Step 1. Decision and Documentation
|
|
|
- Julia Whitehead
- 5 years ago
- Views:
Transcription
1 Appendix C Removal of Mechanical Ventilation (RMV) Guidelines This guideline has been developed to assist physicians, nurses, respiratory care therapists, social workers, spiritual counselors and other staff in providing a compassionate process for removing mechanical ventilation (RMV) from a dying patient in ICU. This guideline is to be used when death is the expected outcome following RMV. Step 1. Decision and Documentation 1. The prognosis, options and goals of care have been fully explored with the patient/legal surrogates/family; consensus has been reached that RMV with expected death is the optimal treatment course. The Attending Physician must be involved in this discussion. The patient s primary nurse, respiratory therapist, social worker/case manager, chaplain and palliative care team may be included in this discussion unless the family requests otherwise. Related issues to be discussed prior to RMV include: withdrawal of artificial hydration/feeding withdrawal of blood pressure support withdrawal of antibiotics and blood products wishes concerning organ donation-(see Organ & Tissue Donation Policy if applicable) withdrawal of endotracheal tube (ET) tube after ventilator is discontinued Note: there is no compelling ethical or medical rationale for continuing the above treatments once a decision has been made to RMV. 2. The Attending Physician documents in the medical record the date/time of the RMV discussion, who was present and the agreed goals and plan. A Do Not Resuscitate (DNR) order is written. 3. When prolonged survival is expected, the Palliative Care team is notified of the plan for RMV and potential for transfer to non-icu patient room. 4. A time/date is established for RMV. 5. Nursing staff to initiate Nursing Tip Sheet (Appendix C-2) not to be retained as part of the patient s permanent record. Step 2. Preparation for RMV 1. A staff physician (attending physician or Palliative Care physician) will be available before, during and immediately after RMV, to supervise symptom control and provide counseling/support to family and staff. An order is written to discontinue mechanical ventilation. (see Appendix C-1: Discussion points for educating Patients/families about ventilator withdrawal) 2. The primary nurse and physician will provide information to the patient or family attending the RMV process: potential outcomes (rapid vs. delayed death), potential symptoms/signs, process of withdrawal (Ventilator, ET tube, other tubes). 3. Notify Respiratory Therapy of RMV timing; ask therapist to be present. 4. Notify chaplain; ask family/surrogates if they wish chaplain or other clergy present before or during RMV. 5. Pre-medication for analgesia and sedation is indicated. (Note: the primary goal of sedation is to prevent post-extubation dyspnea. Unintentional apnea following sedative administration may occur, but in general, if all parties have agreed upon the plan of care, a decision to continue with ventilator withdrawal is appropriate. Reversing agents (e.g. Naloxone) should not be administered.) [See Medication section of Appendix C-3: Removal of Mechanical Ventilation (Comfort Care/ICU)]
2 6. Discontinue paralytics and test for return of neuromuscular function. 7. If previously agreed to, discontinue blood pressure support medication, artificial hydration/nutrition, antibiotics, and dialysis. Remove OG/NG tubes. 8. Remove restraints and unnecessary medical paraphernalia. 9. Discontinue vital signs, labs, x-rays, and pulse oximetry. Step 3. Removal of Mechanical Ventilation 1. Ensure adequate sedation and analgesia. 2. Prepare space at the bedside for family members. 3. A nurse or respiratory therapist should be stationed at the opposite side of the bed with a washcloth and oral suction catheter. 4. Follow Ventilator Management section of Appendix C-3: Removal of Mechanical Ventilation (Comfort Care/ICU) 5. A clean towel should be placed over the ET tube to collect any secretions. If excessive secretions are observed, suction them away. 6. Nursing to have extra tissues available for extra secretions, if needed, and for family use. Family should be encouraged to hold the patient s hand and provide assurances to their loved one. 7. Observe for signs of respiratory distress; adjust medication if indicated. Step 4. Actions following RMV 1. Document in the medical record the procedure, medications and immediate outcome of the process of RMV. 2. Continually monitor for adequate sedation and comfort. 3. Have additional support (Palliative Care, Spiritual care, etc) available to family. 4. Transfer to a non-icu bed if patient status remains stable (for example, after 2 hours). 5. Offer family the option of Complementary Therapies or Caring Presence assistance if desired. References: Campbell, M. (2010) Mechanical Ventilation. (Nelson, P.) Withdrawal of Life-Sustaining Therapies (pp ) Pittsburgh, PA, Hospice and Palliative Nurses Association Principles and practice of withdrawing life-sustaining treatment in the ICU. Rubenfeld GD and Crawford SW, in Managing death in the Intensive Care Unit. Curtis JR and Rubenfeld GD (eds) Oxford University Press, 2001 pgs: Krieger BP. Compassionate extubation: Withdrawing mechanical ventilator support. Mediguide to pulmonary medicine. 2001; 8:1-5. Von Gunten, C & Weissman, D. (2005) #33 Ventilator Withdrawal protocol 2 nd edition. Retrieved July 2011 from Von Gunten, C & Weissman, D. (2005) #35 Information for Patients and Families about Ventilator Withdrawal 2 nd edition. Retrieved July 2011 from Von Gunten, C & Weissman, D. (2005) #34 Symptom Control for Ventilator Withdrawal in the Dying Patient 2 nd edition. Retrieved July 2011 from
3 Appendix C-1 Discussion points for Staff in educating Patients and families about ventilator withdrawal Removal of mechanical ventilation is a medical decision made by the physician. The role of the family is to ensure the physician understands the patient s wishes. Family support is a critical aspect of care for the dying patient who is to be removed from a ventilator. Before withdrawal, the following issues should be discussed. Potential outcome of ventilator withdrawal When all other life-sustaining treatments have been stopped, including artificial hydration and nutrition, there are several possible outcomes: rapid death within minutes (typically patients with sepsis on maximal blood pressure support), death within hours to days, or stable cardiopulmonary function leading to a different set of care plans, including potential hospital discharge. If the latter possibility is realistic, future management plans should be discussed prior to ventilator removal, since some families may desire to resume certain treatments, notably artificial hydration/nutrition. Generally, by the nature of the underlying illness and the established goals, it is fairly easy to predict which category will be operative, but all families should be prepared for some degree of prognostic uncertainty. The procedure of ventilator withdrawal Explain to family, clergy and others how they can best support their loved one at the bedside before, during and after withdrawal. Encourage family to make arrangements for special music or rituals or support during and following the procedure. If asked, provide examples and model comfort measures such as showing love and support through touch, wiping of the patient s forehead, holding a hand and talking to him or her. Never make assumptions about what the family understands. Describe the procedure in clear, simple terms and answer any questions. Families should be told before-hand the steps of withdrawal and whether or not it is planned/desired to remove the endotracheal tube. In addition, they should be counseled about the use of oxygen and medications for symptom control. Tell families that sedative medication may lead to decreased breathing, but this does not represent euthanasia or assisted suicide. Assure them that the patient s comfort is of primary concern. Explain that breathlessness may occur, but that it can be effectively managed with medication. Confirm that you will have medication available to manage any discomfort. Ensure they know that the patient will likely need to be kept asleep to control their symptoms and that involuntary moving or gasping does not reflect suffering if the patient is properly sedated or in a coma. Support the decision When a family is able to make a definite decision for ventilator withdrawal, such a decision is always emotionally charged. Families will constantly second-guess themselves, especially if there is a prolonged dying process following ventilator withdrawal. Support, guidance and leadership from the entire medical team is crucial, as the family will be looking to the team to ensure them that they are doing the right thing. Furthermore, it is common for families to have concerns that their decision constitutes euthanasia or assisted suicide explicit support, education and explanations from the team will be needed.
