Health Care Payment System Reform: Impact on Physician Assistants
|
|
|
- Warren Farmer
- 5 years ago
- Views:
Transcription
1 Health Care Payment System Reform: Impact on Physician Assistants Clearly, the Massachusetts universal coverage health care initiative has been a success in providing increased coverage to citizens of Massachusetts. Data continues to show that well over 90% of Massachusetts residents are covered. But that accomplishment is just the first, and some would argue the easiest, step in a very complicated and arduous process of reforming health care in the state, and in the country. Two equally important pieces of the puzzle include finding appropriate ways to control rapidly escalating costs while at the same time achieving improvements in the quality of the care being delivered. The Massachusetts Association of Physician Assistants (MAPA) appreciates the opportunity to provide input into the discussion as policy makers seek to further develop the frame work and methodology of payment system reform. MAPA is strongly committed to participating in health reform activities that will lead to improved health outcomes for the citizens of the Commonwealth. Caring for our patients remains the overarching goal and focus of our efforts. Thoughts on accountable care organizations (ACOs) are included in our comments. We also focus on the specific impact that such care models and potential payment reform activities will have on the ability of physician assistants (PAs) to maintain and increase their role as key providers of care in the state, and what changes could be made in state policies to enhance patient care by strengthening the PA role. PAs are part of the physician PA team and share many of the same concerns as physicians. However, there are some unique challenges faced by the PA profession as part of these reform activities. Access and Maximum Utilization of Health Care Professionals Any successful care model requires an adequate supply and mix of health care professionals. There has been an acknowledged decline in the primary care work force making it all the more important to fully engage health care professionals who can deliver primary care services. The Physician Workforce Study published by the Massachusetts Medical Society has shown that close to fifty percent of internists are not accepting new patients. Physician assistants are educated and trained in the generalist model making them ideally suited to be important players in integrated and interdisciplinary teams, and coordinated care models. PAs increase access to primary care services, provide continuity of care to some of the sickest patients within the healthcare system and provide high quality care in many cases at a lower cost. As the health care system seeks to reform payment methodologies and promote new models of care, it is imperative that the contribution of all health care professionals be recognized and supported within the system. One factor that hinders efficiency in the health care arena occurs when health care professionals are not authorized and enabled to deliver care to the full extent of their education and training. (Please see Appendix A for a summary of barriers to PA practice and how PAs fit into payment reform in Massachusetts) Recognition of the medical skill set that PAs offer and their ability to deliver care autonomously as part of the physician PA team Recognition of PAs as eligible professionals in all programs (e.g., medical home, ACOs). Removal of barriers in state law and federal regulations to allow PAs to deliver care to the highest level of their license. Practice friendly supervision and co signature requirements. Hospital physician gainsharing arrangements and necessary anti trust exemptions being extended to PAs. 12/6/2010 1
2 Assistance in the education of PA students (rotation sights/loan forgiveness). Examples/Consequences When PAs Were Excluded from Health Care Programs Several years ago, when state Medicaid programs shifted to managed care type plans through the waiver process, PAs were not listed by the federal government as primary care providers (PCPs). The federal government allowed, but did not mandate, that PAs be considered as PCPs. States often assigned a certain number of Medicaid patients to a practice based on the number of PCPs (i.e., 1500 patients per PCP). This was often known as a panel of patients. A practice that had a physician and a PA had the capacity to treat 3,000 Medicaid patients. However, if the particular state did not recognize PAs as PCPs, the state often assigned only 1,500 patients to the practice, severely underutilizing the physician PA team and often limiting access to Medicaid patients. State officials assumed that because PAs worked closely with physicians there was no need to separately list them in health care programs. This was an incorrect assumption and we do not want to repeat that scenario as the net effect is to limit patient access to needed medical care services. ACOs Accountable care organizations (ACOs) have the ability to marshal the resources to provide the wide spectrum of care required by patients. Coordination of care principles and a reliance on best practices guidelines maintained across the ACO would, in theory, bring about higher quality, consistent care. The federal health care reform bill, the Patient Protection and Affordable Care Act, includes PAs in its definition of eligible providers in ACOs. State guidelines/language should also specifically include PAs as authorized or eligible health care professionals. Better care coordination will improve patient health status and lower health costs, but results may not be immediate. ACOs and other arrangements are, for the most part, theoretical entities that need time to develop efficiencies and create effective interdisciplinary teams among the health care professionals and the organizations that will be affiliated with the ACO. It may take some time before substantial cost savings are realized. 12/6/2010 2
3 Global (Bundled) Payments We acknowledge that the predominant payment systems currently in use, those based on a fee forservice (FFS) model, improperly incentivize volume of care as opposed to quality of care and quality outcomes. The FFS model, almost by design, encourages gaps in care or fragmentation in the system with little incentive for coordinated care. Global payments for episodes of care or care encounters in and of themselves will not reduce health care cost or improve the quality of care. Policy makers must determine, not necessarily utilizing the traditional fee for service fee schedules, a reasonable payment for an episode of care that covers the true cost of delivering care. Using the fee for service model as a template will simply perpetuate a payment system that has traditionally overpaid specialty and procedure based care and underpaid primary care services. A step by step analysis of the actual steps and professionals delivering services or episodes of care (including all professionals who play a medically necessary role) might be the only method to properly determine a reasonable cost of providing care. Competition over payments may lead to the trickledown theory. PAs are potentially at a disadvantage when compared to hospitals and physicians in terms of who controls the payment and how it will be divided. PAs may be employed by the hospital, by a physician group, or as independent contractors. No matter which arrangement is in place, appropriate coverage of the professional services delivered by the PA must be maintained, even within an ACO type of delivery model. Exposure to risk (and reward) will likely be an important component of global payments with rewards due to savings in the system being available for incentivizing optimal outcomes. Simply being an efficient health care professional or practice will not guarantee success. If other players who share in the responsibility for patient care (hospitals, physician practices, physical therapy, home health agencies, etc.) are not efficient providers of care then the expected savings of coordinated care could be lost for all involved. Good clinical behavior by some could go unrewarded if other parts of the ACO fail in their attempts to deliver high quality care. Recognizing PAs as providers creates a mechanism to properly collect and measure quality data on the care being delivered by the PAs. Right now the system is only able to track those providers billing under their specific identifiers, most of the work done by PAs is silent to the system because it is captured under a physician identifier. PAs saw 257 million patients nationwide in Most health care professionals are not accustomed to dealing with risk. Under fee for service there is little risk since variables such as patient outcomes were not factored into payment. There will need to be certain financial safeguards built into global payments to assure that there are appropriate limits on downside risk due to inadequate global payments or inaccurate patient acuity assessments (risk adjusters). If payments are artificially low and fail to cover the cost of delivering care, access issues will only be exacerbated as more health care professionals will leave medicine, leave the state, or potentially limit the care they provide. 12/6/2010 3
4 The concept of attempting to align traditionally dissimilar entities, such as hospitals and health care professionals, is one that historically has been difficult to manage. A lack of trust permeates the atmosphere whenever there is a discussion about changing rates or methodologies related to payment all sides want to know who will win or lose. Many health care professionals and institutions are experiencing a type of déjà vu. Unsuccessful familiar concepts utilized in the 90s include managed care models, hospitals buying physician practices, then called PHO or physician hospital organizations, and capitated payments. Irrespective of the type of delivery and payment systems that are ultimately adopted in the state, there will be a need for appropriately trained health care professionals. PAs are an essential component of the provider infrastructure and it is imperative that they be included among those who deliver primary medical care to patients. 12/6/2010 4
