improvement Science Competencies: Successes & Challenges Terry L. Jones RN, PhD Objectives Review literature related to educational preparation for IS competencies. Describe an exemplar course
AF4Q and TCAB: An Introduction
 AF4Q and TCAB: An Introduction July 13, 2011 Ellen Interlandi, MHM, RN, NE-BC Patricia Montoya, MPA, BSN 1 What is Aligning Forces for Quality? An unprecedented commitment by the Robert Wood Johnson Foundation
AF4Q and TCAB: An Introduction July 13, 2011 Ellen Interlandi, MHM, RN, NE-BC Patricia Montoya, MPA, BSN 1 What is Aligning Forces for Quality? An unprecedented commitment by the Robert Wood Johnson Foundation
A Comprehensive Framework for Patient Safety
 A Comprehensive Framework for Patient Safety A Framework for a System of Safety Objectives 1. Link safety to organizational strategy and resources 2. Define a culture of safety 3. Apply improvement methods
A Comprehensive Framework for Patient Safety A Framework for a System of Safety Objectives 1. Link safety to organizational strategy and resources 2. Define a culture of safety 3. Apply improvement methods
Innovations for Integrating Quality and Safety in Education and Practice: The QSEN Project
 Innovations for Integrating Quality and Safety in Education and Practice: The QSEN Project Linda Cronenwett, PhD, RN, FAAN Principal Investigator, QSEN Gwen Sherwood, PhD, RN, FAAN Co-Investigator, QSEN
Innovations for Integrating Quality and Safety in Education and Practice: The QSEN Project Linda Cronenwett, PhD, RN, FAAN Principal Investigator, QSEN Gwen Sherwood, PhD, RN, FAAN Co-Investigator, QSEN
National League for Nursing February 5, 2016 Interprofessional Education and Collaborative Practice: The New Forty-Year-Old Field
 National League for Nursing February 5, 2016 Interprofessional Education and Collaborative Practice: The New Forty-Year-Old Field Barbara F. Brandt, PhD, Director Associate Vice President for Education
National League for Nursing February 5, 2016 Interprofessional Education and Collaborative Practice: The New Forty-Year-Old Field Barbara F. Brandt, PhD, Director Associate Vice President for Education
Quality Framework. for a High Performing Health and Wellness System in Nova Scotia
 Quality Framework for a High Performing Health and Wellness System in Nova Scotia Quality Framework for a High Performing Health and Wellness System in Nova Scotia Crown copyright, Province of Nova Scotia,
Quality Framework for a High Performing Health and Wellness System in Nova Scotia Quality Framework for a High Performing Health and Wellness System in Nova Scotia Crown copyright, Province of Nova Scotia,
POPULATION HEALTH MANAGEMENT, PROGRAMS, MODELS, AND TOOLS A. LEE MARTINEZ DBH-C, MA, LAC, CPHQ
 POPULATION HEALTH MANAGEMENT, PROGRAMS, MODELS, AND TOOLS A. LEE MARTINEZ DBH-C, MA, LAC, CPHQ Learning objectives At the conclusion of this session, the participant will be able to: Learning Objective
POPULATION HEALTH MANAGEMENT, PROGRAMS, MODELS, AND TOOLS A. LEE MARTINEZ DBH-C, MA, LAC, CPHQ Learning objectives At the conclusion of this session, the participant will be able to: Learning Objective
Hospital Flow Professional Development Program
 Hospital Flow Professional Development Program April 4-7, 2016 Cambridge, MA Disclaimer: Consistent with the IHI s policy, faculty for this program are expected to disclose at the beginning of their presentation(s)
Hospital Flow Professional Development Program April 4-7, 2016 Cambridge, MA Disclaimer: Consistent with the IHI s policy, faculty for this program are expected to disclose at the beginning of their presentation(s)
Nursing Mission, Philosophy, Curriculum Framework and Program Outcomes
 Nursing Mission, Philosophy, Curriculum Framework and Program Outcomes The mission and philosophy of the Nursing Program are in agreement with the mission and philosophy of the West Virginia Junior College.
Nursing Mission, Philosophy, Curriculum Framework and Program Outcomes The mission and philosophy of the Nursing Program are in agreement with the mission and philosophy of the West Virginia Junior College.
