EDUCATION ON PATIENT-
|
|
|
- Hillary James
- 6 years ago
- Views:
Transcription
1 Pulmonary Critical Care EDUCATION ON PATIENT- VENTILATOR SYNCHRONY, CLINICIANS KNOWLEDGE LEVEL, AND DURATION OF MECHANICAL VENTILATION By Donna Lynch-Smith, DNP, ACNP-BC, APN, NE-BC, CNL, Carol Lynn Thompson, PhD, DNP, ACNP, FNP, CCRN, Rexann G. Pickering, RN, PhD, CIP, and Jim Y. Wan, PhD 2016 American Association of Critical-Care Nurses doi: Background Improved recognition of patient-ventilator asynchrony may reduce duration of mechanical ventilation. Objective To evaluate the effects of education about patientventilator synchrony on clinicians level of knowledge and patients mean duration of mechanical ventilation. Methods A quasi-experimental 1-group pretest-posttest study was performed in a 16-bed intensive care unit. Analysis included 33 clinicians and 97 ventilator patients. The intervention consisted of PowerPoint lectures on patientventilator synchrony. Data included test scores before and after the education, scores on the Acute Physiology and Chronic Health Evaluation II, and mean duration of mechanical ventilation. Differences in scores before and after education, mean duration of mechanical ventilation, and mean health evaluation scores before and after education were determined by using t tests. Results Of the 33 clinicians, 17 were registered nurses and 16 were respiratory therapists. Posttest scores were 63% higher than pretest scores (P <.001). Before the lecture, 47 patients had a mean health evaluation score of 21 (SD, 7.8) and mean duration of mechanical ventilation of 5.4 (SD, 4.6) days. After the lecture, 50 patients had a mean health evaluation score of 24.6 (SD, 8.2) and mean duration of mechanical ventilation of 4.8 (SD, 4.3) days. Mean health evaluation score was marginally higher after the lecture (P =.054). Mean duration of mechanical ventilation did not differ (P =.54). Conclusions Clinicians test scores increased significantly after patient-ventilator synchrony lectures. Mean duration of mechanical ventilation decreased by 0.6 days and health evaluation scores were marginally higher after the lectures. (American Journal of Critical Care. 2016; 25: ) AJCC AMERICAN JOURNAL OF CRITICAL CARE, November 2016, Volume 25, No
2 The purpose of mechanical ventilation is to improve oxygenation and ventilation while reversing the underlying disease process that is causing respiratory failure. Optimal oxygenation and ventilation require synchronous interaction between the ventilator and the patient. Patient-ventilator synchrony (see Figure) is defined as harmonious interaction between 2 pumps: the patient s respiratory system and the ventilator. 1 The patient s respiratory system is affected by the neuromuscular system and the mechanical properties of the lungs and thorax, and the ventilator is controlled by the operator and the demand valve. 2 Patient-ventilator synchrony can be detected by clinical inspection of the patient and interpretation of breath-to-breath real-time ventilator waveforms. Patient-ventilator asynchrony is a mismatch of patient-initiated breaths and ventilator-assisted breaths. The opposite of patient-ventilator synchrony is patient-ventilator asynchrony. Patient-ventilator asynchrony was described as early as the 1970s as fighting the ventilator. 3 More recently, Sassoon and Foster 4 described patient-ventilator asynchrony as mismatching of patient-initiated breaths and ventilator-assisted breaths. Therefore, patient-ventilator synchrony consists of patient- related factors and ventilator-related factors. 1 Patient-related factors include respiratory neural inspiratory time and respiratory system mechanics. 1 Ventilator-related factors are triggering, flow delivery, breath termination, and intrinsic positive end-expiratory pressure (autopeep). 1 Triggering is responsible for initiation of the breath. Flow delivery is the rate at which the tidal volume of air is delivered. Breath termination is the end of the ventilatorassisted breath. Last, autopeep is gas trapped during dynamic hyperinflation states; that is, an increase in lung volume due to a decrease in expiratory time that is referred to as air stacking. 5 The main categories of asynchrony in ventilatorassisted breaths are triggering, flow, and rate. 6 The About the Authors Donna Lynch-Smith is an assistant professor and concentration coordinator of the AG-ACNP program, and Jim Y. Wan is a professor in the College of Biostatistics and Epidemiology, University of Tennessee Health Science Center, Memphis, Tennessee. Carol Lynn Thompson is a professor in the College of Nursing at the University of Kentucky, Lexington. Rexann G. Pickering is an administrator, Human Protection, Methodist Healthcare Memphis Hospitals and University of Tennessee Methodist Physicians, Memphis, Tennessee. Corresponding author: Donna Lynch-Smith, DNP, ACNP-BC, APN, NE-BC, CNL, Assistant Professor, College of Nursing, University of Tennessee Health Science Center, 920 Madison, Ste 948, Memphis, TN ( most common asynchrony is ineffective triggering. 6-9 This asynchrony occurs when a patient s inspiratory effort does not trigger a machine breath because of inappropriate triggering or flow sensitivity setting, decreased respiratory drive, muscle weakness, or dynamic hyperinflation. 1,10,11 Other triggering asynchronies include auto triggering and double triggering. Auto triggering occurs when a patient receives a mechanical breath in the absence of inspiratory effort. This event is due to artifacts in the ventilator, such as motion in the circuit, and cardiac oscillation in the patient. 2,11,12 Double triggering is the occurrence of two consecutive inspirations with an interval less than the mean inspiratory time 8 and occurs when the volume and flow settings do not meet the demands of the patient. 2,11,12 Rate asynchrony occurs when a patient s respiratory rate and the ventilator rate are not synchronized. 13 It takes place during the end of the patient s inspiratory phase and the beginning of the expiratory phase, thus causing asynchrony between the patient s rate and the ventilator s rate. Causes of rate asynchrony may be air hunger or neurological injury resulting in an increase in spontaneous rate. 13 Last, flow asynchrony occurs during inspiration when the ventilator does not meet the flow demands of the patient, thus causing air hunger, which usually occurs in patients with acute respiratory failure. 2,11 Several studies have been done on the prevalence of patient-ventilator asynchrony; however, only a few have been focused on standardization of clinical inspection, ventilator waveform analysis, and management of patient-ventilator asynchrony. Chao et al 7 found that greater than 10% of patients receiving mechanical ventilation had indications of triggering asynchrony, with a resultant duration of mechanical ventilation twice that of patients who did not have triggering asynchrony. Similarly, Thille et al 8 found that the presence of triggering asynchrony occurred in one-fourth of patients who were receiving 546 AJCC AMERICAN JOURNAL OF CRITICAL CARE, November 2016, Volume 25, No. 6
3 Patient Mechanical feedback (lung volume and velocity of contraction of respiratory muscles) Chemical feedback (PaO 2, PaCO 2, and ph) Reflex feedback (Hering-Breuer) Behavioral feedback Response of patient s effort to ventilator-delivered breaths Ventilator Patient-related factors Respiratory Neural Inspiratory time Respiratory system mechanics Synchrony Response ventilator to patient s efforts Trigger variable Pressure delivery Cycling-off variable Ventilator-related factors Triggering Flow delivery Breath termination AutoPEEP Assessment of patient-ventilator synchrony 1. Absence of (a) agitation and restlessness, (b) use of accessory muscle, and (c) paradoxical abdominal breathing 2. Peak inspiratory pressure < 35 cm H 2 O 3. Plateau pressure < 30 cm H 2 O 4. Absence of autopeep 5. Alveolar/arterial ratio > PaO 2 /FIO 2 ratio > Ventilator graphics absence of Trigger asynchrony Flow asynchrony Rate asynchrony Ventilator setting parameters Changes by physicians, respiratory therapists, and nurses Figure Patient-ventilator synchrony. Abbreviations: FIO 2, fraction of inspired oxygen; PEEP, positive end-expiratory pressure. mechanical ventilation. In addition, the duration of mechanical ventilation was more than 3 times longer than the duration in patients who did not experience asynchrony. In another study, Thille and Brochard 6 evaluated 3 strategies (reduction in pressure support, reduction in insufflation time, and application of PEEP) for their effects on patient-ventilator asynchrony. Use of these strategies significantly reduced patient-ventilator asynchrony and clinicians recognition of asynchrony and resulted in a significant decrease in duration of mechanical ventilation. In an observational study on the relationship of sedation to patient-ventilator asynchrony, de Wit et al 9 found that ineffective triggering was the most frequent asynchrony (88%). Short cycling and double triggering were the next most frequent asynchronies. Also of note, unlike in the aforementioned studies, 7,8 the mode of mechanical ventilation, including levels of pressure support, peak inspiratory pressure, plateau pressure, and level of PCO 2, and the presence of chronic obstructive pulmonary disease had no effect on the occurrence of ineffective triggering. In a prospective crossover randomized controlled trial of 14 intubated patients randomly given 25-minute trials of pressure support ventilation and neutrally adjusted ventilator assist who were lightly or deeply sedated, Vaschetto et al 14 found increased asynchronies in those patients who were receiving pressure support ventilation and were in deep sedation. Mellott et al 15 found that among 27 patients, 77% experienced several types of asynchronous events. Similar to the findings of other studies, the most common asynchronous event was ineffective triggering, occurring in 63% of asynchronous events. Mellott et al also identified new asynchronous events during the flow phase that have not been previously reported: variant inspiratory effort, unusual double trigger, combined phase premature termination flow, combined phase double trigger flow, double triggerpremature termination, combined phase active AJCC AMERICAN JOURNAL OF CRITICAL CARE, November 2016, Volume 25, No