5 Appendix A: Summary of Barriers to PA Practice and how PAs fit into payment reform in Massachusetts Define PAs as eligible providers in ACOS; federal health care reform bill, the Patient Protection and Affordable Care Act, includes PAs in its definition of eligible providers in ACOs. State guidelines/language should also specifically include PAs as authorized or eligible health care professionals. Hospital physician gainsharing arrangements and necessary anti trust exemptions should be extended to PAs. Recognize the role of PAs as primary care providers; this has been made at the federal level, with passage of the landmark Patient Protection and Affordable Care Act. PAs are recognized as providers within the primary care team and allows PAs to lead a home based primary care team as part of an independence at home medical practice. This is not to be interpreted as independent practice but should be viewed as autonomous practice within a team oriented physician PA team. Maximize the number of necessary providers of primary care creating much needed access to primary care services which lowers the overall cost of healthcare. Recognize and reimburse for services provided by PAs based on quality measures and outcome data. No matter which arrangement is in place, appropriate coverage of the professional services delivered by the PA must be maintained, even within an ACO type of delivery model. All providers will need to accept risk within the system. Federal health care reform bill, the Patient Protection and Affordable Care Act, creates a 5 year 10% Medicare bonus for select primary care codes furnished by PAs, as well as other primary care providers. This holds all providers to equal and high quality medical practice standards. Assess how PAs will fit into a new payment structure by reviewing data provided to state entities like the Roadmap to Cost Containment presented by the Rand Health Corporation to the Massachusetts HCQCC which states the average cost of a PA visit is 20% to 35% lower than the average cost of an office visit with a physician with an estimated savings range of $4.2 billion to $8.4 billion over ten years. A stepby step analysis of the actual steps and professionals delivering services or episodes of care might be the only method to properly determine a reasonable cost of providing care. There is much literature out there in regards to the high quality care PAs provide, by reviewing and understanding this data, decisions for including PAs will be based on sound data analysis. Eliminate the restriction specifying the number of PAs a physician can supervise; the American Medical Association (AMA) has officially supported the principle that the appropriate ratio of physician to PA should be determined by the physicians at the practice level as long as its consistent with high quality medical practice. This was a recommendation included as a barrier to increased utilization of PAs in the state by the Rand Health Corporation Study aforementioned above. Many PAs provide off hours coverage for patients keeping them out of hospitals and emergency rooms. Removing this barrier ensures efficient health care delivery based on the needs of the practice and patients. 12/6/2010 5
6 Include PAs in loan repayment programs and institutional recruitment efforts; Chapter 305 of the Acts of 2008 initiated the creation of Workforce Center which was tasked with addressing the workforce shortage in part through loan repayment programs and support for institutional recruitment efforts for physicians and nurse who serve in primary care and underserved areas. PAs were NOT included in this effort and should be. Increases much needed access in underserved areas and community centers for patients. Modernize Medicaid regulations to be inline with current Medicare standards to include; mandate the credentialing and enrollment of PAs reimburse for first assisting when Medicare standards are met, remove the requirement for physician co signature on hospital medical records, PT/OT/Speech referrals. Removes unnecessary barriers to MD and PA practice, encouraging more efficient practice. Appoint PA representation from the Massachusetts Association of PAs to appropriate health reform committees moving forward. PA representation was not included when the Advisory Committee to the Health Care Quality and Cost Council was formed after the passage of Chapter 305. Both MD and NP representation were included. The Advisory Committee members serve on other committees involved in state healthcare and payment reform like the Committee on the Status of Payment Reform Legislation. Having PA representation and input on reform policy and legislation would allow for expert input to PA practice moving forward. Make PAs a licensed profession, rather than registered ; 46 states and D.C. use the term licensure for PAs. Only Massachusetts and New York use registered, while Ohio and Vermont use certified. Both New York and Vermont are planning legislative action to move to licensure in Avoid patient confusion and recognition of what the actual credentials are for PAs. Eliminate requirement for chart co signature on all Sch. II prescriptions by PAs within 96 hours; this can cause inefficiencies in the delivery of patient care and creates an unnecessary burden on the supervising physician. Decisions about chart co signature should be made at the practice level to allow for maximum practice efficiency. Prescriptive practice guidelines which are already in place provide the necessary communication between PA and MD regarding the prescribing of medication. 12/6/2010 6
Comparison of ACP Policy and IOM Report Graduate Medical Education That Meets the Nation's Health Needs
 IOM Recommendation Recommendation 1: Maintain Medicare graduate medical education (GME) support at the current aggregate amount (i.e., the total of indirect medical education and direct graduate medical
IOM Recommendation Recommendation 1: Maintain Medicare graduate medical education (GME) support at the current aggregate amount (i.e., the total of indirect medical education and direct graduate medical
Re: Medicare Program; Medicare Shared Savings Program: Accountable Care Organizations, Proposed rule.
 June 3, 2011 Donald Berwick, MD Administrator Centers for Medicare & Medicaid Services, Department of Health and Human Services, Attention: CMS-1345-P, Mail Stop C4-26-05, 7500 Security Boulevard, Baltimore,
June 3, 2011 Donald Berwick, MD Administrator Centers for Medicare & Medicaid Services, Department of Health and Human Services, Attention: CMS-1345-P, Mail Stop C4-26-05, 7500 Security Boulevard, Baltimore,
Alternative Managed Care Reimbursement Models
 Alternative Managed Care Reimbursement Models David R. Swann, MA, LCSA, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Healthcare Reform Trends in 2015 Moving from carve out Medicaid
Alternative Managed Care Reimbursement Models David R. Swann, MA, LCSA, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Healthcare Reform Trends in 2015 Moving from carve out Medicaid
The Accountable Care Organization Specific Objectives
 Accountable Care Organizations and You E. Christopher h Ellison, MD, F.A.C.S Senior Associate Vice President for Health Sciences CEO, OSU Faculty Group Practice Chair, Department of Surgery Ohio State
Accountable Care Organizations and You E. Christopher h Ellison, MD, F.A.C.S Senior Associate Vice President for Health Sciences CEO, OSU Faculty Group Practice Chair, Department of Surgery Ohio State
Medicaid Efficiency and Cost-Containment Strategies
 Medicaid Efficiency and Cost-Containment Strategies Medicaid provides comprehensive health services to approximately 2 million Ohioans, including low-income children and their parents, as well as frail
Medicaid Efficiency and Cost-Containment Strategies Medicaid provides comprehensive health services to approximately 2 million Ohioans, including low-income children and their parents, as well as frail
Transitioning to a Value-Based Accountable Health System Preparing for the New Business Model. The New Accountable Care Business Model
 Transitioning to a Value-Based Accountable Health System Preparing for the New Business Model Michael C. Tobin, D.O., M.B.A. Interim Chief medical Officer Health Networks February 12, 2011 2011 North Iowa
Transitioning to a Value-Based Accountable Health System Preparing for the New Business Model Michael C. Tobin, D.O., M.B.A. Interim Chief medical Officer Health Networks February 12, 2011 2011 North Iowa
Request for Information Regarding Accountable Care Organizations (ACOs) and Medicare Shared Savings Programs (CMS-1345-NC)
 Via Electronic Submission Donald Berwick, MD, MPP Administrator Centers for Medicare & Medicaid Services ATTN: CMS-1345-NC 7500 Security Blvd. Baltimore, MD 21244-8013 Re: Request for Information Regarding
Via Electronic Submission Donald Berwick, MD, MPP Administrator Centers for Medicare & Medicaid Services ATTN: CMS-1345-NC 7500 Security Blvd. Baltimore, MD 21244-8013 Re: Request for Information Regarding
Physician-led health care teams. AMA Advocacy Resource Center. Resource materials to support state legislative and regulatory campaigns
 ama-assn.org/go/physicianledteams AMA Advocacy Resource Center Physician-led health care teams Resource materials to support state legislative and regulatory campaigns Page 2 AMA Advocacy Resource Center
ama-assn.org/go/physicianledteams AMA Advocacy Resource Center Physician-led health care teams Resource materials to support state legislative and regulatory campaigns Page 2 AMA Advocacy Resource Center
The Center for Medicare & Medicaid Innovations: Programs & Initiatives
 The Center for Medicare & Medicaid Innovations: Programs & Initiatives Rob Stone, Esq. American Health Lawyers Association Institute on Medicare & Medicaid Payment Issues March 30-April 1, 2012 CMMI Mission
The Center for Medicare & Medicaid Innovations: Programs & Initiatives Rob Stone, Esq. American Health Lawyers Association Institute on Medicare & Medicaid Payment Issues March 30-April 1, 2012 CMMI Mission
The Pain or the Gain?