TRINITY HEALTH THE VALUE OF SPIRITUAL CARE
 TRINITY HEALTH THE VALUE OF SPIRITUAL CARE 2015 Trinity Health, Livonia, MI 20555 Victor Parkway Livonia, Michigan 48152?k The Good Samaritan MISSION We, Trinity Health, serve together in the spirit of
TRINITY HEALTH THE VALUE OF SPIRITUAL CARE 2015 Trinity Health, Livonia, MI 20555 Victor Parkway Livonia, Michigan 48152?k The Good Samaritan MISSION We, Trinity Health, serve together in the spirit of
PATIENT AND FAMILY-CENTERED CARE
 PATIENT AND FAMILY-CENTERED CARE Annual Report 2017 PATIENT AND FAMILY-CENTERED CARE We are pleased to present the 2017 Patient and Family-Centered Care (PFCC) Annual Report for Beaumont Health. This inaugural
PATIENT AND FAMILY-CENTERED CARE Annual Report 2017 PATIENT AND FAMILY-CENTERED CARE We are pleased to present the 2017 Patient and Family-Centered Care (PFCC) Annual Report for Beaumont Health. This inaugural
Baptist Health Nurse Leader Competency Model
 Baptist Health Nurse Leader Competency Model Strategic Visionary Systems Thinking Quality Care and Performance Improvement Fiscal and Management Excellence Management of Self and Others 1 - Strategic,
Baptist Health Nurse Leader Competency Model Strategic Visionary Systems Thinking Quality Care and Performance Improvement Fiscal and Management Excellence Management of Self and Others 1 - Strategic,
Design Principles for Learning and Caring in Patient-Centered Primary Care Homes
 The H.R. Bob Brettell, MD, Memorial Lectureship January 29, 2013 Design Principles for Learning and Caring in Patient-Centered Primary Care Homes Judith L. Bowen, MD, FACP Professor of Medicine Oregon
The H.R. Bob Brettell, MD, Memorial Lectureship January 29, 2013 Design Principles for Learning and Caring in Patient-Centered Primary Care Homes Judith L. Bowen, MD, FACP Professor of Medicine Oregon
Quality Improvement Developing Psychology s QI Capability
 Quality Improvement Developing Psychology s QI Capability APPIC May 2016 Liza Bonin, Ph.D. labonin@texaschildrens.org Disclosure UpToDate clinical decision support resource Wolters Kluwer Health UpToDate
Quality Improvement Developing Psychology s QI Capability APPIC May 2016 Liza Bonin, Ph.D. labonin@texaschildrens.org Disclosure UpToDate clinical decision support resource Wolters Kluwer Health UpToDate
Leveraging Health Care IT Investment
 Leveraging Health Care IT Investment A Harvard Business Review Webinar featuring David M. Cutler and Robert S. Huckman Sponsored by OVERVIEW In recent years, health care organizations have made massive
Leveraging Health Care IT Investment A Harvard Business Review Webinar featuring David M. Cutler and Robert S. Huckman Sponsored by OVERVIEW In recent years, health care organizations have made massive
Transformational Patient Care Redesign Project
 Transformational Patient Care Redesign Project Kaveh Houshmand Azad 1 Summary In 2008 2009, Providence Holy Cross Medical Center, a 340- bed hospital located in Mission Hills, California embarked upon
Transformational Patient Care Redesign Project Kaveh Houshmand Azad 1 Summary In 2008 2009, Providence Holy Cross Medical Center, a 340- bed hospital located in Mission Hills, California embarked upon
Engaging Leaders: From Turf Wars to Appreciative Inquiry
 Engaging Leaders: From Turf Wars to Appreciative Inquiry Principles of Leadership for a Quality and Safety Culture Harvard Safety Certificate Program 2010 Gwen Sherwood, PhD, RN, FAAN Gwen Sherwood, PhD,
Engaging Leaders: From Turf Wars to Appreciative Inquiry Principles of Leadership for a Quality and Safety Culture Harvard Safety Certificate Program 2010 Gwen Sherwood, PhD, RN, FAAN Gwen Sherwood, PhD,
Patient Safety Executive Development Program
 Patient Safety Executive Development Program March 2-8, 2017 Cambridge, MA Consistent with the IHI's policy, faculty for this conference are expected to disclose at the beginning of their presentation(s),
Patient Safety Executive Development Program March 2-8, 2017 Cambridge, MA Consistent with the IHI's policy, faculty for this conference are expected to disclose at the beginning of their presentation(s),
Unit Based Culture of Safety and Learning. Owensboro Health March, 2017
 Unit Based Culture of Safety and Learning Owensboro Health March, 2017 Owensboro Health 477 Bed Regional Hospital 32 Bed ICU 30 Transitional Care Beds Level III Trauma Center Level III NICU Largest employer
Unit Based Culture of Safety and Learning Owensboro Health March, 2017 Owensboro Health 477 Bed Regional Hospital 32 Bed ICU 30 Transitional Care Beds Level III Trauma Center Level III NICU Largest employer
Select the correct response and jot down your rationale for choosing the answer.