4 The educational presentation for nurses consisted of a 54-slide PowerPoint presentation. multiple trigger premature termination, and combined phase patient gasp. With this new knowledge of more types of asynchronies, the need to educate bedside clinicians on identification and management of patient-ventilator asynchrony is obvious. Patient-ventilator asynchronies can be detected by clinical inspection, determination of esophageal pressure, measurement of diaphragm electrical activity, and use of the BetterCare system. 8,16-18 BetterCare is a software platform that processes data and airflow waveforms from ventilators. 18 Ventilator graphics depicting patient-ventilator synchrony are pressure-time waveforms, flow-time waveforms, and volume-time waveforms. With pressure plotted on the vertical axis and time plotted on the horizontal axis, an accelerated waveform that reaches a peak is inspiration, and the decelerated aspect of the wave represents expiration. In flow-time waveforms, flow is plotted on the vertical axis and time is plotted on the horizontal axis. In a volume breath, inspiration can be depicted as a square, decelerating, or sinusoidal waveform above the baseline. Expiration is reflected below baseline and terminates at baseline. In volume-time waveforms, inspiration starts at baseline and moves upward to a peak until it reaches the set tidal volume. Expiration begins from the peak and descends downward and back to baseline. In 2009, this pilot study was carried out to determine if educating critical care nurses and respiratory therapists on patient-ventilator synchrony and asynchrony would have an effect on the clinicians level of knowledge. The hypothesis was that education would increase the clinicians knowledge scores. A safety study was included to see if education would have any effect on patients mean duration of mechanical ventilation. Methods We conducted a prospective quasi-experimental study. The study was approved by the appropriate institutional review boards, and a waiver of consent and Health Insurance Portability and Accountability Act authorization for the patients in the study was granted by the boards. Because we were evaluating an educational program, both review boards allowed a cover statement to be used instead of a consent form for the staff members in the study. The research was carried out at Methodist University Hospital, an urban teaching medical center in Memphis, Tennessee. The information on patient-ventilator synchrony and asynchrony was presented in the critical care and respiratory care classrooms. Staff members were included if they were a registered nurse or a registered respiratory therapist not currently in a critical care orientation program. Definitions of asynchrony according to Thille et al, 8 Sassoon and Foster, 4 Nilsestuen and Hargett, 2 and Waugh et al 13 were used for the education. A 1-hour lecture on patient-ventilator synchrony and asynchrony was given by the investigator (D.L-S.) 7 different times in the critical care classroom, the respiratory care department classroom, and the critical care unit. The educational presentation consisted of a 54-slide PowerPoint presentation for nurses that included definitions of patient-ventilator synchrony and asynchrony; basic mechanical ventilation waveforms and interpretations; synchronous and asynchronous waveforms and interpretations; strategies to improve triggering, flow, and rate asynchronies; measures of oxygenation and ventilation; and ventilator setup and adjustments. The educational presentation for respiratory therapists consisted of the same 54 slides used for nurses plus an additional 23 PowerPoint slides on inspiratory rise time and pressure- and flow-volume loop interpretation. Handouts of the PowerPoint presentation were given to all participants at the beginning of the lecture. A closed-book pretest was administered before the 1-hour lecture on patient-ventilator synchrony and asynchrony. The pretests were collected immediately after their completion. After the lecture, a closed-book posttest was administered and was collected immediately after the posttests were completed. Answers to the test questions were made known to the staff after completion of the study. The pretest and the posttest were the same except for the ordering of questions. The content included questions on determinants of patientventilator synchrony, phases of patient-ventilator synchrony, causes of patient-ventilator asynchrony, management of patient-ventilator asynchrony, and basic waveform analysis. Each test consisted of 12 questions worth a total of 25 points. Among the questions, 3 were multiple choice (3 points), 1 was true-false (1 point), 1 was check all that apply (8 points), 1 was a matching question (3 points), 5 were waveform analyses (5 points), and 1 was a case study (5 points). Data on patients mean duration of mechanical ventilation were collected by personnel in the respiratory care department 1 month before and 1 month after the lecture on patient-ventilator synchrony and asynchrony. 548 AJCC AMERICAN JOURNAL OF CRITICAL CARE, November 2016, Volume 25, No. 6
5 Table 1 Staff demographics and changes in test scores from pretest to posttest Mean (SD) Group Years in critical care Pretest score Posttest score Increase in score, % P a All staff (N = 33) Registered nurses (n = 17) Respiratory therapists (n = 16) 9.4 (11.4) 5.8 (6.1) 13.2 (14.2) 12.4 (4.5) 10.3 (3.2) 14.6 (4.6) 18 (3.7) 15.9 (3.6) 20.3 (2.3) <.001 < a From t test or 2 test. A safety study was conducted in the medical intensive care unit 1 month before and 1 month after the lecture on patient-ventilator synchrony and asynchrony. The inclusion criterion for patients was treatment with mechanical ventilation for 24 hours or longer. Demographic data collected on patients included age, sex, scores on the Acute Physiology and Chronic Health Evaluation (APACHE) II, and the primary cause of respiratory failure. The effects of the educational lectures on the knowledge of nurses and respiratory therapists were assessed by using paired t tests to detect any difference between pretest and posttest scores. Improvement as a percent increase in the posttest score compared with the pretest score was assessed by using simple t tests and a null value of zero. A 2-sample t test was used to determine whether the duration of mechanical ventilation was the same before and after the educational intervention. The results are depicted as means and standard deviations. Findings were considered significant at P =.05, without adjustment for multiplicity. Results Education Intervention A total of 33 staff members volunteered to participate in the study: 17 of 30 nurses from the medical intensive care unit and 16 of 44 registered respiratory therapists from the respiratory care department. The mean number of years of critical care experience of the 2 groups was similar (P =.06). Mean number of years of critical care experience was 5.8 (SD, 6.1; range, 1-20) for nurses and 13.2 (SD, 14.2; range, 1-40) for respiratory therapists. For all participants, scores on the posttests were higher than the scores on the pretests (Table 1). For nurses, mean overall scores were 10.3 (SD, 3.2) before the lecture and 15.9 (SD, 3.6) after the lecture. The mean increase in posttest scores compared with pretest scores was 5.6 (SD, 2.9) points (P <.001), for a mean improvement of 71% (SD, 69%; P <.001). For respiratory therapists, the mean overall pretest score was 14.6 (SD, 4.6) points, and the mean overall posttest score was 20.3 (SD, 2.3) points. The mean increase in the posttest score compared with the pretest score was 5.6 (SD, 3.8) points (P <.001), for a mean improvement of 55% (SD, 60%; P =.002). Whether measured as points or as a percentage, improvement did not differ between the nurses and the respiratory therapists. For both groups of participants, years of critical care experience was independent of the increase in knowledge as measured by increase in posttest score over the pretest score. Posttest scores increased by 63% (P <.001). Safety Study A total of 97 patients were treated with mechanical ventilation during the safety study. Of the 97, a total of 47 were receiving mechanical ventilation the month before the patient-ventilator lectures. In this group of 47, the The educational intervention made a significant difference in the posttest scores of nurses and respiratory therapists. cumulative mean duration of mechanical ventilation for the month was 5.36 days (252 ventilator days). Fifty patients were treated with mechanical ventilation during the month after the patient-ventilator lectures. The cumulative mean duration of mechanical ventilation for the month after the lectures was 4.8 days (240 ventilator days) Demographic characteristics and main causes of respiratory failure in the 2 groups of patients are given in Table 2. The mean APACHE score in patients after the lectures was higher than the score in patients before the lectures, but the difference was not significant (P =.054). The postlecture group was slightly younger than the prelecture group. The main cause of respiratory failure in both groups of patients was pulmonary. The mean duration of mechanical ventilation represents aggregate data for the 2 groups of patients. Mean duration was 5.4 (SD, 4.6) days for the prelecture group and 4.8 (SD, 4.3) days for the postlecture group (P =.54). The postlecture group had a minimal nonsignificant decrease in mean duration of 0.6 days. AJCC AMERICAN JOURNAL OF CRITICAL CARE, November 2016, Volume 25, No
