Blood clot prevention. A guide for patients and carers
|
|
|
- Joanna McCormick
- 6 years ago
- Views:
Transcription
1 Blood clot prevention A guide for patients and carers
2
3 Contents Introduction 1 What is a venous thromboembolism (VTE)? 1 What is a deep vein thrombosis (also known as a DVT)? 1 What is a pulmonary embolism (also known as a PE)? 2 What are the signs and symptoms of two types a VTE? 3 Who is at risk of a VTE? 3 Will my risk of a VTE be assessed while I am in hospital? 4 When I am in hospital what will be done to help prevent a VTE? 5 When I am at home how can I prevent a VTE 6 What anticoagulant might I be offered? 6 I am taking warfarin and have been prescribed anti-cancer medicines (chemotherapy), what do I need to consider? 6 Can I take other medicines whilst on anticoagulant therapy? 7 Should I avoid any particular food or drink 7 Are there any side effects associated with anticoagulants? 7 Monitoring your anticoagulation treatment 7 How anticoagulants may affect dental treatment 8 Taking anticoagulants if you are planning pregnancy or become pregnant 8 How anticogulants may affect activities such as sport and travel 8
4 If you have missed a dose of anticoagulant 8 Try to avoid injury while using anticoagulant 8 If I am taking a anticoagulant how long should I continue to take it? 8 Anti-embolic stockings 9 How long will I need to wear the anti-embolic stockings for? 9 Wearing instructions 10 Looking after your anti-embolic stockings 10 What are the risks of wearing anti-embolic stockings? 10 What should I do if I think I have a VTE? 11 If a VTE is diagnosed 11 Who do I contact if I have any problems with the stockings or anticoagulants? 12 Resources 12 Notes and questions 13
5 Introduction Having cancer can increase the risk of developing a blood clot. The risk varies across different types of cancer and the risk factors can change over time, this can be based on your general health and the specific types of cancer treatment received. Although not all blood clots are preventable, we want you to be assured that we will minimise the risk during your treatment and care. This booklet explains how you can help us to reduce the risk. It covers how blood clots develop, who is most at risk, and the signs to look out for. What is a venous thromboembolism (VTE)? VTE is one of a number of medical terms used when talking about blood clots. VTE is the collective name for deep vein thrombosis (DVT) and pulmonary embolism (PE). What is deep vein thrombosis (also known as a DVT)? This is a blood clot which develops in a deep vein, most commonly in the leg or pelvis (less commonly in the deep veins of your arms but this can occur if you have a PICC line). 1
6 If a blood clot forms in a deep vein in the leg or pelvis it can block the blood flow within the vein. This can result in the leg becoming swollen and painful. What is a pulmonary embolism (also known as a PE)? Sometimes part of the blood clot causing the DVT separates and travels towards the heart and onwards to the lungs. A pulmonary embolism is a blood clot in the blood vessels that supply the lungs. Pulmonary embolism can be life threatening and therefore needs urgent medical attention. If you develop a DVT/PE you may have to take anticoagulation (blood thinning) treatment for 3-6 months, possibly longer. The doctors will keep you informed of how long you will need anticoagulation treatment. 2
7 What are the signs and symptoms of two types of VTE? If you experience the following problems you may be suffering from a DVT sometimes there are no symptoms pain, swelling and tenderness in a leg discolouration of the leg, red, blue or purple changes difficulty weight-bearing on the affected leg If you experience the following problems you may be suffering from a PE: coughing up small amounts of blood chest pain which is made worse when you take a deep breath shortness of breath If you experience any of these symptoms please urgently attend the nearest Accident and Emergency department (A&E). Who is at risk of a VTE? Any patient can be at risk of developing a VTE. However, there are a number of factors that can increase your chance of this happening. Your risk may be increased if you: have cancer or are undergoing cancer treatment 3
8 have had a previous clot are less mobile than usual for more than three days i.e. confined to or spend a large part of the day in bed or in a chair are due to have surgery are over 60 years old are over weight smoke have previously had a VTE have certain blood conditions such as clotting disorders are using an oestrogen-containing contraceptive (combined pill) are taking hormone replacement tablets (HRT) are dehydrated are pregnant have varicose veins If you are taking an oestrogen- containing oral contraceptive (the combined pill) or having hormone replacement therapy (HRT) and you will be having an operation, your healthcare team will advise you to consider stopping these drugs temporarily four weeks before you have your operation. This will be explained to you at your pre-assessment. If you are sexually active during this time we would strongly recommend that condoms are used. If you are having an operation and you are already taking a drug that thins the blood (for example, aspirin) your healthcare team should assess the risks and benefits of stopping the drug one week before your operation. This will be explained to you at your pre-assessment appointment. After your operation ask the medical team when and if you should restart your medications. Will my risk of a VTE be assessed while I am in hospital? Hospital staff will assess your risk of developing a VTE within 24 hours of your admission. You will be re-assessed if your 4
9 condition or planned care has changed in any way. If you are having surgery, you may also be assessed at your pre-admission assessment appointment. If you are at risk of developing a VTE your healthcare team should also assess whether bleeding might be a problem during your hospital treatment. If the risk of bleeding outweighs the risk of VTE you will not be offered an anticoagulation drug. If your risk of DVT is high but you cannot take anticoagulant drugs and are not able to use anti-embolic stockings you may be offered a temporary vena cava filter. This is an umbrella shaped device that is inserted into a large vein to trap any blood clots and stop them moving towards the lung. This is usually removed following surgery. When I am in hospital what will be done to help prevent a VTE? Stay hydrated if you are allowed to do so, drink plenty of fluid. However, if you are not allowed to do this, the doctors will give you fluids via a vein. Move around keep mobile as much as you can. The physiotherapist will teach you some appropriate leg exercise. Anti-embolic stockings If the doctor decides that you would be suitable for these, the nursing staff will fit you with a pair of stockings. Intermittent calf pumps some patients who have surgery will have a special device which fits like a cuff around each calf (similar to a blood pressure cuff). This will inflate and deflate alternately. These are designed to help prevent clot formation in the calf. Medication (anticoagulants) your doctor might consider it necessary to prescribe you an anticoagulant drug to reduce your risk of developing a blood clot. This is called prophylaxis. Depending on the type of surgery you may be asked to continue this medication for 28 days following the operation. 5
10 Not all methods mentioned above are appropriate for all patients. Your doctor will assess which methods are most suitable for you as an individual. When I am at home how can I help prevent a VTE? Drink plenty of fluids Stop smoking Keep mobile especially on long journeys by performing leg exercises Maintain a healthy weight Consider wearing anti embolic stockings if your mobility is limited What anticoagulant might I be offered? The anti-coagulant most often used is heparin. We usually offer patients a type of heparin injection called Tinzaparin. This is injected under the skin. Heparin comes from animals, if you have any concerns about using animal products, please tell your doctor. If you are already taking anticoagulation medication such as warfarin or Rivaroxiban please tell your doctor. I am taking warfarin and have been prescribed anti-cancer medicines (chemotherapy), what do I need to consider? Like other medications, anti-cancer medicines can sometimes affect how well your warfarin works. Your doctor or nurse will discuss this with you when starting treatment for cancer and will often change your anticoagulation treatment to heparin (Tinzaparin). If your doctor decides to keep you on warfarin it is important to let your GP or anticoagulant dosing service know that you are starting anti-cancer treatment. They may want to temporarily adjust the dose or increase the frequency of your blood tests (INR) to ensure that the warfarin is still working safely. 6