 UNC2 Practice Test 2 Select the correct response and jot down your rationale for choosing the answer. 1. If data are plotted over time, the resulting chart will be a (A) Run chart (B) Histogram (C) Pareto
UNC2 Practice Test 2 Select the correct response and jot down your rationale for choosing the answer. 1. If data are plotted over time, the resulting chart will be a (A) Run chart (B) Histogram (C) Pareto
Presented by Kay Bensing, MA, RN
 Presented by Kay Bensing, MA, RN At the end of this 1-hour session, participants will be able to: Discuss how healthcare consumers evaluate the quality of the healthcare they receive Identify goals for
Presented by Kay Bensing, MA, RN At the end of this 1-hour session, participants will be able to: Discuss how healthcare consumers evaluate the quality of the healthcare they receive Identify goals for
An Opportunity Guide and Prospectus for Industry, Associations, and Foundations ihi.org
 Engaging with the Institute for Healthcare Improvement An Opportunity Guide and Prospectus for Industry, Associations, and Foundations Go Get Your Hat An Irish proverb says, When you come upon a wall,
Engaging with the Institute for Healthcare Improvement An Opportunity Guide and Prospectus for Industry, Associations, and Foundations Go Get Your Hat An Irish proverb says, When you come upon a wall,
Fundamentals of Health Care Improvement
 Fundamentals of Health Care Improvement A Guide to Improving Your Patients Care Gregory S. Ogrinc, MD, MS Linda A. Headrick, MD, MS, FACP Amy J. Barton, PhD, RN, FAAN, ANEF Mary A. Dolansky, PhD, RN, FAAN
Fundamentals of Health Care Improvement A Guide to Improving Your Patients Care Gregory S. Ogrinc, MD, MS Linda A. Headrick, MD, MS, FACP Amy J. Barton, PhD, RN, FAAN, ANEF Mary A. Dolansky, PhD, RN, FAAN
Quality & Patient Safety
 QHI INTEGRATED CURRICULUM Quality & Patient Safety INTEGRATED CURRICULUM April 2015 QUALITY & PATIENT SAFETY INTEGRATED CURRICULUM Table of Contents Introduction... 3... 4 QHI Integrated Curriculum Certificates...
QHI INTEGRATED CURRICULUM Quality & Patient Safety INTEGRATED CURRICULUM April 2015 QUALITY & PATIENT SAFETY INTEGRATED CURRICULUM Table of Contents Introduction... 3... 4 QHI Integrated Curriculum Certificates...
Text-based Document. Building a Culture of Safety: Aligning innovative leadership rounding and staff driven hourly rounding strategies
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
INSERT ORGANIZATION NAME
 INSERT ORGANIZATION NAME Quality Management Program Description Insert Year SAMPLE-QMProgramDescriptionTemplate Page 1 of 13 Table of Contents I. Overview... Purpose Values Guiding Principles II. III.
INSERT ORGANIZATION NAME Quality Management Program Description Insert Year SAMPLE-QMProgramDescriptionTemplate Page 1 of 13 Table of Contents I. Overview... Purpose Values Guiding Principles II. III.
2010 Pittsburgh Regional Health Initiative
 Pay for Performance Summit Karen Wolk Feinstein, PhD President and Chief Executive Officer Jewish Healthcare Foundation and Pittsburgh Regional Health Initiative San Francisco, California March 8, 2010
Pay for Performance Summit Karen Wolk Feinstein, PhD President and Chief Executive Officer Jewish Healthcare Foundation and Pittsburgh Regional Health Initiative San Francisco, California March 8, 2010
Value of Safety Improvement Collaboratives for Home Care: Strategies and Outcomes
 Value of Safety Improvement Collaboratives for Home Care: Strategies and Outcomes Presented by: VIRGINIA FLINTOFT, Manager, Central Measurement Team, Canadian Patient Safety Institute NARDIA BROWN, Clinical
Value of Safety Improvement Collaboratives for Home Care: Strategies and Outcomes Presented by: VIRGINIA FLINTOFT, Manager, Central Measurement Team, Canadian Patient Safety Institute NARDIA BROWN, Clinical
Working with trainees to turn quality improvement into scholarship and dissemination
 Working with trainees to turn quality improvement into scholarship and dissemination James Moses, MD, MPH Chief Quality Officer, Boston Medical Center Academic Advisor, Institute for Healthcare Improvement
Working with trainees to turn quality improvement into scholarship and dissemination James Moses, MD, MPH Chief Quality Officer, Boston Medical Center Academic Advisor, Institute for Healthcare Improvement
Learning from the Patient Safety Champions November 24, 2017
 Learning from the Patient Safety Champions November 24, 2017 1 Audio for this webinar must be accessed via telephone: Dial In Number: 1-888-289-4573 Participant Access Code: 1339131 This webinar will be
Learning from the Patient Safety Champions November 24, 2017 1 Audio for this webinar must be accessed via telephone: Dial In Number: 1-888-289-4573 Participant Access Code: 1339131 This webinar will be
Expanding Role of the HIM Professional: Where Research and HIM Roles Intersect
 Page 1 of 6 The Expanding Role of the HIM Professional: Where Research and HIM Roles Intersect by Jessica Bailey, PhD, RHIA, CCS, and William Rudman, PhD Abstract This article examines the evolving role
Page 1 of 6 The Expanding Role of the HIM Professional: Where Research and HIM Roles Intersect by Jessica Bailey, PhD, RHIA, CCS, and William Rudman, PhD Abstract This article examines the evolving role