6 Table 2 Patient demographics and mean duration of mechanical ventilation (N = 97) Descriptor Age, mean (SD), y Male sex, % APACHE II score at admission, mean (SD) Main cause of respiratory failure, % Cardiac Neurological Pulmonary Gastrointestinal Renal Metabolic Hematologic Days of mechanical ventilation, mean (SD) Prelecture (n = 47) 62.7 (14.6) (7.8) (4.6) Postlecture (n = 50) 58.4 (16.7) (8.2) (4.3) Abbreviation: APACHE, Acute Physiology and Chronic Health Evaluation. P Discussion Patient-ventilator asynchronies occur frequently in patients treated with mechanical ventilation. The most common asynchrony is ineffective triggering, which is associated with increased morbidity and mortality. 9,10 An asynchronous index of 10% or greater is associated with an increase in duration of mechanical ventilation and an increase in the length of stay in the intensive care unit. 18 Clinical inspection and ventilator graphic waveform interpretation of patient-ventilator asynchrony may decrease mean duration of mechanical ventilation and morbidity due to mechanical ventilation. Studies 6-8 have indicated that increasing the knowledge of patientventilator synchrony and interpretation of real-time breath-to-breath waveforms among nurses and respiratory therapists significantly decreased the number of asynchronous events and the duration of mechanical ventilation. In a prospective observational study, Colombo et al 19 found that both physicians who were clinically experienced in waveform analysis and physicians who were not were only able to detect less than one-third of patient-ventilator asynchronies by using flow and airway pressure tracings. In addition, as the rate of asynchronies increased, the rate of detection decreased. Therefore, additional technologies such as esophageal pressure monitoring, diaphragm electrical activity, and BetterCare could aid in identifying more asynchronies that are difficult to detect. 8,16,19 We found that the patient-ventilator synchrony and asynchrony lectures made a significant difference in the posttest scores of nurses (71%) and respiratory therapists (55%). In the safety study, mean duration of mechanical ventilation was not affected; duration decreased only 0.6 days after the lecture. The APACHE scores were higher in the postlecture group than in the prelecture group, but the difference was not significant (P =.054). Limitations Our study had several limitations. First it was a pilot study with a limited power of 33 staff members (17 nurses, and 16 respiratory therapists). All patients treated with mechanical ventilation for more than 24 hours for the month before and the month after the presentation on patient-ventilator synchrony and asynchrony were included in the study. A power analysis will need to be done to estimate adequate sample sizes of staff members and patients receiving mechanical ventilation. Another limitation was that data on mode of mechanical ventilation and level of sedation were gathered for the sample but were not reported. Studies have indicated that certain modes of ventilation and increasing levels of sedation are associated with asynchronous events. 9,18 The fourth limitation was that the pretest and the posttest consisted of the same questions; only the ordering of the questions differed. The time in between the pretest and the posttest was 1.5 hours; therefore, the nurses and the respiratory therapists possibly could have memorized the questions. Future pretests and posttests will need to have different questions with equivalent constructs of patient-ventilator synchrony and asynchrony. Another limitation of the study was that the clinicians were not directly observed during their interpretations of air flow and airway pressure waveforms reflecting patient-ventilator synchrony and asynchrony. Further studies are needed to evaluate clinicians ability to identify patient-ventilator asynchronies according to ventilator waveforms. Collecting aggregate mean duration of mechanical ventilation was also a limitation to the study. Data on mean duration must be collected on all patients. Conclusion In this study, education on patient-ventilator synchrony and asynchrony had a significant effect on nurses and respiratory therapists posttest scores. These results support the hypothesis that education on patient-ventilator synchrony and asynchrony would increase knowledge scores of nurses and respiratory therapists. In order to ascertain if such education has an effect on nurses and respiratory therapists knowledge level at the bedside, direct observations of clinical inspection and waveform interpretation will be required. 550 AJCC AMERICAN JOURNAL OF CRITICAL CARE, November 2016, Volume 25, No. 6
7 ACKNOWLEDGMENTS This research was done at Methodist University Hospital; Memphis, Tennessee. We acknowledge Dr Mona Wicks and Elizabeth Tornquist for content revisions and Gail Spake for editorial revisions. We also acknowledge the outstanding editorial assistance and support provided by Mr Curtis Roby, MA, during preparation of the manuscript. FINANCIAL DISCLOSURES None reported. eletters Now that you ve read the article, create or contribute to an online discussion on this topic. Visit and click Submit a response in either the full-text or PDF view of the article. REFERENCES 1. Kondili E, Prinianakis G, Georgopoulos D. Patient-ventilator interaction. Br J Anaesth. 2003;91(1): Nilsestuen JO, Hargett KD. Using ventilator graphics to identify patient-ventilator asynchrony. Respir Care. 2005; 50(2): Kirby RR. Improving ventilator-patient interaction: reduction of flow dyssynchrony. Crit Care Med. 1997;25(10): Sassoon CS, Foster GT. Patient-ventilator asynchrony. Curr Opin Crit Care. 2001;7(1): Chatburn RL. Classification of ventilator modes: update and proposal for implementation. Respir Care. 2007;52(3): Thille AW, Brochard L. Promoting patient-ventilator synchrony. Clin Pulm Med. 2007;14(6): Chao DC, Scheinhorn DJ, Stearn-Hassenpflug M. Patientventilator trigger asynchrony in prolonged mechanical ventilation. Chest. 1997;112(6): Thille AW, Rodriguez P, Cabello B, Lellouche F, Brochard L. Patient-ventilator asynchrony during assisted mechanical ventilation. Intensive Care Med. 2006;32(10): de Wit M, Pedram S, Best AM, Epstein SK. Observational study of patient-ventilator asynchrony and relationship to sedation level. J Crit Care. 2009;24(1): Branson RD, Blakeman TC, Robinson BR. Asynchrony and dyspnea. Respir Care. 2013;58(6): Gilstrap D, MacIntyre N. Patient-ventilator interactions: implications for clinical management. Am J Respir Crit Care Med. 2013;188(9): Epstein SK. How often does patient-ventilator asynchrony occur and what are the consequences? Respir Care. 2011; 56(1): Waugh JB, Deshpande V, Harwood RJ. Rapid Interpretation of Ventilator Waveforms. Upper Saddle River, NJ: Prentice Hall; Vaschetto R, Cammarota G, Colombo D, et al. Effects of propofol on patient-ventilator synchrony and interaction during pressure support ventilation and neurally adjusted ventilatory assist. Crit Care Med. 2014;42(1): Mellott KG, Grap MJ, Munro CL, et al. Patient ventilator asynchrony in critically ill adults: frequency and types. Heart Lung. 2014;43(3): Georgopoulos D, Prinianakis G, Kondili E. Bedside waveforms interpretation as a tool to identify patient-ventilator asynchronies. Intensive Care Med. 2006;32(1): Chen CW, Lin WC, Hsu CH, Cheng KS, Lo CS. Detecting ineffective triggering in the expiratory phase in mechanically ventilated patients based on airway flow and pressure deflection: feasibility of using a computer algorithm. Crit Care Med. 2008;36(2): Blanch L, Sales B, Montanya J, et al. Validation of the Better Care system to detect ineffective efforts during expiration in mechanically ventilated patients: a pilot study [published correction appears in Intensive Care Med. 2013;39(2):341]. Intensive Care Med. 2012;38(5): Colombo D, Cammarota G, Alemani M, et al. Efficacy of ventilator waveforms observation in detecting patientventilator asynchrony. Crit Care Med. 2011;39(11): To purchase electronic or print reprints, contact American Association of Critical-Care Nurses, 101 Columbia, Aliso Viejo, CA Phone, (800) or (949) (ext 532); fax, (949) ; , reprints@aacn.org.
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland
 Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Admissions with neutropenic sepsis in adult, general critical care units in England, Wales and Northern Ireland Question What were the: age; gender; APACHE II score; ICNARC physiology score; critical care
Suctioning in Adult. Pulmonary Critical Care. 1.0 Hour
 Pulmonary Critical Care Clinical Indicators for Endotracheal Suctioning in Adult Patients Receiving Mechanical Ventilation By Mary Lou Sole, RN, PhD, CCNS, Melody Bennett, RN, MN, CCRN, and Suzanne Ashworth,
Pulmonary Critical Care Clinical Indicators for Endotracheal Suctioning in Adult Patients Receiving Mechanical Ventilation By Mary Lou Sole, RN, PhD, CCNS, Melody Bennett, RN, MN, CCRN, and Suzanne Ashworth,
Patients Being Weaned From the Ventilator: Positive Effects of Guided Imagery. Authors McVay, Frank; Spiva, Elizabeth; Hart, Patricia L.