11 Can I take other medicines whilst on anticoagulant therapy? When buying over the counter medicines, tell the pharmacist that you are taking anticoagulants. Also tell any doctor or nurse who is prescribing, or making changes to, your medication that you are taking anticoagulants. If you have been prescribed any new medication, you should inform the team who prescribed your anticoagulant. Medicines containing aspirin should only be taken if prescribed by your doctor or hospital consultant. Ibuprofen based medicines should also be avoided. You can take paracetamol. Should I avoid any particular food or drink? You should eat a well balanced diet and maintain a healthy weight. You should not consume more than two units of alcohol per day. Avoid binge drinking as it interferes with anticoagulant treatment. Up to two units of alcohol every day is better then a large amount once a week. Are there any side effects associated with anticoagulants? The possible side effects include: Skin rash or allergy Bleeding HITS (heparin induced thrombocytopenia) very rarely patients can develop this condition which affects the platelet count (this will be monitored through blood tests) If you have kidney failure you may be offered a different type of heparin to protect your kidneys. Monitoring your anticoagulation treatment The medical team may take a blood test before you start having this medication and while you are having it. This is to check the level of the clotting cells (platelets) and potassium in your blood. If you are an older person your doctor may also check how well your kidneys are working. 7
12 How anticoagulants may affect dental treatment If you are going to have surgery or dental work, tell your prescriber or health care professional that you have received anticoagulants prior to any treatment. Taking anticoagulants if you are planning pregnancy or become pregnant If you are either pregnant or think you may be so, please tell your doctor. How anticogulants may affect activities such as sport and travel You should avoid contact sport. If you have missed a dose of anticoagulant Give the missed dose as soon as you remember, unless it is almost time for the next dose. Do not use double doses. Try to avoid injury while taking anticoagulants Take special care brushing or flossing your teeth, shaving, cutting your fingernails or toe nails, and when using sharp objects. Report any injuries to your prescriber or health care professional. If I am taking a anticoagulant how long should I continue to take it? Your doctor will assess whether or not you will need to continue with the medicine or injections after you leave hospital. This depends on an assessment of the risk of your developing a clot. It will also depend on the nature of any surgery that you may have undergone. If you are to continue with the medication we will give the appropriate amount of medicine/injections to continue at home. 8
13 Anti-embolic stockings Anti-embolic stockings provide support to the muscles in your leg to help the flow of blood in your veins. Anti-embolic stockings are not suitable for all people. You should not wear them if you have had a recent stroke or have peripheral arterial disease, peripheral neuropathy, recent leg skin grafts, eczema, fragile skin or very swollen legs. As an inpatient you may be provided thigh or knee length anti-embolic stockings, the nursing team will measure your legs to ensure the correct fit. If you would like to consider antiembolic stockings as an outpatient, for example, because you re increasingly tired and less mobile, it is important to speak to your keyworker or the MDU staff first. This is because anti-embolic stockings may not be an appropriate or safe option for you. Below the knee Above the knee How long will I need to wear the anti-embolic stockings for? You will need to wear your stockings day and night for the duration of your stay in hospital. If you have been given stockings to prevent VTE after leaving hospital you should continue to wear these until you regain your previous level of mobility. If you are receiving anti-cancer treatment and you notice your mobility becoming restricted you could consider buying specialist stockings from your local pharmacy, or speak to the staff in the MDU/OPD at your next appointment. 9
14 Wearing instructions If you have difficulty putting the stockings on please ask your nurse to help you. The stockings should feel firm but should also be comfortable. If they feel too tight or too loose please tell your nurse. They should be wrinkle free and worn throughout the day and night. Do not roll the stockings down as this could restrict blood flow. You should remove your stockings daily for up to 30 minutes. During this time you can wash and moisturize your legs with cream (if you have an existing skin condition please ask your doctor as to which is the most appropriate moisturiser to use). During the time your stockings are removed you should check the condition of your skin. If you are experiencing any of the following please inform your nurse immediately: pain, numbness, leg swelling or skin problems such as rashes, blistering or discolouration. Looking after your anti-embolic stockings One pair of stockings should be worn daily for three months and then discarded. The stockings should be washed regularly to renew the compression and remove skin flakes and sweat. The stockings should be washed by hand or on a delicate wash cycle (40 o C) in a washing machine. Hang them up to dry. Do not tumble dry as the heat will damage the stockings. Do not dry them directly on a radiator as this will damage the fabric and reduce its useful wear time. What are the risks of wearing anti-embolic stockings? If the stockings are too tight they may limit the blood flow within your legs. If they are too tight you may experience one or more of the following symptoms: 10
15 blistering skin discolouration skin markings numbness pins and needles soreness If you have any of these symptoms you must report them immediately to your nurse. Looseness, if the stockings are too loose they will not provide enough pressure to reduce the risk of DVT. Rash, if you develop a rash you may be allergic to the materials in the stockings What should I do if I think I have a VTE? VTE needs immediate treatment. If you develop any symptoms while you are in hospital please inform the nursing staff or doctors promptly. If you develop these symptoms once you have left hospital, please seek medical advice immediately from your local A&E department. If you have symptoms of a DVT you will need an ultrasound scan (ideally within 4 hours of reporting the symptoms). If a PE is suspected, you will need an urgent CT scan. A treatment dose of anticoagulant may be given if there is a delay. Both tests will usually identify the VTE if there is one. If a VTE is diagnosed If you are diagnosed with a VTE you will start anticoagulation injections immediately, you may have to have these for 3-6 months or even longer. The hospital doctors will inform your GP of the diagnosis and the GP will manage your anticoagulation care perhaps referring you to a local anti-coagulation clinic. 11
16 Who do I contact if I have any problems with the antiembolic stockings or anticoagulant? If you have any concerns you should speak to a member of your medical or surgical team, or your Clinical Nurse Specialist (Keyworker). Out of normal office hours you can contact the Site Nurse Practitioner at The Royal Marsden on: bleep 017 (Sutton) bleep 022 (Chelsea) However if you experience severe symptoms you should visit your local accident and emergency department. Resources To watch a film addressing safety concerns you may have about your hospital stay, go to or ask a member of staff Useful websites: References This booklet is evidence based wherever the appropriate evidence is available and represents an accumulation of expert opinion and professional interpretation. Details of the references used in writing this booklet are available on request from: The Royal Marsden Help Centre Freephone: patientcentre@rmh.nhs.uk. 12
17 The Royal Marsden Macmillan Hotline: You can ring the hotline 24 hours a day, 7 days a week. Call us straight away if you are feeling unwell or are worried about the side effects of cancer treatments. This service provides specialist advice and support to all Royal Marsden patients, as well as to their carers, and both hospital and community-based doctors and nurses caring for Royal Marsden patients. 13
18 Notes and questions
19 Copyright 2015 The Royal Marsden NHS Foundation Trust All rights reserved Printed August 2015 Planned review date August 2018 No conflicts of interest were declared in the production of this booklet PI
20
Are you at risk of blood clots?