 The Pain or the Gain? Comprehensive Care Joint Replacement (CJR) Model DRG 469 (Major joint replacement with major complications) DRG 470 (Major joint without major complications or comorbidities) Actual
The Pain or the Gain? Comprehensive Care Joint Replacement (CJR) Model DRG 469 (Major joint replacement with major complications) DRG 470 (Major joint without major complications or comorbidities) Actual
Roadmap for Transforming America s Health Care System
 Roadmap for Transforming America s Health Care System America s health care system requires transformational change to provide all health care participants with broader access and choice, improved quality
Roadmap for Transforming America s Health Care System America s health care system requires transformational change to provide all health care participants with broader access and choice, improved quality
REPORT OF THE BOARD OF TRUSTEES
 REPORT OF THE BOARD OF TRUSTEES B of T Report 21-A-17 Subject: Presented by: Risk Adjustment Refinement in Accountable Care Organization (ACO) Settings and Medicare Shared Savings Programs (MSSP) Patrice
REPORT OF THE BOARD OF TRUSTEES B of T Report 21-A-17 Subject: Presented by: Risk Adjustment Refinement in Accountable Care Organization (ACO) Settings and Medicare Shared Savings Programs (MSSP) Patrice
Evaluation & Management ( E/M ) Payment and Documentation Requirements
 National Partnership for Hospice Innovation 1299 Pennsylvania Ave., Suite 1175 Washington DC, 20004 September 10, 2017 Seema Verma Administrator Centers for Medicare & Medicaid Services, Department of
National Partnership for Hospice Innovation 1299 Pennsylvania Ave., Suite 1175 Washington DC, 20004 September 10, 2017 Seema Verma Administrator Centers for Medicare & Medicaid Services, Department of
Long term commitment to a new vision. Medical Director February 9, 2011
 ACCOUNTABLE CARE ORGANIZATION (ACO): Long term commitment to a new vision Michael Belman MD Michael Belman MD Medical Director February 9, 2011 Physician Reimbursement There are three ways to pay a physician,
ACCOUNTABLE CARE ORGANIZATION (ACO): Long term commitment to a new vision Michael Belman MD Michael Belman MD Medical Director February 9, 2011 Physician Reimbursement There are three ways to pay a physician,
Succeeding with Accountable Care Organizations
 Succeeding with Accountable Care Organizations The Point B Webinar Series October 25, 2011 Today s Discussion Key ACO trends and emerging models Critical success factors for building an ACO Developing
Succeeding with Accountable Care Organizations The Point B Webinar Series October 25, 2011 Today s Discussion Key ACO trends and emerging models Critical success factors for building an ACO Developing
Connected Care Partners
 Connected Care Partners Our Discussion Today Introducing the Connected Care Partners CIN What is a Clinically Integrated Network (CIN) and why is the time right to join the Connected Care Partners CIN?
Connected Care Partners Our Discussion Today Introducing the Connected Care Partners CIN What is a Clinically Integrated Network (CIN) and why is the time right to join the Connected Care Partners CIN?
Doctor Shortage: CONDITION CRITICAL RESULTS OF HANYS 2012 PHYSICIAN ADVOCACY SURVEY
 Doctor Shortage: CONDITION CRITICAL RESULTS OF HANYS 2012 PHYSICIAN ADVOCACY SURVEY Primary care physicians are at the forefront of a physician shortage that continues to worsen in New York State, according
Doctor Shortage: CONDITION CRITICAL RESULTS OF HANYS 2012 PHYSICIAN ADVOCACY SURVEY Primary care physicians are at the forefront of a physician shortage that continues to worsen in New York State, according
April 26, Ms. Seema Verma, MPH Administrator Centers for Medicare & Medicaid Services. Dear Secretary Price and Administrator Verma:
 April 26, 2017 Thomas E. Price, MD Secretary Department of Health and Human Services Hubert H. Humphrey Building 200 Independence Avenue, SW Washington, DC 20201 Ms. Seema Verma, MPH Administrator Centers
April 26, 2017 Thomas E. Price, MD Secretary Department of Health and Human Services Hubert H. Humphrey Building 200 Independence Avenue, SW Washington, DC 20201 Ms. Seema Verma, MPH Administrator Centers
UAMS/SVI Partnership Agreement. Proposal
 UAMS/SVI Partnership Agreement Proposal Introduction The University of Arkansas for Medical Sciences (UAMS) is the health sciences and academic medical component of the University of Arkansas. St Vincent
UAMS/SVI Partnership Agreement Proposal Introduction The University of Arkansas for Medical Sciences (UAMS) is the health sciences and academic medical component of the University of Arkansas. St Vincent
Mental Health Liaison Group
 Mental Health Liaison Group The Honorable Nancy Pelosi The Honorable Harry Reid Speaker Majority Leader United States House of Representatives United States Senate Washington, DC 20515 Washington, DC 20510
Mental Health Liaison Group The Honorable Nancy Pelosi The Honorable Harry Reid Speaker Majority Leader United States House of Representatives United States Senate Washington, DC 20515 Washington, DC 20510
Nov. 17, Dear Mr. Slavitt:
 Nov. 17, 2015 Mr. Andrew Slavitt Acting Administrator Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services 200 Independence Avenue, S.W. Washington, DC 20201 Re: NAMD
Nov. 17, 2015 Mr. Andrew Slavitt Acting Administrator Centers for Medicare and Medicaid Services U.S. Department of Health and Human Services 200 Independence Avenue, S.W. Washington, DC 20201 Re: NAMD
EHR Implementation Best Practices. EHR White Paper
 EHR White Paper EHR Implementation Best Practices An EHR implementation that increases efficiencies versus an EHR that is underutilized, abandoned or replaced. pulseinc.com EHR Implementation Best Practices
EHR White Paper EHR Implementation Best Practices An EHR implementation that increases efficiencies versus an EHR that is underutilized, abandoned or replaced. pulseinc.com EHR Implementation Best Practices
Federal Policy Agenda / 2016 & Beyond
 Federal Policy Agenda / 2016 & Beyond Compassion & Choices is the leading national nonprofit organization dedicated to improving care and expanding choice for people with advanced illness, and nearing
Federal Policy Agenda / 2016 & Beyond Compassion & Choices is the leading national nonprofit organization dedicated to improving care and expanding choice for people with advanced illness, and nearing
Is Audiology effected by the Changes or will it be?