4 Appendix C-2 Progress Notes NURSING TIP SHEET (Not a part of the Patients permanent record) REMOVAL OF MECHANICAL VENTILATION (COMFORT CARE/ICU) Chart documentation: goal of care and plan; Date/time for RMV is established Decisions established re: hydration/feeding/pressors/antibiotics/et tube Orders DNR order Referral call to Donor Referral Line Order to discontinue ventilator RMV order form completed and faxed to Pharmacy Comfort Cart from Dietary (if requested) Staff Respiratory therapy Case Management Palliative Care (if consulted) Spiritual Care notified (if requested) Complementary Therapies (if requested) Staff physician is available for RMV (Attending, Palliative Care or Critical Care) Families Information provided to families ( By ICU staff Palliative Care Other) Encourage family to make arrangements for special music, rituals or support during and following the procedure. Bereavement kits: Offer to make clay hand prints, and clip keepsake locks of hair for family/loved ones. Condolence cards available for staff to send to families after patient expires. Procedural steps Pre-medications and palliative medications at bedside for pain, dyspnea, sedation Ventilator alarms and other monitors silenced Wash cloth and oral suction equipment ready Tissues available in room for family and/or staff T-piece and/or aerosol delivery devices available at bedside if indicated Oxygen therapy devices available at bedside if indicated Restraints removed Side rails down when appropriate
5 Appendix C-3 REMOVAL OF MECHANICAL VENTILATION (COMFORT CARE/ICU) Preparations: Do Not Resuscitate (DNR) order written Verify that patient has been evaluated for organ donation before withdrawal Chart documentation of rationale for withdrawal of life-sustaining treatments, discussions with physicians and family/legal surrogates (or attempts to contact) Verify adequate IV access (consult physician if access is insufficient) Notify Respiratory Therapy, Case Management, Palliative Care, Spiritual Care & Complementary Therapy (if consulted) of the planned time of withdrawal Remove gastric contents by suctioning gastric tube until no return of material Remove devices not necessary for comfort including monitors, blood pressure cuffs, leg compression devices. Remove all unnecessary restraints, lines, and equipment from room. Liberalize visitation and determine which family members desire to be present for withdrawal Provide family members with items to assist their comfort (tissues, chairs, comfort cart, etc) Position patient to facilitate hand holding with family. Evaluate and ensure symptom control is present; o Consult with family about their perception of patient comfort Keep head of bed elevated 30 degrees Reposition patient PRN comfort. Medications: Discontinue all paralytic orders. Discontinue all previous medication orders unless ordered below. Goals of medication therapy: o Respiratory rate less than 28 o No labored breathing o No signs of pain or discomfort ESTABLISH ANALGESIA AND SEDATION ANALGESIA: (CHOOSE ONE) Morphine Hydromorphone Bolus mg IV prior to extubation AND begin continuous infusion at mg/hour; If signs of discomfort; may increase infusion rate up to 50% every 30 minutes Give additional boluses up to 50% of current infusion rate every 5 minutes if discomfort persists Fentanyl Bolus mcg IV prior to extubation AND begin continuous infusion at mcg/hour; If signs of discomfort; may increase infusion rate up to 50% every 30 minutes Give additional boluses up to 50% of current infusion rate every 5 minutes if discomfort persists DATE: TIME: SIGNATURE: MD/DO/ DATE: TIME: SIGNATURE: RN REMOVAL OF MECHANICAL VENTILATION (COMFORT CARE/ICU) Page 1 of 2. FORM ###### Rev 01, ##/2013 (barcoding strip here) Please Attach Patient Sticker Here
6 Page 2. REMOVAL OF MECHANICAL VENTILATION (COMFORT CARE/ICU) SEDATION: (CHOOSE ONE) Lorazepam Midazolam Bolus mg IV prior to extubation AND begin continuous infusion at mg/hour; May increase infusion rate up to 50% every 30 minutes PRN anxiety or agitation OR Bolus mg IV prior to extubation AND every minutes PRN anxiety or agitation Other VENTILATOR MANAGEMENT: Once patient is adequately sedated and comfortable, proceed with following: Weaning protocol: 1. Silence all ventilator alarms. 2. Set FiO2 to 21% and PEEP to zero over approximately 5 minutes. Observe for signs of respiratory distress; titrate medication for sedation and comfort. 3. Wean IMV to 4 and/or pressure support to 5 over 5-15 minutes; Observe for signs of respiratory distress and adjust medications to optimize patient comfort. 4. When patient is comfortable on IMV of 4 and/or pressure support of 5, THEN (choose one): Extubate patient to air, suction if necessary. Extubate to cannula at L/min; titrate to comfort T-piece with air (not CPAP on ventilator) 5. Move ventilator away from bedside. Extubate without weaning. DATE: TIME: SIGNATURE: MD/DO/ DATE: TIME: SIGNATURE: RN REMOVAL OF MECHANICAL VENTILATION (COMFORT CARE/ICU) Page 2 of 2. FORM ###### Rev 01, ##/2013 (barcoding strip here) Please Attach Patient Sticker Here
End of Life Care in the ICU
 End of Life Care in the ICU C.M. Stafford, MD, FCCP Medical Director, Intensive Care Unit Chairman, Healthcare Ethics Committee Naval Medical Center San Diego The views expressed in this presentation are
End of Life Care in the ICU C.M. Stafford, MD, FCCP Medical Director, Intensive Care Unit Chairman, Healthcare Ethics Committee Naval Medical Center San Diego The views expressed in this presentation are
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth
 Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Individualised End of Life Care Plan for the Last Days or Hours of Life Patient name Hospital number Date of birth NHS number Informed by Five Priorities for Care: Recognise, Communicate, Involve, Support,
Policies and Procedures. ID Number: 1138
 Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
Policies and Procedures Title: VENTILATION Acute-Care of Mechanically Ventilated Patient - Adult RN Specialty Practice: RN Clinical Protocol: Advanced RN Intervention ID Number: 1138 Authorization: [X]
YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE
 YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE Communicating Your Health Care Choices In 1990, Congress passed the Patient Self-Determination Introduction Act. It requires
YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE YOUR RIGHT TO DECIDE Communicating Your Health Care Choices In 1990, Congress passed the Patient Self-Determination Introduction Act. It requires
Moral Conversations with ICU Patients and Families