 Are you at risk of blood clots? DVT (deep vein thrombosis) & PE (pulmonary embolism) Information for patients in hospital or going home from hospital Are you at risk of blood clots? (DVT & PE) This leaflet
Are you at risk of blood clots? DVT (deep vein thrombosis) & PE (pulmonary embolism) Information for patients in hospital or going home from hospital Are you at risk of blood clots? (DVT & PE) This leaflet
Preventing hospital-acquired blood clots
 Preventing hospital-acquired blood clots Haematology Department Patient information leaflet This leaflet explains more about blood clots, which can form after illness and surgery. What are hospital-acquired
Preventing hospital-acquired blood clots Haematology Department Patient information leaflet This leaflet explains more about blood clots, which can form after illness and surgery. What are hospital-acquired
University College London Hospitals (UCLH) Preventing venous thromboembolism (VTE)
 University College London Hospitals (UCLH) Preventing venous thromboembolism (VTE) Information for adult inpatients and for patients due to be admitted If you need a large print, audio, braille, easy read
University College London Hospitals (UCLH) Preventing venous thromboembolism (VTE) Information for adult inpatients and for patients due to be admitted If you need a large print, audio, braille, easy read
Deep Vein Thrombosis (DVT) - Blood Clots
 Patient information Deep Vein Thrombosis (DVT) - Blood Clots i Important information for all patients. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Patient information Deep Vein Thrombosis (DVT) - Blood Clots i Important information for all patients. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Also available from Huntleigh Healthcare. Patient Information: Pressure ulcers. Venous leg ulcer: A patient carer guide
 Also available from Huntleigh Healthcare Patient Information: Pressure ulcers WoundASSIST TNP therapy: A patient information leaflet Venous leg ulcer: A patient carer guide Lympoedema: A patient carer
Also available from Huntleigh Healthcare Patient Information: Pressure ulcers WoundASSIST TNP therapy: A patient information leaflet Venous leg ulcer: A patient carer guide Lympoedema: A patient carer
Care of Your Peripherally Inserted Central Catheter
 Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Care of Your Peripherally Inserted Central Catheter A guide for patients and their carers Acute Oncology Patient Information Leaflet Contents Information for patients: What is a PICC? How is it put in?
Best Practice Guidelines - BPG 7 VTE (Venous Thrombo Embolism)
 Best Practice Guidelines - BPG 7 VTE (Venous Thrombo Embolism) (Venous Thrombo Embolism) 1 DOCUMENT STATUS: Approved DATE ISSUED: 10 th November 2015 DATE TO BE REVIEWED: 10 th November 2017 AMENDMENT
Best Practice Guidelines - BPG 7 VTE (Venous Thrombo Embolism) (Venous Thrombo Embolism) 1 DOCUMENT STATUS: Approved DATE ISSUED: 10 th November 2015 DATE TO BE REVIEWED: 10 th November 2017 AMENDMENT
Prevention and Treatment of Venous Thromboembolism (VTE) Policy
 CONTROLLED DOCUMENT Prevention and Treatment of Venous Thromboembolism (VTE) Policy CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled
CONTROLLED DOCUMENT Prevention and Treatment of Venous Thromboembolism (VTE) Policy CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 3 Controlled Document Sponsor: Controlled
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet
 Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Enhanced Recovery Programme for total hip and knee replacement Orthopaedic Department Patient Information Leaflet What is the Enhanced Recovery Programme? This leaflet aims to give you information on what
Having a Vena Cava Filter
 Having a Vena Cava Filter Department of Radiology Information for Patients i Radiology Leaflet No. 30 Contents Page number Introduction 3 Referral and consent 3 Why do I need a vena cava filter inserted?
Having a Vena Cava Filter Department of Radiology Information for Patients i Radiology Leaflet No. 30 Contents Page number Introduction 3 Referral and consent 3 Why do I need a vena cava filter inserted?
About your PICC line. Information for patients Weston Park Hospital
 About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
About your PICC line Information for patients Weston Park Hospital This booklet explains what a PICC line is, how it is inserted and some general advice on its use and care. What is a PICC line? A Peripherally
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath
 You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
You and your Totally Implanted Vascular Access Device (TIVAD) - Portacath Nursing A guide for patients and carers Contents What is a TIVAD?... 1 Why is a TIVAD necessary?... 2 How a TIVAD is inserted...