 Is Audiology effected by the Changes or will it be? The basic problem The U.S. has the highest absolute medical expenditures and highest per capita medical expenditures of any nation. The U.S. also has
Is Audiology effected by the Changes or will it be? The basic problem The U.S. has the highest absolute medical expenditures and highest per capita medical expenditures of any nation. The U.S. also has
Shifting from Volume to Value-based Healthcare. November 2014 Briefing
 Shifting from Volume to Value-based Healthcare November 2014 Briefing The Healthcare Collaborative of Greater Columbus is a non-profit, public-private partnership. We serve as a catalyst, convener, and
Shifting from Volume to Value-based Healthcare November 2014 Briefing The Healthcare Collaborative of Greater Columbus is a non-profit, public-private partnership. We serve as a catalyst, convener, and
Assignment of Medicare Fee-for-Service Beneficiaries
 February 6, 2015 Ms. Marilyn B. Tavenner, Administrator Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-1461-P Room 445-G, Hubert H. Humphrey Building 200
February 6, 2015 Ms. Marilyn B. Tavenner, Administrator Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-1461-P Room 445-G, Hubert H. Humphrey Building 200
Medicaid Update Special Edition Budget Highlights New York State Budget: Health Reform Highlights
 Page 1 of 6 New York State April 2009 Volume 25, Number 4 Medicaid Update Special Edition 2009-10 Budget Highlights David A. Paterson, Governor State of New York Richard F. Daines, M.D. Commissioner New
Page 1 of 6 New York State April 2009 Volume 25, Number 4 Medicaid Update Special Edition 2009-10 Budget Highlights David A. Paterson, Governor State of New York Richard F. Daines, M.D. Commissioner New
Partnering with hospitals to create an accountable care organization Elias N. Matsakis, Esq.
 Partnering with hospitals to create an accountable care organization Elias N. Matsakis, Esq. There are many opportunities for physicians and hospitals to affiliate and clinically integrate so as to enable
Partnering with hospitals to create an accountable care organization Elias N. Matsakis, Esq. There are many opportunities for physicians and hospitals to affiliate and clinically integrate so as to enable
Value-Based Contracting
 Value-Based Contracting AUTHOR Melissa Stahl Research Manager, The Health Management Academy 2018 Lumeris, Inc 1.888.586.3747 lumeris.com Introduction As the healthcare industry continues to undergo transformative
Value-Based Contracting AUTHOR Melissa Stahl Research Manager, The Health Management Academy 2018 Lumeris, Inc 1.888.586.3747 lumeris.com Introduction As the healthcare industry continues to undergo transformative
HEALTH PROFESSIONAL WORKFORCE
 HEALTH PROFESSIONAL WORKFORCE (SECTION-BY-SECTION ANALYSIS) (Information compiled from the Democratic Policy Committee (DPC) Report on The Patient Protection and Affordable Care Act and the Health Care
HEALTH PROFESSIONAL WORKFORCE (SECTION-BY-SECTION ANALYSIS) (Information compiled from the Democratic Policy Committee (DPC) Report on The Patient Protection and Affordable Care Act and the Health Care
Global Budget Revenue. October 8, 2015
 Global Budget Revenue October 8, 2015 Goals Understand GBR s connection to the goals of Maryland s Demonstration Understand impact on budgeting and planning for RFP and future phases Answer questions that
Global Budget Revenue October 8, 2015 Goals Understand GBR s connection to the goals of Maryland s Demonstration Understand impact on budgeting and planning for RFP and future phases Answer questions that
December 3, 2010 BY COURIER AND ELECTRONIC MAIL
 Charles N. Kahn III President & CEO December 3, 2010 BY COURIER AND ELECTRONIC MAIL Donald Berwick, M.D. Administrator Centers for Medicare & Medicaid Services Attention: CMS-6028-P Hubert H. Humphrey
Charles N. Kahn III President & CEO December 3, 2010 BY COURIER AND ELECTRONIC MAIL Donald Berwick, M.D. Administrator Centers for Medicare & Medicaid Services Attention: CMS-6028-P Hubert H. Humphrey
Re: CMS Code 3310-P. May 29, 2015
 May 29, 2015 Centers for Medicare & Medicaid Services Department of Health and Human Services P.O. Box 8013 Baltimore, MD 21244-8013 Attention: CMS-3310-P Re: The Centers for Medicare Medicaid Services
May 29, 2015 Centers for Medicare & Medicaid Services Department of Health and Human Services P.O. Box 8013 Baltimore, MD 21244-8013 Attention: CMS-3310-P Re: The Centers for Medicare Medicaid Services
The Evolving Practice of Nursing Pamela S. Dickerson, PhD, RN-BC. PRN Continuing Education January-March, 2011
 The Evolving Practice of Nursing Pamela S. Dickerson, PhD, RN-BC PRN Continuing Education January-March, 2011 Disclaimer/Disclosures Purpose: The purpose of this session is to enable the nurse to be proactive
The Evolving Practice of Nursing Pamela S. Dickerson, PhD, RN-BC PRN Continuing Education January-March, 2011 Disclaimer/Disclosures Purpose: The purpose of this session is to enable the nurse to be proactive
North Country Community Mental Health Response to MDCH Request for Information Medicare and Medicaid Dual Eligible Project September 2011
 North Country Community Mental Health Response to MDCH Request for Information Medicare and Medicaid Dual Eligible Project September 2011 1. What is working well in the current system of services and supports
North Country Community Mental Health Response to MDCH Request for Information Medicare and Medicaid Dual Eligible Project September 2011 1. What is working well in the current system of services and supports
National Multiple Sclerosis Society
 National Multiple Sclerosis Society National 1 Kim, National diagnosed MS in Society 2000 > HEALTH CARE REFORM PRINCIPLES America s health care crisis prevents many people with multiple sclerosis from
National Multiple Sclerosis Society National 1 Kim, National diagnosed MS in Society 2000 > HEALTH CARE REFORM PRINCIPLES America s health care crisis prevents many people with multiple sclerosis from
Primary Care 101: A Glossary for Prevention Practitioners
 PREVENTION COLLABORATION IN ACTION Engaging the Right Partners Primary Care 101: A Glossary for Prevention Practitioners As the U.S. healthcare landscape continues to change under the Affordable Care Act
PREVENTION COLLABORATION IN ACTION Engaging the Right Partners Primary Care 101: A Glossary for Prevention Practitioners As the U.S. healthcare landscape continues to change under the Affordable Care Act
The American Recovery and Reinvestment Act: Incentivizing Investments in Healthcare
 The American Recovery and Reinvestment Act: Incentivizing Investments in Healthcare AT&T, Healthcare, and You Overview The American Recovery and Reinvestment Act of 2009 (ARRA) allocated more than $180
The American Recovery and Reinvestment Act: Incentivizing Investments in Healthcare AT&T, Healthcare, and You Overview The American Recovery and Reinvestment Act of 2009 (ARRA) allocated more than $180
1. The new state-based insurance exchange for small businesses (SHOP) stands for:
 Chapter 5 Review Questions 1. The new state-based insurance exchange for small businesses (SHOP) stands for: a. Small Business Health Options Program b. Small Business Health Option Plans c. State Health
Chapter 5 Review Questions 1. The new state-based insurance exchange for small businesses (SHOP) stands for: a. Small Business Health Options Program b. Small Business Health Option Plans c. State Health
Re: Rewarding Provider Performance: Aligning Incentives in Medicare
 September 25, 2006 Institute of Medicine 500 Fifth Street NW Washington DC 20001 Re: Rewarding Provider Performance: Aligning Incentives in Medicare The American College of Physicians (ACP), representing
September 25, 2006 Institute of Medicine 500 Fifth Street NW Washington DC 20001 Re: Rewarding Provider Performance: Aligning Incentives in Medicare The American College of Physicians (ACP), representing
NYS Value Based Payments (VBP):
 NYS Value Based Payments (VBP): Provider Associations, Community Based Organizations, and Consumer Advocates Town Hall Meeting Jason Helgerson NYS Medicaid Director December 16, 2016 2 Today s Agenda Agenda
NYS Value Based Payments (VBP): Provider Associations, Community Based Organizations, and Consumer Advocates Town Hall Meeting Jason Helgerson NYS Medicaid Director December 16, 2016 2 Today s Agenda Agenda
MEDICAL HOMES Arkansas Hospital Association
 MEDICAL HOMES Arkansas Hospital Association Framing our discussion Environmental snapshot of health care Hospitals and the PCMH Arkansas Medical Homes Patients/Consumers 2 1 Health Policy is changing Budget
MEDICAL HOMES Arkansas Hospital Association Framing our discussion Environmental snapshot of health care Hospitals and the PCMH Arkansas Medical Homes Patients/Consumers 2 1 Health Policy is changing Budget
Healthy Aging Recommendations 2015 White House Conference on Aging
 Healthy Aging Recommendations 2015 White House Conference on Aging Chronic diseases are the leading causes of death and disability in the U.S. and account for 75% of the nation s health care spending.