A Comprehensive Framework for Patient Safety, Reliability and Clinical Excellence
 14 November 2016 Oslo, Norway A Comprehensive Framework for Patient, and Clinical Excellence Frank Federico A Framework 1. Link safety and reliability to organizational strategy and resources 2. Define
14 November 2016 Oslo, Norway A Comprehensive Framework for Patient, and Clinical Excellence Frank Federico A Framework 1. Link safety and reliability to organizational strategy and resources 2. Define
Program Director Dr. Leonard Friedman
 School of Public Health and Health Services Department of Health Services and Leadership Master of Health Services Administration 2011-2012 Note: All curriculum revisions will be updated immediately on
School of Public Health and Health Services Department of Health Services and Leadership Master of Health Services Administration 2011-2012 Note: All curriculum revisions will be updated immediately on
Delivering on A Promise to Learn A Commitment to Act. The National Patient Safety Collaborative learning event
 Delivering on A Promise to Learn A Commitment to Act The National Patient Safety Collaborative learning event Dr Mike Durkin NHS National Director of Patient Safety NHS Improvement Aidan Fowler Director
Delivering on A Promise to Learn A Commitment to Act The National Patient Safety Collaborative learning event Dr Mike Durkin NHS National Director of Patient Safety NHS Improvement Aidan Fowler Director
Through the Veil of Language:
 Through the Veil of Language: Safe, Effective and Humanistic Care for Patients with Limited English Proficiency Alexander Green, MD, MPH Associate Director, The Disparities Solutions Center The Mongan
Through the Veil of Language: Safe, Effective and Humanistic Care for Patients with Limited English Proficiency Alexander Green, MD, MPH Associate Director, The Disparities Solutions Center The Mongan
Iora Health is looking for a primary care physician for new practices in Boston, Las Vegas, New York City and the American Southwest.
 Unique Opportunities for a Primary Care (Internal Medicine, Med/Peds or Family Practice) Physician at Innovative New Medical Practices in Boston, Las Vegas, New York City and the Southwest Introduction
Unique Opportunities for a Primary Care (Internal Medicine, Med/Peds or Family Practice) Physician at Innovative New Medical Practices in Boston, Las Vegas, New York City and the Southwest Introduction
Results tell the story
 Sponsor: Discover why leaders at 1400+ hospitals have made this webinar series the #1 HCAHPS education program in America! Results tell the story Webinar Series Faculty: Brian Lee, CSP Founder of CLS David
Sponsor: Discover why leaders at 1400+ hospitals have made this webinar series the #1 HCAHPS education program in America! Results tell the story Webinar Series Faculty: Brian Lee, CSP Founder of CLS David
The State of Patient Safety: 15 Years Since the IOM Report To Err Is Human EXPERT PANEL
 The State of Patient Safety: 15 Years Since the IOM Report To Err Is Human EXPERT PANEL Co-Chairs Donald M. Berwick, MD, MPP Emeritus and Senior Fellow Lecturer, Department of Health Care Policy Harvard
The State of Patient Safety: 15 Years Since the IOM Report To Err Is Human EXPERT PANEL Co-Chairs Donald M. Berwick, MD, MPP Emeritus and Senior Fellow Lecturer, Department of Health Care Policy Harvard
Bachelor of Science (BS) in Health Care Administration with a specialization in. Health Information Management
 Bachelor of Science (BS) in Health Care Administration with a specialization in Health Information Management Effective January 8, 2018 Bachelor of Science (BS) in Health Care Administration with a specialization
Bachelor of Science (BS) in Health Care Administration with a specialization in Health Information Management Effective January 8, 2018 Bachelor of Science (BS) in Health Care Administration with a specialization
PREPARING FOR THE CLER SITE VISIT FOR BEN TAUB GENERAL HOSPITAL
 PREPARING FOR THE CLER SITE VISIT FOR BEN TAUB GENERAL HOSPITAL 1 Goals and Objectives Overview the Clinical Learning Environment Review (CLER) program Discuss the concept of maintaining a culture of readiness
PREPARING FOR THE CLER SITE VISIT FOR BEN TAUB GENERAL HOSPITAL 1 Goals and Objectives Overview the Clinical Learning Environment Review (CLER) program Discuss the concept of maintaining a culture of readiness
UNIVERSITY OF MISSISSIPPI MEDICAL CENTER PATIENT SAFETY PLAN
 UNIVERSITY OF MISSISSIPPI MEDICAL CENTER PATIENT SAFETY PLAN 2014 1 PATIENT SAFETY PLAN 2014 PROGRAM GOALS The goal of the Patient Safety Program at University of Mississippi Medical Center (UMMC) is to
UNIVERSITY OF MISSISSIPPI MEDICAL CENTER PATIENT SAFETY PLAN 2014 1 PATIENT SAFETY PLAN 2014 PROGRAM GOALS The goal of the Patient Safety Program at University of Mississippi Medical Center (UMMC) is to
Visit to download this and other modules and to access dozens of helpful tools and resources.
 This is the third module of Coach Medical Home a six-module curriculum designed for practice facilitators who are coaching primary care practices around patient-centered medical home (PCMH) transformation.