Inferior Vena Cava (IVC) Filter Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Inferior Vena Cava (IVC) Filter Insertion Radiology This leaflet informs you about the procedure known as an Inferior Vena
Having a blue light cystoscopy
 Having a blue light cystoscopy The aim of this information sheet is to help answer some of the questions you may have about having a blue light cystoscopy. It explains the benefits, risks and alternatives
Having a blue light cystoscopy The aim of this information sheet is to help answer some of the questions you may have about having a blue light cystoscopy. It explains the benefits, risks and alternatives
Pancreaticoduodenectomy enhanced recovery programme (PD ERP) Information for patients
 Pancreaticoduodenectomy enhanced recovery programme (PD ERP) Information for patients Welcome to the pancreaticoduodenectomy enhanced recovery programme (PD ERP). The aim of the programme is for you to
Pancreaticoduodenectomy enhanced recovery programme (PD ERP) Information for patients Welcome to the pancreaticoduodenectomy enhanced recovery programme (PD ERP). The aim of the programme is for you to
Hickman line insertion and caring for your line
 Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your
Hickman line insertion and caring for your line Information for patients This booklet explains how a Hickman line is put in, the benefits, the risks and the alternatives, as well as how to care for your
Clinical Policies Group notified to Quality and Safety Operational Group Approval Date 31/05/2017 Initial Equality Impact Screening
 Document Details Title Reducing the Risk of Venous Thromboembolism Policy Trust Ref No 1544-36862 Local Ref (optional) NA This policy is intended to support clinical staff at Shropshire Main points the
Document Details Title Reducing the Risk of Venous Thromboembolism Policy Trust Ref No 1544-36862 Local Ref (optional) NA This policy is intended to support clinical staff at Shropshire Main points the
Patient information. Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5
 Patient information Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5 Your consultant has recommended that you have a TRAM flap to reconstruct your breast. TRAM stands for Transverse Rectus
Patient information Breast Reconstruction TRAM Breast Services Directorate PIF 102 V5 Your consultant has recommended that you have a TRAM flap to reconstruct your breast. TRAM stands for Transverse Rectus
patientinformation Blood Clots Reducing your risk in hospital and at home Patient Safety The Rotherham NHS Foundation Trust
 The Rotherham NHS Foundation Trust Blood Clots Reducing your risk in hospital and at home atient Safety patientinformation Your health, your life, your choice, our passion Bring your medicines when you
The Rotherham NHS Foundation Trust Blood Clots Reducing your risk in hospital and at home atient Safety patientinformation Your health, your life, your choice, our passion Bring your medicines when you
ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION
 Apixaban ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION 1 WHAT DOES APIXABAN (ELIQUIS ) DO? blood thinner Prevents or treats blood clots This is how a blood clot might look inside a blood
Apixaban ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION 1 WHAT DOES APIXABAN (ELIQUIS ) DO? blood thinner Prevents or treats blood clots This is how a blood clot might look inside a blood
Skin Tunnelled Catheter (STC), also known as Central line
 Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
Skin Tunnelled Catheter (STC), also known as Central line Intravenous Therapy Department Patient information leaflet What is a skin tunnelled catheter? A skin tunnelled catheter (STC) is a long flexible
ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION
 Rivaroxaban ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION 1 WHAT DOES RIVAROXABAN (XARELTO ) DO? blood thinner Prevents or treats blood clots This is how a blood clot might look inside
Rivaroxaban ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION 1 WHAT DOES RIVAROXABAN (XARELTO ) DO? blood thinner Prevents or treats blood clots This is how a blood clot might look inside
Venous Thromboprophylaxis (VTE) Policy
 Venous Thromboprophylaxis (VTE) Policy Document Summary The intention of this policy is to ensure that all adult patients and service users of Cumbria Partnership Foundation NHS Trust are assessed for
Venous Thromboprophylaxis (VTE) Policy Document Summary The intention of this policy is to ensure that all adult patients and service users of Cumbria Partnership Foundation NHS Trust are assessed for
Inferior Vena Cava (IVC) Filter Placement
 If you have any questions, ask your doctor or nurse. Filters may also be used. Inferior Vena Cava (IVC) Filter Placement An IVC filter is used to prevent blood clots from moving from the lower part of
If you have any questions, ask your doctor or nurse. Filters may also be used. Inferior Vena Cava (IVC) Filter Placement An IVC filter is used to prevent blood clots from moving from the lower part of
Cardiac catheterisation. Cardiology Department Patient Information Leaflet
 Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Cardiac catheterisation Cardiology Department Patient Information Leaflet Introduction The purpose of this leaflet is to address some of the questions you might have including: What is cardiac catheterisation?
Ambulatory Emergency Care Pathways. Pulmonary Embolism
 Ambulatory Emergency Care Pathways Pulmonary Embolism Effective Date: September 2011 Content Summary Ref Title Description 1 Condition Details Identifies pathway details and clinical sign-off 2 Pathway
Ambulatory Emergency Care Pathways Pulmonary Embolism Effective Date: September 2011 Content Summary Ref Title Description 1 Condition Details Identifies pathway details and clinical sign-off 2 Pathway
Oxfordshire Anticoagulation Service. Important information about anticoagulation with vitamin K antagonists Information for patients
 Oxfordshire Anticoagulation Service Important information about anticoagulation with vitamin K antagonists Information for patients Page 2 Your information Name:... Address:......... or patient stickie
Oxfordshire Anticoagulation Service Important information about anticoagulation with vitamin K antagonists Information for patients Page 2 Your information Name:... Address:......... or patient stickie
ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION
 Dabigatran ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION 1 WHAT DOES DABIGATRAN (PRADAXA ) DO? blood thinner Prevents or treats blood clots This is how a blood clot might look inside
Dabigatran ANTICOAGULATION MANAGEMENT SERVICE PATIENT AND FAMILY EDUCATION 1 WHAT DOES DABIGATRAN (PRADAXA ) DO? blood thinner Prevents or treats blood clots This is how a blood clot might look inside
Sentinel Node Biopsy for Breast Cancer
 Sentinel Node Biopsy for Breast Cancer Breast Care Centre Information for Patients Name of Consultant: i... Date of surgery:... Key worker:... Direct line: 0116 250 2513 Monday - Friday 9 am - 4 pm (except
Sentinel Node Biopsy for Breast Cancer Breast Care Centre Information for Patients Name of Consultant: i... Date of surgery:... Key worker:... Direct line: 0116 250 2513 Monday - Friday 9 am - 4 pm (except
Recovering from a hip fracture following an accident
 South Tyneside NHS Foundation Trust Recovering from a hip fracture following an accident Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. What is a hip fracture? The hip joint
South Tyneside NHS Foundation Trust Recovering from a hip fracture following an accident Providing a range of NHS services in Gateshead, South Tyneside and Sunderland. What is a hip fracture? The hip joint
Day Case Unit/ Treatment Centre. Varicose Veins
 Day Case Unit/ Treatment Centre Varicose Veins What are varicose veins? When the superficial veins in the leg become enlarged and distorted they are said to be varicosed. They are often found in people
Day Case Unit/ Treatment Centre Varicose Veins What are varicose veins? When the superficial veins in the leg become enlarged and distorted they are said to be varicosed. They are often found in people
Patient Diary. Enhanced Recovery After Surgery (ERAS) Total Knee Replacement. Helping patients get better sooner after surgery.