Healthy Aging Recommendations 2015 White House Conference on Aging Chronic diseases are the leading causes of death and disability in the U.S. and account for 75% of the nation s health care spending.
RE: CMS-1631-PM Medicare Program; Revisions to Payment Policies under the Physician Fee Schedule and Other Revisions to Part B for CY 2016
 September 8, 2015 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-2333-P Mail Stop C4-26-05 7500 Security Boulevard Baltimore, MD 21244-1850 Main Office
September 8, 2015 Centers for Medicare & Medicaid Services Department of Health and Human Services Attention: CMS-2333-P Mail Stop C4-26-05 7500 Security Boulevard Baltimore, MD 21244-1850 Main Office
Alternative Payment Models for Behavioral Health Kim Cox VP, Provider Network
 Alternative Payment Models for Behavioral Health Kim Cox VP, Provider Network Kim Cox Vice President, Provider Network, Optum Kim Cox is Vice President of Provider Network. She joined Optum in February
Alternative Payment Models for Behavioral Health Kim Cox VP, Provider Network Kim Cox Vice President, Provider Network, Optum Kim Cox is Vice President of Provider Network. She joined Optum in February
Executive, Legislative & Regulatory 2018 AGENDA. unitypoint.org/govaffairs
 Executive, Legislative & Regulatory 2018 AGENDA unitypoint.org/govaffairs Dear Policy Makers and Community Stakeholders, In the midst of tumultuous times, we bring you our 2018 State Legislative Agenda.
Executive, Legislative & Regulatory 2018 AGENDA unitypoint.org/govaffairs Dear Policy Makers and Community Stakeholders, In the midst of tumultuous times, we bring you our 2018 State Legislative Agenda.
Paying for Value and Aligning with Other Purchasers
 Paying for Value and Aligning with Other Purchasers NAMD Bootcamp, Lake Tahoe, May 18, 2014 Dianne Hasselman, Director, Value Based Purchasing, Center for Health Care Strategies Deidre Gifford, MD, Medicaid
Paying for Value and Aligning with Other Purchasers NAMD Bootcamp, Lake Tahoe, May 18, 2014 Dianne Hasselman, Director, Value Based Purchasing, Center for Health Care Strategies Deidre Gifford, MD, Medicaid
PHCA Webinar January 30, Latsha Davis & McKenna, P.C. Kimber L. Latsha, Esq.
 PHCA Webinar January 30, 2014 Latsha Davis & McKenna, P.C. Kimber L. Latsha, Esq. 1 2 Intended to: Encourage the development of ACOs in Medicare Promotes accountability for a patient population and coordinates
PHCA Webinar January 30, 2014 Latsha Davis & McKenna, P.C. Kimber L. Latsha, Esq. 1 2 Intended to: Encourage the development of ACOs in Medicare Promotes accountability for a patient population and coordinates
National Coalition on Care Coordination (N3C) Care Coordination and the Role of the Aging Network. Monday, September 12, 2011
 National Coalition on Care Coordination (N3C) Care Coordination and the Role of the Aging Network Monday, September 12, 2011 Washington, DC Hyatt Regency on Capitol Hill Yellowstone/Everglades 4:00 PM
National Coalition on Care Coordination (N3C) Care Coordination and the Role of the Aging Network Monday, September 12, 2011 Washington, DC Hyatt Regency on Capitol Hill Yellowstone/Everglades 4:00 PM
Thought Leadership Series White Paper The Journey to Population Health and Risk
 AMGA Consulting Thought Leadership Series White Paper The Journey to Population Health and Risk The Journey to Population Health and Risk Howard B. Graman, M.D., FACP White Paper, January 2016 While the
AMGA Consulting Thought Leadership Series White Paper The Journey to Population Health and Risk The Journey to Population Health and Risk Howard B. Graman, M.D., FACP White Paper, January 2016 While the
Low-Cost, Low-Administrative Burden Ways to Better Integrate Care for Medicare-Medicaid Enrollees
 TECHNICAL ASSISTANCE BRIEF J UNE 2 0 1 2 Low-Cost, Low-Administrative Burden Ways to Better Integrate Care for Medicare-Medicaid Enrollees I ndividuals eligible for both Medicare and Medicaid (Medicare-Medicaid
TECHNICAL ASSISTANCE BRIEF J UNE 2 0 1 2 Low-Cost, Low-Administrative Burden Ways to Better Integrate Care for Medicare-Medicaid Enrollees I ndividuals eligible for both Medicare and Medicaid (Medicare-Medicaid
ACOs the Medicare Shared Savings Program And Other Healthcare Reform Payment Methods
 A unique vision for an ever-changing healthcare environment ACOs the Medicare Shared Savings Program And Other Healthcare Reform Payment Methods Presented by Joe Laden, President, ORVA, LLC The Environment
A unique vision for an ever-changing healthcare environment ACOs the Medicare Shared Savings Program And Other Healthcare Reform Payment Methods Presented by Joe Laden, President, ORVA, LLC The Environment
Background and Context:
 Session Objectives: Practice Transformation: Preparing for a Value Based Purchasing Environment Susan Brown, MPH, CPHIMS May 2, 2016 Understand the timeline and impact of MACRA/MIPS on health care payment
Session Objectives: Practice Transformation: Preparing for a Value Based Purchasing Environment Susan Brown, MPH, CPHIMS May 2, 2016 Understand the timeline and impact of MACRA/MIPS on health care payment
STATEMENT. of the. American Medical Association. for the Record. United States Senate Committee on Veterans Affairs.