 Moral Conversations with ICU Patients and Families Barb Supanich,RSM, MD,FAAHPM Medical Director, Palliative Care and Senior Services Holy Cross Hospital March 11, 2010 Learner Objectives Describe three
Moral Conversations with ICU Patients and Families Barb Supanich,RSM, MD,FAAHPM Medical Director, Palliative Care and Senior Services Holy Cross Hospital March 11, 2010 Learner Objectives Describe three
Family/Caregiver Education Checklist Return Demonstration of Knowledge FIRST 24 HOURS
 of Knowledge FIRST 24 HOURS The following checklists will be completed by a PDN RN or LPN to ensure family/caregiver s skill level is adequate to safely take care of their child independently Teaching
of Knowledge FIRST 24 HOURS The following checklists will be completed by a PDN RN or LPN to ensure family/caregiver s skill level is adequate to safely take care of their child independently Teaching
Liverpool Care Pathway for the Dying Patient (LCP) supporting care in the last hours or days of life
 Liverpool Care Pathway for the Dying Patient (LCP) supporting care in the last hours or days of life Information sheet to be given to the relative or carer following a discussion regarding the plan of
Liverpool Care Pathway for the Dying Patient (LCP) supporting care in the last hours or days of life Information sheet to be given to the relative or carer following a discussion regarding the plan of
DIRECTIVE TO PHYSICIANS AND FAMILY OR SURROGATES Advance Directives Act (see , Health and Safety Code) DIRECTIVE
 DIRECTIVE TO PHYSICIANS AND FAMILY OR SURROGATES Advance Directives Act (see 166.033, Health and Safety Code) Instructions for completing this document: This is an important legal document known as an
DIRECTIVE TO PHYSICIANS AND FAMILY OR SURROGATES Advance Directives Act (see 166.033, Health and Safety Code) Instructions for completing this document: This is an important legal document known as an
When Your Loved One is Dying at Home
 When Your Loved One is Dying at Home What can I expect? What can I do? Although it is impossible to totally prepare for a death it may be easier if you know what to expect. Hospice Palliative Care aims
When Your Loved One is Dying at Home What can I expect? What can I do? Although it is impossible to totally prepare for a death it may be easier if you know what to expect. Hospice Palliative Care aims
TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee
 TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee Advance Directives Living Wills Power of Attorney The Values History: A Worksheet for Advanced Directives
TheValues History: A Worksheet for Advance Directives Courtesy of Somerset Hospital s Ethics Committee Advance Directives Living Wills Power of Attorney The Values History: A Worksheet for Advanced Directives
Your Results for: "NCLEX Review"
 Your Results for: "NCLEX Review" Site Title: Medical-Surgical Nursing Book Title: Medical-Surgical Nursing Location on Site: PART 1: MEDICAL-SURGICAL NURSING PRACTICE > Chapter 5: Nursing Care of Clients
Your Results for: "NCLEX Review" Site Title: Medical-Surgical Nursing Book Title: Medical-Surgical Nursing Location on Site: PART 1: MEDICAL-SURGICAL NURSING PRACTICE > Chapter 5: Nursing Care of Clients
ADVANCE DIRECTIVE INFORMATION
 ADVANCE DIRECTIVE INFORMATION NOTE: This Advance Directive Information and the form Living Will and Durable Power of Attorney for Health Care on the Arkansas Bar Association s website are being provided
ADVANCE DIRECTIVE INFORMATION NOTE: This Advance Directive Information and the form Living Will and Durable Power of Attorney for Health Care on the Arkansas Bar Association s website are being provided
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care
 Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
Royal Liverpool Children s NHS Trust Alder Hey Rapid Discharge Pathway for End of Life Care Pathway for patients where a consensus decision has been made by the child s / young person s family & multi-professional
HealthStream Regulatory Script
 HealthStream Regulatory Script Advance Directives Version: [May 2006] Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney Lesson 5: Other Advance
HealthStream Regulatory Script Advance Directives Version: [May 2006] Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney Lesson 5: Other Advance
Facing Serious Illness: Make Your Wishes Known to your Health Care Professional
 Facing Serious Illness: Make Your Wishes Known to your Health Care Professional Your Guide to the Oregon POLST Program Physician Orders for Life-Sustaining Treatment Revised: February 19, 2015 This material
Facing Serious Illness: Make Your Wishes Known to your Health Care Professional Your Guide to the Oregon POLST Program Physician Orders for Life-Sustaining Treatment Revised: February 19, 2015 This material
Directive To Physicians and Family Or Surrogates (Living Will)
 Directive To Physicians and Family Or Surrogates (Living Will) INSTRUCTIONS FOR COMPLETING THIS DOCUMENT: This is an important legal document known as an Advance Directive. It is designed to help you communicate
Directive To Physicians and Family Or Surrogates (Living Will) INSTRUCTIONS FOR COMPLETING THIS DOCUMENT: This is an important legal document known as an Advance Directive. It is designed to help you communicate
DURABLE POWER OF ATTORNEY FOR HEALTH CARE (Rhode Island Version) You must be at least eighteen (18) years of age.
 MASSASOIT INTERNAL MEDICINE (401) 434-2704 massasoitmed.com DURABLE POWER OF ATTORNEY FOR HEALTH CARE (Rhode Island Version) THE DURABLE POWER OF ATTORNEY FOR HEALTH CARE DOCUMENT lets you appoint someone
MASSASOIT INTERNAL MEDICINE (401) 434-2704 massasoitmed.com DURABLE POWER OF ATTORNEY FOR HEALTH CARE (Rhode Island Version) THE DURABLE POWER OF ATTORNEY FOR HEALTH CARE DOCUMENT lets you appoint someone
Measuring the Quality of Palliative Care in the Intensive Care Unit. Mitchell Levy MD, J. Randall Curtis MD, MPH, John Luce MD, Judith Nelson JD, MD
 ICU Palliative Care Quality Assessment Tool Attending/Housestaff Survey Measuring the Quality of Palliative Care in the Intensive Care Unit Mitchell Levy MD, J. Randall Curtis MD, MPH, John Luce MD, Judith
ICU Palliative Care Quality Assessment Tool Attending/Housestaff Survey Measuring the Quality of Palliative Care in the Intensive Care Unit Mitchell Levy MD, J. Randall Curtis MD, MPH, John Luce MD, Judith
Policies and Procedures. I.D. Number: 1145
 Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Policies and Procedures Title: VENTILATION CHRONIC- CARE OF MECHANICALLY VENTILATED ADULT PERSON RNSP: RN Clinical Protocol: Advanced RN Intervention LPN Additional Competency: Care of Chronically Mechanically
Goals & Objectives 4/17/2014 UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN. Why would someone need to do this?
 UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN Goals & Objectives Participants will increase their knowledge about AHCD Review AHCD documents used at the hospital Role
UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES (AHCD) By Maureen Kroning, EdD, RN Goals & Objectives Participants will increase their knowledge about AHCD Review AHCD documents used at the hospital Role
LOUISIANA ADVANCE DIRECTIVES
 LOUISIANA ADVANCE DIRECTIVES Legal Documents that Ensure that Your Choices for Future Medical Care or the Refusal of Same are Honored and Implemented by Your Health Care Providers Peoples Health is a Medicare
LOUISIANA ADVANCE DIRECTIVES Legal Documents that Ensure that Your Choices for Future Medical Care or the Refusal of Same are Honored and Implemented by Your Health Care Providers Peoples Health is a Medicare
MY CHOICES. Information on: Advance Care Directive Living Will POLST Orders
 MY CHOICES Information on: Advance Care Directive Living Will POLST Orders My Choices Adults have the right to accept or refuse medical care. As long as you can make health care decisions for yourself,
MY CHOICES Information on: Advance Care Directive Living Will POLST Orders My Choices Adults have the right to accept or refuse medical care. As long as you can make health care decisions for yourself,
483.10(b)(4) and (8) Rights Regarding Advance Directives, Treatment, and Experimental Research
 483.10(b)(4) and (8) Rights Regarding Advance Directives, Treatment, and Experimental Research (F155) Surveyor Training of Trainers: Interpretive Guidance Investigative Protocol Federal Regulatory Language
483.10(b)(4) and (8) Rights Regarding Advance Directives, Treatment, and Experimental Research (F155) Surveyor Training of Trainers: Interpretive Guidance Investigative Protocol Federal Regulatory Language
MAKING YOUR WISHES KNOWN: Advance Care Planning Guide
 MAKING YOUR WISHES KNOWN: Advance Care Planning Guide ADVANCE CARE PLANNING The process of learning about the type of medical decisions that may need to be made, considering those decisions ahead of time
MAKING YOUR WISHES KNOWN: Advance Care Planning Guide ADVANCE CARE PLANNING The process of learning about the type of medical decisions that may need to be made, considering those decisions ahead of time
does staff intervene; used? If not, describe.
 Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Use this pathway for a resident who requires or receives respiratory care services (i.e., oxygen therapy, breathing exercises, sleep apnea, nebulizers/metered-dose inhalers, tracheostomy, or ventilator)
Advance [Health Care] Directive
![Advance [Health Care] Directive Advance [Health Care] Directive](/thumbs/77/75352901.jpg) Advance [Health Care] Directive Introduction I have completed this Advance Directive with much thought. This document gives my treatment choices and preferences, and/or appoints a Health Care Agent (also
Advance [Health Care] Directive Introduction I have completed this Advance Directive with much thought. This document gives my treatment choices and preferences, and/or appoints a Health Care Agent (also
Your Guide to Advance Directives
 Starting Points: Your Guide to Advance Directives Values Statements Healthcare Directives Durable Power of Attorney for Healthcare 1 2 Advances in medicine are helping people to live longer than ever before.
Starting Points: Your Guide to Advance Directives Values Statements Healthcare Directives Durable Power of Attorney for Healthcare 1 2 Advances in medicine are helping people to live longer than ever before.
HealthStream Regulatory Script
 HealthStream Regulatory Script Advance Directives Release Date: August 2008 HLC Version: 602 Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney
HealthStream Regulatory Script Advance Directives Release Date: August 2008 HLC Version: 602 Lesson 1: Introduction Lesson 2: Advance Directives Lesson 3: Living Wills Lesson 4: Medical Power of Attorney
HAWAII HEALTH SYSTEMS CORPORATION
 All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
All Positions HE-13 6.822 Function and Location This position works in the respiratory therapy unit of a hospital and is responsible for supervising several respiratory therapy technicians in providing
Adult: Any person eighteen years of age or older, or emancipated minor.
 Advance Directives Policy and Procedure Purpose To provide an atmosphere of respect and caring and to ensure that each patient's ability and right to participate in medical decision making is maximized
Advance Directives Policy and Procedure Purpose To provide an atmosphere of respect and caring and to ensure that each patient's ability and right to participate in medical decision making is maximized
My Voice - My Choice
 My Voice - My Choice My Advance Directive Table of Contents Introduction... 2 Words You Need to Know... 3 Legal Document... 4 Helpful Information about your Advance Directive... 10 What makes your life
My Voice - My Choice My Advance Directive Table of Contents Introduction... 2 Words You Need to Know... 3 Legal Document... 4 Helpful Information about your Advance Directive... 10 What makes your life
Making Decisions About Your Health Care. (Information about Durable Power of Attorney for Health Care and Living Wills)
 Making Decisions About Your Health Care (Information about Durable Power of Attorney for Health Care and Living Wills) Following guidelines set by federal regulations, we would like to inform you of your
Making Decisions About Your Health Care (Information about Durable Power of Attorney for Health Care and Living Wills) Following guidelines set by federal regulations, we would like to inform you of your
ALLINA HOME & COMMUNITY SERVICES ALLINA HEALTH. Advance Care Planning. Discussion guide. Discussion Guide. Advance care planning
 ALLINA HOME & COMMUNITY SERVICES ALLINA HEALTH Advance Care Planning Discussion guide Discussion Guide Advance care planning Advance care planning Any of us could think of a time when we might be too sick
ALLINA HOME & COMMUNITY SERVICES ALLINA HEALTH Advance Care Planning Discussion guide Discussion Guide Advance care planning Advance care planning Any of us could think of a time when we might be too sick
FOR ILLUSTRATIVE PURPOSES ONLY
 - Page 1 of 15 GUIDANCE Health Professional Guidance for the Care Plan for the Dying Person - Victoria RECOGNISING DYING The possibility that a person may die within the next few days or hours is recognised
- Page 1 of 15 GUIDANCE Health Professional Guidance for the Care Plan for the Dying Person - Victoria RECOGNISING DYING The possibility that a person may die within the next few days or hours is recognised
Fine Bore Tubing Set
 Negotiations Meetings with CME Director (lived on East coast, but came to meet me here on a few occasions) Asked for 2 pumps on loan for a few months Discussed use of locking drivers, so they can only
Negotiations Meetings with CME Director (lived on East coast, but came to meet me here on a few occasions) Asked for 2 pumps on loan for a few months Discussed use of locking drivers, so they can only
I,,, Social Security number
 Durable power of attorney for health care choices & health care choices DIRECTIVE 6- FORM Part I. Durable power of attorney for health care choices I,,, Name Social Security number appoint,, Name Phone
Durable power of attorney for health care choices & health care choices DIRECTIVE 6- FORM Part I. Durable power of attorney for health care choices I,,, Name Social Security number appoint,, Name Phone
 NEW YORK STATE DEPARTMENT OF HEALTH Medical Orders for Life Sustaining Treatment (MOLST) THE PATIENT KEEPS THE ORIGINAL MOLST FORM DURING TRAVEL TO DIFFERENT CARE SETTINGS. THE PHYSICIAN KEEPS A COPY.