 Contact numbers If you need any support or advice before or after surgery please do not hesitate to call us. Claire Ward enhanced recovery nurse (Monday Friday 8-4) 07816448518 Ward 12B 01494426398 How
Contact numbers If you need any support or advice before or after surgery please do not hesitate to call us. Claire Ward enhanced recovery nurse (Monday Friday 8-4) 07816448518 Ward 12B 01494426398 How
Your varicose vein operation
 Day Surgery Centre Your varicose vein operation patientinformation Rotherham Hospital Your health, your choice, our passion Your varicose vein operation This booklet gives a guide to your day case varicose
Day Surgery Centre Your varicose vein operation patientinformation Rotherham Hospital Your health, your choice, our passion Your varicose vein operation This booklet gives a guide to your day case varicose
Patient information. Axillary Node Surgery (Operations on the Armpit) Breast Directorate PIF 1370 V3
 Patient information Axillary Node Surgery (Operations on the Armpit) Breast Directorate PIF 1370 V3 What is Axillary Node Surgery? As part of any breast cancer operation the surgeon will usually remove
Patient information Axillary Node Surgery (Operations on the Armpit) Breast Directorate PIF 1370 V3 What is Axillary Node Surgery? As part of any breast cancer operation the surgeon will usually remove
Patients First. Inferior Vena Cava (IVC) Filter Placement. If you have any questions, ask your doctor or nurse. Patient Education TESTS AND PROCEDURES
 Patient Education TESTS AND PROCEDURES If you have any questions, ask your doctor or nurse. Inferior Vena Cava (IVC) Filter Placement An IVC filter is used to prevent blood clots from moving from the lower
Patient Education TESTS AND PROCEDURES If you have any questions, ask your doctor or nurse. Inferior Vena Cava (IVC) Filter Placement An IVC filter is used to prevent blood clots from moving from the lower
Non-cancer related bilateral mastectomy pre-operative information sheet
 Non-cancer related bilateral mastectomy pre-operative information sheet This leaflet explains more about non-cancer related bilateral mastectomy surgery, including the benefits, risks and any alternatives
Non-cancer related bilateral mastectomy pre-operative information sheet This leaflet explains more about non-cancer related bilateral mastectomy surgery, including the benefits, risks and any alternatives
Laparoscopic Radical Nephrectomy
 Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Urology Department Laparoscopic Radical Nephrectomy Information Aims of this leaflet To give information on the intended benefits and potential risks of kidney surgery To guide you in the decisions you
Enhanced recovery after laparoscopic surgery (ERALS) programme. Patient information and advice
 Enhanced recovery after laparoscopic surgery (ERALS) programme Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to
Enhanced recovery after laparoscopic surgery (ERALS) programme Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to
Policy for Venous Thromboembolism Prevention and Treatment
 Policy for Venous Thromboembolism Prevention and Treatment Start date: May 2013 Next Review: May 2015 Committee approval: Endorsed by: Distribution: Location Thrombosis and Thromboprophylaxis Steering
Policy for Venous Thromboembolism Prevention and Treatment Start date: May 2013 Next Review: May 2015 Committee approval: Endorsed by: Distribution: Location Thrombosis and Thromboprophylaxis Steering
CarePartners Nursing Care Plan Anticoagulant Therapy
 CarePartners Nursing Care Plan Anticoagulant Therapy ** If a CarePartners wound pathway, palliative care plan or oncology care plan is being used to guide the patient s care, this Nursing Care Plan may
CarePartners Nursing Care Plan Anticoagulant Therapy ** If a CarePartners wound pathway, palliative care plan or oncology care plan is being used to guide the patient s care, this Nursing Care Plan may
UW MEDICINE PATIENT EDUCATION. How to prepare and what to expect DRAFT. What is an IVC filter?
 UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
UW MEDICINE PATIENT EDUCATION Angiography: Inferior Vena Cava (IVC) Filter How to prepare and what to expect This handout explains what an inferior vena cava filter is and what to expect when you have
Laparoscopic partial nephrectomy
 Laparoscopic partial nephrectomy This leaflet is written to give you information and answer questions you may have about your surgery. If you have any further questions, please speak to your doctor or
Laparoscopic partial nephrectomy This leaflet is written to give you information and answer questions you may have about your surgery. If you have any further questions, please speak to your doctor or
Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients
 Oxford University Hospitals NHS Trust Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
Oxford University Hospitals NHS Trust Enhanced Recovery After Surgery (ERAS) Liver Resection Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest
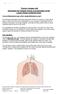 Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
Thoracic Surgery Unit Information for Patients Having an Examination of the Lymph Glands Inside the Chest Cervical Mediastinoscopy (often simply Mediastinoscopy ) The following information has been prepared
The Newcastle upon Tyne Hospitals NHS Foundation Trust Venous. Thromboembolism (VTE) Assessment and Management
 The Newcastle upon Tyne Hospitals NHS Foundation Trust Venous Thromboembolism (VTE) Assessment and Management Version No: 2.0 Effective From: 16 April 2018 Expiry Date: 16 April 2021 Date Ratified: 23
The Newcastle upon Tyne Hospitals NHS Foundation Trust Venous Thromboembolism (VTE) Assessment and Management Version No: 2.0 Effective From: 16 April 2018 Expiry Date: 16 April 2021 Date Ratified: 23
Mediastinal Venogram and Stent Insertion
 Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Mediastinal Venogram and Stent Insertion Radiology Department Patient information leaflet This leaflet tells you about the procedure known as a mediastinal venogram. It explains what is involved and the
Your anaesthetic for a broken hip
 Your anaesthetic for a broken hip Information to help patients, relatives and carers prepare for an anaesthetic for a broken hip First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what
Your anaesthetic for a broken hip Information to help patients, relatives and carers prepare for an anaesthetic for a broken hip First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what
Mediastinal Venogram and Stent Insertion
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Mediastinal Venogram and Stent Insertion Radiology This leaflet tells you about the procedure known as a mediastinal venogram.