 STATEMENT of the American Medical Association for the Record United States Senate Committee on Veterans Affairs Re: Pending Legislation: Improving the Veterans Choice Program S. 2646, Veterans Choice Improvement
STATEMENT of the American Medical Association for the Record United States Senate Committee on Veterans Affairs Re: Pending Legislation: Improving the Veterans Choice Program S. 2646, Veterans Choice Improvement
Seeing the Value and Transparency of Medicare Part B: Four Case Studies of Medicare Successes
 Seeing the Value and Transparency of Medicare Part B: Four Case Studies of Medicare Successes As the largest payer of healthcare services in the United States, the Centers for Medicare & Medicaid Services
Seeing the Value and Transparency of Medicare Part B: Four Case Studies of Medicare Successes As the largest payer of healthcare services in the United States, the Centers for Medicare & Medicaid Services
ACADEMIC GROUP PRACTICE AND THE LEADERSHIP OF APRN S
 ACADEMIC GROUP PRACTICE AND THE LEADERSHIP OF APRN S Margaret Head, Chief Operating Officer/Chief Nursing Officer Susan Moseley Gent, Administrative Director Vanderbilt Medical Group March 10, 2012 With
ACADEMIC GROUP PRACTICE AND THE LEADERSHIP OF APRN S Margaret Head, Chief Operating Officer/Chief Nursing Officer Susan Moseley Gent, Administrative Director Vanderbilt Medical Group March 10, 2012 With
MAKING PROGRESS, SEEING RESULTS
 MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
MAKING PROGRESS, SEEING RESULTS VALUE-BASED CARE REPORT HUMANA.COM/VALUEBASEDCARE Y0040_GCHK4DYEN 1117 Accepted 2 Americans are sick and getting sicker, with millions of us living with chronic conditions
Swapping, Kickbacks, Fair Market Value: Risks for a Post-Acute Provider
 Swapping, Kickbacks, Fair Market Value: Risks for a Post-Acute Provider Alan Schabes, Partner Benesch, Friedlander, Coplan & Aronoff LLP Shannon Drake, VP, Associate General Counsel Kindred at Home Amanda
Swapping, Kickbacks, Fair Market Value: Risks for a Post-Acute Provider Alan Schabes, Partner Benesch, Friedlander, Coplan & Aronoff LLP Shannon Drake, VP, Associate General Counsel Kindred at Home Amanda
CIGNA Collaborative Accountable Care
 CIGNA Collaborative Accountable Care Connecting in ways that help make achieving health easier, more effective and more affordable October 14, 2016 Michael L. Howell, MD, MBA, FACP Market Medical Executive/Sr.
CIGNA Collaborative Accountable Care Connecting in ways that help make achieving health easier, more effective and more affordable October 14, 2016 Michael L. Howell, MD, MBA, FACP Market Medical Executive/Sr.
Arkansas Center for Nursing Arkansas Nurse Practitioner Association Arkansas Nurses Association Arkansas Pediatric Nurse Practitioners
 Remove the Mandatory Collaborative Practice Agreement on APRN prescribing HB 1181 Rep. Dan Sullivan HB 1186 Rep. Karilyn Brown Advanced Practice Registered Nurses (APRNs) are nurses with advanced education
Remove the Mandatory Collaborative Practice Agreement on APRN prescribing HB 1181 Rep. Dan Sullivan HB 1186 Rep. Karilyn Brown Advanced Practice Registered Nurses (APRNs) are nurses with advanced education
Summary and Analysis of CMS Proposed and Final Rules versus AAOS Comments: Comprehensive Care for Joint Replacement Model (CJR)
 Summary and Analysis of CMS Proposed and Final Rules versus AAOS Comments: Comprehensive Care for Joint Replacement Model (CJR) The table below summarizes the specific provisions noted in the Medicare
Summary and Analysis of CMS Proposed and Final Rules versus AAOS Comments: Comprehensive Care for Joint Replacement Model (CJR) The table below summarizes the specific provisions noted in the Medicare
New York s 1115 Waiver Programs Downstate Public Comment and PAOP Working Session. Comments of Christy Parque, MSW.
 New York s 1115 Waiver Programs Downstate Public Comment and PAOP Working Session Comments of Christy Parque, MSW President and CEO November 29, 2017 The Coalition for Behavioral Health, Inc. (The Coalition)
New York s 1115 Waiver Programs Downstate Public Comment and PAOP Working Session Comments of Christy Parque, MSW President and CEO November 29, 2017 The Coalition for Behavioral Health, Inc. (The Coalition)
Re: Request for Information by the Centers for Medicare and Medicaid Services Innovation Center
 November 20, 2017 Seema Verma Administrator, Centers for Medicare and Medicaid Services Department of Health and Human Services Room 445 G, Hubert H. Humphrey Building, 200 Independence Avenue, SW Washington,
November 20, 2017 Seema Verma Administrator, Centers for Medicare and Medicaid Services Department of Health and Human Services Room 445 G, Hubert H. Humphrey Building, 200 Independence Avenue, SW Washington,
Policy Considerations for Community Health Workers in an Era of Health Reform
 University of Southern Maine USM Digital Commons Muskie School Capstones Student Scholarship 5-2015 Policy Considerations for Community Health Workers in an Era of Health Reform Sara Kahn-Troster University
University of Southern Maine USM Digital Commons Muskie School Capstones Student Scholarship 5-2015 Policy Considerations for Community Health Workers in an Era of Health Reform Sara Kahn-Troster University
Value-Based Reimbursements are Here: Are you Ready?
 Value-Based Reimbursements are Here: Are you Ready? White Paper ELLIS MAC KNIGHT, MD Senior Vice President/CMO Published by Becker s Hospital Review April 2016 White Paper Value-Based Reimbursements are
Value-Based Reimbursements are Here: Are you Ready? White Paper ELLIS MAC KNIGHT, MD Senior Vice President/CMO Published by Becker s Hospital Review April 2016 White Paper Value-Based Reimbursements are
Osteopathic Advocacy: Partnering to Advance Sound Health Policy. Nicholas Schilligo, MS Associate Vice President, State Government Affairs
 Osteopathic Advocacy: Partnering to Advance Sound Health Policy Nicholas Schilligo, MS Associate Vice President, State Government Affairs Our Work Work with a variety of stakeholders to promote AOA policies
Osteopathic Advocacy: Partnering to Advance Sound Health Policy Nicholas Schilligo, MS Associate Vice President, State Government Affairs Our Work Work with a variety of stakeholders to promote AOA policies
Thank CMS for New Process for Evaluation of CPT Codes and Support Proposed Change to Eliminate the Use of Refinement Panels
 September 8, 2015 Submitted via www.regulations.gov Andrew M. Slavitt Acting Administrator Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1631-P P.O. Box 8013
September 8, 2015 Submitted via www.regulations.gov Andrew M. Slavitt Acting Administrator Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1631-P P.O. Box 8013
Health System Transformation, CMS Priorities, and the Medicare Access and CHIP Reauthorization Act
 Health System Transformation, CMS Priorities, and the Medicare Access and CHIP Reauthorization Act Ashby Wolfe, MD, MPP, MPH Chief Medical Officer, Region IX Centers for Medicare and Medicaid Services
Health System Transformation, CMS Priorities, and the Medicare Access and CHIP Reauthorization Act Ashby Wolfe, MD, MPP, MPH Chief Medical Officer, Region IX Centers for Medicare and Medicaid Services
Payment and Delivery System Reform in Vermont: 2016 and Beyond
 Payment and Delivery System Reform in Vermont: 2016 and Beyond Richard Slusky, Director of Reform Green Mountain Care Board Presentation to GMCB August 13, 2015 Transition Year 2016 1. Medicare Waiver
Payment and Delivery System Reform in Vermont: 2016 and Beyond Richard Slusky, Director of Reform Green Mountain Care Board Presentation to GMCB August 13, 2015 Transition Year 2016 1. Medicare Waiver
States of Change: Expanding the Health Care Workforce and Creating Community-Clinical Partnerships
 States of Change: Expanding the Health Care Workforce and Creating Community-Clinical Partnerships Thursday, November 7, 2013 12:00 1:30 pm ET Sponsored by Merck Foundation www.alliancefordiabetes.org
States of Change: Expanding the Health Care Workforce and Creating Community-Clinical Partnerships Thursday, November 7, 2013 12:00 1:30 pm ET Sponsored by Merck Foundation www.alliancefordiabetes.org