NEW YORK STATE DEPARTMENT OF HEALTH Medical Orders for Life Sustaining Treatment (MOLST) THE PATIENT KEEPS THE ORIGINAL MOLST FORM DURING TRAVEL TO DIFFERENT CARE SETTINGS. THE PHYSICIAN KEEPS A COPY.
VIRGINIA Advance Directive Planning for Important Health Care Decisions
 VIRGINIA Advance Directive Planning for Important Health Care Decisions Caring Connections 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CARING CONNECTIONS Caring Connections,
VIRGINIA Advance Directive Planning for Important Health Care Decisions Caring Connections 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CARING CONNECTIONS Caring Connections,
Liverpool Care Pathway for the Dying Patient (LCP) supporting care in the last hours or days of life
 Liverpool Care Pathway for the Dying Patient (LCP) supporting care in the last hours or days of life Please detach perforated Information sheets and give to the relative or carer following a discussion
Liverpool Care Pathway for the Dying Patient (LCP) supporting care in the last hours or days of life Please detach perforated Information sheets and give to the relative or carer following a discussion
Supersedes/Updates: 99-10
 No. 08-07 New York State Department of Health Bureau of Emergency Medical Services POLICY STATEMENT Supersedes/Updates: 99-10 November 20, 2008 Re: Medical Orders for Life Sustaining Treatment (MOLST)
No. 08-07 New York State Department of Health Bureau of Emergency Medical Services POLICY STATEMENT Supersedes/Updates: 99-10 November 20, 2008 Re: Medical Orders for Life Sustaining Treatment (MOLST)
Sedation/Analgesia by Non-Anesthesiologists. THE UNIVERSITY OF TOLEDO Approving Officer:
 Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
Name of Policy: Policy Number: 3364-100-53-11 Department: Hospital Administration Medical Staff ^HEALTH THE UNIVERSITY OF TOLEDO Approving Officer: Chief Executive Officer - UTMC Responsible Agent: -Chief
What would you like to accomplish in the process of advance care planning and/or in completing a health care directive?
 Completing a health care directive is an important step in making sure your loved ones and health care providers understand your values and choices for health care treatment if you are not able to speak
Completing a health care directive is an important step in making sure your loved ones and health care providers understand your values and choices for health care treatment if you are not able to speak
Case 1 Standard of Care. Disclosures. Defending Critical Care: Navigating Through the Malpractice Maze 5/9/2015. Defending Critical Care:
 Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
Defending Critical Care: Navigating Through the Malpractice Maze Defending Critical Care: Navigating Through the Malpractice Maze Joseph Picchi, JD Richard Schoenberger, JD Critical Care Medicine Update
If patient is 24 hour dependent on NIV and decides to discontinue it, support and forward planning are essential
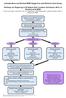 Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Leicestershire and Rutland MND Supportive and Palliative Care Group Pathway for Preparing to Withdraw Non-Invasive Ventilation (NIV) in Patients with MND This is to be read in conjunction with the Guidelines
Using the MOST Form Guidance for Health Care Professionals
 Updated 12.30.14 Using the MOST Form Guidance for Health Care Professionals Introduction and Overview According to the ethical principle of respect for patient autonomy and the legal principle of patient
Updated 12.30.14 Using the MOST Form Guidance for Health Care Professionals Introduction and Overview According to the ethical principle of respect for patient autonomy and the legal principle of patient
VAE PROJECT MASTER ACTION PLAN. Note: Please be aware that these areas overlap to reduce duplication and optimize the synergies
 VAE PROJECT MASTER ACTION PLAN Note: Please be aware that these areas overlap to reduce duplication and optimize the synergies Practice NHSN Surveillance Data Collection Is VAE NHSN Surveillance data collection
VAE PROJECT MASTER ACTION PLAN Note: Please be aware that these areas overlap to reduce duplication and optimize the synergies Practice NHSN Surveillance Data Collection Is VAE NHSN Surveillance data collection
Advance Directive for Health Care
 Advance Directive for Health Care respecting your right to: Choose Your Healthcare Agent Choose the Authority Given to Your Healthcare Agent Choose Your Preferences Related to Treatment & Care Printed
Advance Directive for Health Care respecting your right to: Choose Your Healthcare Agent Choose the Authority Given to Your Healthcare Agent Choose Your Preferences Related to Treatment & Care Printed
A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES. By Maureen Kroning EdD, RN
 A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES By Maureen Kroning EdD, RN Dedication This handbook is dedicated to patients, families, communities and the nurses that touch their lives
A PATIENT S GUIDE TO UNDERSTANDING ADVANCE HEALTH CARE DIRECTIVES By Maureen Kroning EdD, RN Dedication This handbook is dedicated to patients, families, communities and the nurses that touch their lives
ABOUT THE ADVANCE DIRECTIVE FOR RECEIVING ORAL FOOD AND FLUIDS IN DEMENTIA. Introduction
 ABOUT THE ADVANCE DIRECTIVE FOR RECEIVING ORAL FOOD AND FLUIDS IN DEMENTIA Introduction There are two purposes to completing an Advance Directive for Receiving Oral Food and Fluids In Dementia. The first
ABOUT THE ADVANCE DIRECTIVE FOR RECEIVING ORAL FOOD AND FLUIDS IN DEMENTIA Introduction There are two purposes to completing an Advance Directive for Receiving Oral Food and Fluids In Dementia. The first
YOUR RIGHT TO MAKE YOUR OWN HEALTH CARE DECISIONS
 Upon admission to Western Connecticut Health Network, you will be asked if you have any form of an Advance Directive such as a Living Will or a Health Care Representative. If you have such a document,
Upon admission to Western Connecticut Health Network, you will be asked if you have any form of an Advance Directive such as a Living Will or a Health Care Representative. If you have such a document,
2
 1 2 3 4 Designation of Health Care Surrogate I, (please print) want Phone Address to be my Health Care Surrogate and make health care decisions for me as indicated by my initials below: Effective only
1 2 3 4 Designation of Health Care Surrogate I, (please print) want Phone Address to be my Health Care Surrogate and make health care decisions for me as indicated by my initials below: Effective only
Advance Health Care Planning: Making Your Wishes Known. MC rev0813
 Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Advance Health Care Planning: Making Your Wishes Known MC2107-14rev0813 What s Inside Why Health Care Planning Is Important... 2 What You Can Do... 4 Work through the advance health care planning process...