Enhanced Recovery Programme for Nephrectomy (Kidney Removal)
 Enhanced Recovery Programme for Nephrectomy (Kidney Removal) This information leaflet will explain what will happen when you come to the hospital for your operation. The enhanced Recovery Programme is
Enhanced Recovery Programme for Nephrectomy (Kidney Removal) This information leaflet will explain what will happen when you come to the hospital for your operation. The enhanced Recovery Programme is
Getting ready for your operation at the Churchill Hospital Information for patients
 Getting ready for your operation at the Churchill Hospital Information for patients Welcome to the Day Surgery Unit You are being admitted for surgery on the same day as your operation. All urology patients
Getting ready for your operation at the Churchill Hospital Information for patients Welcome to the Day Surgery Unit You are being admitted for surgery on the same day as your operation. All urology patients
Discharge Advice Following Breast Reconstructive Surgery
 Oxford University Hospitals NHS Trust Discharge Advice Following Breast Reconstructive Surgery Information for patients This leaflet contains answers to some of the questions people most often ask when
Oxford University Hospitals NHS Trust Discharge Advice Following Breast Reconstructive Surgery Information for patients This leaflet contains answers to some of the questions people most often ask when
PATIENT AGREEMENT TO SYSTEMIC ANTI- CANCER THERAPY:
 PATIENT AGREEMENT TO SYSTEMIC ANTI- CANCER THERAPY: Gemcitabine-Doxorubicin PATIENT DETAILS PATIENT S SURNAME/FAMILY NAME: PATIENT S FIRST NAME(S): DATE OF BIRTH: NHS NUMBER: (or other identifier) HOSPITAL
PATIENT AGREEMENT TO SYSTEMIC ANTI- CANCER THERAPY: Gemcitabine-Doxorubicin PATIENT DETAILS PATIENT S SURNAME/FAMILY NAME: PATIENT S FIRST NAME(S): DATE OF BIRTH: NHS NUMBER: (or other identifier) HOSPITAL
PATIENT AGREEMENT TO SYSTEMIC ANTI- CANCER THERAPY:
 PATIENT AGREEMENT TO SYSTEMIC ANTI- CANCER THERAPY: Gemcitabine-Cisplatin PATIENT DETAILS PATIENT S SURNAME/FAMILY NAME: PATIENT S FIRST NAME(S): DATE OF BIRTH: NHS NUMBER: (or other identifier) HOSPITAL
PATIENT AGREEMENT TO SYSTEMIC ANTI- CANCER THERAPY: Gemcitabine-Cisplatin PATIENT DETAILS PATIENT S SURNAME/FAMILY NAME: PATIENT S FIRST NAME(S): DATE OF BIRTH: NHS NUMBER: (or other identifier) HOSPITAL
Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department.
 Total Knee Replacement Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. Introduction This booklet is designed to provide information about total knee replacement and inform you
Total Knee Replacement Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. Introduction This booklet is designed to provide information about total knee replacement and inform you
Peripherally Inserted Central Catheter (PICC Line)
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
A Guide to Your Hospital Stay When Having Gynecology Surgery
 Patient/Family Material A Guide to Your Hospital Stay When Having Gynecology Surgery For all your visits and on the day of your surgery, please bring with you: Manitoba Health Registration Card Any other
Patient/Family Material A Guide to Your Hospital Stay When Having Gynecology Surgery For all your visits and on the day of your surgery, please bring with you: Manitoba Health Registration Card Any other
Trans Urethral Resection of Bladder Tumour (TURBT) (Day Case)
 Trans Urethral Resection of Bladder Tumour (TURBT) (Day Case) Department of Urology Information for patients i What is a Trans Urethral Resection of Bladder Tumour (TURBT)? Your recent cystoscopy has shown
Trans Urethral Resection of Bladder Tumour (TURBT) (Day Case) Department of Urology Information for patients i What is a Trans Urethral Resection of Bladder Tumour (TURBT)? Your recent cystoscopy has shown
A Patient s guide to. Diagnostic Shoulder Arthroscopy
 A Patient s guide to Diagnostic Shoulder Arthroscopy This leaflet provides information regarding a diagnostic shoulder arthroscopy, which will help you prepare for your admission to hospital. The Shoulder
A Patient s guide to Diagnostic Shoulder Arthroscopy This leaflet provides information regarding a diagnostic shoulder arthroscopy, which will help you prepare for your admission to hospital. The Shoulder
Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt
 Department of Neurosurgery Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt Information for patients Shunt surgery This leaflet explains what to expect when you are in hospital and during
Department of Neurosurgery Insertion of a ventriculo-peritoneal or ventriculo-atrial shunt Information for patients Shunt surgery This leaflet explains what to expect when you are in hospital and during
Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet
 Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet Originator: Mr Raj Patel Date: May 2011 Version: 2 Date for Review: May 2014 DGOH Ref No: DGOH/PIL/00364
Guidance on the Enhanced Recovery Programme in Colorectal Surgery Surgery Patient Information Leaflet Originator: Mr Raj Patel Date: May 2011 Version: 2 Date for Review: May 2014 DGOH Ref No: DGOH/PIL/00364
Endoscopy Suite Patient Information
 Having a flexible sigmoidoscopy Endoscopy Suite Patient Information Contents Introduction 1 What is a flexible sigmoidoscopy? 1 What preparation will I need for my flexible sigmoidoscopy? 2 What should
Having a flexible sigmoidoscopy Endoscopy Suite Patient Information Contents Introduction 1 What is a flexible sigmoidoscopy? 1 What preparation will I need for my flexible sigmoidoscopy? 2 What should
All about Your Implanted Venous Access Device (IVAD, Port )
 All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
All about Your Implanted Venous Access Device (IVAD, Port ) Your doctor has chosen an Implanted Venous Access Device (IVAD) for you based on your treatment needs. Because the IVAD can remain in place for
Hickman line insertion in the interventional radiology department
 Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Hickman line insertion in the interventional radiology department This leaflet explains more about what a Hickman line is, how it is inserted into the body and why your doctor has recommended this for
Rectal prolapse. Information for patients General Surgery
 Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Rectal prolapse Information for patients General Surgery Introduction Our aim is for you and your family to understand as much as possible about your condition and your operation. This booklet will help
Enhanced recovery after oesophagogastric surgery (EROS) Patient information and advice
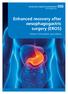 Enhanced recovery after oesophagogastric surgery (EROS) Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to go home
Enhanced recovery after oesophagogastric surgery (EROS) Patient information and advice Welcome to the enhanced recovery programme. The aim of the programme is to enable you to be well enough to go home
CARDIFF AND VALE NHS TRUST YMDDIRIEDOLAETH GIG CAERDYDD A R FRO CARDIAC SURGERY PATIENT INFORMATION BOOKLET