Advanced Practice Registered Nurses (APRNs)
 - 4 - Advanced Practice Registered Nurses (APRNs) - 5 - Advanced Practice Registered Nurses (APRNs) APRNs are registered nurses who have at a minimum completed graduate coursework (masters degree), passed
- 4 - Advanced Practice Registered Nurses (APRNs) - 5 - Advanced Practice Registered Nurses (APRNs) APRNs are registered nurses who have at a minimum completed graduate coursework (masters degree), passed
Aligning Executive, Physician and Staff Compensation with Population Health Goals
 Aligning Executive, Physician and Staff Compensation with Population Health Goals WILLIAM F. JESSEE, MD, FACMPE Becker s Hospital Review 8th Annual Meeting Chicago, IL April 17, 2017 0 Welcome Today s
Aligning Executive, Physician and Staff Compensation with Population Health Goals WILLIAM F. JESSEE, MD, FACMPE Becker s Hospital Review 8th Annual Meeting Chicago, IL April 17, 2017 0 Welcome Today s
MassHealth Restructuring Overview
 1 MassHealth Restructuring Overview State of the State, Assuring Access, Equity and Integrated Care Massachusetts League of Community Health Centers Marylou Sudders, Secretary Executive Office of Health
1 MassHealth Restructuring Overview State of the State, Assuring Access, Equity and Integrated Care Massachusetts League of Community Health Centers Marylou Sudders, Secretary Executive Office of Health
3/16/2016. Swapping, Kickbacks, Fair Market Value: Risks for a Post-Acute Provider. AKS designed to prevent improper referrals, which can lead to:
 Swapping, Kickbacks, Fair Market Value: Risks for a Post-Acute Provider Alan Schabes, Partner Benesch, Friedlander, Coplan & Aronoff LLP Shannon Drake, VP, Associate General Counsel Kindred at Home Amanda
Swapping, Kickbacks, Fair Market Value: Risks for a Post-Acute Provider Alan Schabes, Partner Benesch, Friedlander, Coplan & Aronoff LLP Shannon Drake, VP, Associate General Counsel Kindred at Home Amanda
Health Reform and IRFs
 American Medical Rehabilitation Providers Association 8 th Annual AMRPA Educational Conference New Orleans, LA Health Reform and IRFs Planning Today for Success Tomorrow October 14, 2010 Agenda Introduce
American Medical Rehabilitation Providers Association 8 th Annual AMRPA Educational Conference New Orleans, LA Health Reform and IRFs Planning Today for Success Tomorrow October 14, 2010 Agenda Introduce
State Policy Report #47. October Health Center Payment Reform: State Initiatives to Meet the Triple Aim. Introduction
 Health Center Payment Reform: State Initiatives to Meet the Triple Aim State Policy Report #47 October 2013 Introduction Policymakers at both the federal and state levels are focusing on how best to structure
Health Center Payment Reform: State Initiatives to Meet the Triple Aim State Policy Report #47 October 2013 Introduction Policymakers at both the federal and state levels are focusing on how best to structure
Adopting a Care Coordination Strategy
 Adopting a Care Coordination Strategy Authors: Henna Zaidi, Manager, and Catherine Castillo, Senior Consultant Current state of health care The traditional approach to health care delivery is quickly becoming
Adopting a Care Coordination Strategy Authors: Henna Zaidi, Manager, and Catherine Castillo, Senior Consultant Current state of health care The traditional approach to health care delivery is quickly becoming
Health Care Reform Provisions Affecting Older Adults and Persons with Special Needs 3/30/10
 Health Care Reform Provisions Affecting Older Adults and Persons with Special Needs 3/30/10 On March 23, 2010, President Obama signed a comprehensive health care reform bill (H.R. 3590) into law. On March
Health Care Reform Provisions Affecting Older Adults and Persons with Special Needs 3/30/10 On March 23, 2010, President Obama signed a comprehensive health care reform bill (H.R. 3590) into law. On March
Accountable Care Organizations. What the Nurse Executive Needs to Know. Rebecca F. Cady, Esq., RNC, BSN, JD, CPHRM
 JONA S Healthcare Law, Ethics, and Regulation / Volume 13, Number 2 / Copyright B 2011 Wolters Kluwer Health Lippincott Williams & Wilkins Accountable Care Organizations What the Nurse Executive Needs
JONA S Healthcare Law, Ethics, and Regulation / Volume 13, Number 2 / Copyright B 2011 Wolters Kluwer Health Lippincott Williams & Wilkins Accountable Care Organizations What the Nurse Executive Needs
Physician Compensation in an Era of New Reimbursement Models
 2014 IHA Annual Membership Meeting Physician Compensation in an Era of New Reimbursement Models Taryn E. Stone Ice Miller LLP (317) 236-5872 taryn.stone@ Agenda Background New Reimbursement Models Trends
2014 IHA Annual Membership Meeting Physician Compensation in an Era of New Reimbursement Models Taryn E. Stone Ice Miller LLP (317) 236-5872 taryn.stone@ Agenda Background New Reimbursement Models Trends
Seema Verma Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1696-P P.O. Box 8016 Baltimore, MD
 June 26, 2018 Seema Verma Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1696-P P.O. Box 8016 Baltimore, MD 21244-1850 Re: CMS-1696-P Medicare Program; Prospective
June 26, 2018 Seema Verma Centers for Medicare & Medicaid Services Department of Health and Human Services Attn: CMS-1696-P P.O. Box 8016 Baltimore, MD 21244-1850 Re: CMS-1696-P Medicare Program; Prospective
Re: CMS Patient Relationship Categories and Codes Second Request for Information
 January 6, 2017 Andrew Slavitt Acting Administrator Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: CMS Patient Relationship Categories and Codes Second Request
January 6, 2017 Andrew Slavitt Acting Administrator Centers for Medicare & Medicaid Services 7500 Security Boulevard Baltimore, MD 21244 Re: CMS Patient Relationship Categories and Codes Second Request
Reimbursement Models of the Future A Look at Proposed Models
 Experience the Eide Bailly Difference Reimbursement Models of the Future A Look at Proposed Models Ralph J. Llewellyn, CPA, CHFP Partner rllewellyn@eidebailly.com 701.239.8594 Introduction CAH reimbursement
Experience the Eide Bailly Difference Reimbursement Models of the Future A Look at Proposed Models Ralph J. Llewellyn, CPA, CHFP Partner rllewellyn@eidebailly.com 701.239.8594 Introduction CAH reimbursement
VALUE-BASED CARE REPORT
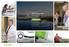 VALUE-BASED CARE REPORT PREVENTION & OUTCOMES. Patients treated by physicians in Humana Medicare Advantage (MA) value-based agreements had more preventive care screenings and better health outcomes compared
VALUE-BASED CARE REPORT PREVENTION & OUTCOMES. Patients treated by physicians in Humana Medicare Advantage (MA) value-based agreements had more preventive care screenings and better health outcomes compared
REDESIGNING HEALTH CARE FROM THE BOTTOM UP INSTEAD OF FROM THE TOP DOWN
 REDESIGNING HEALTH CARE FROM THE BOTTOM UP INSTEAD OF FROM THE TOP DOWN Supporting Collaborative Regional Approaches to Sustainable High-Value Healthcare Harold D. Miller President and CEO Center for Healthcare
REDESIGNING HEALTH CARE FROM THE BOTTOM UP INSTEAD OF FROM THE TOP DOWN Supporting Collaborative Regional Approaches to Sustainable High-Value Healthcare Harold D. Miller President and CEO Center for Healthcare
I. LIVE INTERACTIVE TELEDERMATOLOGY
 Position Statement on Teledermatology (Approved by the Board of Directors: February 22, 2002; Amended by the Board of Directors: May 22, 2004; November 9, 2013; August 9, 2014; May 16, 2015; March 7, 2016)
Position Statement on Teledermatology (Approved by the Board of Directors: February 22, 2002; Amended by the Board of Directors: May 22, 2004; November 9, 2013; August 9, 2014; May 16, 2015; March 7, 2016)
ESSENTIAL STRATEGIES IN MEDI-CAL PAYMENT REFORM. Richard Popper, Director, Medicaid & Duals Strategy August 3, 2017
 ESSENTIAL STRATEGIES IN MEDI-CAL PAYMENT REFORM Richard Popper, Director, Medicaid & Duals Strategy August 3, 2017 1 DISCLAIMER The enclosed materials are highly sensitive, proprietary and confidential.