This is the third module of Coach Medical Home a six-module curriculum designed for practice facilitators who are coaching primary care practices around patient-centered medical home (PCMH) transformation.
A9/B9: Integrating Patient Safety into Your System s DNA
 A9/B9: Integrating Patient Safety into Your System s DNA Doug Bonacum Frank Federico A9 Moderator: Abdulaziz Darwish B9 Moderator: Ibrahim Fawzy Hassan Saturday 26th April A9: 11:00 12:15 B9: 13:30 14:45
A9/B9: Integrating Patient Safety into Your System s DNA Doug Bonacum Frank Federico A9 Moderator: Abdulaziz Darwish B9 Moderator: Ibrahim Fawzy Hassan Saturday 26th April A9: 11:00 12:15 B9: 13:30 14:45
Incident Reporting Systems and Future Strategies for Patient Safety Improvement
 WHITE PAPER: Incident Reporting Systems and Future Strategies for Patient Safety Improvement Author: Datix Date: 2016/17 Driving down harm How can healthcare providers most successfully pursue the goal
WHITE PAPER: Incident Reporting Systems and Future Strategies for Patient Safety Improvement Author: Datix Date: 2016/17 Driving down harm How can healthcare providers most successfully pursue the goal
Copyright 2011 Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited.
 32 May 2011 Nursing Management Future of Nursing special Leadership at all levels By Tim Porter-O Grady, DM, EdD, ScD(h), FAAN This five-part editorial series examines the Institute of Medicine s (IOM)
32 May 2011 Nursing Management Future of Nursing special Leadership at all levels By Tim Porter-O Grady, DM, EdD, ScD(h), FAAN This five-part editorial series examines the Institute of Medicine s (IOM)
TeamSTEPPS TM National Implementation
 TeamSTEPPS TM National Implementation Implementing TeamSTEPPS in Critical Access Hospitals Katherine Jones, PT, PhD University of Nebraska Medical Center Implementing TeamSTEPPS in Critical Access Hospitals
TeamSTEPPS TM National Implementation Implementing TeamSTEPPS in Critical Access Hospitals Katherine Jones, PT, PhD University of Nebraska Medical Center Implementing TeamSTEPPS in Critical Access Hospitals
Identifying and Preventing Medical Errors in Patients with Limited-English Proficiency: New Tools for the Field
 Welcome to the Disparities Solutions Center s Web Seminar Series Identifying and Preventing Medical Errors in Patients with Limited-English Proficiency: New Tools for the Field Tuesday, October16, 2012
Welcome to the Disparities Solutions Center s Web Seminar Series Identifying and Preventing Medical Errors in Patients with Limited-English Proficiency: New Tools for the Field Tuesday, October16, 2012
Meaningful Patient and Family Partnerships: Evidence and Leadership
 Meaningful Patient and Family Partnerships: Evidence and Leadership 6 th International Conference on Patient- and Family-Centered Care Westin Bayshore Hotel, Vancouver, BC August 7, 2014 cfhi-fcass.ca
Meaningful Patient and Family Partnerships: Evidence and Leadership 6 th International Conference on Patient- and Family-Centered Care Westin Bayshore Hotel, Vancouver, BC August 7, 2014 cfhi-fcass.ca
Patient Advocate Certification Board. Competencies and Best Practices required for a Board Certified Patient Advocate (BCPA)
 Patient Advocate Certification Board Competencies and Best Practices required for a Board Certified Patient Advocate (BCPA) Attribution The Patient Advocate Certification Board (PACB) recognizes the importance
Patient Advocate Certification Board Competencies and Best Practices required for a Board Certified Patient Advocate (BCPA) Attribution The Patient Advocate Certification Board (PACB) recognizes the importance
Improving Clinical Flow ECHO Collaborative Change Package
 Primary Drivers (driver diagram) Change Concepts Change Ideas Examples, Tips, and Resources Engaged Leadership Develop culture for transformation Use walk-arounds and attendance at team meetings to talk
Primary Drivers (driver diagram) Change Concepts Change Ideas Examples, Tips, and Resources Engaged Leadership Develop culture for transformation Use walk-arounds and attendance at team meetings to talk
UPMC Passavant POLICY MANUAL
 UPMC Passavant POLICY MANUAL SUBJECT: Organizational Plan, Patient Care Services POLICY: 200.142 DATE: November 2015 INDEX TITLE: Nursing MISSION: Patient Care Services at UPMC Passavant is integral to
UPMC Passavant POLICY MANUAL SUBJECT: Organizational Plan, Patient Care Services POLICY: 200.142 DATE: November 2015 INDEX TITLE: Nursing MISSION: Patient Care Services at UPMC Passavant is integral to
Quality Improvement in Health and Social Care
 Some Fundamentals on Quality Improvement in Health and Social Care Towards a Shared Understanding EPSO, Reykjavik, 2017-09-26 Johan Thor, MD, MPH, PhD Associate Professor E-mail: johan.thor@ju.se The death
Some Fundamentals on Quality Improvement in Health and Social Care Towards a Shared Understanding EPSO, Reykjavik, 2017-09-26 Johan Thor, MD, MPH, PhD Associate Professor E-mail: johan.thor@ju.se The death