 CARDIFF AND VALE NHS TRUST YMDDIRIEDOLAETH GIG CAERDYDD A R FRO CARDIAC SURGERY PATIENT INFORMATION BOOKLET Welcome / Croeso Welcome to the Cardiothoracic Department unit at the University Hospital of
CARDIFF AND VALE NHS TRUST YMDDIRIEDOLAETH GIG CAERDYDD A R FRO CARDIAC SURGERY PATIENT INFORMATION BOOKLET Welcome / Croeso Welcome to the Cardiothoracic Department unit at the University Hospital of
Peripherally Inserted Central Catheter (PICC)
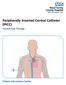 Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
Peripherally Inserted Central Catheter (PICC) Intravenous Therapy Patient information leaflet What is a PICC? A PICC is a very fine flexible tube measuring 50 60 cm in length. It is placed in a vein in
RIGHT HEMICOLECTOMY. Patient information Leaflet
 RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
RIGHT HEMICOLECTOMY Patient information Leaflet April 2017 WHAT IS A RIGHT HEMICOLECTOMY? This is an operation that is designed to remove the right side of your large bowel. Part of the large bowel is
Excision of Submandibular Gland
 Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Patient information Excision of Submandibular Gland Ear, Nose and Throat Directorate PIF 863 V5 Your consultant has advised that you have excision of submandibular gland. What is excision of submandibular
Patient Information Varicose Vein Surgery Dr Marek Garbowski. Varicose Veins
 Contents: Welcome Varicose veins Our expectations Preadmission clinic The day of your operation In preparation of going home Discharge advice following varicose veins surgery Contacts Varicose Veins Welcome
Contents: Welcome Varicose veins Our expectations Preadmission clinic The day of your operation In preparation of going home Discharge advice following varicose veins surgery Contacts Varicose Veins Welcome
Contents. Welcome to the Cath Lab P4/5
 Contents Welcome to the Cath Lab Preparation Instructions : information to ensure you are ready for your procedure in the Cath Lab, set out for you as questions (Q) and answers (A) How the day will go
Contents Welcome to the Cath Lab Preparation Instructions : information to ensure you are ready for your procedure in the Cath Lab, set out for you as questions (Q) and answers (A) How the day will go
Having an operation. Patient information factsheet
 Having an operation Patient information factsheet The purpose of this factsheet This factsheet contains important information to prepare you for your operation at the Whittington Hospital. All patients
Having an operation Patient information factsheet The purpose of this factsheet This factsheet contains important information to prepare you for your operation at the Whittington Hospital. All patients
A Patient s Guide to Surgery
 A Patient s Guide to Surgery Welcome Welcome to Carolinas Medical Center-NorthEast. Our staff of skilled professionals look forward to providing the care you need. We want your stay to be pleasant and
A Patient s Guide to Surgery Welcome Welcome to Carolinas Medical Center-NorthEast. Our staff of skilled professionals look forward to providing the care you need. We want your stay to be pleasant and
Split thickness skin grafts
 Split thickness skin grafts This leaflet explains more about returning to your everyday activities after your split thickness skin graft. If you have any further questions, please speak to a doctor or
Split thickness skin grafts This leaflet explains more about returning to your everyday activities after your split thickness skin graft. If you have any further questions, please speak to a doctor or
What is Latissimus Dorsi Flap Breast Reconstruction?
 What is Latissimus Dorsi Flap Breast Reconstruction? Information for patients from General Surgery and Cancer Services This leaflet is for women having breast reconstruction at the same time as, or following,
What is Latissimus Dorsi Flap Breast Reconstruction? Information for patients from General Surgery and Cancer Services This leaflet is for women having breast reconstruction at the same time as, or following,
Partial glossectomy. Your operation explained. Information for patients Head and Neck Centre
 Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Partial glossectomy Your operation explained Information for patients Head and Neck Centre page 2 of 12 This leaflet provides information about the procedure known as partial glossectomy. It explains what
Intranet version. Bradford Teaching Hospitals. NHS Foundation Trust. Colonoscopy. Gastroenterology Unit patient information booklet
 Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
Intranet version Bradford Teaching Hospitals NHS Foundation Trust Colonoscopy Gastroenterology Unit patient information booklet What is a colonoscopy? A colonoscopy is a procedure generally performed under
THE ROY CASTLE LUNG CANCER FOUNDATION
 Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Surgery for lung cancer How will it be decided if I am suitable for surgery? Successful surgery for lung cancer, with the chance of cure, may only be possible after the surgeon has considered the following
Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients
 Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience and well-being of people who need major
Enhanced Recovery After Surgery (ERAS) Cystectomy Information for patients What is Enhanced Recovery? Enhanced Recovery is a new way of improving the experience and well-being of people who need major
Having an open partial nephrectomy
 Having an open partial nephrectomy The aim of this information sheet is to help answer some of the questions you may have about having part of your kidney removed using conventional open surgery this is
Having an open partial nephrectomy The aim of this information sheet is to help answer some of the questions you may have about having part of your kidney removed using conventional open surgery this is
INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY
 St James s Hospital Department of Cardiothoracic Surgery INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY R 255 JULY 2014 CONTENTS Your lungs and how they work...1 Why do I need surgery?...1
St James s Hospital Department of Cardiothoracic Surgery INFORMATION FOR PATIENTS WHO ARE PREPARING FOR LUNG RESECTION SURGERY R 255 JULY 2014 CONTENTS Your lungs and how they work...1 Why do I need surgery?...1
Coordinating Access to Obtain ZOLINZA
 ACT Now: 1-866-363-6379 Coordinating Access to Obtain ZOLINZA Reimbursement Support Services Patient Assistance BEFORE YOU LEAVE, please have your physician s office fax your prescription for ZOLINZA and
ACT Now: 1-866-363-6379 Coordinating Access to Obtain ZOLINZA Reimbursement Support Services Patient Assistance BEFORE YOU LEAVE, please have your physician s office fax your prescription for ZOLINZA and
Peripherally Inserted Central Catheter (PICC)
 University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
University Teaching Trust Peripherally Inserted Central Catheter (PICC) IV Team 0161 206 0459 All Rights Reserved 2017. Document for issue as handout. Contents l What is a PICC? l Why do I need a PICC?