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
CRITICAL CARE CLINICIANS KNOWLEDGE GUIDELINES FOR PREVENTING VENTILATOR-ASSOCIATED PNEUMONIA OF EVIDENCE-BASED. C E 1.0 Hour. Pulmonary Critical Care
 Pulmonary Critical Care CRITICAL CARE CLINICIANS KNOWLEDGE OF EVIDENCE-BASED GUIDELINES FOR PREVENTING VENTILATOR-ASSOCIATED PNEUMONIA By Mohamad F. El-Khatib, MB, PhD, Salah Zeineldine, MD, Chakib Ayoub,
Pulmonary Critical Care CRITICAL CARE CLINICIANS KNOWLEDGE OF EVIDENCE-BASED GUIDELINES FOR PREVENTING VENTILATOR-ASSOCIATED PNEUMONIA By Mohamad F. El-Khatib, MB, PhD, Salah Zeineldine, MD, Chakib Ayoub,
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Human and financial costs of noninvasive mechanical ventilation in patients affected by COPD and acute respiratory failure Nava S, Evangelisti I, Rampulla C, Compagnoni M L, Fracchia C, Rubini F Record
Human and financial costs of noninvasive mechanical ventilation in patients affected by COPD and acute respiratory failure Nava S, Evangelisti I, Rampulla C, Compagnoni M L, Fracchia C, Rubini F Record
VENTILATION SERVO-U THE NEW POWER OF YOU
 VENTILATION SERVO-U THE NEW POWER OF YOU Critical Care SERVO-U 3 SERVO-U THE NEW POWER OF YOU SERVO-U delivers many effective options for protective ventilation. All of them more accessible, under standable
VENTILATION SERVO-U THE NEW POWER OF YOU Critical Care SERVO-U 3 SERVO-U THE NEW POWER OF YOU SERVO-U delivers many effective options for protective ventilation. All of them more accessible, under standable
The impact of nighttime intensivists on medical intensive care unit infection-related indicators
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 The impact of nighttime intensivists on medical intensive care unit infection-related indicators Abhaya Trivedi
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 The impact of nighttime intensivists on medical intensive care unit infection-related indicators Abhaya Trivedi
Current practice of closed-loop mechanical ventilation modes on intensive care units a nationwide survey in the Netherlands
 ORIGINAL ARTICLE Current practice of closed-loop mechanical ventilation modes on intensive care units a nationwide survey in the Netherlands E.F.E. Wenstedt 1 *, A.J.R. De Bie Dekker 1, A.N. Roos 1, J.J.M.
ORIGINAL ARTICLE Current practice of closed-loop mechanical ventilation modes on intensive care units a nationwide survey in the Netherlands E.F.E. Wenstedt 1 *, A.J.R. De Bie Dekker 1, A.N. Roos 1, J.J.M.
1. Introduction. Volume 6 Issue 4, April Hussein Hadi Atiyah, PhD 1, Musaab Majid Abdul-Wahhab, MSc.N 2, Sadeq A.
 Nurses Knowledge toward Essential Care for Adult Patients Undergoing Mechanical Ventilation at Critical Care Unit in Baghdad City Hussein Hadi Atiyah, PhD 1, Musaab Majid Abdul-Wahhab, MSc.N 2, Sadeq A.Al-Fayyadh,
Nurses Knowledge toward Essential Care for Adult Patients Undergoing Mechanical Ventilation at Critical Care Unit in Baghdad City Hussein Hadi Atiyah, PhD 1, Musaab Majid Abdul-Wahhab, MSc.N 2, Sadeq A.Al-Fayyadh,
National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI)
 October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
October 27, 2016 To: Subject: National Institutes of Health, National Heart, Lung and Blood Institute (NHLBI) COPD National Action Plan As the national professional organization with a membership of over
Primus. Your personal anesthesia assistant. Because you care. Emergency Care Perioperative Care Critical Care Perinatal Care Home Care
 Primus Your personal anesthesia assistant Emergency Care Perioperative Care Critical Care Perinatal Care Home Care Because you care You re part of a complex healthcare environment... In an increasingly
Primus Your personal anesthesia assistant Emergency Care Perioperative Care Critical Care Perinatal Care Home Care Because you care You re part of a complex healthcare environment... In an increasingly
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Department of Veterans Affairs VHA HANDBOOK HOME RESPIRATORY CARE PROGRAM
 Department of Veterans Affairs VHA HANDBOOK 1173.13 Veterans Health Administration Transmittal Sheet Washington, DC 20420 November 1, 2000 HOME RESPIRATORY CARE PROGRAM 1. REASON FOR ISSUE: This VHA Handbook
Department of Veterans Affairs VHA HANDBOOK 1173.13 Veterans Health Administration Transmittal Sheet Washington, DC 20420 November 1, 2000 HOME RESPIRATORY CARE PROGRAM 1. REASON FOR ISSUE: This VHA Handbook
END-TIDAL CARBON DIOXIDE AS A MEASURE
 Critical Care Techniques END-TIDAL CARBON DIOXIDE AS A MEASURE OF STRESS RESPONSE TO CLUSTERED NURSING INTERVENTIONS IN NEUROLOGIC PATIENTS By Laura Genzler, RN, BSN, Pamela Jo Johnson, MPH, PhD, Neha
Critical Care Techniques END-TIDAL CARBON DIOXIDE AS A MEASURE OF STRESS RESPONSE TO CLUSTERED NURSING INTERVENTIONS IN NEUROLOGIC PATIENTS By Laura Genzler, RN, BSN, Pamela Jo Johnson, MPH, PhD, Neha
Prone Ventilation of the Critically Ill Patient
 Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Prone Ventilation of the Critically Ill Patient Statement of Best Practice Patients who require prone ventilation will be clinically assessed by the appropriate medical team, taking into account indications/contraindications,
Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Young D, Lamb SE, Shah S, et al. High-frequency oscillation for acute
Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Young D, Lamb SE, Shah S, et al. High-frequency oscillation for acute
Effectiveness of Planned Teaching Programme on Cardiopulmonary Resuscitation among Policemen in selected Police-Station at Mangalore, India
 IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 6, Issue 4 Ver. III (Jul. - Aug. 2017), PP 59-63 www.iosrjournals.org Effectiveness of Planned Teaching
IOSR Journal of Nursing and Health Science (IOSR-JNHS) e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 6, Issue 4 Ver. III (Jul. - Aug. 2017), PP 59-63 www.iosrjournals.org Effectiveness of Planned Teaching
Effectiveness of Structured Teaching Program on Knowledge and Practice of Adult Basic Life Support Among Staff Nurses
 American Journal of Nursing Science 2018; 7(3): 100-105 http://www.sciencepublishinggroup.com/j/ajns doi: 10.11648/j.ajns.20180703.13 ISSN: 2328-5745 (Print); ISSN: 2328-5753 (Online) Effectiveness of
American Journal of Nursing Science 2018; 7(3): 100-105 http://www.sciencepublishinggroup.com/j/ajns doi: 10.11648/j.ajns.20180703.13 ISSN: 2328-5745 (Print); ISSN: 2328-5753 (Online) Effectiveness of
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP
 Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Effect of DNP & MSN Evidence-Based Practice (EBP) Courses on Nursing Students Use of EBP Richard Watters, PhD, RN Elizabeth R Moore PhD, RN Kenneth A. Wallston PhD Page 1 Disclosures Conflict of interest
Title: Length of use guidelines for oxygen tubing and face mask equipment
 Title: Length of use guidelines for oxygen tubing and face mask equipment Date: September 12, 2007 Context and policy issues: There is concern that oxygen tubing and face mask equipment in the ventilator
Title: Length of use guidelines for oxygen tubing and face mask equipment Date: September 12, 2007 Context and policy issues: There is concern that oxygen tubing and face mask equipment in the ventilator
Coding Guidelines for Certain Respiratory Care Services January 2018 (updates in red)
 Coding Guidelines for Certain Respiratory Care Services (updates in red) Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line
Coding Guidelines for Certain Respiratory Care Services (updates in red) Overview From time to time the AARC receives inquiries about respiratory-related coding and coverage issues through its Help Line
CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU. Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia
 CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia OBJECTIVES To discuss some of the factors that may predict duration of invasive
CLINICAL PREDICTORS OF DURATION OF MECHANICAL VENTILATION IN THE ICU Jessica Spence, BMR(OT), BSc(Med), MD PGY2 Anesthesia OBJECTIVES To discuss some of the factors that may predict duration of invasive
Feedback from Anesthesia clinicians. 2.1 Intubate Patient Workflow
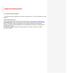 Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Feedback from Anesthesia clinicians 2.1 Intubate Patient Workflow The following section describes the workflow as derived from the Intubate Patient use case analysis. Intubate Patient (Process) This process
Standardizing ventilation technology up to the MRI suite, in an expanding hospital environment
 No. 16 Standardizing ventilation technology up to the MRI suite, in an expanding hospital environment Critical Care News is published by Maquet Critical Care. Maquet Critical Care AB 171 95 Solna, Sweden