ESSENTIAL STRATEGIES IN MEDI-CAL PAYMENT REFORM Richard Popper, Director, Medicaid & Duals Strategy August 3, 2017 1 DISCLAIMER The enclosed materials are highly sensitive, proprietary and confidential.
Defunding the Affordable Care Act: Discretionary Programs to Target in the Healthcare Reform Law Schalla Ross l November 2010
 Defunding the Affordable Care Act: Discretionary Programs to Target in the Healthcare Reform Law Schalla Ross l November 2010 Introduction During the 2010 midterm elections Republican Congressional Candidates
Defunding the Affordable Care Act: Discretionary Programs to Target in the Healthcare Reform Law Schalla Ross l November 2010 Introduction During the 2010 midterm elections Republican Congressional Candidates
Optimal Team Practice
 Optimal Team Practice Updates to AAPA s Guidelines for State Regulation of PAs Montana Academy of PAs 2018 Annual Conference June 6, 2018 Ann Davis, MS, PA-C VP, Constituent Organization Outreach and Advocacy,
Optimal Team Practice Updates to AAPA s Guidelines for State Regulation of PAs Montana Academy of PAs 2018 Annual Conference June 6, 2018 Ann Davis, MS, PA-C VP, Constituent Organization Outreach and Advocacy,
A pathway to a reformed and expanded MO HealthNet system:
 A pathway to a reformed and expanded MO HealthNet system: Competitive, accountable, and simplified Contents Executive Summary...................... 3 How this report was made 6 Findings from the research...................
A pathway to a reformed and expanded MO HealthNet system: Competitive, accountable, and simplified Contents Executive Summary...................... 3 How this report was made 6 Findings from the research...................
Future of Patient Safety and Healthcare Quality
 Future of Patient Safety and Healthcare Quality Patrick Conway, M.D., MSc CMS Chief Medical Officer Director, Center for Clinical Standards and Quality Acting Director, Center for Medicare and Medicaid
Future of Patient Safety and Healthcare Quality Patrick Conway, M.D., MSc CMS Chief Medical Officer Director, Center for Clinical Standards and Quality Acting Director, Center for Medicare and Medicaid
Policy Analysis. Matching Supply to Demand: Addressing the U.S. Primary Care Workforce Shortage
 Policy Analysis NO. 7 DECEMBER 2011 CONTENT Increasing Primary Care Capacity Other Policy Options Expanding Scope of Practice Payment Policies for Team-Based Care Looking Ahead About the Institute. The
Policy Analysis NO. 7 DECEMBER 2011 CONTENT Increasing Primary Care Capacity Other Policy Options Expanding Scope of Practice Payment Policies for Team-Based Care Looking Ahead About the Institute. The
Pennsylvania Patient and Provider Network (P3N)
 Pennsylvania Patient and Provider Network (P3N) Cross-Boundary Collaboration and Partnerships Commonwealth of Pennsylvania David Grinberg, Deputy Executive Director 717-214-2273 dgrinberg@pa.gov Project
Pennsylvania Patient and Provider Network (P3N) Cross-Boundary Collaboration and Partnerships Commonwealth of Pennsylvania David Grinberg, Deputy Executive Director 717-214-2273 dgrinberg@pa.gov Project
The Patient Protection and Affordable Care Act Summary of Key Health Information Technology Provisions June 1, 2010
 The Patient Protection and Affordable Care Act Summary of Key Health Information Technology Provisions June 1, 2010 This document is a summary of the key health information technology (IT) related provisions
The Patient Protection and Affordable Care Act Summary of Key Health Information Technology Provisions June 1, 2010 This document is a summary of the key health information technology (IT) related provisions
General Information. Overview. Purpose. Table of Contents
 Blue Cross and Blue Shield of Georgia, Inc. and Blue Cross Blue Shield Healthcare Plan of Georgia, Inc.engage Inovalonto conduct outreach efforts for ouraca individual and small group on and off exchange
Blue Cross and Blue Shield of Georgia, Inc. and Blue Cross Blue Shield Healthcare Plan of Georgia, Inc.engage Inovalonto conduct outreach efforts for ouraca individual and small group on and off exchange
Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers
 Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers Beth Waldman, JD, MPH June 14, 2016 Presentation Overview 1. Brief overview of payment reform strategies
Implementing Medicaid Value-Based Purchasing Initiatives with Federally Qualified Health Centers Beth Waldman, JD, MPH June 14, 2016 Presentation Overview 1. Brief overview of payment reform strategies
ACCOUNTABLE CARE ORGANIZATION & ALTERNATIVE PAYMENT MODEL SUMMIT
 ACCOUNTABLE CARE ORGANIZATION & ALTERNATIVE PAYMENT MODEL SUMMIT The Centers for Medicare and Medicaid Services Kate Goodrich, MD MHS Director, Clinical Standards & Quality Chief Medical Officer 1 DISCLAIMERS
ACCOUNTABLE CARE ORGANIZATION & ALTERNATIVE PAYMENT MODEL SUMMIT The Centers for Medicare and Medicaid Services Kate Goodrich, MD MHS Director, Clinical Standards & Quality Chief Medical Officer 1 DISCLAIMERS
Forces of Change- Seeing Stepping Stones Not Potholes
 May 19, 2014 Forces of Change- Seeing Stepping Stones Not Potholes 2 3 4 Overview Demographics Long Term Care Financing Challenges Broad Health System Challenges Payment Reform Delivery System Reform Where
May 19, 2014 Forces of Change- Seeing Stepping Stones Not Potholes 2 3 4 Overview Demographics Long Term Care Financing Challenges Broad Health System Challenges Payment Reform Delivery System Reform Where
The Quality Payment Program Overview Fact Sheet
 Quality Payment Program The Quality Payment Program Overview Background On October 14, 2016, the Department of Health and Human Services (HHS) issued its final rule with comment period implementing the
Quality Payment Program The Quality Payment Program Overview Background On October 14, 2016, the Department of Health and Human Services (HHS) issued its final rule with comment period implementing the
CMS Meaningful Use Incentives NPRM
 CMS Meaningful Use Incentives NPRM Margret Amatayakul MBA, RHIA, CHPS, CPHIT, CPEHR, CPHIE, FHIMSS President, Margret\A Consulting, LLC Faculty and Board of Examiners, Health IT Certification, LLC Notice
CMS Meaningful Use Incentives NPRM Margret Amatayakul MBA, RHIA, CHPS, CPHIT, CPEHR, CPHIE, FHIMSS President, Margret\A Consulting, LLC Faculty and Board of Examiners, Health IT Certification, LLC Notice