Communication Challenges Overcoming the Barriers to Improve Quality. Presented by: Christy Brinkman LNHA Laura Seleen RN
 Communication Challenges Overcoming the Barriers to Improve Quality Presented by: Christy Brinkman LNHA Laura Seleen RN 6-16-16 Objectives The participant will be able to identify a process to follow to
Communication Challenges Overcoming the Barriers to Improve Quality Presented by: Christy Brinkman LNHA Laura Seleen RN 6-16-16 Objectives The participant will be able to identify a process to follow to
Using the PFCC Methodology and Practice: Creating the Ideal Patient Centered Medical Home
 Using the PFCC Methodology and Practice: Creating the Ideal Patient Centered Medical Home Michael Celender Anthony M. DiGioia, MD and PFCC Partners @ The Innovation Center of UPMC February 28, 2012 (celendermh@upmc.edu)
Using the PFCC Methodology and Practice: Creating the Ideal Patient Centered Medical Home Michael Celender Anthony M. DiGioia, MD and PFCC Partners @ The Innovation Center of UPMC February 28, 2012 (celendermh@upmc.edu)
Your Guide to IHI s. Upcoming Programs. ihi.org/education
 Your Guide to IHI s Upcoming Programs 2018 ihi.org/education We can help you in 2018 Your mission to improve health and health care is our mission, too. In any community or clinical setting that you work
Your Guide to IHI s Upcoming Programs 2018 ihi.org/education We can help you in 2018 Your mission to improve health and health care is our mission, too. In any community or clinical setting that you work
To err is human. When things go wrong: apology and communication. Apology and communication position statement
 When things go wrong: apology and communication Kristi Eldredge R.N., J.D., CPHRM Senior Risk and Safety Consultant Fresident To err is human position statement To err is human. Mistakes are part of the
When things go wrong: apology and communication Kristi Eldredge R.N., J.D., CPHRM Senior Risk and Safety Consultant Fresident To err is human position statement To err is human. Mistakes are part of the
NCQA WHITE PAPER. NCQA Accreditation of Accountable Care Organizations. Better Quality. Lower Cost. Coordinated Care
 NCQA Accreditation of Accountable Care Organizations Better Quality. Lower Cost. Coordinated Care. NCQA WHITE PAPER NCQA Accreditation of Accountable Care Organizations Accountable Care Organizations (ACO)
NCQA Accreditation of Accountable Care Organizations Better Quality. Lower Cost. Coordinated Care. NCQA WHITE PAPER NCQA Accreditation of Accountable Care Organizations Accountable Care Organizations (ACO)
THE DNP AT THE UNIVERSITY OF
 UNIVERSITY OF MARYLAND The University of Maryland was established in Baltimore in 1807 and is the founding campus of the University System of Maryland. A national leader in health sciences research, public
UNIVERSITY OF MARYLAND The University of Maryland was established in Baltimore in 1807 and is the founding campus of the University System of Maryland. A national leader in health sciences research, public
Creating an Ohio Nurse Competency Model-Based RN Job Description Utilizing Delphi Methodology
 Creating an Ohio Nurse Competency Model-Based RN Job Description Utilizing Delphi Methodology Lisa A. Aurilio, MSN, MBA, RN, NEA-BC Neil L. McNinch, MS, RN Eileen M. Zehe, MSN, RN, SPHR, SHRM-SCP The presenters
Creating an Ohio Nurse Competency Model-Based RN Job Description Utilizing Delphi Methodology Lisa A. Aurilio, MSN, MBA, RN, NEA-BC Neil L. McNinch, MS, RN Eileen M. Zehe, MSN, RN, SPHR, SHRM-SCP The presenters
Care of the Caregiver STARTS and ENDS with full leadership support and involvement!
 Care of the Caregiver STARTS and ENDS with full leadership support and involvement! Care of the caregiver following an unintentional error or near miss should ideally incorporate: Unsafe Acts Algorithm
Care of the Caregiver STARTS and ENDS with full leadership support and involvement! Care of the caregiver following an unintentional error or near miss should ideally incorporate: Unsafe Acts Algorithm
WHITE PAPER. Transforming the Healthcare Organization through Process Improvement
 WHITE PAPER Transforming the Healthcare Organization through Process Improvement The movement towards value-based purchasing models has made the concept of process improvement and its methodologies an
WHITE PAPER Transforming the Healthcare Organization through Process Improvement The movement towards value-based purchasing models has made the concept of process improvement and its methodologies an
Project ECHO: Action for Improvement Elizabeth Clewett, PhD, MBA Cory Sevin, RN, MSN December 13, 2017
 D21/E21 These presenters have nothing to disclose Project ECHO: Action for Improvement Elizabeth Clewett, PhD, MBA Cory Sevin, RN, MSN December 13, 2017 Session Objectives P2 Describe how Project ECHO
D21/E21 These presenters have nothing to disclose Project ECHO: Action for Improvement Elizabeth Clewett, PhD, MBA Cory Sevin, RN, MSN December 13, 2017 Session Objectives P2 Describe how Project ECHO
Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall. Total. Application Analysis 1.
 Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall Application Analysis Total 1. CULTURE 2 12 4 18 A. Assessment of Patient Safety Culture 1. Identify work settings
Cognitive Level Certified Professional in Patient Safety Detailed Content Outline Recall Application Analysis Total 1. CULTURE 2 12 4 18 A. Assessment of Patient Safety Culture 1. Identify work settings
Healthcare 9/15/2017. Learning Outcomes. Transforming Clinical and Fiscal Outcomes through Staff Nurse Driven Change
 Transforming Clinical and Fiscal Outcomes through Staff Nurse Driven Change Marian Altman RN, MS, CNS-BC, CCRN-K,ANP American Association of Critical Care Nurses Clinical Practice Specialist Learning Outcomes
Transforming Clinical and Fiscal Outcomes through Staff Nurse Driven Change Marian Altman RN, MS, CNS-BC, CCRN-K,ANP American Association of Critical Care Nurses Clinical Practice Specialist Learning Outcomes
School of Nursing Philosophy (AASN/BSN/MSN/DNP)
 School of Nursing Mission The mission of the School of Nursing is to educate, enhance and enrich students for evolving professional nursing practice. The core values: The School of Nursing values the following
School of Nursing Mission The mission of the School of Nursing is to educate, enhance and enrich students for evolving professional nursing practice. The core values: The School of Nursing values the following
A Blueprint for Alignment
 A Blueprint for Alignment Engaging Residents in the Quality and Safety Mission of Penn Medicine PJ Brennan, MD Chief Medical Officer, UPHS Jennifer S. Myers, MD Director of Quality and Safety Education
A Blueprint for Alignment Engaging Residents in the Quality and Safety Mission of Penn Medicine PJ Brennan, MD Chief Medical Officer, UPHS Jennifer S. Myers, MD Director of Quality and Safety Education
National Agenda for Action: Patients and Families in Patient Safety Nothing About Me, Without Me *
 The National Patient Safety Foundation National Agenda for Action: Patients and Families in Patient Safety Nothing About Me, Without Me * Executive Summary This summary (and complete document) is a report
The National Patient Safety Foundation National Agenda for Action: Patients and Families in Patient Safety Nothing About Me, Without Me * Executive Summary This summary (and complete document) is a report
RWJMS Strategic Plan
 RWJMS Strategic Plan 2016-2021 Rutgers, The State University of New Jersey Table of Contents Overview 3 Organizational Direction (Mission, Vision, Values) 6 Strategic Priorities Education 11 Research 17
RWJMS Strategic Plan 2016-2021 Rutgers, The State University of New Jersey Table of Contents Overview 3 Organizational Direction (Mission, Vision, Values) 6 Strategic Priorities Education 11 Research 17
2014 QAPI Plan for [Facility Name]
![2014 QAPI Plan for [Facility Name] 2014 QAPI Plan for [Facility Name]](/thumbs/74/70066237.jpg) presented by: Quality Leadership for Long-Term Care 2014 QAPI Plan for [Facility Name] Vision A vision statement is sometimes called a picture of your organization in the future; it is your inspiration
presented by: Quality Leadership for Long-Term Care 2014 QAPI Plan for [Facility Name] Vision A vision statement is sometimes called a picture of your organization in the future; it is your inspiration
Delivering Great Care with High Reliability The Orlando Health Journey
 FE5 These presenters have nothing to disclose Delivering Great Care with High Reliability The Orlando Health Journey December 11, 2017 Frank Federico, RPh Vice President Patricia McGaffigan, RN, MS, CPPS
FE5 These presenters have nothing to disclose Delivering Great Care with High Reliability The Orlando Health Journey December 11, 2017 Frank Federico, RPh Vice President Patricia McGaffigan, RN, MS, CPPS
Health Care Ethics and Safety: A Quality Case for Consumer Engagement April 24, Panelist. Susan Hassmiller, RN, PhD, FAAN
 Health Care Ethics and Safety: A Quality Case for Consumer Engagement April 24, 2018 Introductions Moderator Mary Jo Jerde, MBA, BSN, RN, FAAN Senior Vice President, Center for Clinician Advancement Minnetonka,
Health Care Ethics and Safety: A Quality Case for Consumer Engagement April 24, 2018 Introductions Moderator Mary Jo Jerde, MBA, BSN, RN, FAAN Senior Vice President, Center for Clinician Advancement Minnetonka,
RN to BSN Completion Program Practicum Handbook: NSG 442A NSG 444A NSG 447A
 RN to BSN Completion Program Practicum Handbook: NSG 442A NSG 444A NSG 447A May, 2017 TABLE OF CONTENTS Welcome and Lead Faculty Information 3 Preamble 4 Required Practicum Courses 4 The Mentor Role 5
RN to BSN Completion Program Practicum Handbook: NSG 442A NSG 444A NSG 447A May, 2017 TABLE OF CONTENTS Welcome and Lead Faculty Information 3 Preamble 4 Required Practicum Courses 4 The Mentor Role 5
1875 Connecticut Ave. NW / Suite 650 / Washington, D.C / / fax /