No. 16 Standardizing ventilation technology up to the MRI suite, in an expanding hospital environment Critical Care News is published by Maquet Critical Care. Maquet Critical Care AB 171 95 Solna, Sweden
Analysis of Unplanned Extubation Risk Factors in Intensive Care Units
 10 Analysis of Unplanned Extubation Risk Factors in Intensive Care Units Yuan-Chia Cheng 1, Liang-Chi Kuo 1, Wei-Che Lee 1, Chao-Wen Chen 1, Jiun-Nong Lin 2, Yen-Ko Lin 1, Tsung-Ying Lin 1 Background:
10 Analysis of Unplanned Extubation Risk Factors in Intensive Care Units Yuan-Chia Cheng 1, Liang-Chi Kuo 1, Wei-Che Lee 1, Chao-Wen Chen 1, Jiun-Nong Lin 2, Yen-Ko Lin 1, Tsung-Ying Lin 1 Background:
HAWAII HEALTH SYSTEMS CORPORATION
 All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
Early Recognition of In-Hospital Patient Deterioration Outside of The Intensive Care Unit: The Case For Continuous Monitoring
 Early Recognition of In-Hospital Patient Deterioration Outside of The Intensive Care Unit: The Case For Continuous Monitoring Israeli Society of Internal Medicine Meeting July 5, 2013 Eyal Zimlichman MD,
Early Recognition of In-Hospital Patient Deterioration Outside of The Intensive Care Unit: The Case For Continuous Monitoring Israeli Society of Internal Medicine Meeting July 5, 2013 Eyal Zimlichman MD,
Intensive care unit mobility practices in Australia and New Zealand: a point prevalence study
 Intensive care unit mobility practices in Australia and New Zealand: a point prevalence study Susan C Berney, Megan Harrold, Steven A Webb, Ian Seppelt, Shane Patman, Peter J Thomas and Linda Denehy Immobility,
Intensive care unit mobility practices in Australia and New Zealand: a point prevalence study Susan C Berney, Megan Harrold, Steven A Webb, Ian Seppelt, Shane Patman, Peter J Thomas and Linda Denehy Immobility,
"Working Smartly: Better Communication and Reduced Error through Improved Clinical Informatics"
 "Working Smartly: Better Communication and Reduced Error through Improved Clinical Informatics" Healthcare Transformation Services Lisa Pahl, MSN, Principal, Practice Lead Alarm Management May, 2017 Data,
"Working Smartly: Better Communication and Reduced Error through Improved Clinical Informatics" Healthcare Transformation Services Lisa Pahl, MSN, Principal, Practice Lead Alarm Management May, 2017 Data,
NURSES PERCEPTIONS DURING RESUSCITATION OF FAMILY PRESENCE. Families in Critical Care
 Families in Critical Care NURSES PERCEPTIONS OF FAMILY PRESENCE DURING RESUSCITATION By Kelly Tudor, RN, BSN, CCRN, Jill Berger, RN, MSN, MBA, NE-BC, Barbara J. Polivka, RN, PhD, Rachael Chlebowy, RN,
Families in Critical Care NURSES PERCEPTIONS OF FAMILY PRESENCE DURING RESUSCITATION By Kelly Tudor, RN, BSN, CCRN, Jill Berger, RN, MSN, MBA, NE-BC, Barbara J. Polivka, RN, PhD, Rachael Chlebowy, RN,
The impact of an ICU liaison nurse service on patient outcomes
 The impact of an ICU liaison nurse service on patient outcomes Suzanne J Eliott, David Ernest, Andrea G Doric, Karen N Page, Linda J Worrall-Carter, Lukman Thalib and Wendy Chaboyer Increasing interest
The impact of an ICU liaison nurse service on patient outcomes Suzanne J Eliott, David Ernest, Andrea G Doric, Karen N Page, Linda J Worrall-Carter, Lukman Thalib and Wendy Chaboyer Increasing interest
Supplementary Online Content
 Supplementary Online Content Kaukonen KM, Bailey M, Suzuki S, Pilcher D, Bellomo R. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000-2012.
Supplementary Online Content Kaukonen KM, Bailey M, Suzuki S, Pilcher D, Bellomo R. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000-2012.
Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center
 Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of an Early
Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division of Cardiovascular Medicine The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of an Early
Ruchika D. Husa, MD, MS
 Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division i i of Cardiovascular Medicine i The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of
Early Response Teams Ruchika D. Husa, MD, MS Assistant Professor of Medicine Division i i of Cardiovascular Medicine i The Ohio State University Wexner Medical Center OBJECTIVES Provide an overview of
Unit length of stay and APACHE II scores for ventilated admissions to critical care in England, Wales and Northern Ireland
 Unit length of stay and APACHE II scores for ventilated admissions to critical care in England, Wales and Northern Ireland Questions What was the unit length of stay and APACHE II scores for ventilated
Unit length of stay and APACHE II scores for ventilated admissions to critical care in England, Wales and Northern Ireland Questions What was the unit length of stay and APACHE II scores for ventilated
Version 2 15/12/2013
 The METHOD study 1 15/12/2013 The Medical Emergency Team: Hospital Outcomes after a Day (METHOD) study Version 2 15/12/2013 The METHOD Study Investigators: Principal Investigator Christian P Subbe, Consultant
The METHOD study 1 15/12/2013 The Medical Emergency Team: Hospital Outcomes after a Day (METHOD) study Version 2 15/12/2013 The METHOD Study Investigators: Principal Investigator Christian P Subbe, Consultant
Case Managers and Their Role in Improving Patient Outcomes in Idiopathic Pulmonary Fibrosis
 Case Managers and Their Role in Improving Patient Outcomes in Idiopathic Pulmonary Fibrosis Final Outcomes Report May 2018 Genentech Grant ID: G-52505 Overview Activity Description: This text-based activity
Case Managers and Their Role in Improving Patient Outcomes in Idiopathic Pulmonary Fibrosis Final Outcomes Report May 2018 Genentech Grant ID: G-52505 Overview Activity Description: This text-based activity
Integrated care for asthma: matching care to the patient
 Eur Respir J, 1996, 9, 444 448 DOI: 10.1183/09031936.96.09030444 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Integrated care for asthma:
Eur Respir J, 1996, 9, 444 448 DOI: 10.1183/09031936.96.09030444 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Integrated care for asthma:
Seattle Nursing Research Consortium Abstract Style and Reference Guide
 Seattle Nursing Research Consortium Abstract Style and Reference Guide Page 1 SNRC Revised 7/2015 Table of Contents Content Page How to classify your Project. 3 Research Abstract Guidelines 4 Research
Seattle Nursing Research Consortium Abstract Style and Reference Guide Page 1 SNRC Revised 7/2015 Table of Contents Content Page How to classify your Project. 3 Research Abstract Guidelines 4 Research
Effect of information booklet about home care management of post operative cardiac patient in selected hospital, New Delhi
 Available Online at http://www.uphtr.com/ijnrp/home International Journal of Nursing Research and Practice EISSN 0-; Vol. No. (06) July December Original Article Effect of information booklet about home
Available Online at http://www.uphtr.com/ijnrp/home International Journal of Nursing Research and Practice EISSN 0-; Vol. No. (06) July December Original Article Effect of information booklet about home
Long Term Care Hospital Clinical Coverage Policy No: 2A-2 Services (LTCH) Amended Date: October 1, Table of Contents
 Long Term Care Hospital Clinical Coverage Policy No: 2A-2 Services (LTCH) Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements...
Long Term Care Hospital Clinical Coverage Policy No: 2A-2 Services (LTCH) Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligibility Requirements...
NCLEX PROGRAM REPORTS
 for the period of OCT 2014 - MAR 2015 NCLEX-RN REPORTS US48500300 000001 NRN001 04/30/15 TABLE OF CONTENTS Introduction Using and Interpreting the NCLEX Program Reports Glossary Summary Overview NCLEX-RN
for the period of OCT 2014 - MAR 2015 NCLEX-RN REPORTS US48500300 000001 NRN001 04/30/15 TABLE OF CONTENTS Introduction Using and Interpreting the NCLEX Program Reports Glossary Summary Overview NCLEX-RN
Know your tools: Improving the effectiveness of nurses using the confusion assessment method (CAM) to detect delirium
 Know your tools: Improving the effectiveness of nurses using the confusion assessment method (CAM) to detect delirium 1 Julie Plagenhoef, MPH, RN, CMSRN Preparing for Improvement: Why Delirium? Increases
Know your tools: Improving the effectiveness of nurses using the confusion assessment method (CAM) to detect delirium 1 Julie Plagenhoef, MPH, RN, CMSRN Preparing for Improvement: Why Delirium? Increases
Daily Interruptions of Sedation: A Clinical Approach to Improve Outcomes in Critically Ill Patients
 Feature Daily Interruptions of Sedation: A Clinical Approach to Improve Outcomes in Critically Ill Patients Elizabeth Berry, MSN, ACNP-BC Heather Zecca, MSN, ACNP-BC The continuous infusion of sedative
Feature Daily Interruptions of Sedation: A Clinical Approach to Improve Outcomes in Critically Ill Patients Elizabeth Berry, MSN, ACNP-BC Heather Zecca, MSN, ACNP-BC The continuous infusion of sedative
ROTOPRONE THERAPY SYSTEM. with people in mind.