Peripherally Inserted Central Catheter
 UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
UW MEDICINE PATIENT EDUCATION Peripherally Inserted Central Catheter Understanding your PICC procedure and consent form Please read this handout before reading and signing the form Special Consent for
Bowel Surgery Hartmann s Procedure Your operation explained
 Bowel Surgery Hartmann s Procedure Your operation explained Introduction This information is for people considering having a Hartmann s Procedure operation. It explains what is involved and some possible
Bowel Surgery Hartmann s Procedure Your operation explained Introduction This information is for people considering having a Hartmann s Procedure operation. It explains what is involved and some possible
Etoposide (VePesid ) ( e-toe-poe-side )
 Etoposide (VePesid ) ( e-toe-poe-side ) How drug is given: by mouth Purpose: to stop the growth of cancer cells in ovarian cancer, small cell lung cancer, Hodgkin disease, and other cancers How to take
Etoposide (VePesid ) ( e-toe-poe-side ) How drug is given: by mouth Purpose: to stop the growth of cancer cells in ovarian cancer, small cell lung cancer, Hodgkin disease, and other cancers How to take
POLICY FOR the Assessment, Prevention and Treatment of Venous Thrombo-Embolism. Policy Reference: Version: 1 Status: Approved
 POLICY FOR the Assessment, Prevention and Treatment of Venous Thrombo-Embolism Policy Reference: Version: 1 Status: Approved Type: Clinical Policy applies to : All SCH staff within relevant groups; community
POLICY FOR the Assessment, Prevention and Treatment of Venous Thrombo-Embolism Policy Reference: Version: 1 Status: Approved Type: Clinical Policy applies to : All SCH staff within relevant groups; community
Your Anesthesiologist, Anesthesia and Pain Control
 You should avoid having pain after surgery by planning ahead. For example, if you know that you are going to be getting up to do your exercises with the therapist, ask for pain control medication in advance.
You should avoid having pain after surgery by planning ahead. For example, if you know that you are going to be getting up to do your exercises with the therapist, ask for pain control medication in advance.
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients
 Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Specialist Surgery Inpatients Breast Reconstruction Surgery Information for patients Your hospital stay This leaflet has been written to give you information about your surgery and what will happen during
Having an Oesophageal Dilatation
 Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Having an Oesophageal Dilatation Information for Patients In this leaflet: Introduction 2 What is an Oesophageal Dilatation?...2 What are the benefits of an Oeosphageal Dilatation? 2 Are there any risks?.2
Patient information. Ankle Arthroscopy. Trauma and Orthopaedic Directorate PIF 713 / V4
 Patient information Ankle Arthroscopy Trauma and Orthopaedic Directorate PIF 713 / V4 Your Consultant / Doctor has advised you to have an ankle arthroscopy. The aim of surgery is to help to confirm a diagnosis
Patient information Ankle Arthroscopy Trauma and Orthopaedic Directorate PIF 713 / V4 Your Consultant / Doctor has advised you to have an ankle arthroscopy. The aim of surgery is to help to confirm a diagnosis
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DOCETAXEL + PREDNISOLONE. Patient s first names
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DOCETAXEL + PREDNISOLONE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM DOCETAXEL + PREDNISOLONE Patient s surname/family name Patient s first names Date of birth Hospital Name: Guy s
Laparoscopy. Women's Health Unit. Patient Information Leaflet
 Laparoscopy Women's Health Unit Patient Information Leaflet February 2017 WHAT IS A LAPAROSCOPY? Laparoscopy is direct visual examination of the inside of the abdomen, using a viewing device called a laparoscope.
Laparoscopy Women's Health Unit Patient Information Leaflet February 2017 WHAT IS A LAPAROSCOPY? Laparoscopy is direct visual examination of the inside of the abdomen, using a viewing device called a laparoscope.
Having a portacath insertion in the x-ray department
 Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Having a portacath insertion in the x-ray department This leaflet provides information about a portacath insertion, including the benefits, risks and any alternatives. It also explains what you can expect
Percutaneous nephrolithotomy (PCNL)
 Percutaneous nephrolithotomy (PCNL) This leaflet explains more about the PCNL procedure to clear kidney stones, including the benefits, risks and any alternatives and what you can expect when you come
Percutaneous nephrolithotomy (PCNL) This leaflet explains more about the PCNL procedure to clear kidney stones, including the benefits, risks and any alternatives and what you can expect when you come
Oral Ibrutinib (single agent)
 Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM IBRUTINIB Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other
Patient identifier/label: Page 1 of 6 PATIENT AGREEMENT TO SYSTEMIC THERAPY: CONSENT FORM IBRUTINIB Patient s surname/family name Patient s first names Date of birth Hospital Name: NHS number (or other
Venous Thromboembolism (VTE) Prevention and Management Policy and Procedures
 PLEASE NOTE: Whilst the review date for this policy has passed, it is still the current version that should be used by staff. Director of Nursing and Medical Director, April 2014 Venous Thromboembolism
PLEASE NOTE: Whilst the review date for this policy has passed, it is still the current version that should be used by staff. Director of Nursing and Medical Director, April 2014 Venous Thromboembolism
Local anaesthesia for your eye operation
 Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
Local anaesthesia for your eye operation Information for patients Fourth Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet explains what to expect when you have an eye operation with a local anaesthetic.
Department of Neurological Surgery John Radcliffe Hospital Thalamotomy and Pallidotomy Pre-operative information for people with tremor and/or
 Department of Neurological Surgery John Radcliffe Hospital Thalamotomy and Pallidotomy Pre-operative information for people with tremor and/or Parkinson s disease We have been able to help many people
Department of Neurological Surgery John Radcliffe Hospital Thalamotomy and Pallidotomy Pre-operative information for people with tremor and/or Parkinson s disease We have been able to help many people
Urology Enhanced Recovery Programme: Laparoscopic/open simple/radical/partial/donor nephrectomy. Information For Patients
 Urology Enhanced Recovery Programme: Laparoscopic/open simple/radical/partial/donor nephrectomy Information For Patients 2 This information leaflet aims to help you understand the Enhanced Recovery Programme
Urology Enhanced Recovery Programme: Laparoscopic/open simple/radical/partial/donor nephrectomy Information For Patients 2 This information leaflet aims to help you understand the Enhanced Recovery Programme