Advance Directives The Patient s Right To Decide CH Oct. 2013
 Advance Directives The Patient s Right To Decide CH80850040 Oct. 2013 Advance Directives Your Right To Make Health Care Decisions Under The Law In Tennessee Tennessee and federal law give every competent
Advance Directives The Patient s Right To Decide CH80850040 Oct. 2013 Advance Directives Your Right To Make Health Care Decisions Under The Law In Tennessee Tennessee and federal law give every competent
CHPCA appreciates and thanks our funding partner GlaxoSmithKline for their unrestricted funding support for Advance Care Planning in Canada.
 CHPCA appreciates and thanks our funding partner GlaxoSmithKline for their unrestricted funding support for Advance Care Planning in Canada. For more information about advance care planning, please visit
CHPCA appreciates and thanks our funding partner GlaxoSmithKline for their unrestricted funding support for Advance Care Planning in Canada. For more information about advance care planning, please visit
VANDERBILT UNIVERSITY MEDICAL CENTER MULTIDISCIPLINARY SURGICAL CRITICAL CARE PERCUTANEOUS TRACHEOSTOMY MANAGEMENT GUIDELINE
 PERCUTANEOUS TRACHEOSTOMY MANAGEMENT GUIDELINE I. PURPOSE: - To standardize the steps and processes involved in the performance of bedside percutaneous tracheostomies in the SICU. - This document should
PERCUTANEOUS TRACHEOSTOMY MANAGEMENT GUIDELINE I. PURPOSE: - To standardize the steps and processes involved in the performance of bedside percutaneous tracheostomies in the SICU. - This document should
Activation of the Rapid Response Team
 Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
Approved by: Activation of the Rapid Response Team Senior Operating Officer, Acute Services, GNCH; and Senior Operating Officer, Acute Services, MCH Edmonton Acute Care Patient Care Policy & Procedures
MASSACHUSETTS Advance Directive Planning for Important Healthcare Decisions
 MASSACHUSETTS Advance Directive Planning for Important Healthcare Decisions Caring Connections 1700 Diagonal Road, Suite 625, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a
MASSACHUSETTS Advance Directive Planning for Important Healthcare Decisions Caring Connections 1700 Diagonal Road, Suite 625, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a
The POLST Conversation POLST Script
 The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes realistic
The POLST Conversation POLST Script The POLST Script provides detailed information in order to develop comfort and competence when facilitating a POLST conversation. The POLST conversation utilizes realistic
CLINICAL SKILLS & OBSERVATION CHECKLIST
 CLINICAL SKILLS & OBSERVATION CHECKLIST Employee: Please check Yes or No at time of hire and annually for Adult and/or Pediatric experience RN Supervisor: Please date and initial after observation & demonstration
CLINICAL SKILLS & OBSERVATION CHECKLIST Employee: Please check Yes or No at time of hire and annually for Adult and/or Pediatric experience RN Supervisor: Please date and initial after observation & demonstration
End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces.
 End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces. Terms Definitions End of Life Care To assist persons who
End of Life Terminology The definitions below applies within the province of Ontario, terms may be used or defined differently in other provinces. Terms Definitions End of Life Care To assist persons who
Objectives. Integrating Palliative Care Principles into Critical Care Nursing
 1 Integrating Palliative Care Principles into Critical Care Nursing It s the Caring, Compassionate, Holistic, Patient and Family Centered, Better Communication, Keeping my patient comfortable amidst the
1 Integrating Palliative Care Principles into Critical Care Nursing It s the Caring, Compassionate, Holistic, Patient and Family Centered, Better Communication, Keeping my patient comfortable amidst the
Directive to Physicians and Family or Surrogates
 Directive to Physicians and Family or Surrogates This is an important legal document, known as an Advance Directive. It is designed to help you communicate your wishes about medical treatment at some time
Directive to Physicians and Family or Surrogates This is an important legal document, known as an Advance Directive. It is designed to help you communicate your wishes about medical treatment at some time
L e g a l I s s u e s i n H e a l t h C a r e
 Page 1 L e g a l I s s u e s i n H e a l t h C a r e Tutorial #6 January 2008 Introduction Patients have the right to accept or refuse health care treatment. For a patient to exercise that right, he or
Page 1 L e g a l I s s u e s i n H e a l t h C a r e Tutorial #6 January 2008 Introduction Patients have the right to accept or refuse health care treatment. For a patient to exercise that right, he or
Advanced Directive. Artificial nutrition and hydration--when food and water are fed to a person through a tube.
 This form is a combined durable power of attorney for health care and a living will (in some jurisdictions). With this form, you can name someone to make medical decisions for you if in the future you're
This form is a combined durable power of attorney for health care and a living will (in some jurisdictions). With this form, you can name someone to make medical decisions for you if in the future you're
Patient Care Protocol
 Patient Care Protocol Document: prtcl_dcd.doc Donation after Circulatory Determination of Death [Pre-Mortem] Site Setting/Population Clinician BCH Only ICU/OR/All Patients with Circulatory Determination
Patient Care Protocol Document: prtcl_dcd.doc Donation after Circulatory Determination of Death [Pre-Mortem] Site Setting/Population Clinician BCH Only ICU/OR/All Patients with Circulatory Determination
Health Care Directive
 Health Care Directive Overview Adults with decision-making capacity have the right to make choices about their health care. No treatments may be given to someone who does not want them. The attached Durable
Health Care Directive Overview Adults with decision-making capacity have the right to make choices about their health care. No treatments may be given to someone who does not want them. The attached Durable
Maryland MOLST. Guide for Patients. Maryland MOLST Training Task Force
 Maryland MOLST Guide for Patients Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Explanatory Guide for Patients Contents Introduction Section I Section
Maryland MOLST Guide for Patients Maryland MOLST Training Task Force May 2012 Health Care Decision Making: Goals and Treatment Options Explanatory Guide for Patients Contents Introduction Section I Section
VIRGINIA Advance Directive Planning for Important Health Care Decisions
 VIRGINIA Advance Directive Planning for Important Health Care Decisions Caring Info 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CARING INFO Caring Info, a program of
VIRGINIA Advance Directive Planning for Important Health Care Decisions Caring Info 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CARING INFO Caring Info, a program of
MY VOICE (STANDARD FORM)
 MY VOICE (STANDARD FORM) a workbook and personal directive for advance care planning WHAT IS ADVANCE CARE PLANNING? Advance care planning is a process for you to: think about what is important to you when