 ROTOPRONE THERAPY SYSTEM with people in mind www.arjohuntleigh.com THE CLINICAL CHALLENGE: MINIMIZING MORTALITY AND POTENTIAL COMPLICATIONS IN ARDS PATIENTS WHILE MAKING IT EASIER TO DELIVER PRONE THERAPY
ROTOPRONE THERAPY SYSTEM with people in mind www.arjohuntleigh.com THE CLINICAL CHALLENGE: MINIMIZING MORTALITY AND POTENTIAL COMPLICATIONS IN ARDS PATIENTS WHILE MAKING IT EASIER TO DELIVER PRONE THERAPY
International Journal of Scientific and Research Publications, Volume 7, Issue 8, August ISSN
 International Journal of Scientific and Research Publications, Volume 7, Issue 8, August 2017 469 (Effectiveness of an Educational Program upon nurses knowledge toward The Continuous Positive Airway Pressure
International Journal of Scientific and Research Publications, Volume 7, Issue 8, August 2017 469 (Effectiveness of an Educational Program upon nurses knowledge toward The Continuous Positive Airway Pressure
Learning Objectives. Registration and Continental Breakfast 7:00 AM -7:30 AM
 Fundamental Critical Care Support Provided by USF Health Date: Program Number SF2014136B At CLS (Center for Advanced Medical Learning and Simulation) Tampa, Florida Day One Schedule Session Learning Format
Fundamental Critical Care Support Provided by USF Health Date: Program Number SF2014136B At CLS (Center for Advanced Medical Learning and Simulation) Tampa, Florida Day One Schedule Session Learning Format
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool
 Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Improving Patient Surveillance: Instituting a Respiratory Risk Screening Tool Sandra Maddux, RN, MSN, CNS-BC, Michelle Giffin, RN, BSN, & Patti Leglar, RN-C, BSN Purpose To share an evidence-based protocol
Measuring Harm. Objectives and Overview
 Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3. Measuring Harm
 Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Patient Safety Research Introductory Course Session 3 Measuring Harm Albert W Wu, MD, MPH Former Senior Adviser, WHO Professor of Health Policy & Management, Johns Hopkins Bloomberg School of Public Health
Study Title: Optimal resuscitation in pediatric trauma an EAST multicenter study
 Study Title: Optimal resuscitation in pediatric trauma an EAST multicenter study PI/senior researcher: Richard Falcone Jr. MD, MPH Co-primary investigator: Stephanie Polites MD, MPH; Juan Gurria MD My
Study Title: Optimal resuscitation in pediatric trauma an EAST multicenter study PI/senior researcher: Richard Falcone Jr. MD, MPH Co-primary investigator: Stephanie Polites MD, MPH; Juan Gurria MD My
Nursing orientation for acute or critical care
 Clinical Evidence Review A regular feature of the American Journal of Critical Care, Clinical Evidence Review unveils available scientific evidence to answer questions faced in contemporary clinical practice.
Clinical Evidence Review A regular feature of the American Journal of Critical Care, Clinical Evidence Review unveils available scientific evidence to answer questions faced in contemporary clinical practice.
Passy-MuirInc. Helping the Chronically Critically Ill To Communicate: Speaking Valve Pilot Trial. A. Desai, MD1, L. Rho, MD1and J.
 American Journal of Respiratory Critical Care Medicine 179;2009:A3083 Helping the Chronically Critically Ill To Communicate: Speaking Valve Pilot Trial A. Desai, MD1, L. Rho, MD1and J. Nelson, MD, JD1
American Journal of Respiratory Critical Care Medicine 179;2009:A3083 Helping the Chronically Critically Ill To Communicate: Speaking Valve Pilot Trial A. Desai, MD1, L. Rho, MD1and J. Nelson, MD, JD1
Policy for Admission to Adult Critical Care Services
 Policy Number: CCaNNI 008 Title: Policy for Admission to Adult Critical Care Services Operational Date: Review Date: December 2009 December 2012 Type of Document: EQIA Screening Date: Corporate x Clinical
Policy Number: CCaNNI 008 Title: Policy for Admission to Adult Critical Care Services Operational Date: Review Date: December 2009 December 2012 Type of Document: EQIA Screening Date: Corporate x Clinical
The Hashemite University- School of Nursing Master s Degree in Nursing Fall Semester
 The Hashemite University- School of Nursing Master s Degree in Nursing Fall Semester Course Title: Statistical Methods Course Number: 0703702 Course Pre-requisite: None Credit Hours: 3 credit hours Day,
The Hashemite University- School of Nursing Master s Degree in Nursing Fall Semester Course Title: Statistical Methods Course Number: 0703702 Course Pre-requisite: None Credit Hours: 3 credit hours Day,
NURSING GUIDELINES TO PROCEDURAL SEDATION Finalized 1/18/2012 Procedural Sedation Task Force
 Intention (responsiveness) Responds normally to commands Responds purposefully to verbal commands/or light touch DEEP Responds to pain Reflex withdrawal No response Anticipated Outcomes (Airway, Cardiovascular)
Intention (responsiveness) Responds normally to commands Responds purposefully to verbal commands/or light touch DEEP Responds to pain Reflex withdrawal No response Anticipated Outcomes (Airway, Cardiovascular)
Effectiveness of respiratory rates in determining clinical deterioration: a systematic review protocol
 Effectiveness of respiratory rates in determining clinical deterioration: a systematic review protocol Rikke Rishøj Mølgaard 1 Palle Larsen 2 Sasja Jul Håkonsen 2 1 Department of Nursing, University College
Effectiveness of respiratory rates in determining clinical deterioration: a systematic review protocol Rikke Rishøj Mølgaard 1 Palle Larsen 2 Sasja Jul Håkonsen 2 1 Department of Nursing, University College
Improving Patient Satisfaction in the Orthopaedic Trauma Population
 ORIGINAL ARTICLE Improving Patient Satisfaction in the Orthopaedic Trauma Population Brent J. Morris, MD,* Justin E. Richards, MD, Kristin R. Archer, PhD, Melissa Lasater, MSN, ACNP, Denise Rabalais, BA,
ORIGINAL ARTICLE Improving Patient Satisfaction in the Orthopaedic Trauma Population Brent J. Morris, MD,* Justin E. Richards, MD, Kristin R. Archer, PhD, Melissa Lasater, MSN, ACNP, Denise Rabalais, BA,
A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs.
 6. Referral process Key findings A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs. Consultant physicians had no knowledge or input into
6. Referral process Key findings A high percentage of patients were referred to critical care by staff in training; 21% of referrals were made by SHOs. Consultant physicians had no knowledge or input into
Downloaded from ijn.iums.ac.ir at 18:00 IRDT on Saturday July 7th 2018
 :.... : ( ) ( ).. ().... SPSS. " ( ) : ".(P=/).(P=/ P=/ P=/ ) :. - - - - - - - : // : // : ( * ) () (). () ". Expiratory rib cage )" (compression (Squeezing) ().. (Forced expiratory volume). (). (-) ().
:.... : ( ) ( ).. ().... SPSS. " ( ) : ".(P=/).(P=/ P=/ P=/ ) :. - - - - - - - : // : // : ( * ) () (). () ". Expiratory rib cage )" (compression (Squeezing) ().. (Forced expiratory volume). (). (-) ().