 Testimony of Jane Loewenson Director of Health Policy, National Partnership for Women & Families Before the U.S. House of Representatives Energy & Commerce Subcommittee on Health Hearing on Patient Safety
Testimony of Jane Loewenson Director of Health Policy, National Partnership for Women & Families Before the U.S. House of Representatives Energy & Commerce Subcommittee on Health Hearing on Patient Safety
Journey to an Effective Safety Culture Part I of III Exploring the Role of Culture in Safety Outcomes. Embracing Patient Safety Culture
 White Paper Journey to an Effective Safety Culture Part I of III Exploring the Role of Culture in Safety Outcomes Embracing Patient Safety Culture What is the Purpose of this Series? The purpose of this
White Paper Journey to an Effective Safety Culture Part I of III Exploring the Role of Culture in Safety Outcomes Embracing Patient Safety Culture What is the Purpose of this Series? The purpose of this
POSITIVELY AFFECTING NEONATAL OUTCOMES WORLDWIDE
 POSITIVELY AFFECTING NEONATAL OUTCOMES WORLDWIDE Our network includes 1200+ centers across 30+ countries, collecting critical information on 2.5+ million infants and 72.5+ million patient days. 1 VERMONT
POSITIVELY AFFECTING NEONATAL OUTCOMES WORLDWIDE Our network includes 1200+ centers across 30+ countries, collecting critical information on 2.5+ million infants and 72.5+ million patient days. 1 VERMONT
Table of Contents. Introduction: Letter to managers... viii. How to use this book... x. Chapter 1: Performance improvement as a management tool...
 Table of Contents Introduction: Letter to managers......................... viii How to use this book.................................. x Chapter 1: Performance improvement as a management tool..................................
Table of Contents Introduction: Letter to managers......................... viii How to use this book.................................. x Chapter 1: Performance improvement as a management tool..................................
Running head: CLINICAL/PRACTICUM LEARNING ANALYSIS PAPER
 Clinical/Practicum Learning Analysis 1 Running head: CLINICAL/PRACTICUM LEARNING ANALYSIS PAPER Clinical/Practicum Learning Analysis Paper Carol A. Lamoureux-Lewallen Briar Cliff University Clinical/Practicum
Clinical/Practicum Learning Analysis 1 Running head: CLINICAL/PRACTICUM LEARNING ANALYSIS PAPER Clinical/Practicum Learning Analysis Paper Carol A. Lamoureux-Lewallen Briar Cliff University Clinical/Practicum
Faculty Session 1 Time Title Objectives Tied to others Brent James, MD. Always together w/pragmatic 1. Always together w/modelling Processes 1
 Faculty Session Time Title Objectives Tied to others Managing Clinical Processes: An Definition of processes Always together w/ Methods Introduction to Clinical QI Quality improvement as the science of
Faculty Session Time Title Objectives Tied to others Managing Clinical Processes: An Definition of processes Always together w/ Methods Introduction to Clinical QI Quality improvement as the science of
The Clinical Learning Environment Review (CLER) Program Update
 Accreditation Council for Graduate Medical Education The Clinical Learning Environment Review (CLER) Program Update October 10, 2013 Updates CLER program development Early observations CLER Evaluation
Accreditation Council for Graduate Medical Education The Clinical Learning Environment Review (CLER) Program Update October 10, 2013 Updates CLER program development Early observations CLER Evaluation
EXECUTIVE SUMMARY. The Military Health System. Military Health System Review Final Report August 29, 2014
 EXECUTIVE SUMMARY On May 28, 2014, the Secretary of Defense ordered a comprehensive review of the Military Health System (MHS). The review was directed to assess whether: 1) access to medical care in the
EXECUTIVE SUMMARY On May 28, 2014, the Secretary of Defense ordered a comprehensive review of the Military Health System (MHS). The review was directed to assess whether: 1) access to medical care in the
Oregon Health & Science University. Vision v OHSU Strategic Plan
 Oregon Health & Science University Vision 2020 v. 2013 OHSU Strategic Plan 2013 2017 Adopted by the OHSU Board of Directors January 2014 Strategic Planning at OHSU Vision 2020, OHSU s strategic plan, was
Oregon Health & Science University Vision 2020 v. 2013 OHSU Strategic Plan 2013 2017 Adopted by the OHSU Board of Directors January 2014 Strategic Planning at OHSU Vision 2020, OHSU s strategic plan, was
Integrated Leadership for Hospitals and Health Systems: Principles for Success
 Integrated Leadership for Hospitals and Health Systems: Principles for Success In the current healthcare environment, there are many forces, both internal and external, that require some physicians and
Integrated Leadership for Hospitals and Health Systems: Principles for Success In the current healthcare environment, there are many forces, both internal and external, that require some physicians and