MY VOICE (STANDARD FORM) a workbook and personal directive for advance care planning WHAT IS ADVANCE CARE PLANNING? Advance care planning is a process for you to: think about what is important to you when
Advance Health Care Directive. LIFE CARE planning. my values, my choices, my care. kp.org/lifecareplan
 Advance Health Care Directive LIFE CARE planning my values, my choices, my care kp.org/lifecareplan Name of provider: Introduction This Advance Health Care Directive allows you to share your values, your
Advance Health Care Directive LIFE CARE planning my values, my choices, my care kp.org/lifecareplan Name of provider: Introduction This Advance Health Care Directive allows you to share your values, your
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee
 Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
Cynthia Ann LaSala, MS, RN Nursing Practice Specialist Phillips 20 Medicine Advisor, Patient Care Services Ethics in Clinical Practice Committee What is Advance Care Planning (ACP)? Understanding/clarifying
OREGON Advance Directive Planning for Important Healthcare Decisions
 OREGON Advance Directive Planning for Important Healthcare Decisions Caring Connections 1700 Diagonal Road, Suite 625, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a program
OREGON Advance Directive Planning for Important Healthcare Decisions Caring Connections 1700 Diagonal Road, Suite 625, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a program
Abbreviations used in Care Pathway. CNS Clinical Nurse C Chaplain / clergy / religious adviser
 Patient's Name: D.O.B: Patient GP: Named Nurse: Name: Adapted LCP Version 12 PALLIATIVE CARE PATHWAY (End Stage) PRIMARY CARE DO NOT PUT PATIENT ON THIS PATHWAY UNLESS The Multi-professional Team have
Patient's Name: D.O.B: Patient GP: Named Nurse: Name: Adapted LCP Version 12 PALLIATIVE CARE PATHWAY (End Stage) PRIMARY CARE DO NOT PUT PATIENT ON THIS PATHWAY UNLESS The Multi-professional Team have
WYOMING Advance Directive Planning for Important Healthcare Decisions
 WYOMING Advance Directive Planning for Important Healthcare Decisions Caring Connections 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CARING CONNECTIONS Caring Connections,
WYOMING Advance Directive Planning for Important Healthcare Decisions Caring Connections 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 CARING CONNECTIONS Caring Connections,
Process
 www.theroyl.com Advance Directive And Durable Power Of Attorney Advance Medical Directive State of Virginia The Rest of Your Life recommends that you review completed documents with an attorney, especially
www.theroyl.com Advance Directive And Durable Power Of Attorney Advance Medical Directive State of Virginia The Rest of Your Life recommends that you review completed documents with an attorney, especially
Health Care Directive
 Health Care Directive Overview Adults with decision-making capacity have the right to make choices about their health care. No treatments may be given to someone who does not want them. The attached Durable
Health Care Directive Overview Adults with decision-making capacity have the right to make choices about their health care. No treatments may be given to someone who does not want them. The attached Durable
Many who are interested in medicine, palliative care and hospice and bioethics have been
 NEW "DNR" RULES WENT INTO EFFECT MAY 20, 1999 Many who are interested in medicine, palliative care and hospice and bioethics have been carefully following the progress of the legislation on "portable DNR"
NEW "DNR" RULES WENT INTO EFFECT MAY 20, 1999 Many who are interested in medicine, palliative care and hospice and bioethics have been carefully following the progress of the legislation on "portable DNR"
DURABLE HEALTH CARE POWER OF ATTORNEY AND HEALTH CARE TREATMENT INSTRUCTIONS (LIVING WILL) PART I INTRODUCTORY REMARKS ON HEALTH CARE DECISION MAKING
 DURABLE HEALTH CARE POWER OF ATTORNEY AND HEALTH CARE TREATMENT INSTRUCTIONS (LIVING WILL) PART I INTRODUCTORY REMARKS ON HEALTH CARE DECISION MAKING You have the right to decide the type of health care
DURABLE HEALTH CARE POWER OF ATTORNEY AND HEALTH CARE TREATMENT INSTRUCTIONS (LIVING WILL) PART I INTRODUCTORY REMARKS ON HEALTH CARE DECISION MAKING You have the right to decide the type of health care
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NURSING AND PHARMACY GUIDELINES FOR THE ADMINISTRATION OF IV TREPROSTINIL (REMODULIN ) Job Title of Reviewer: Director, Pharmacy POLICY
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NURSING AND PHARMACY GUIDELINES FOR THE ADMINISTRATION OF IV TREPROSTINIL (REMODULIN ) Job Title of Reviewer: Director, Pharmacy POLICY
Missouri Outside the Hospital Do Not Resuscitate Order. Boone County Fire Protection District EMS Education
 Missouri Outside the Hospital Do Not Resuscitate Order 4 Times to Withhold CPR Obviously mortal wound such as decapitation Rigor mortis Livor mortis also known as dependent lividity or venous pooling Valid
Missouri Outside the Hospital Do Not Resuscitate Order 4 Times to Withhold CPR Obviously mortal wound such as decapitation Rigor mortis Livor mortis also known as dependent lividity or venous pooling Valid
Unit 301 Understand how to provide support when working in end of life care Supporting information
 Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Unit 301 Understand how to provide support when working in end of life care Supporting information Guidance This unit must be assessed in accordance with Skills for Care and Development s QCF Assessment
Advance Directive. What Are Advance Medical Directives? Deciding What You Want. Recording Your Wishes
 Advance Directive What Are Advance Medical Directives? These documents could be a living will or a durable power of attorney for healthcare (also called a healthcare proxy). They allow you to give directions
Advance Directive What Are Advance Medical Directives? These documents could be a living will or a durable power of attorney for healthcare (also called a healthcare proxy). They allow you to give directions
Subacute Care. 1. Define important words in the chapter. 2. Discuss the types of residents who are in a subacute setting
 175 26 Subacute Care 1. Define important words in this chapter 2. Discuss the types of residents who are in a subacute setting 3. List care guidelines for pulse oximetry 4. Describe telemetry and list
175 26 Subacute Care 1. Define important words in this chapter 2. Discuss the types of residents who are in a subacute setting 3. List care guidelines for pulse oximetry 4. Describe telemetry and list
Vermont Advance Directive for Health Care
 Vermont Advance Directive for Health Care Prepared by the Vermont Ethics Network Explanation and Instructions You have the right to give instructions about what types of health care you want or do not
Vermont Advance Directive for Health Care Prepared by the Vermont Ethics Network Explanation and Instructions You have the right to give instructions about what types of health care you want or do not
MY ADVANCE CARE PLANNING GUIDE