Reimbursement for Non-Invasive Respiratory Support in Hospital Inpatient, Emergency Department and Other Outpatient Settings 1
 2400 Beacon St., #203, Chestnut Hill, MA 02467 617-645-8452 Reimbursement for Non-Invasive Respiratory Support in Hospital Inpatient, Emergency Department and Other Outpatient Settings 1 The purpose of
2400 Beacon St., #203, Chestnut Hill, MA 02467 617-645-8452 Reimbursement for Non-Invasive Respiratory Support in Hospital Inpatient, Emergency Department and Other Outpatient Settings 1 The purpose of
The Critical-Care Pain Observation Tool (CPOT) (Adapted from Gélinas et al., AJCC 2006; 15(4): )
 The Critical-Care Pain Observation Tool (CPOT) (Adapted from Gélinas et al., AJCC 2006; 15(4):420-427) Indicator Score Description Facial expressions Relaxed, neutral 0 No muscle tension observed Tense
The Critical-Care Pain Observation Tool (CPOT) (Adapted from Gélinas et al., AJCC 2006; 15(4):420-427) Indicator Score Description Facial expressions Relaxed, neutral 0 No muscle tension observed Tense
Implementation of a Multidisciplinary Ventilator-Weaning and Sedation Protocol in a Community Intensive Care Unit
 Research DIMENSION Implementation of a Multidisciplinary Ventilator-Weaning and Sedation Protocol in a Community Intensive Care Unit Amanda L. Rumpke, RN, MSN, ACNP, CCRN; Beth A. Zimmerman, RN, BSN Prolongation
Research DIMENSION Implementation of a Multidisciplinary Ventilator-Weaning and Sedation Protocol in a Community Intensive Care Unit Amanda L. Rumpke, RN, MSN, ACNP, CCRN; Beth A. Zimmerman, RN, BSN Prolongation
Thomas E Belda RRT, Ognjen Gajic MD, Jeffrey T Rabatin MD, and Barry A Harrison MD RESPIRATORY CARE SEPTEMBER 2004 VOL 49 NO
 Practice Variability in Management of Acute Respiratory Distress Syndrome: Bringing Evidence and Clinician Education to the Bedside Using a Web-Based Teaching Tool Thomas E Belda RRT, Ognjen Gajic MD,
Practice Variability in Management of Acute Respiratory Distress Syndrome: Bringing Evidence and Clinician Education to the Bedside Using a Web-Based Teaching Tool Thomas E Belda RRT, Ognjen Gajic MD,
PROMOTING HEALTHY BEHAVIORS IN NURSING STUDENTS. Donna Callaghan, PhD, RN-BC, GCNS-BC, CNE Associate Professor Faith Community Nurse
 PROMOTING HEALTHY BEHAVIORS IN NURSING STUDENTS Donna Callaghan, PhD, RN-BC, GCNS-BC, CNE Associate Professor Faith Community Nurse DISCLOSURE SLIDE AUTHOR: Donna Callaghan LEARNER OBJECTIVES: 1. Summarize
PROMOTING HEALTHY BEHAVIORS IN NURSING STUDENTS Donna Callaghan, PhD, RN-BC, GCNS-BC, CNE Associate Professor Faith Community Nurse DISCLOSURE SLIDE AUTHOR: Donna Callaghan LEARNER OBJECTIVES: 1. Summarize
does staff intervene; used? If not, describe.
 Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Cause of death in intensive care patients within 2 years of discharge from hospital
 Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Cause of death in intensive care patients within 2 years of discharge from hospital Peter R Hicks and Diane M Mackle Understanding of intensive care outcomes has moved from focusing on intensive care unit
Hospital-acquired infections (HAIs) can lead to longer stays, higher health care costs, and
 Feature Patients Hand Washing and Reducing Hospital- Acquired Infection Stacy Haverstick, RN, BSN, PCCN Cara Goodrich, MS, AGPCNP-BC Regi Freeman, RN, MSN, ACNS-BC Shandra James, RN, DNP Rajkiran Kullar,
Feature Patients Hand Washing and Reducing Hospital- Acquired Infection Stacy Haverstick, RN, BSN, PCCN Cara Goodrich, MS, AGPCNP-BC Regi Freeman, RN, MSN, ACNS-BC Shandra James, RN, DNP Rajkiran Kullar,
PULMONARY FUNCTION STUDIES
 Pulmonary Function StudiesApril 1, 2015 PREAMBLE PULMONARY FUNCTION STUDIES SPECIFIC ELEMENTS Pulmonary Function diagnostic procedures are divided into a professional component listed in the columns headed
Pulmonary Function StudiesApril 1, 2015 PREAMBLE PULMONARY FUNCTION STUDIES SPECIFIC ELEMENTS Pulmonary Function diagnostic procedures are divided into a professional component listed in the columns headed
Questions. Background to the ICNARC Case Mix Programme
 Number of admissions, unit length of stay and days of mechanical ventilation for admissions with blunt chest trauma to critical care in England, Wales and Northern Ireland Questions What were the number,
Number of admissions, unit length of stay and days of mechanical ventilation for admissions with blunt chest trauma to critical care in England, Wales and Northern Ireland Questions What were the number,
CLINICAL INVESTIGATIONS. Evaluation of simple criteria to predict successful weaning from mechanical ventilation in intensive care patients
 British Journal of Anaesthesia 92 (6): 793±9 (2004) DOI: 10.1093/bja/aeh139 Advance Access publication April 30, 2004 Evaluation of simple criteria to predict successful weaning from mechanical ventilation
British Journal of Anaesthesia 92 (6): 793±9 (2004) DOI: 10.1093/bja/aeh139 Advance Access publication April 30, 2004 Evaluation of simple criteria to predict successful weaning from mechanical ventilation
Identify Knowledge of Basic Cardiac Life Support among Nursing Student
 International Journal of Scientific and Research Publications, Volume 7, Issue 6, June 2017 733 Abstract Identify Knowledge of Basic Cardiac Life Support among Nursing Student Misbah Sabir Lahore School
International Journal of Scientific and Research Publications, Volume 7, Issue 6, June 2017 733 Abstract Identify Knowledge of Basic Cardiac Life Support among Nursing Student Misbah Sabir Lahore School
Changes in NHS organization of care and management of hospital admissions with COPD exacerbations between the national COPD audits of 2003 and 2008
 Q J Med 2011; 104:859 866 doi:10.1093/qjmed/hcr083 Advance Access Publication 26 May 2011 Changes in NHS organization of care and management of hospital admissions with COPD exacerbations between the national
Q J Med 2011; 104:859 866 doi:10.1093/qjmed/hcr083 Advance Access Publication 26 May 2011 Changes in NHS organization of care and management of hospital admissions with COPD exacerbations between the national
Technical Notes on the Standardized Hospitalization Ratio (SHR) For the Dialysis Facility Reports
 Technical Notes on the Standardized Hospitalization Ratio (SHR) For the Dialysis Facility Reports July 2017 Contents 1 Introduction 2 2 Assignment of Patients to Facilities for the SHR Calculation 3 2.1
Technical Notes on the Standardized Hospitalization Ratio (SHR) For the Dialysis Facility Reports July 2017 Contents 1 Introduction 2 2 Assignment of Patients to Facilities for the SHR Calculation 3 2.1
Gantt Chart. Critical Path Method 9/23/2013. Some of the common tools that managers use to create operational plan
 Some of the common tools that managers use to create operational plan Gantt Chart The Gantt chart is useful for planning and scheduling projects. It allows the manager to assess how long a project should
Some of the common tools that managers use to create operational plan Gantt Chart The Gantt chart is useful for planning and scheduling projects. It allows the manager to assess how long a project should
Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W
 Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W Record Status This is a critical abstract of an economic evaluation
Domiciliary non-invasive ventilation for recurrent acidotic exacerbations of COPD: an economic analysis Tuggey J M, Plant P K, Elliott M W Record Status This is a critical abstract of an economic evaluation
Using People, Process and Technology to Enhance Outcomes for Patients and Their Caregivers
 Using People, Process and Technology to Enhance Outcomes for Patients and Their Caregivers Melissa A. Fitzpatrick, RN, MSN, FAAN VP & Chief Clinical Officer, Hill-Rom Trends Driving Our Industry Aging
Using People, Process and Technology to Enhance Outcomes for Patients and Their Caregivers Melissa A. Fitzpatrick, RN, MSN, FAAN VP & Chief Clinical Officer, Hill-Rom Trends Driving Our Industry Aging
Mechanical Ventilation for Infants and Children Conference
 Duke University School of Medicine Division of 15th Optimizing Mechanical Ventilation for Infants and Children Conference An Interactive Conference April 16-18, 2018 COURSE DIRECTORS Ira Cheifetz MD FAARC
Duke University School of Medicine Division of 15th Optimizing Mechanical Ventilation for Infants and Children Conference An Interactive Conference April 16-18, 2018 COURSE DIRECTORS Ira Cheifetz MD FAARC
CA-1 CRITICAL CARE ROTATION University of Minnesota Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks
 CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
CA-1 CRITICAL CARE ROTATION Medical Center Fairview (UMMC) Rotation Site Director: Dr. Martin Birch Rotation Duration: 4 weeks Introduction: Critical Care is an integral aspect of anesthesiology training.
Guidelines on Postanaesthetic Recovery Care
 Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
Page 1 of 10 Guidelines on Postanaesthetic Recovery Care Version Effective Date 1 OCT 1992 2 FEB 2002 3 APR 2012 4 JUN 2017 Document No. HKCA P3 v4 Prepared by College Guidelines Committee Endorsed by
AICU/CICU guidelines for Prone Ventilation in Severe Hypoxic ARDS
 AICU/CICU guidelines for Prone Ventilation in Severe Hypoxic ARDS Issue:- Version2 Issue Date:- March2014 Review Date:- March 2017 Issued To:- All staff AICU Consultant Jonathan Chantler, Senior Sister
AICU/CICU guidelines for Prone Ventilation in Severe Hypoxic ARDS Issue:- Version2 Issue Date:- March2014 Review Date:- March 2017 Issued To:- All staff AICU Consultant Jonathan Chantler, Senior Sister
EFFECTIVENESS OF VIDEO ASSISTED TEACHING (VAT) ON KNOWLEDGE AND PRACTICE REGARDING PERSONAL HYGIENE AMONG SCHOOL CHILDREN
 Original Research Article Nursing International Journal of Pharma and Bio Sciences ISSN 0975-6299 EFFECTIVENESS OF VIDEO ASSISTED TEACHING (VAT) ON KNOWLEDGE AND PRACTICE REGARDING PERSONAL HYGIENE AMONG
Original Research Article Nursing International Journal of Pharma and Bio Sciences ISSN 0975-6299 EFFECTIVENESS OF VIDEO ASSISTED TEACHING (VAT) ON KNOWLEDGE AND PRACTICE REGARDING PERSONAL HYGIENE AMONG
Number of sepsis admissions to critical care and associated mortality, 1 April March 2013
 Number of sepsis admissions to critical care and associated mortality, 1 April 2010 31 March 2013 Question How many sepsis admissions to an adult, general critical care unit in England, Wales and Northern
Number of sepsis admissions to critical care and associated mortality, 1 April 2010 31 March 2013 Question How many sepsis admissions to an adult, general critical care unit in England, Wales and Northern
MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY
 POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
POLICY MONITORING AND SUPPORT OF PATIENTS RECEIVING MODERATE SEDATION AND ANALGESIA DURING DIAGNOSTIC AND THERAPUTIC PROCEDURES POLICY A policy sets forth the guiding principles for a specified targeted
Text-based Document. Daniel, Esther Shirley. Downloaded 12-May :19:50.
 The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
The Henderson Repository is a free resource of the Honor Society of Nursing, Sigma Theta Tau International. It is dedicated to the dissemination of nursing research, researchrelated, and evidence-based
Barriers to Early Rehabilitation in Critically Ill Patients. Shannon Goddard, MD Sunnybrook Health Sciences Centre
 Barriers to Early Rehabilitation in Critically Ill Patients Shannon Goddard, MD Sunnybrook Health Sciences Centre Disclosures/Funding No financial disclosures or conflicts of interest Work is funding by
Barriers to Early Rehabilitation in Critically Ill Patients Shannon Goddard, MD Sunnybrook Health Sciences Centre Disclosures/Funding No financial disclosures or conflicts of interest Work is funding by
Information systems with electronic
 Technology Innovations IT Sophistication and Quality Measures in Nursing Homes Gregory L. Alexander, PhD, RN; and Richard Madsen, PhD Abstract This study explores relationships between current levels of
Technology Innovations IT Sophistication and Quality Measures in Nursing Homes Gregory L. Alexander, PhD, RN; and Richard Madsen, PhD Abstract This study explores relationships between current levels of
Systematic Determination of Transplant In-Patient Acuity, Patient and Nurse Satisfaction. Objectives. Overview
 Systematic Determination of Transplant In-Patient Acuity, Patient and Nurse Satisfaction Michelle Floyd, RN Pre Transplant Coordinator and Presenter Ruth Tutor PhD, RN, APN, CCRN, CCNS, APRN-BC Critical
Systematic Determination of Transplant In-Patient Acuity, Patient and Nurse Satisfaction Michelle Floyd, RN Pre Transplant Coordinator and Presenter Ruth Tutor PhD, RN, APN, CCRN, CCNS, APRN-BC Critical
BeneVision N22/N19 Patient monitor
 BeneVision TM N22/N19 Patient Monitor Change your perspective, again. Maximize your confidence. Built for a paperless future. BeneVision N22/N19 Patient monitor Always in sight, always in mind Pls refer
BeneVision TM N22/N19 Patient Monitor Change your perspective, again. Maximize your confidence. Built for a paperless future. BeneVision N22/N19 Patient monitor Always in sight, always in mind Pls refer
Statistical Analysis of the EPIRARE Survey on Registries Data Elements
 Deliverable D9.2 Statistical Analysis of the EPIRARE Survey on Registries Data Elements Michele Santoro, Michele Lipucci, Fabrizio Bianchi CONTENTS Overview of the documents produced by EPIRARE... 3 Disclaimer...
Deliverable D9.2 Statistical Analysis of the EPIRARE Survey on Registries Data Elements Michele Santoro, Michele Lipucci, Fabrizio Bianchi CONTENTS Overview of the documents produced by EPIRARE... 3 Disclaimer...
ADVERSE EVENTS such as unexpected cardiac
 CONTINUING EDUCATION J Nurs Care Qual Vol. 22, No. 4, pp. 307 313 Copyright c 2007 Wolters Kluwer Health Lippincott Williams & Wilkins Implementation and Outcomes of a Rapid Response Team Susan J. McFarlan,
CONTINUING EDUCATION J Nurs Care Qual Vol. 22, No. 4, pp. 307 313 Copyright c 2007 Wolters Kluwer Health Lippincott Williams & Wilkins Implementation and Outcomes of a Rapid Response Team Susan J. McFarlan,
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert
 For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
For Vanderbilt Medical Center Carolyn Buppert, NP, JD Law Office of Carolyn Buppert www.buppert.com Describe the services in critical care that nurse practitioners perform that are billable Discuss what
ICU Restraint Reduction: Development of Evidence Based Tools to Guide Interventions
 ICU Restraint Reduction: Development of Evidence Based Tools to Guide Interventions January 2012 Sandy Maag, BSN, RN Manager of Nursing Quality Malissa Mulkey, MSN, APRN, CCRN, CCNS Neuroscience ICU &
ICU Restraint Reduction: Development of Evidence Based Tools to Guide Interventions January 2012 Sandy Maag, BSN, RN Manager of Nursing Quality Malissa Mulkey, MSN, APRN, CCRN, CCNS Neuroscience ICU &
CROSSING THE CHASM: ENGAGING NURSES IN QUALITY IMPROVEMENT AND EVIDENCE BASED PRACTICE
 CROSSING THE CHASM: ENGAGING NURSES IN QUALITY IMPROVEMENT AND EVIDENCE BASED PRACTICE Joy Goebel RN MN PhD Associate Professor of Nursing California State University Long Beach Objectives Discuss similarities
CROSSING THE CHASM: ENGAGING NURSES IN QUALITY IMPROVEMENT AND EVIDENCE BASED PRACTICE Joy Goebel RN MN PhD Associate Professor of Nursing California State University Long Beach Objectives Discuss similarities
The curriculum is based on achievement of the clinical competencies outlined below:
 ANESTHESIOLOGY CRITICAL CARE MEDICINE FELLOWSHIP Program Goals and Objectives The curriculum is based on achievement of the clinical competencies outlined below: Patient Care Fellows will provide clinical
ANESTHESIOLOGY CRITICAL CARE MEDICINE FELLOWSHIP Program Goals and Objectives The curriculum is based on achievement of the clinical competencies outlined below: Patient Care Fellows will provide clinical
Advisory on Granting Privileges for Deep Sedation to Non-Anesthesiologist Physicians
 Advisory on Granting Privileges for Deep Sedation to Non-Anesthesiologist Physicians Committee of Origin: Quality Management and Departmental Administration (Approved by the ASA House of Delegates on October
Advisory on Granting Privileges for Deep Sedation to Non-Anesthesiologist Physicians Committee of Origin: Quality Management and Departmental Administration (Approved by the ASA House of Delegates on October
SV 300 Ventilator. Compact yet powerful. Globally experienced, locally accessible
 Globally experienced, locally accessible Mindray is one of the leading global providers of medical devices and solutions. Firmly committed to our mission of sharing medical technologies with the world,
Globally experienced, locally accessible Mindray is one of the leading global providers of medical devices and solutions. Firmly committed to our mission of sharing medical technologies with the world,
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience. Presented by: Fadwa Jabboury, RN, MSN
 Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
Unplanned Extubation In Intensive Care Units (ICU) CMC Experience Presented by: Fadwa Jabboury, RN, MSN Introduction Basic Definitions: 1. Endotracheal intubation: A life saving procedure for critically
Part 4. Change Concepts for Improving Adult Cardiac Surgery. In this section, you will learn a group. of change concepts that can be applied in
 Change Concepts for Improving Adult Cardiac Surgery Part 4 In this section, you will learn a group of change concepts that can be applied in different ways throughout the system of adult cardiac surgery.
Change Concepts for Improving Adult Cardiac Surgery Part 4 In this section, you will learn a group of change concepts that can be applied in different ways throughout the system of adult cardiac surgery.