 MY DVNCE CRE PLNNING GUIDE Let s TLK! Tell us your values and beliefs about your healthcare. Take time to have the conversation with your physician and your family. lways be open and honest. Leave no doubt
MY DVNCE CRE PLNNING GUIDE Let s TLK! Tell us your values and beliefs about your healthcare. Take time to have the conversation with your physician and your family. lways be open and honest. Leave no doubt
MASSACHUSETTS ADVANCE DIRECTIVES
 MASSACHUSETTS ADVANCE DIRECTIVES Advance directives are legal documents that protect your right to refuse medical treatment you do not want, or to request treatment you do want, in the event you lose the
MASSACHUSETTS ADVANCE DIRECTIVES Advance directives are legal documents that protect your right to refuse medical treatment you do not want, or to request treatment you do want, in the event you lose the
ADVANCE DIRECTIVE FOR MENTAL AND PHYSICAL HEALTH CARE
 ADVANCE DIRECTIVE FOR MENTAL AND PHYSICAL HEALTH CARE I,, hereby make known my desire that, should I lose the capacity to make health care decisions, the following are my instructions regarding consent
ADVANCE DIRECTIVE FOR MENTAL AND PHYSICAL HEALTH CARE I,, hereby make known my desire that, should I lose the capacity to make health care decisions, the following are my instructions regarding consent
HEALTH CARE DIRECTIVE
 1 HEALTH CARE DIRECTIVE I,, understand this document allows me to do ONE OR BOTH of the following: PART I: Name another person (called the health care agent) to make health care decisions for me if I am
1 HEALTH CARE DIRECTIVE I,, understand this document allows me to do ONE OR BOTH of the following: PART I: Name another person (called the health care agent) to make health care decisions for me if I am
COLORADO Advance Directive Planning for Important Healthcare Decisions
 COLORADO Advance Directive Planning for Important Healthcare Decisions Caring Connections 1700 Diagonal Road, Suite 625, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a program
COLORADO Advance Directive Planning for Important Healthcare Decisions Caring Connections 1700 Diagonal Road, Suite 625, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a program
PATIENT RIGHTS, PRIVACY, AND PROTECTION
 REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
REGIONAL POLICY Subject/Title: ADVANCE CARE PLANNING: GOALS OF CARE DESIGNATION (ADULT) Approving Authority: EXECUTIVE MANAGEMENT Classification: Category: CLINICAL PATIENT RIGHTS, PRIVACY, AND PROTECTION
MY ADVANCE CARE PLANNING GUIDE
 MY DVNCE CRE PLNNING GUIDE Let s TLK! Tell us your values and beliefs about your healthcare. Take time to have the conversation with your physician and your family. lways be open and honest. Leave no doubt
MY DVNCE CRE PLNNING GUIDE Let s TLK! Tell us your values and beliefs about your healthcare. Take time to have the conversation with your physician and your family. lways be open and honest. Leave no doubt
Liza Barbarello Andrews, Pharm.D., R.Ph., BCCCP, BCPS
 Making the Shift from Sedation to Managing Pain: Implementing the 2013 SCCM Pain, Agitation & Delirium (PAD) Guidelines Reliably in an Open Community-based ICU Submitted by: Liza Barbarello Andrews, Pharm.D.,
Making the Shift from Sedation to Managing Pain: Implementing the 2013 SCCM Pain, Agitation & Delirium (PAD) Guidelines Reliably in an Open Community-based ICU Submitted by: Liza Barbarello Andrews, Pharm.D.,
Advance Health Care Directive MARYLAND. LIFE CARE planning my values, my choices, my care. kp.org/lifecareplan
 Advance Health Care Directive LIFE CARE planning kp.org/lifecareplan MARYLAND Introduction This advance health care directive lets you share your values, your choices, and your instructions about your
Advance Health Care Directive LIFE CARE planning kp.org/lifecareplan MARYLAND Introduction This advance health care directive lets you share your values, your choices, and your instructions about your
1. Receives report from EMS and/or outlying facility. 5. Adheres to safety and universal precaution guidelines.
 Trauma Nurse Specialist 1. Receives report from EMS and/or outlying facility. 2. Reports to trauma room and signs in. 3. Relays reports to trauma team members. 4. Assists with resuscitation readiness:
Trauma Nurse Specialist 1. Receives report from EMS and/or outlying facility. 2. Reports to trauma room and signs in. 3. Relays reports to trauma team members. 4. Assists with resuscitation readiness:
Adult Patient Controlled Analgesia (PCA)
 Contents... 1 Policy... 1 Scope/Audience... 1 Associated Documents... 1 Statement... 2 Criteria... 2 Patient and Whanau Education... 2 Procedural Considerations... 3 Pre Administration... 3 Patient Monitoring...
Contents... 1 Policy... 1 Scope/Audience... 1 Associated Documents... 1 Statement... 2 Criteria... 2 Patient and Whanau Education... 2 Procedural Considerations... 3 Pre Administration... 3 Patient Monitoring...
Health Care Directive. Choose whether you want life-sustaining treatments in certain situations.
 Durable Power of Attorney (DPOA) for Health Care Health Care Directive Documents are legally valid in Washington What is advance care planning? Advance care planning is for all adults 18 and older. It
Durable Power of Attorney (DPOA) for Health Care Health Care Directive Documents are legally valid in Washington What is advance care planning? Advance care planning is for all adults 18 and older. It
Health Care Directive. Choose whether you want life-sustaining treatments in certain situations.
 Durable Power of Attorney (DPOA) for Health Care Health Care Directive Documents are legally valid in Washington What is advance care planning? Advance care planning is for all adults 18 and older. It
Durable Power of Attorney (DPOA) for Health Care Health Care Directive Documents are legally valid in Washington What is advance care planning? Advance care planning is for all adults 18 and older. It
NEBRASKA Advance Directive Planning for Important Healthcare Decisions
 NEBRASKA Advance Directive Planning for Important Healthcare Decisions Caring Connections 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a program of
NEBRASKA Advance Directive Planning for Important Healthcare Decisions Caring Connections 1731 King St., Suite 100, Alexandria, VA 22314 www.caringinfo.org 800/658-8898 Caring Connections, a program of
LIFE CARE planning. Advance Health Care Directive. my values, my choices, my care OREGON. kp.org/lifecareplan
 Advance Health Care Directive OREGON LIFE CARE planning kp.org/lifecareplan 60418810_NW All plans offered and underwritten by Kaiser Foundation Health Plan of the Northwest. 500 NE Multnomah St., Suite
Advance Health Care Directive OREGON LIFE CARE planning kp.org/lifecareplan 60418810_NW All plans offered and underwritten by Kaiser Foundation Health Plan of the Northwest. 500 NE Multnomah St., Suite
ADVANCED HEALTH CARE DIRECTIVE OF LAWRENCE HALL JR.
 ADVANCED HEALTH CARE DIRECTIVE OF LAWRENCE HALL JR. Identification. I, Lawrence Hall Jr., being a competent adult of sound mind, having the capacity to make health care decisions, willfully and voluntarily
ADVANCED HEALTH CARE DIRECTIVE OF LAWRENCE HALL JR. Identification. I, Lawrence Hall Jr., being a competent adult of sound mind, having the capacity to make health care decisions, willfully and voluntarily
